Adaptive Immunity: Overview - The Smart Defenders
- Specificity: Precisely targets unique pathogen antigens.
- Memory: Enables faster, stronger response upon re-exposure (anamnestic response). 📌 Secondary response is Stronger & Swifter.
- Diversity: Generates a vast repertoire of antigen receptors.
- Self/Non-self Discrimination: Crucial for preventing autoimmunity.
- Key players: T lymphocytes (cell-mediated immunity) & B lymphocytes (humoral immunity).

⭐ Clonal selection theory, proposed by Burnet, forms the basis of adaptive immunity, explaining lymphocyte specificity and memory.
Cells: T & B Lymphocytes - The Immune Troops
- T-Lymphocytes (T-cells): Cell-mediated immunity.
- Origin: Bone Marrow. Maturation: Thymus (📌 T for Thymus).
- Markers: CD3 (pan T-cell), CD4 (Helper), CD8 (Cytotoxic).
- CD4+ T-cells (Helper): Orchestrate response; activate B-cells, macrophages.
- CD8+ T-cells (Cytotoxic): Lyse infected/tumor cells.
- B-Lymphocytes (B-cells): Humoral immunity.
- Origin & Maturation: Bone Marrow (📌 B for Bone Marrow).
- Function: Differentiate to plasma cells → secrete antibodies.
- Markers: CD19, CD20.
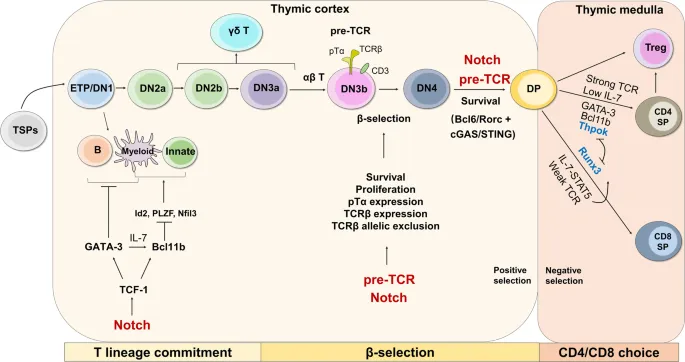
⭐ Positive and negative selection in the thymus are crucial for T cell development and self-tolerance.
Antigen Presentation: MHC - The ID Checkpoint
- MHC (HLA in humans): Cell surface glycoproteins; present processed antigen peptides to T-cells.
- Key for T-cell activation and self/non-self discrimination.
| Feature | MHC Class I | MHC Class II |
|---|---|---|
| Cells | All nucleated | APCs (macrophages, DCs, B-cells) |
| Antigen | Endogenous (viral, tumor) | Exogenous (e.g., bacterial) |
| Binds | CD8+ T-cells | CD4+ T-cells |
| Pathway | Cytosolic; TAP to ER | Endocytic; MIIC |
| 📌 Mnemonic | Rule of 8: 1 x 8 = 8 | Rule of 8: 2 x 4 = 8 |
⭐ MHC gene polymorphism (HLA in humans) is responsible for transplant rejection and susceptibility to autoimmune diseases.
Humoral Immunity: Antibodies - The Armada Unleashed
- B-cells, activated by antigen (often with T-cell help), differentiate into plasma cells (antibody factories) and memory B-cells.
- Antibodies (Immunoglobulins - Ig): Y-shaped proteins.
- Fab region: Antigen-binding.
- Fc region: Effector functions (e.g., opsonization, complement activation).
- Key Functions: Neutralization, Opsonization, Complement activation (classical pathway), Antibody-Dependent Cell-mediated Cytotoxicity (ADCC).
- 📌 Antibody Isotypes (Mnemonic: GAMED):
Isotype Structure Key Feature(s) IgG Monomer Main serum Ab, crosses placenta, opsonization IgA Dimer (secretory) Mucosal immunity (tears, saliva, gut) IgM Pentamer First responder (primary), potent complement fixer IgE Monomer Allergic reactions, parasite defense IgD Monomer B-cell surface receptor, role unclear

⭐ IgM is the first antibody produced during a primary immune response and exists as a pentamer, making it highly effective at activating complement.
Cell-Mediated Immunity: T Cells - The Direct Attackers
- Primary defense: Intracellular pathogens (viruses, specific bacteria) & tumor cells.
- Key Players:
- Cytotoxic T Lymphocytes (CTLs/CD8+): Directly kill target cells. Recognize antigen + MHC-I.
- Mechanisms: Perforin, Granzymes, Fas-FasL.
- Helper T Lymphocytes (Th/CD4+): Orchestrate immunity. Recognize antigen + MHC-II.
- Subsets: Th1 (CMI), Th2 (Humoral), Th17 (Inflammation).
- Cytotoxic T Lymphocytes (CTLs/CD8+): Directly kill target cells. Recognize antigen + MHC-I.
- Activation: TCR binds Ag-MHC + co-stimulation (e.g., CD28-B7).
⭐ IFN-γ, produced by Th1 cells and NK cells, is crucial for macrophage activation and cell-mediated immunity against intracellular pathogens.
High‑Yield Points - ⚡ Biggest Takeaways
- T cells mature in the thymus; B cells in bone marrow.
- MHC I (all nucleated cells) presents endogenous antigens to CD8+ T cells.
- MHC II (APCs) presents exogenous antigens to CD4+ T cells.
- T-cell activation requires two signals: TCR-MHC/peptide and B7-CD28 co-stimulation.
- B cells undergo isotype switching and somatic hypermutation for antibody diversity.
- Memory B and T cells mediate rapid and robust secondary immune responses.
- Regulatory T cells (Tregs), often CD4+ CD25+ FOXP3+, maintain peripheral tolerance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

