MPN Overview & Classification - Proliferation Powerhouse
⭐ MPNs are clonal hematopoietic stem cell disorders characterized by proliferation of one or more myeloid lineages, often with a relatively mature phenotype.
- Hallmark: Autonomous proliferation of myeloid cells.
- WHO Classification (Major):
- Chronic Myeloid Leukemia (CML): BCR-ABL1 positive.
- Polycythemia Vera (PV): ↑ RBCs.
- Essential Thrombocythemia (ET): ↑ Platelets.
- Primary Myelofibrosis (PMF): Marrow fibrosis, splenomegaly.
- Chronic Neutrophilic Leukemia (CNL)
- Chronic Eosinophilic Leukemia, NOS (CEL, NOS)
- Key Pathogenesis: Tyrosine kinase activation (e.g., JAK2 V617F, CALR, MPL).
- Clinical: ↑ Blood counts, organomegaly, thrombosis/bleeding risk.
Chronic Myeloid Leukemia (CML) - Philly's Chromosome Tale
- MPN: Dysregulated production of mature/maturing granulocytes.
- Pathogenesis:
- ⭐ > The Philadelphia chromosome, t(9;22)(q34.1;q11.2), resulting in the BCR-ABL1 fusion oncogene, is the pathognomonic molecular lesion in CML.
- BCR-ABL1: Constitutively active tyrosine kinase.
- Clinical Phases (📌 CAB):
- Chronic: <10% blasts. Most common.
- Accelerated: 10-19% blasts, basophilia ≥20%, worsening splenomegaly/cytopenias.
- Blast Crisis: ≥20% blasts (myeloid/lymphoid). Like acute leukemia.
- Diagnosis:
- PBS: Marked leukocytosis, left shift, basophilia, eosinophilia.
- BM: Hypercellular, ↑M:E ratio.
- t(9;22) or BCR-ABL1 (Cytogenetics/FISH/PCR).
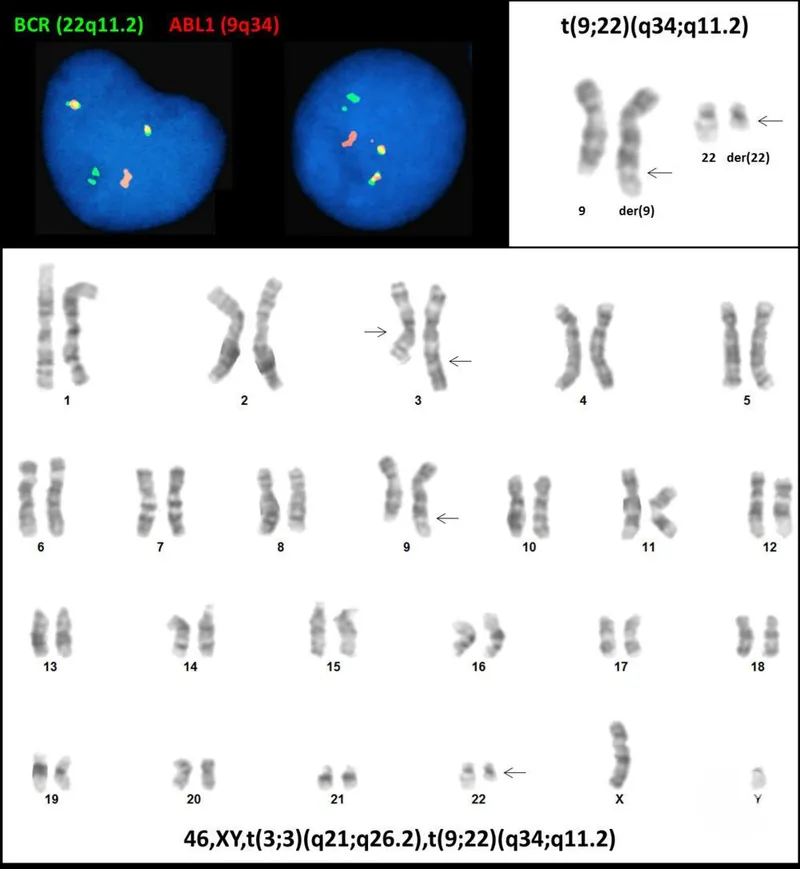 Philadelphia chromosome OR CML peripheral blood smear with marked leukocytosis, left shift, basophilia)
Philadelphia chromosome OR CML peripheral blood smear with marked leukocytosis, left shift, basophilia)
- Treatment:
- Tyrosine Kinase Inhibitors (TKIs) e.g., Imatinib.
PV, ET, & PMF - The JAK/CALR/MPL Crew
⭐ JAK2 V617F mutation is the most common driver mutation in BCR-ABL1 negative MPNs, present in >95% of Polycythemia Vera cases and ~50-60% of Essential Thrombocythemia and Primary Myelofibrosis cases.
| Feature | Polycythemia Vera (PV) | Essential Thrombocythemia (ET) | Primary Myelofibrosis (PMF) |
|---|---|---|---|
| Defining | ↑ RBC mass (Hb >16.5/16 g/dL), Panmyelosis | Sustained ↑ Platelets (≥450,000/μL), no reactive cause | BM fibrosis, Extramedullary hematopoiesis (EMH), cytopenias |
| Mutations | JAK2 V617F (>95%), JAK2 Exon 12 | JAK2 V617F ( | JAK2 V617F ( |
| Key Labs | ↓ Serum EPO; ↑WBC, ↑Platelets often; ↑LDH, ↑Uric acid | Normal/↑ EPO; Platelets ≥450,000/μL | Anemia (often severe); Leukoerythroblastosis; Teardrop RBCs |
| Bone Marrow | Hypercellular (panmyelosis); Pleomorphic megakaryocytes | ↑ Megakaryocytes (large, staghorn clusters); No/minimal fibrosis | Fibrosis (reticulin/collagen); Dry tap; Osteosclerosis |
| Clinical | Plethora, aquagenic pruritus, splenomegaly, thrombosis, gout | Thrombosis/hemorrhage, erythromelalgia, mild/no splenomegaly | Massive splenomegaly, B-symptoms, bone pain, cachexia |
| Progression | Myelofibrosis (MF) (~10-15%), Acute Myeloid Leukemia (AML) (~2-5%) | MF (<10%), AML (~1-2%) | AML (~5-20%) |
MPN Complications & Progression - Trouble Brewing
- Thrombotic/Hemorrhagic Events: Arterial (MI, CVA), venous (DVT, PE); often due to abnormal platelet function or count.
- Hyperuricemia & Gout: Result of ↑ cell turnover.
- Progressive Splenomegaly: Common, from extramedullary hematopoiesis.
- Disease Progression:
- Myelofibrosis (Spent Phase / Post-PV/ET MF)
- Acute Myeloid Leukemia (AML) transformation (poor prognosis)
⭐ The major long-term risks across MPNs include thrombotic and hemorrhagic events, progression to myelofibrosis (spent phase), and transformation to acute myeloid leukemia (AML).
High‑Yield Points - ⚡ Biggest Takeaways
- JAK2 V617F mutation is a common driver in PV, ET, and PMF.
- Polycythemia Vera (PV): ↑RBC mass, ↓EPO, and characteristic aquagenic pruritus.
- Essential Thrombocythemia (ET): Marked thrombocytosis, with thrombotic/hemorrhagic risks.
- Primary Myelofibrosis (PMF): Features bone marrow fibrosis, extramedullary hematopoiesis, and dacrocytes.
- CML: BCR-ABL1 fusion (Philadelphia chromosome) is pathognomonic; treat with TKIs.
- MPNs can transform to AML or progress to myelofibrosis (spent phase).
- CALR and MPL mutations are significant in JAK2-negative ET/PMF.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

