QA Fundamentals - Setting the Stage
- Core Aim: Guaranteeing accuracy, reliability, & reproducibility in cytological diagnoses for superior patient management.
- Significance:
- Crucial for patient safety; ↓ diagnostic errors (false positives/negatives), preventing misdiagnosis.
- Upholds high laboratory standards & consistency.
- Essential for accreditation (e.g., NABL in India).
- Comprehensive Process: Covers all phases:
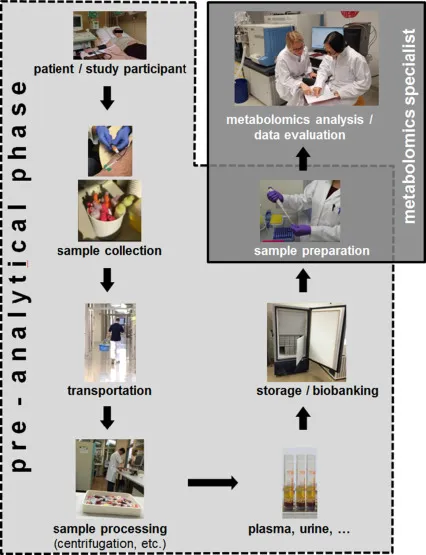
- Pre-analytical: Specimen collection, handling, adequacy.
- Analytical: Staining, screening accuracy, interpretation.
- Post-analytical: Reporting, record-keeping, corrective actions.
- Foundation: Fostering a culture of quality and accountability through Continuous Quality Improvement (CQI).
⭐ QA in cytopathology significantly focuses on reducing the false negative rate, especially critical in screening programs like Pap smears for cervical cancer.
Pre & Post Analytics - Bookends of Quality
Quality in cytopathology hinges on robust pre-analytical and post-analytical processes, minimizing errors and ensuring diagnostic accuracy.
- Pre-analytical Phase (Foundation):
- Patient/Specimen ID: CRITICAL, use ≥2 identifiers.
- Request Form: Complete clinical data (history, site).
- Collection: Proper technique, adequate material, correct fixative (e.g., 95% Ethanol for Pap; 50% for fluids).
- Transport: Timely, appropriate conditions to prevent degradation.
- Accessioning: Unique lab number, error check.
- Post-analytical Phase (Completion & Feedback):
- Reporting: Standardized terminology (e.g., Bethesda), clarity, TAT (<3-5 days for routine).
- Delivery: Secure, to correct clinician.
- Archiving: Slides (5-10 years), reports (20+ years).
- Error Review: Root Cause Analysis (RCA) for discrepancies.
- Clinico-Pathological Correlation (CPC): Essential for continuous improvement.
⭐ The majority (up to 70%) of errors in laboratory medicine, including cytopathology, occur in the pre-analytical phase.
Analytical Phase - Microscope & Mind
- Microscopy & Interpretation:
- Standardized criteria (e.g., Bethesda).
- Systematic screening; adequacy check.
- Screening & QC:
- Primary screening: Cytotechnologist (CT).
- Rapid On-Site Evaluation (ROSE) by pathologist.
- QC: 10% random rescreen (negative GYN); targeted rescreen (high-risk).
- Workload & TAT:
- Max: 80 GYN slides/day/CT (IAPM); 100 slides/24h (CLIA).
- Monitor Turnaround Time; report critical values.
- Consultation & Peer Review:
- Second opinions for difficult/equivocal cases.
- Multi-headed scope: training, consensus.
- Proficiency Testing (PT):
- Mandatory for GYN screeners (annual).
- Min. 90% passing score (individual).
- Cytology-Histology Correlation (CHC):
- Essential QA: Cytology vs. biopsy.
- Discrepancy analysis; improves accuracy. 📌 Mnemonic: "Cy-Hi" Check!

⭐ Workload Limit: IAPM: max 80 GYN smears/day/CT. CLIA '88: 100 slides (any type)/8h per individual.
QA Metrics & Tools - Numbers Don't Lie
- KPIs: Track lab performance & identify improvement areas.
- Turnaround Time (TAT): Monitor sample processing efficiency.
- Adequacy Rates: E.g., Unsatisfactory Pap smears ideally < 1%.
- Error Rates:
- False Negative Rate (FNR): $FNR = FN / (FN + TP)$
- False Positive Rate (FPR): $FPR = FP / (FP + TN)$
- ASCUS/SIL Ratio: Target range 2:1 to 3:1.
⭐ The ASCUS/SIL ratio is a key indicator for monitoring diagnostic thresholds in cervical cytology, helping prevent over/under-diagnosis.
- Rescreening: E.g., 10% random rescreening of negative gynecologic smears.
- Proficiency Testing (PT): Mandatory external quality assessment participation.
- Cytotechnologist Workload Limits: E.g., Max 100 slides/24 hrs (as per CLIA '88, often adapted).
High‑Yield Points - ⚡ Biggest Takeaways
- Turnaround Time (TAT) and specimen adequacy are critical for diagnosis.
- Rescreening covers 10% random negative smears and all high-risk/discrepant cases.
- Cyto-histo correlation is mandatory for validating diagnostic accuracy.
- Participation in Proficiency Testing/EQAS is essential for quality assessment.
- Systematic error documentation with Root Cause Analysis (RCA) drives improvement.
- Laboratory accreditation (e.g., NABL) ensures adherence to quality standards.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

