Autoimmunity Basics - Tolerance Lost & Found (Not!)
- Autoimmunity: Immune system mistakenly attacks self-tissues due to failure of self-tolerance.
- Self-Tolerance: Body's unresponsiveness to its own antigens.
- Central: Deletion of self-reactive T cells (thymus) & B cells (bone marrow).
- Peripheral: Anergy, suppression by Tregs, or apoptosis of escaped self-reactive cells.
- Breakdown of Tolerance:
- Genetic: HLA associations (e.g., HLA-B27: Ankylosing Spondylitis; HLA-DR3/DR4: T1DM, RA).
- Environmental: Infections (molecular mimicry, bystander activation), drugs, tissue injury.
- Hormonal: Estrogen often ↑ autoimmunity risk.

⭐ Molecular mimicry: Microbial antigens resemble self-antigens, triggering autoimmunity (e.g., Rheumatic Fever post-Streptococcal infection).
SLE Spotlight - Wolf's Masquerade
Chronic, multi-system autoimmune disease. Pathogenesis: Type III Hypersensitivity Reaction (immune complex deposition).
- Key Autoantibodies:
- ANA: Sensitive (screening).
- Anti-dsDNA: Highly specific; correlates with nephritis activity.
- Anti-Sm: Most specific diagnostic marker.
- Clinical Criteria: 📌 SOAP BRAIN MD (mnemonic for ACR/EULAR criteria)
- Serositis (pleuritis or pericarditis)
- Oral ulcers (painless)
- Arthritis (non-erosive, ≥2 joints)
- Photosensitivity (rash after UV exposure)
- Blood disorders (hemolytic anemia, leukopenia, thrombocytopenia)
- Renal (proteinuria >0.5 g/day or cellular casts)
- ANA positive
- Immunologic (anti-dsDNA, anti-Sm, antiphospholipid Abs)
- Neurologic (seizures, psychosis)
- Malar rash (butterfly rash)
- Discoid rash (scarring plaques)
- Cardiac: Libman-Sacks endocarditis (sterile, verrucous vegetations on valves).
⭐ Anti-dsDNA and Anti-Sm antibodies are highly specific for SLE.

RA & Sjogren's - Joint & Dry Misery
- Rheumatoid Arthritis (RA):
- Pathogenesis: Type IV HSR; CD4+ T cells, cytokines (TNF-α, IL-1); pannus formation (inflamed synovial tissue).
- Clinical Features: Symmetrical polyarthritis (small joints: MCP, PIP); morning stiffness >1hr; deformities (swan neck, boutonniere, ulnar deviation). Extra-articular: nodules, vasculitis.
- Antibodies: Rheumatoid Factor (RF), Anti-CCP (highly specific).
- Sjogren's Syndrome (SS):
- Pathogenesis: Autoimmune lymphocytic infiltration of exocrine glands (lacrimal, salivary).
- Clinical Features: Keratoconjunctivitis sicca (dry eyes), xerostomia (dry mouth). Risk of B-cell lymphoma.
- Antibodies: Anti-Ro/SSA, Anti-La/SSB. (📌 RoLanda has Sjogren's with SS-A and SS-B).
⭐ Anti-CCP antibodies are more specific for Rheumatoid Arthritis than Rheumatoid Factor.

Organ-Specific Autoimmunity - Organ Under Siege
- Hashimoto's Thyroiditis: Autoimmune destruction (Type II & IV HSR) → hypothyroidism. Antibodies: Anti-TPO, Anti-Tg. Histo: Lymphocytic infiltrate, Hurthle cells.
- Graves' Disease: Type II HSR, TSH-Receptor stimulating antibodies (TSI) → hyperthyroidism, exophthalmos. Antibodies: Anti-TSHR.
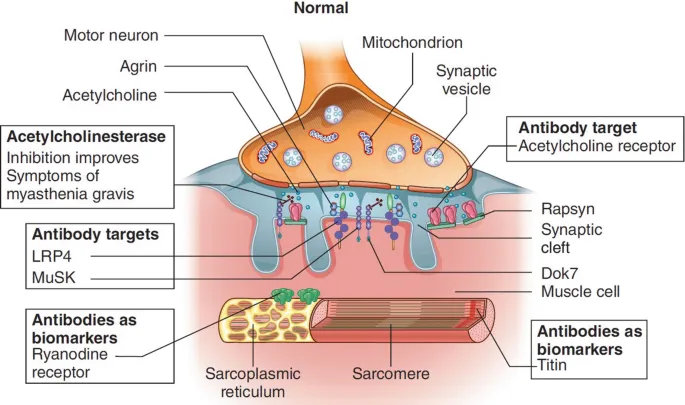
- Myasthenia Gravis: Type II HSR, Anti-AChR antibodies at NMJ → fluctuating muscle weakness (ptosis, diplopia), worse with exertion.
⭐ Myasthenia Gravis is frequently associated with thymic hyperplasia (approx. 65%) or thymoma (approx. 10-15%).
High‑Yield Points - ⚡ Biggest Takeaways
- Molecular mimicry & epitope spreading are key pathogenetic mechanisms in autoimmunity.
- Strong HLA associations are common (e.g., HLA-B27 with Ankylosing Spondylitis).
- SLE: ANA is sensitive; anti-dsDNA & anti-Sm are highly specific markers.
- Rheumatoid Arthritis: Symmetric small joint arthritis; Rheumatoid Factor (RF) & anti-CCP positive.
- Sjögren's Syndrome: Sicca symptoms (dry eyes/mouth); Anti-Ro/SSA & Anti-La/SSB characteristic.
- Systemic Sclerosis: Fibrosis is hallmark; Anti-Scl-70 (diffuse), Anti-centromere (CREST).
- Autoimmunity often involves Type II, III, & IV hypersensitivity reactions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

