Basal Cell Carcinoma - The Pearly Peril
- Epidemiology: Most common malignant skin tumor.
- Pathogenesis: Associated with mutations in PTCH1 gene, leading to aberrant Hedgehog pathway signaling.
- Clinical Features: Typically a pearly papule or nodule, often with telangiectasias, a rolled border, and potential central ulceration (rodent ulcer).
- Histopathology: Shows nests of basaloid cells with characteristic peripheral palisading of nuclei and stromal retraction artifact.

- Common Variants: Nodular (most frequent), superficial, morpheaform, infiltrative.
- Prognosis: Locally invasive growth pattern; however, metastatic potential is very low.
⭐ Gorlin syndrome (Nevoid Basal Cell Carcinoma Syndrome) is associated with multiple BCCs from a young age due to germline PTCH1 gene mutations.
Squamous Cell Carcinoma & Precursors - Scaly Invaders
- Precursors:
- Actinic Keratosis (AK): sandpaper feel, sun-exposed.
- Bowen's Disease (SCC in situ): erythematous patch.
- Leukoplakia: mucosal white patch.
- Risk Factors: 📌 Sun (UV - primary), Scars (chronic inflammation, Marjolin's ulcer), Suppression (immuno-), Arsenic, HPV. TP53 mutations common.
- Clinical: Indurated, erythematous, scaling/crusted papules/plaques; ulceration, cutaneous horn.
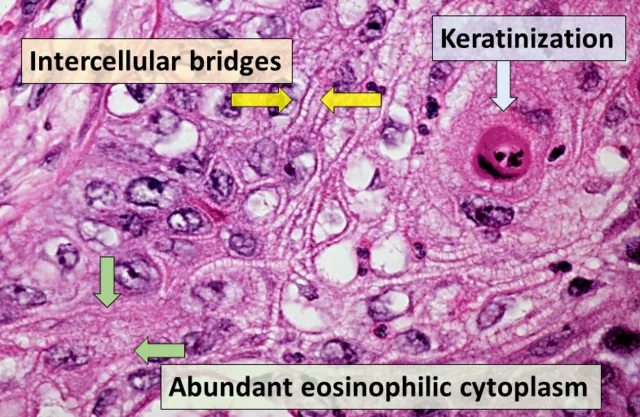
- Histopathology: Invasive atypical squamous cell nests; pleomorphism, keratin pearls, intercellular bridges (desmosomes).
- Grading: Well, moderately, poorly differentiated.
⭐ Marjolin's ulcer (SCC in chronic wounds/scars) is more aggressive with higher metastatic potential.
Malignant Melanoma - The Dark Danger
Highest mortality of common skin cancers. Risk factors: UV (intense, intermittent), fair skin, multiple/dysplastic nevi, family hx, CDKN2A, BRAF mutations.
-
Clinical Recognition: 📌 ABCDE criteria:
- Asymmetry
- Border irregularity
- Color variegation
- Diameter >6mm
- Evolving lesion

-
Key Histopathological Types:
- Superficial Spreading: Most common, radial growth.
- Nodular: Aggressive, vertical growth, poorer prognosis.
- Lentigo Maligna: Elderly, sun-damaged skin.
- Acral Lentiginous: Palms/soles/subungual, darker skin.
-
Prognosis & IHC:
- Most important: Breslow thickness (depth in mm).
- Others: Ulceration, mitotic rate, Clark level (less used), LN status.
- IHC: S-100, HMB-45, Melan-A, SOX10.
⭐ Breslow thickness, measured in millimeters from the granular layer of the epidermis to the deepest point of tumor invasion, is the single most important prognostic factor in malignant melanoma.
Other Tumors & Syndromes - Rare But Real Threats
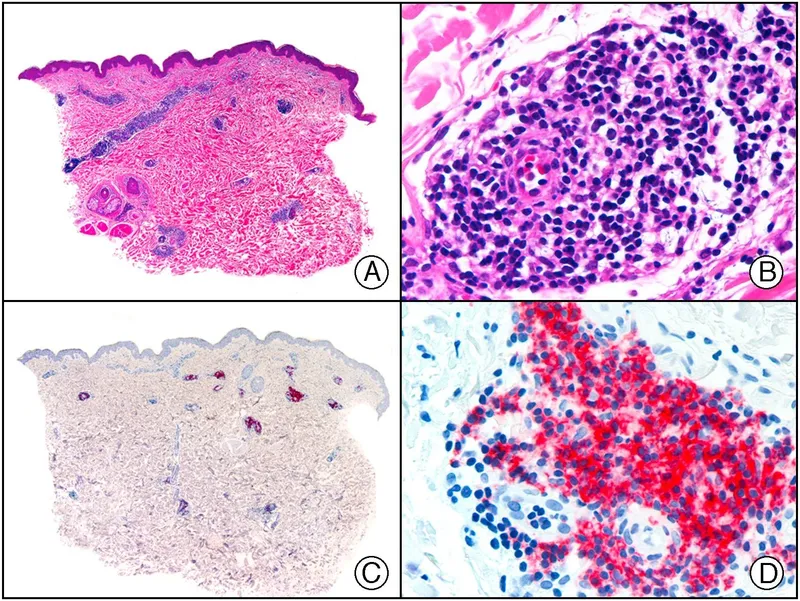
- Merkel Cell: Aggressive, MCPyV.
⭐ Merkel cell carcinoma is characterized by perinuclear dot-like staining for Cytokeratin 20 (CK20) on immunohistochemistry.
- DFSP: Locally aggressive, COL1A1-PDGFB, storiform.
- CTCL: MF (Pautrier's), Sézary.
- XP: AR, NER defect, photosensitive, ↑Ca.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Basal Cell Carcinoma (BCC): Most common skin cancer, presents as a pearly papule with telangiectasias; histology shows peripheral palisading of nuclei and stromal retraction.
- Squamous Cell Carcinoma (SCC): Arises from actinic keratosis or de novo; characterized by keratin pearls and intercellular bridges (desmosomes).
- Malignant Melanoma: Deadliest form, remember ABCDE criteria; key markers include S-100 and HMB-45; Breslow thickness is the most important prognostic factor.
- Mycosis Fungoides: Most common cutaneous T-cell lymphoma; features Pautrier's microabscesses (collections of atypical lymphocytes in epidermis) and cerebriform Sézary cells.
- Kaposi Sarcoma: Associated with HHV-8; presents as violaceous plaques/nodules; histology shows spindle cell proliferation, vascular slits, and extravasated RBCs, common in AIDS.
- Merkel Cell Carcinoma: Rare, aggressive neuroendocrine skin tumor; positive for cytokeratin 20 (CK20) with a perinuclear dot-like pattern and neuroendocrine markers (e.g., synaptophysin).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more