Acute Appendicitis - Inflamed & Irate
- Etiology: Luminal obstruction. Common causes: fecalith (adults), lymphoid hyperplasia (children), carcinoid, parasites.
- Pathogenesis Flow:
- Clinical Features:
- Pain: Periumbilical (visceral) → RIF (somatic, McBurney's point).
- Systemic: Anorexia, Nausea/Vomiting, low-grade Fever.
- Signs: Localized RIF tenderness, Rebound tenderness, Guarding. Special signs: Rovsing's, Psoas, Obturator.
- Diagnosis:
- Alvarado Score (📌 MANTRELS) aids: Score ≥7 high probability.
- (M:Migration, A:Anorexia, N:N/V, T:Tenderness RIF, R:Rebound, E:↑Temp(>37.3°C), L:Leukocytosis(>10,000/μL), S:Shift to left(>75%))
- Labs: ↑WBC (neutrophilic leukocytosis), ↑CRP.
- Imaging: USG (appendix >6mm diameter, non-compressible, wall thickening, target sign); CT (most accurate: fat stranding, complications).
- Alvarado Score (📌 MANTRELS) aids: Score ≥7 high probability.
- Pathology (Gross & Micro):
- Gross: Swollen, erythematous, dull serosa; fibrinopurulent exudate.
- Micro:
⭐ Neutrophilic infiltration of the muscularis propria is the pathognomonic histological hallmark.
- Edema, vascular congestion, mucosal ulceration, transmural inflammation and necrosis.
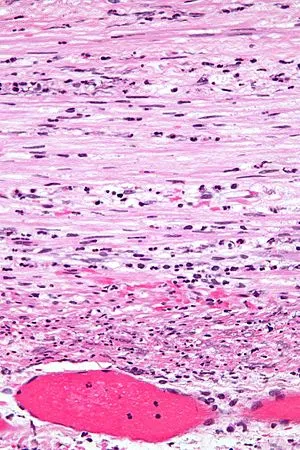
- Edema, vascular congestion, mucosal ulceration, transmural inflammation and necrosis.
- Complications: Perforation, peritonitis (localized/generalized), appendiceal abscess/phlegmon, pylephlebitis.
Appendiceal Neoplasms - Sneaky Surprises
- Often incidental; may mimic appendicitis or present as mass/PMP.
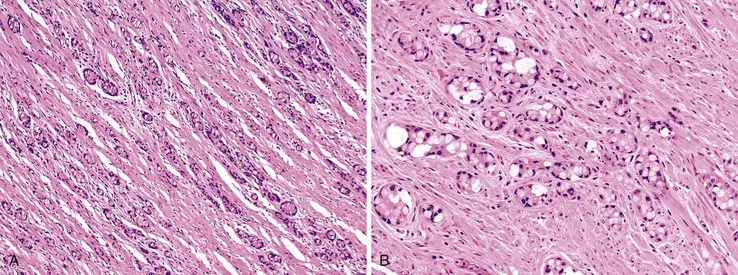
- Neuroendocrine Tumors (NETs/Carcinoids)
- Most common; often at appendix tip.
- Size critical: <1cm excellent prognosis; <2cm & no mesoappendiceal invasion usually benign course.
- Markers: Chromogranin A, Synaptophysin.
- Mucinous Neoplasms
- Spectrum: LAMN → HAMN → Mucinous Adenocarcinoma.
- Low-Grade Appendiceal Mucinous Neoplasm (LAMN):
- Bland cells, pushing border; risk of Pseudomyxoma Peritonei (PMP) if ruptured.
- High-Grade Appendiceal Mucinous Neoplasm (HAMN): More atypical cells, higher risk.
- Mucinous Adenocarcinoma: Invasive, desmoplastic, poorer prognosis.
- Goblet Cell Adenocarcinoma (GCA)
- Aggressive; mixed glandular & neuroendocrine features. 📌 "Goblet cells gone rogue: a dangerous duo."
- Pseudomyxoma Peritonei (PMP)
- "Jelly belly" from mucinous ascites, often due to ruptured appendiceal mucinous neoplasm (esp. LAMN).
- Non-Mucinous Adenocarcinoma
- Colonic-type adenocarcinoma; generally poorer prognosis than NETs.
⭐ Appendiceal NETs <2cm without mesoappendiceal invasion are often cured by appendectomy alone.
Mucocele & Other Lesions - Appendix Oddities
- Mucocele: Grossly dilated appendix, mucin-filled.
- Types:
- Simple Mucocele: Obstruction (e.g., fecalith).
- Mucinous Hyperplasia: No atypia.
- Mucinous Cystadenoma: Benign, low-grade atypia.
- Mucinous Cystadenocarcinoma: Malignant, invasive.
- Risk: Rupture → Pseudomyxoma Peritonei (PMP) - gelatinous peritoneal material.
⭐ PMP: Gelatinous ascites from ruptured appendiceal mucinous neoplasms (LAMN/cystadenocarcinoma).
- Types:
- Neuroendocrine Tumors (NETs/Carcinoids):
- Most common appendiceal tumor, often at tip.
- Often incidental. Good prognosis if < 2 cm, non-angioinvasive, no meso-extension.
- Markers: Chromogranin A, Synaptophysin.

- Adenocarcinoma:
- Rare, aggressive, colonic type.
- Lymphoma:
- Rare, usually Non-Hodgkin Lymphoma (NHL).
- Diverticulosis/Diverticulitis:
- Acquired outpouchings; inflammation can mimic appendicitis.
High‑Yield Points - ⚡ Biggest Takeaways
- Acute appendicitis, the most common cause of acute surgical abdomen, is typically due to luminal obstruction (e.g., fecalith, lymphoid hyperplasia).
- Key signs include periumbilical pain migrating to the RIF (Right Iliac Fossa) and McBurney's point tenderness.
- Major complications are perforation, leading to peritonitis, and appendiceal abscess formation.
- Neuroendocrine tumors (NETs/Carcinoids) are the most common appendiceal neoplasms, usually found incidentally at the tip.
- Appendiceal mucocele (dilatation by mucin) can be benign or malignant; rupture of a mucinous neoplasm can cause pseudomyxoma peritonei (PMP).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more