GIT Cytology: Basics - Scope & Smears
- Scope: Rapid diagnosis: neoplasia, inflammation, infections (H. pylori, CMV, Candida). Guides therapy.
- Specimen Types:
- Exfoliative: Brushings (esophagus, stomach, bile duct), washings, ERCP-guided.
- Aspiration: FNA (palpable/intraop), EUS-FNA (deep lesions: pancreas, LNs - gold standard).
- Smear Prep: Direct (quick), Cytospin (concentrates cells), Liquid-Based Cytology (LBC - uniform, less debris).
- Stains: Pap (nuclear detail), MGG/Diff-Quik (cytoplasmic, matrix), special (PAS-mucin, Grocott-fungi).
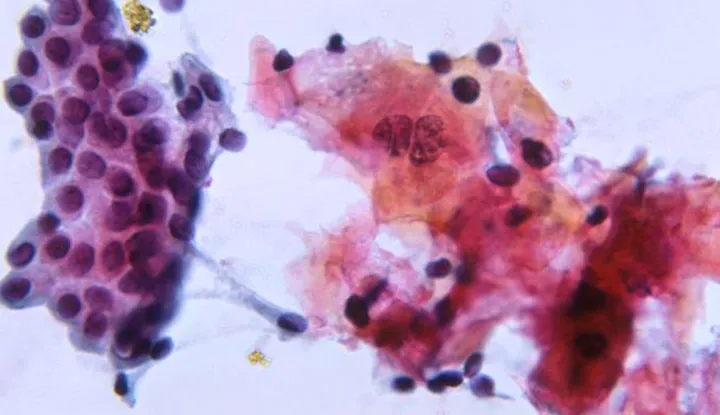
⭐ EUS-FNA offers high diagnostic yield (>85% sensitivity, >95% specificity) for solid pancreatic lesions.
Esophageal Cytology: Lesions - Gullet Gazing
- Normal Cells: Predominantly superficial squamous cells; few parabasal/intermediate.
- Benign Conditions:
- Infections:
- Candida: Pseudohyphae, budding yeasts. Inflammatory background.
- HSV: 📌 3 'M's (Multinucleation, Molding, Margination), Cowdry type A inclusions.
- CMV: Large cells with "owl's eye" intranuclear inclusions; granular cytoplasmic inclusions.
- Reflux Esophagitis: Neutrophils, eosinophils, reactive squamous atypia, parakeratosis.
- Barrett's Esophagus: Intestinal metaplasia: presence of goblet cells. Precursor to adenocarcinoma.
⭐ Goblet cells are the diagnostic hallmark of Barrett's esophagus, indicating intestinal metaplasia.
- Infections:
- Malignant Tumors:
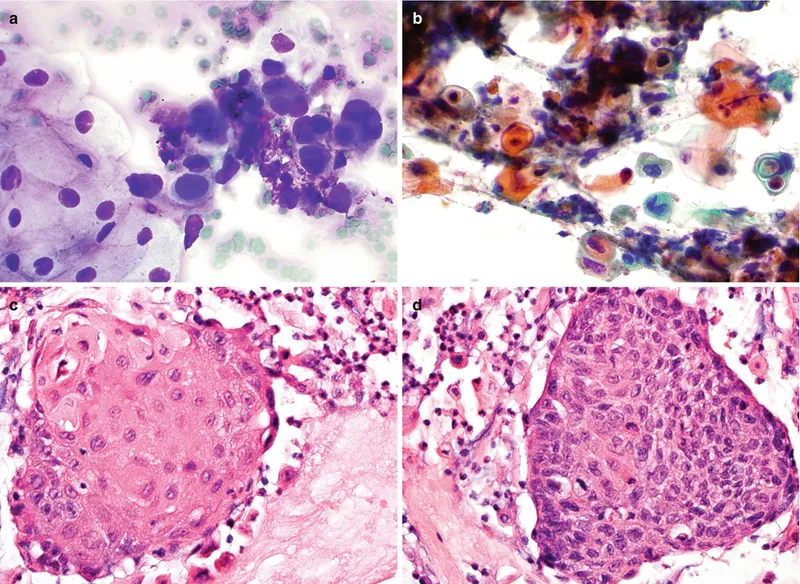
- Squamous Cell Carcinoma (SCC):
- Cellular smears; pleomorphic squamous cells (single/clusters).
- Irregular, hyperchromatic nuclei, ↑N/C ratio.
- Keratinization (dense orangeophilic cytoplasm), "tadpole" or "fiber" cells. Tumor diathesis.
- Adenocarcinoma (AdenoCa):
- Glandular clusters, acini, or papillae.
- Pleomorphic columnar cells, vacuolated cytoplasm, prominent nucleoli.
- Signet ring cells may be present. Typically arises from Barrett's.
- Squamous Cell Carcinoma (SCC):
Gastric Cytology: Findings - Stomach Stories
- Normal Gastric Cells:
- Superficial columnar: Honeycomb sheets, bland nuclei.
- Deep glandular: Smaller, rounder, tight clusters.
- Inflammation & Reactive Changes:
- Neutrophils, lymphocytes, plasma cells.
- Nuclear enlargement, prominent nucleoli, reparative atypia.
- Helicobacter pylori: Curved/S-shaped bacilli on mucus or epithelial surface.
- Intestinal Metaplasia:
- Presence of goblet cells (key diagnostic feature).
- +/- Brush border.
- Dysplasia (Pre-malignant):
- ↑ N/C ratio, hyperchromasia, irregular nuclear membranes, pleomorphism.
- Loss of cellular polarity, architectural disarray.
- Graded: Low-grade (LGD) vs. High-grade (HGD).
- Gastric Adenocarcinoma:
- Intestinal type: Glandular/acinar structures, pleomorphic cells, dirty necrotic background.
- Diffuse type (Signet-ring cell carcinoma): Discohesive cells, large intracytoplasmic mucin vacuole pushing nucleus to periphery.
- MALT Lymphoma:
- Monotonous population of small to medium-sized atypical lymphocytes.
- Lymphoepithelial lesions (infiltrating glands).
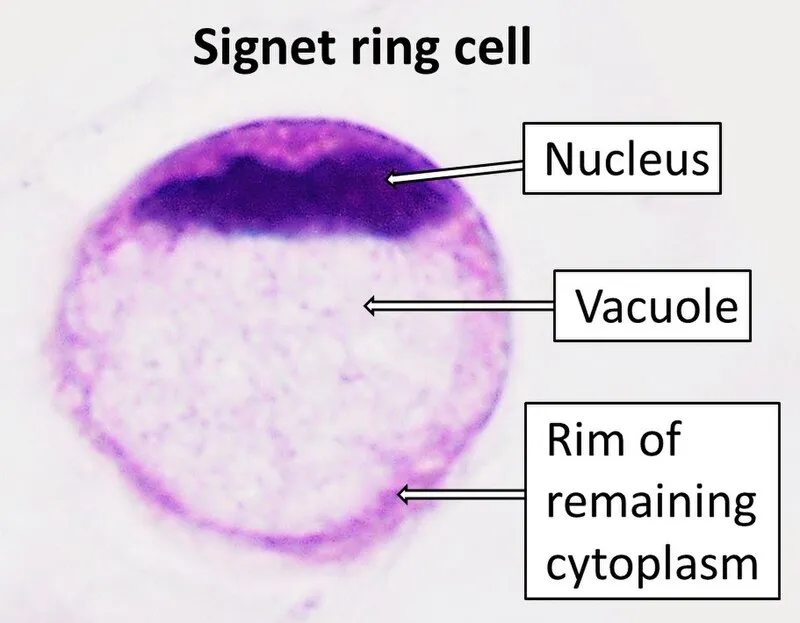
⭐ > Signet-ring cells in gastric cytology, with their eccentric nucleus and mucin-filled cytoplasm, are a hallmark of diffuse-type gastric adenocarcinoma, often associated with linitis plastica.
Pancreato-Biliary Cytology: FNA & Brushings - Deep Dive Diagnostics
- Sampling: Endoscopic Ultrasound-guided FNA (EUS-FNA) for pancreas; Endoscopic Retrograde Cholangiopancreatography (ERCP)-brushings/FNA for biliary tree.
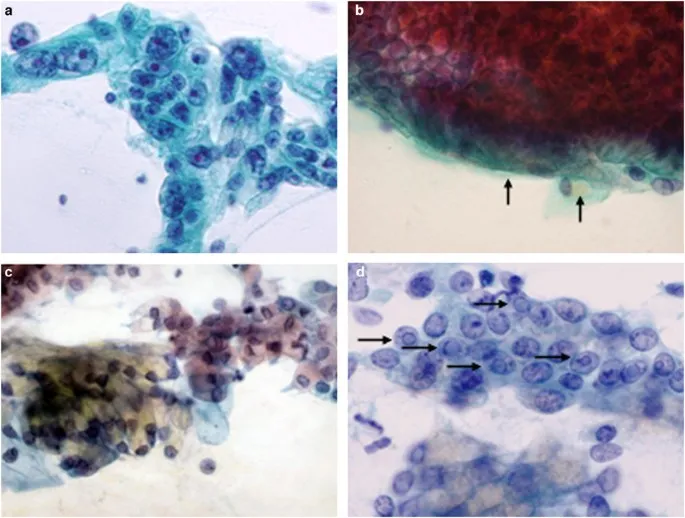
- Pancreatic Ductal Adenocarcinoma (PDAC):
- Cellular smears: 3D clusters, single malignant cells.
- Nuclear atypia: Pleomorphism, irregular membranes, prominent nucleoli, hyperchromasia.
- Often mucinous background.
- 📌 Mnemonic: "Pancreatic Pleomorphism, Prominent nucleoli".
- Cholangiocarcinoma:
- Atypical glandular cells: Sheets, clusters, or single cells.
- Nuclear features: Crowding, hyperchromasia, irregular contours.
- Often less cellular & pleomorphic than PDAC.
- Other Lesions:
- Pancreatic Neuroendocrine Tumors (PNETs): Plasmacytoid cells, "salt-and-pepper" chromatin.
- Cystic lesions (e.g., IPMN, MCN): Mucin, variable epithelial atypia.
- Challenges: Differentiating reactive atypia from low-grade malignancy.
⭐ KRAS mutations are detected in >90% of pancreatic ductal adenocarcinomas and can be assessed on cytology samples.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Barrett's esophagus: goblet cells confirm intestinal metaplasia in esophageal samples.
- H. pylori: identifiable in gastric cytology, linked to gastritis and ulcers.
- Gastric adenocarcinoma: features signet ring cells, high N:C ratio, nuclear atypia.
- Esophageal SCC: shows keratinization, pleomorphism, and orangeophilic cytoplasm.
- GISTs: spindle cells and CD117 (c-KIT) positivity are diagnostic hallmarks.
- NETs: "salt and pepper" chromatin; positive for synaptophysin & chromogranin.
- Viral cytopathy: CMV (owl's eye inclusions), HSV (multinucleation, molding).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

