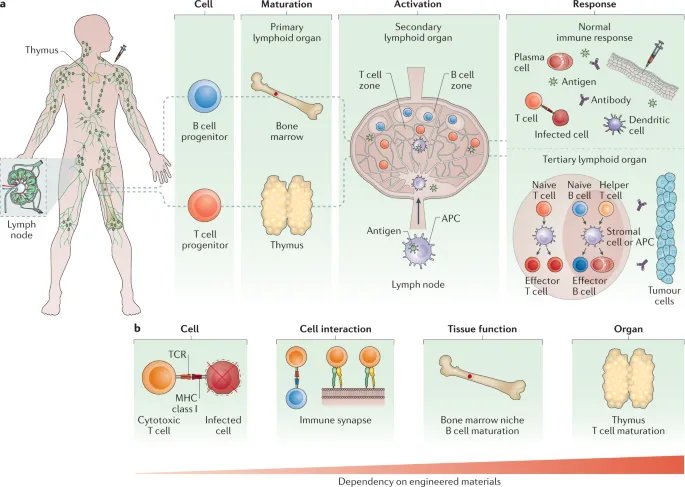
Primary Lymphoid Organs - Cell University
- Sites of lymphocyte development & maturation from stem cells.
- Bone Marrow:
- Central hematopoietic organ: Origin of all blood cells.
- B-lymphocyte (B-cell) maturation site.
- B-cells acquire B-Cell Receptors (BCR); negative selection occurs.
- Thymus:
- Bilobed organ; T-lymphocyte (T-cell) maturation & "education".
- Cortex: Positive selection. T-cells must bind self-MHC. Failure -> apoptosis. Immature thymocytes (CD4+CD8+, double positive).
- Medulla: Negative selection. T-cells binding self-antigens too strongly -> apoptosis (central tolerance). AIRE gene crucial. Mature thymocytes (CD4+ or CD8+, single positive). Hassall's corpuscles present.
⭐ DiGeorge Syndrome (22q11.2 deletion) leads to thymic aplasia/hypoplasia, causing T-cell deficiency, hypocalcemia (parathyroid hypoplasia), and cardiac defects. 📌 CATCH-22: Cardiac defects, Abnormal facies, Thymic hypoplasia, Cleft palate, Hypocalcemia/Hypoparathyroidism due to 22q11 deletion.
Secondary Lymphoid Organs & MALT - Antigen Arenas
- Lymph Nodes: Bean-shaped; filter lymph; initiate adaptive immunity.
- Cortex: B-cell follicles (primary/secondary germinal centers).
- Paracortex: T-cells, dendritic cells.
- Medulla: Plasma cells, macrophages.
- Spleen: Filters blood; removes old RBCs, pathogens.
- White Pulp: Periarteriolar lymphoid sheaths (PALS - T-cells), follicles (B-cells).
- Red Pulp: Sinusoids, macrophages; RBC destruction.
- MALT (Mucosa-Associated Lymphoid Tissue): Protects mucosal surfaces.
- Includes GALT (e.g., Peyer’s patches in ileum), BALT, NALT.
- Site of IgA production.
⭐ Splenectomy significantly increases susceptibility to encapsulated bacteria (e.g., S. pneumoniae, H. influenzae type b, N. meningitidis).
Innate Immune Cells - First Responders
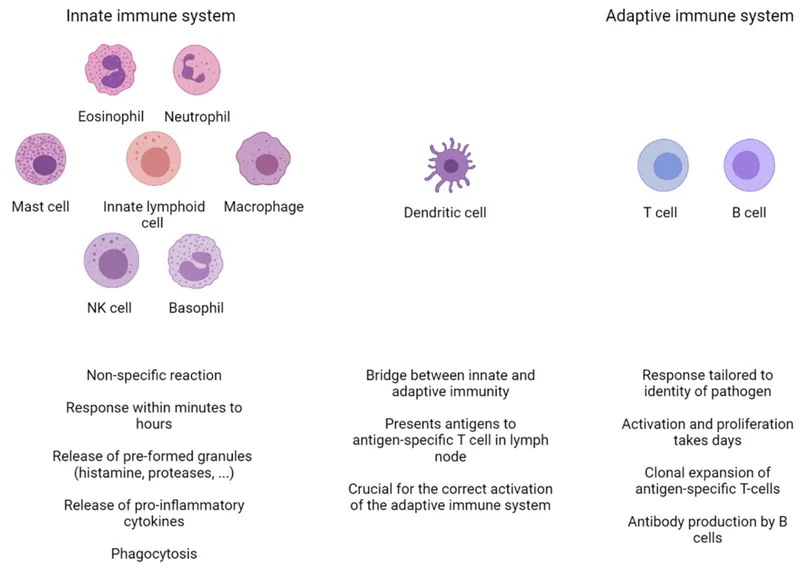
- Neutrophils (Polymorphonuclear Leukocytes, PMNs):
- Most abundant phagocytes; key in acute inflammation.
- Multi-lobed nucleus; granules contain bactericidal enzymes.
- Macrophages:
- Phagocytosis; antigen presentation to T cells; cytokine production.
- Derived from blood monocytes; reside in tissues (e.g., Kupffer cells, alveolar macrophages).
- Natural Killer (NK) Cells:
- Lymphocytes; kill virus-infected cells & tumor cells without prior sensitization.
- Recognize cells lacking MHC class I molecules.
- Dendritic Cells (DCs):
- Most potent antigen-presenting cells (APCs).
- Initiate adaptive immune responses; link innate and adaptive immunity.
- Mast Cells:
- Located in connective tissues, near blood vessels.
- Release histamine, leukotrienes, prostaglandins during allergic reactions & inflammation.
- Eosinophils:
- Combat parasitic helminth infections; modulate allergic inflammatory responses.
- Granules contain major basic protein.
- Basophils:
- Circulating granulocytes; similar functions to mast cells.
- Release histamine and other mediators in allergic responses.
⭐ Chronic Granulomatous Disease (CGD) is caused by a defect in NADPH oxidase, leading to recurrent infections with catalase-positive organisms (e.g., S. aureus, Aspergillus).
Adaptive Immune Cells - Elite Squad
- T-Lymphocytes (Cell-Mediated Immunity): Mature in Thymus.
- Helper T (Th) cells: CD4+. Activate B-cells, Tc cells, macrophages. 📌 MHC-II restricted (CD4 x 2 = 8).
- Cytotoxic T (Tc) cells: CD8+. Kill virus-infected & tumor cells. 📌 MHC-I restricted (CD8 x 1 = 8).
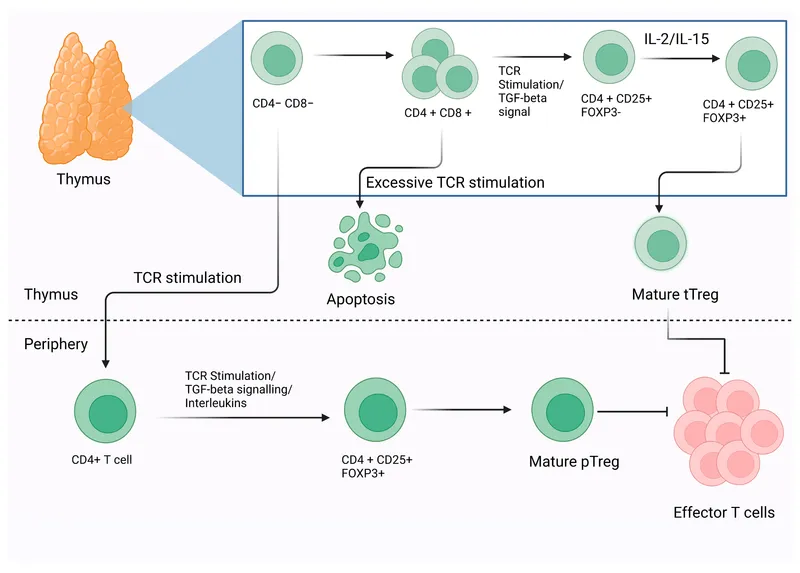
- Regulatory T (Treg) cells: CD4+, CD25+. Suppress immune response, maintain tolerance.
- B-Lymphocytes (Humoral Immunity): Mature in Bone marrow.
- Differentiate into Plasma cells (secrete antibodies) & Memory B-cells (long-term immunity).
- Recognize antigens via B-cell receptors (BCR); require Th cell help for activation (most antigens).
⭐ CD4+ T-cell count is a critical marker for HIV infection progression; a count below 200 cells/μL defines AIDS.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary lymphoid organs: Bone marrow (B-cell maturation) and Thymus (T-cell maturation).
- Secondary lymphoid organs (spleen, lymph nodes, MALT) are sites of antigen encounter and response initiation.
- CD4+ T-cells (helper) recognize MHC-II; CD8+ T-cells (cytotoxic) recognize MHC-I.
- Key B-cell markers include CD19, CD20; NK cells express CD16/CD56 and lack CD3.
- Dendritic cells are the most potent Antigen Presenting Cells (APCs), linking innate and adaptive immunity.
- Thymic negative selection is crucial for self-tolerance, eliminating self-reactive T-cells in the thymus medulla.
- Hassall's corpuscles are characteristic of the thymic medulla; their exact function is still debated but linked to T-reg development.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

