Edema & Fluid Balance - Water Woes
- Edema: Excess interstitial fluid. Body water: ~60% total weight (ICF 2/3, ECF 1/3).
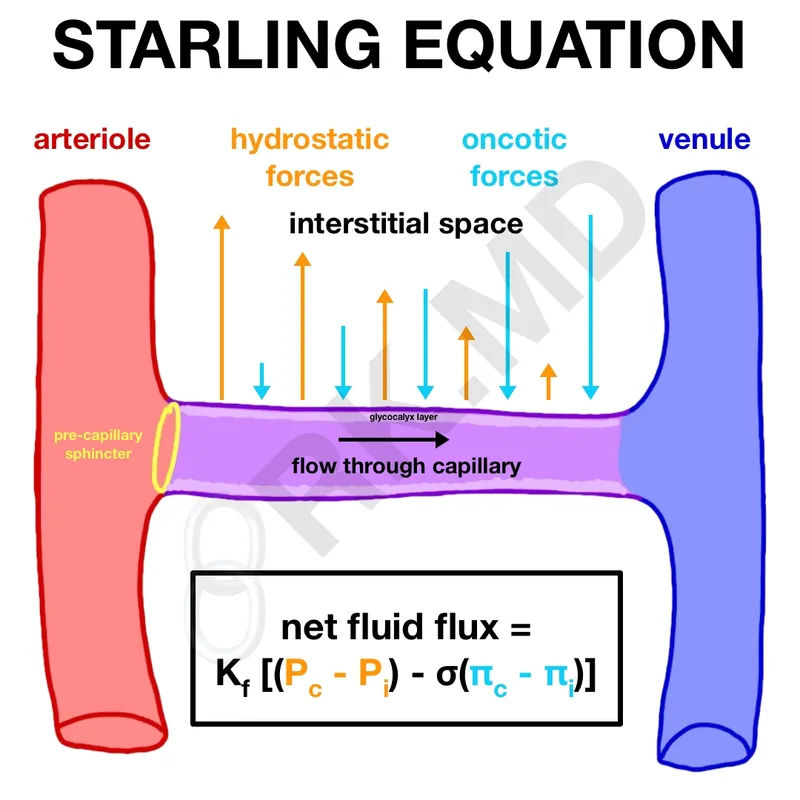
- Starling's Equation: Net Filtration = $K_f \times [(P_c - P_i) - \sigma (\pi_c - \pi_i)]$
- Key Pathophysiology:
- ↑ Capillary hydrostatic pressure ($P_c$): Heart failure, venous obstruction.
- ↓ Plasma oncotic pressure ($%pi_c$): Nephrotic syndrome, liver failure, malnutrition (↓ albumin).
- ↑ Capillary permeability: Inflammation, burns.
- Lymphatic obstruction: Lymphedema, filariasis.
- Sodium & water retention: Renal dysfunction.
- Types:
- Pitting (transudate) vs. Non-pitting (exudate/lymphedema).
- Localized vs. Generalized (Anasarca).
⭐ Pitting edema is characteristic of edema fluid rich in protein-poor interstitial fluid, typically seen in cardiac or renal failure.
Hyperemia & Congestion - Red Alert States
- Hyperemia: Active process. Arteriolar dilation → ↑ inflow. Tissue red (erythema) with oxygenated blood. E.g., inflammation, exercise.
- Congestion: Passive process. Impaired venous outflow → ↑ volume. Tissue blue-red (cyanotic) from deoxygenated Hb.
- Systemic: Cardiac failure.
- Localized: Venous obstruction.
- Chronic Passive Congestion: Chronic hypoxia → cell death, scarring, hemosiderin macrophages.
- Lungs: "Heart failure cells" (hemosiderin-laden alveolar macrophages).
- Liver: "Nutmeg liver" (centrilobular congestion & necrosis).
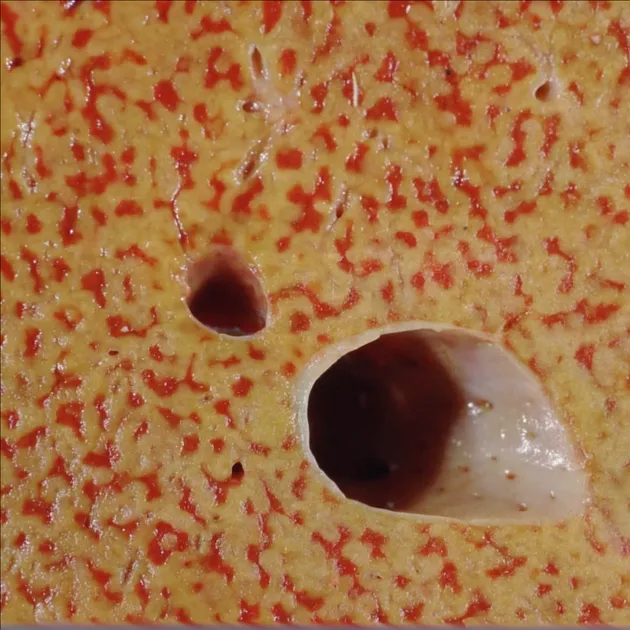
⭐ Nutmeg liver is the classic gross appearance of chronic passive hepatic congestion, often due to right-sided heart failure.
Thrombosis & Embolism - Clot Chronicles & Traveling Troubles
- Thrombosis: Pathological intravascular clot (thrombus) formation.
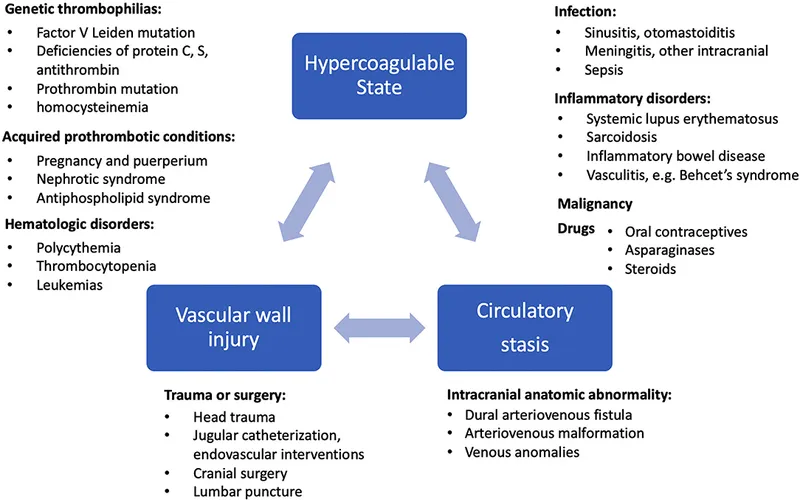
- 📌 Virchow's Triad: Stasis, Hypercoagulability, Endothelial injury.
- Types: Arterial (platelet-rich, pale; e.g., coronary, cerebral arteries); Venous (fibrin-rich, red; e.g., DVT).
- Fate of Thrombus:
⭐ Lines of Zahn (grossly and microscopically visible laminations of pale platelets/fibrin alternating with darker RBC-rich layers) are a hallmark of antemortem thrombi, distinguishing them from postmortem clots.
- Embolism: Detached intravascular solid, liquid, or gaseous mass (embolus) carried by blood to a site distant from its origin.
- Pulmonary Embolism (PE): >95% originate from deep leg vein DVT; can cause sudden death, right ventricular failure.
- Systemic Embolism: 80% arise from intracardiac mural thrombi; lodge in lower extremities (75%), brain (10%), viscera.
- Other types: Fat (long bone fractures), Air (decompression sickness, iatrogenic), Amniotic fluid (labor complication).
Infarction & Shock - Tissue Death & Systemic Shutdown
-
Infarction: Ischemic necrosis from occluded blood supply.
- Coagulative necrosis (most tissues); liquefactive (brain).
- Types:
- Red (hemorrhagic): Venous occlusion, loose tissues (lung, gut), dual circulation, reperfusion injury.
- White (anemic): Arterial occlusion in solid organs (heart, kidney, spleen).
- Influenced by: Vascular anatomy, occlusion rate, tissue hypoxia sensitivity.
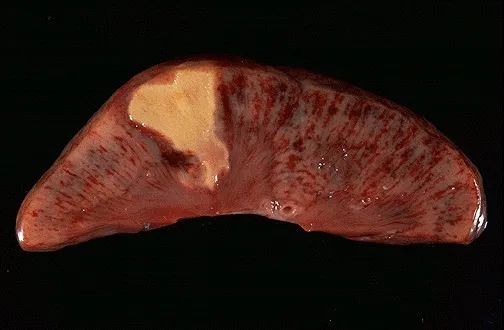
-
Shock: Systemic hypoperfusion leading to cellular hypoxia & vital organ dysfunction.
- Types:
- Cardiogenic: Myocardial pump failure (e.g., MI, arrhythmia).
- Hypovolemic: Reduced circulating blood volume (e.g., hemorrhage, severe dehydration).
- Distributive: Widespread vasodilation.
- Septic: Systemic microbial infection.
⭐ Septic shock is most commonly caused by gram-positive bacteria, followed by gram-negative bacteria and fungi, and is characterized by systemic vasodilation and endothelial injury.
- Neurogenic: Loss of vascular tone (e.g., spinal cord injury).
- Anaphylactic: Systemic hypersensitivity reaction.
- Septic: Systemic microbial infection.
- Obstructive: Mechanical obstruction to cardiac filling or outflow (e.g., pulmonary embolism, cardiac tamponade).
- Stages of Shock:
- Types:
High‑Yield Points - ⚡ Biggest Takeaways
- Virchow's triad (endothelial injury, abnormal blood flow, hypercoagulability) is crucial for thrombosis.
- Pulmonary embolism (PE) most often originates from deep vein thrombosis (DVT).
- Lines of Zahn distinguish ante-mortem thrombi.
- Septic shock is driven by LPS, causing vasodilation and organ dysfunction.
- Red infarcts in dual-supply organs (lung); white infarcts in end-arterial organs (heart, kidney).
- Edema mechanisms: ↑ hydrostatic pressure, ↓ oncotic pressure, lymphatic blockage, Na+ retention.
- DIC features widespread microthrombi and subsequent bleeding_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

