Hemostasis Essentials - Clotting Cascade Crew
Normal hemostasis:
- Vascular Spasm: Rapid vessel constriction, limits initial blood loss.
- Platelet Plug: Platelets adhere, activate, aggregate (Primary Hemostasis).
- Coagulation Cascade: Sequential factor activation for fibrin clot (Secondary Hemostasis).
- Intrinsic: Contact activation (collagen). Factors: XII, XI, IX, VIII. (Monitored by aPTT).
- Extrinsic: Tissue Factor (TF III) release. Factor: VII. (Monitored by PT/INR).
- Common: Convergence of pathways. Factors: X, V, II (Prothrombin), I (Fibrinogen), XIII (stabilizes clot).
- Fibrinolysis: Plasmin-mediated breakdown of fibrin, restoring blood flow.
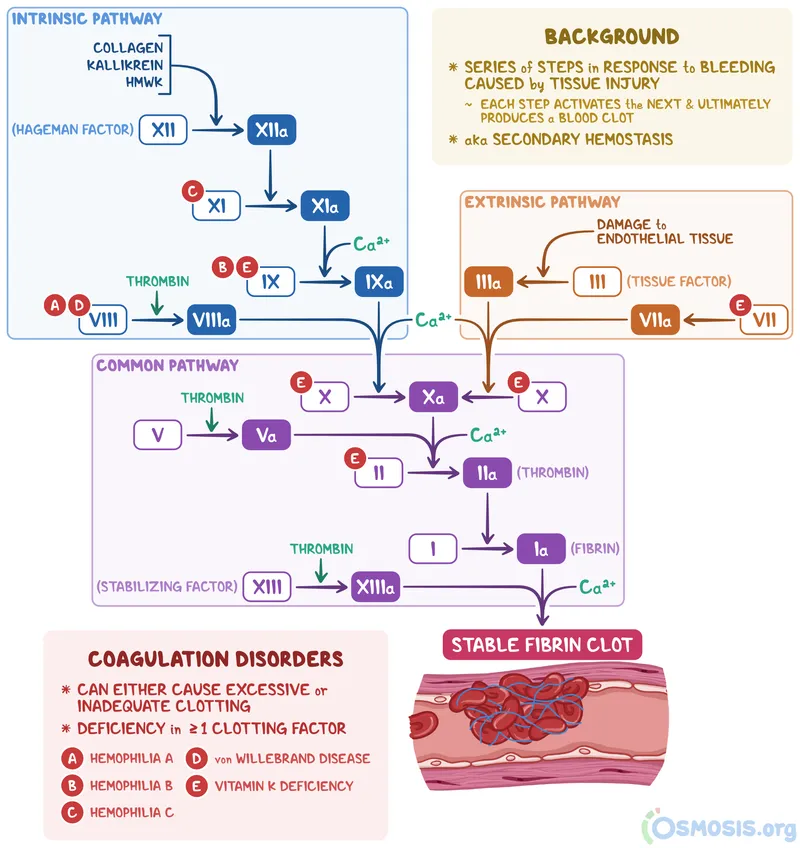
⭐ Vitamin K dependent factors are II, VII, IX, X, Protein C & S. (Mnemonic: 1972, C, S) 📌
Platelet Problems - Plug Pullers' Plight
- Thrombocytopenia (↓ Platelets):
- ITP (Immune Thrombocytopenic Purpura): Autoantibodies vs GpIIb/IIIa. 📌 ITP: Idiots Trashing Platelets. Bleeding if < 10,000-20,000/μL.
- TTP (Thrombotic Thrombocytopenic Purpura): ADAMTS13 deficiency (vWF cleaving protease).
⭐ TTP pentad: Fever, Anemia (microangiopathic hemolytic), Thrombocytopenia, Renal failure, Neurological symptoms (FAT RN).
- HUS (Hemolytic Uremic Syndrome): E. coli O157:H7 (Shiga toxin). Triad: MAHA, thrombocytopenia, ARF.
- DIC (Disseminated Intravascular Coagulation): Widespread clotting activation → consumption → bleeding. ↑PT/PTT/D-dimer, ↓Fibrinogen.
- Qualitative Platelet Defects:
- Bernard-Soulier Syndrome: GpIb defect. Impaired adhesion to vWF. Large platelets.
- Glanzmann Thrombasthenia: GpIIb/IIIa defect. Impaired aggregation.
- Von Willebrand Disease (vWD): Commonest inherited bleeding disorder; vWF defect. Mucocutaneous bleeding.
- Types: 1 (partial quantitative ↓), 2 (qualitative defect), 3 (severe/total quantitative ↓).
- Dx: ↓vWF:Ag, ↓Ristocetin cofactor activity, PTT may be ↑ (due to ↓FVIII).
Coagulation Chaos - Factor Fumbles
- Hemophilias: Inherited X-linked (A & B) or Autosomal (C) bleeding disorders due to specific factor deficiencies.
Feature Hemophilia A (Classic) Hemophilia B (Christmas Dis.) 📌 Hemophilia C Deficiency Factor VIII Factor IX Factor XI Inheritance X-linked recessive X-linked recessive Autosomal Rec. Labs (PT/PTT/BT) N PT, ↑PTT, N BT N PT, ↑PTT, N BT N PT, ↑PTT, N BT Severity (F.VIII/IX) <1% severe, 1-5% mod., >5-40% mild <1% severe, 1-5% mod., >5-40% mild Variable bleeding - Vitamin K Deficiency:
- ↓ Factors II, VII, IX, X, Protein C & S (📌 2,7,9,10,C,S).
- ↑PT (earliest), then ↑PTT. Normal BT.
- Causes: Neonates, malabsorption, broad-spectrum antibiotics, warfarin.
- Liver Disease Coagulopathy:
- ↓ Synthesis of most clotting factors (except FVIII, vWF) & anticoagulants.
- ↑PT, ↑PTT. Dysfibrinogenemia. ↓Platelets (hypersplenism).
- Disseminated Intravascular Coagulation (DIC): Pathological systemic activation of coagulation. Widespread microthrombi consume platelets & factors, leading to bleeding.
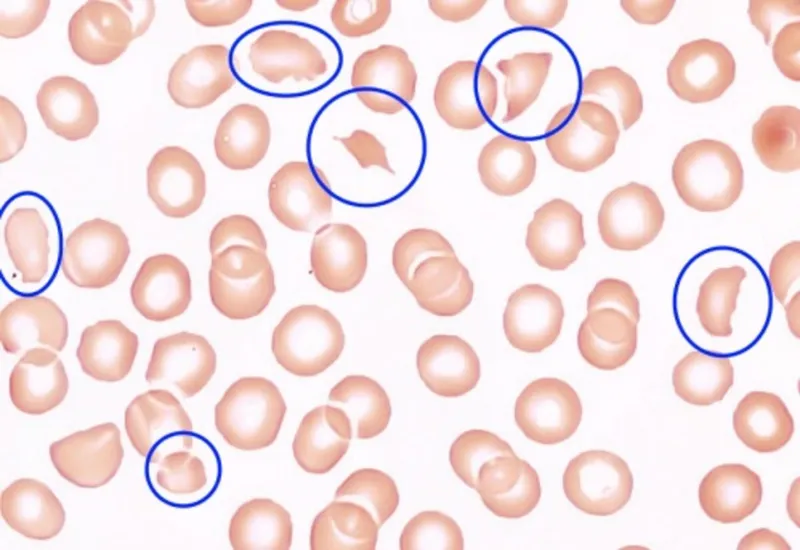
- Labs: ↑PT, ↑PTT, ↑BT, ↓Fibrinogen, ↑D-dimer (key), ↓Platelets, Schistocytes.
- Anticoagulant Effects:
- Heparin: Potentiates Antithrombin III; ↑PTT.
- Warfarin: Inhibits Vit K epoxide reductase; ↑PT/INR.
⭐ Mixing studies differentiate factor deficiency (correction with normal plasma) from an inhibitor (no correction).
Lab Lowdown - Bleed Sleuth
Key tests: Platelet Count (Plt Ct), BT/PFA-100, PT, aPTT. D-dimer for DIC. Fibrinogen levels. Thrombin Time (TT).
Lab Patterns:
| Disorder | Plt Ct | BT/PFA | PT | aPTT | Key |
|---|---|---|---|---|---|
| ITP | ↓↓↓ | ↑ | N | N | Isolated thrombocytopenia |
| Hemophilia A/B | N | N | N | ↑ | Factor VIII/IX deficiency |
| vWD (common) | N | ↑ | N | N/↑ | Most common inherited |
| DIC (acute) | ↓ | ↑ | ↑ | ↑ | ↑D-dimer, ↓Fibrinogen, ↑TT |
| Vit K Def | N | N | ↑ | N/↑ | Early: ↑PT; Severe: ↑PT & ↑aPTT |
High‑Yield Points - ⚡ Biggest Takeaways
- Hemophilia A (FVIII↓) & B (FIX↓): X-linked, ↑aPTT, normal PT/BT.
- Von Willebrand Disease (vWD): Most common inherited, ↑BT, often ↑aPTT (vWF stabilizes FVIII).
- ITP: Isolated thrombocytopenia (anti-GpIIb/IIIa Abs), ↑BT, normal PT/aPTT.
- DIC: Widespread clotting activation, ↑PT/aPTT/BT/D-dimer, ↓platelets, schistocytes.
- Vitamin K Deficiency: Affects II, VII, IX, X, C, S; ↑PT (early), then ↑aPTT.
- TTP: ADAMTS13 deficiency; Pentad: Fever, MAHA, Thrombocytopenia, Renal, Neurologic.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

