Cervical Screening & Sampling - The First Look
- Pap Smear Types:
- Conventional: Direct smear.
- Liquid-Based Cytology (LBC): Cells in preservative, processed.
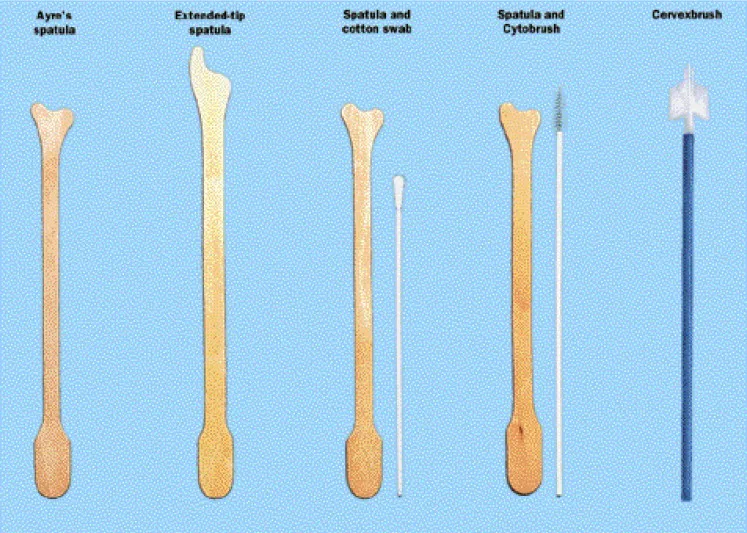
- Sampling Tools:
- Ayre Spatula: Ectocervix.
- Cytobrush: Endocervix.
- Cervex-Brush (Combi): Ecto- & endocervix.
- Fixation: Immediate 95% ethanol or spray fixative.
- Adequacy (Bethesda): ≥ 5,000 squamous cells; endocervical/transformation zone (EC/TZ) component present.
⭐ LBC reduces obscuring elements like blood and mucus, improving sensitivity and allowing ancillary testing (e.g., HPV DNA).
Benign & Reactive Changes - Not Always Scary
-
Normal Cells: Squamous (superficial, intermediate, parabasal), endocervical, endometrial.
-
Reactive Changes: Inflammation (PMNs, lymphocytes), repair, atrophy.
-
Common Infections:
Organism Key Features Candida Pseudohyphae, spores Trichomonas Pear-shaped, flagella Gardnerella Clue cells (bacteria obscuring cell borders) Actinomyces "Sulfur granules" (dense bacterial colonies) HSV 📌 3 M's: Multinucleation, Molding, Margination HPV Koilocytes (perinuclear halo, nuclear atypia)

⭐ Koilocytic atypia, characterized by nuclear atypia and a perinuclear halo, is pathognomonic for HPV infection.
Bethesda System - Decoding Reports
The Bethesda System (TBS) 2014 standardizes gynecologic cytology reporting.
- Specimen Adequacy: Assesses sample quality.
- Satisfactory for evaluation: Requires endocervical/transformation zone (EC/TZ) component. Minimum 5,000 cells (LBC), 8,000-12,000 (conventional).
- Unsatisfactory for evaluation: Reasons provided (e.g., scant cellularity, obscuring factors).
- General Categorization: Main diagnostic groups.
⭐ Presence of an adequate endocervical/transformation zone (EC/TZ) component is crucial for a satisfactory Pap smear.
Squamous Abnormalities - SILs & Squawks
| Category | N/C Ratio | Chromatin | Nuclear Membrane | Cell Shape / Other |
|---|---|---|---|---|
| ASC-US | Sl. ↑ | Fine | Smooth | Superficial/Intermediate; Atypia, not LSIL/HSIL |
| ASC-H | ↑ (>0.5) | Fine/Coarse | Smooth/Irregular | Smaller, metaplastic-like; Cannot exclude HSIL |
| LSIL | ↑ (often <0.5) | Fine, smudged | Smooth/Irregular | Superficial/Intermediate; Koilocytosis (HPV), CIN 1 |
| HSIL | ↑↑ (>0.7) | Coarse, hyper | Irregular | Smaller, round/oval; CIN 2/3, CIS |

⭐ p16INK4a immunostain is typically positive in HSIL, aiding differentiation from mimics such as reactive changes or atrophy.
Glandular Abnormalities - Glands Gone Rogue
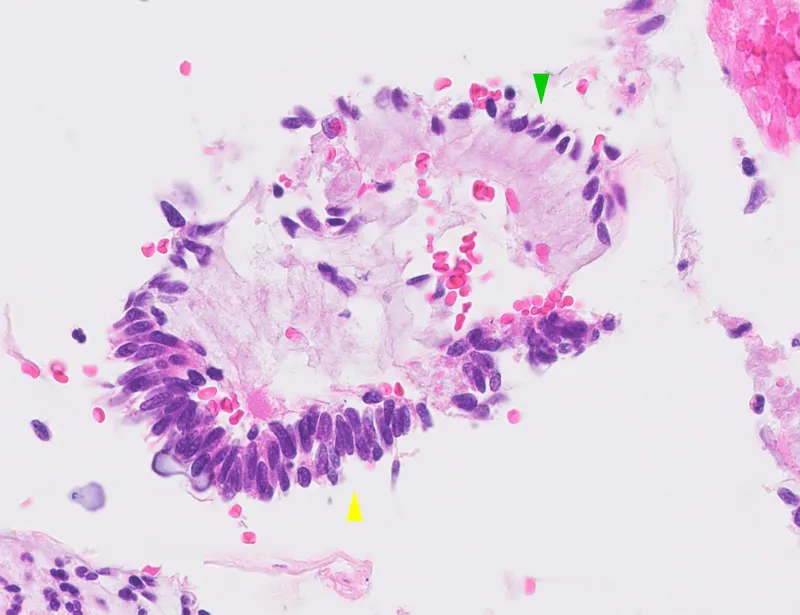
⭐ "Feathering", elongated nuclei, and pseudostratification are characteristic features of Endocervical Adenocarcinoma In Situ (AIS).
| Category | Key Cytomorphologic Features |
|---|---|
| AGC-NOS | Cell crowding, nuclear overlap, mild atypia. (Endocervical/Endometrial origin) |
| AGC-FN | ↑Crowding/overlap, significant atypia; rosettes, feathering suggestive of neoplasia. |
| AIS | Feathering, rosettes, pseudostratification, elongated hyperchromatic nuclei. |
| Adeno-Ca | 3D clusters, single cells, macronucleoli, tumor diathesis. (Endocervical/Endometrial/Extrauterine) |
Management Pathways - Charting the Course
⭐ For women with ASC-US, HPV DNA testing is the preferred management approach to triage for colposcopy.
High‑Yield Points - ⚡ Biggest Takeaways
- Bethesda System (TBS) is crucial for reporting cervical cytology.
- High-risk HPV (16, 18) are major causes of cervical cancer.
- Koilocytes (perinuclear halo, nuclear atypia) are pathognomonic for HPV.
- LSIL often regresses; HSIL carries significant risk of progression to invasive cancer.
- ASC-US is the most common abnormality; requires HPV testing or repeat cytology.
- AGC (Atypical Glandular Cells) necessitates evaluation for endocervical or endometrial lesions.
- Conventional Pap smears and Liquid-Based Cytology (LBC) are primary screening tools.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

