FNAC Fundamentals - Point & Shoot
- Definition: Diagnostic procedure using a fine needle to aspirate cells from a lesion for microscopic examination.
- Principle: Cellular material obtained by suction through a needle, smeared on a slide, stained, and evaluated.
- Advantages: 📌 S.A.F.E.R - Simple, Accurate, Fast, Economical, Reliable. Minimally invasive.
- Disadvantages: Sampling error (may miss lesion), no tissue architecture, operator dependent.
- Indications: Palpable lesions (thyroid, breast, lymph nodes), image-guided for deep lesions (lung, liver).
- Contraindications: Severe bleeding diathesis, uncooperative patient, overlying infection (relative).
⭐ FNAC is a rapid, minimally invasive, and cost-effective diagnostic tool, often the first line of investigation for palpable masses.
FNAC Workflow - Poke, Smear, Stain
1. Poke (Aspiration):
- Needle: Typically 22-25 gauge; length varies.
- Syringe: 10-20 ml, often pistol grip for single-hand operation.
- Techniques:
- Suction: using syringe for negative pressure.
- Non-aspiration (Zajdela/capillary technique): uses capillary action of fine needle.
2. Smear (Slide Preparation):
- Expel material onto slide.
- Methods:
- Direct smear.
- Pull-apart/slide-over-slide (common).
- Crush: for cellular/fragmented material.

3. Stain (Fixation & Staining):
- Fixation & Stains:
- Air-drying: For Romanowsky (e.g., MGG, Giemsa); highlights cytoplasm, matrix.
- Wet fixation: 95% ethanol for Papanicolaou (Pap - nuclear detail, keratin) & H&E (general morphology).
⭐ The choice of fixation and staining (Air-dried/Romanowsky vs. Alcohol-fixed/Pap) depends on the suspected diagnosis and institutional preference, each highlighting different cellular features.
FNAC Procedure Flowchart:
Cytological Interpretation - Decoding the Cells
- Specimen Adequacy:
- Sufficient cellularity
- Presence of diagnostic cells
- Absence of obscuring elements (blood, clot)
- General Cytomorphological Features:
- Background: Clean, bloody, inflammatory, necrotic
- Arrangement: Clusters, sheets, acini, papillary, single cells
- Cell: Size, shape
- Nucleus: N:C ratio, chromatin (fine/coarse), membrane (smooth/irregular), nucleoli (inconspicuous/prominent)
- Cytoplasm: Amount, color, granules, vacuoles, inclusions
- Criteria of Malignancy: 📌 Mnemonic: Ugly Nuclei
- Anisokaryosis/Pleomorphism
- Hyperchromasia
- Irregular nuclear contours
- Prominent/multiple nucleoli
- ↑ N:C ratio
- Abnormal mitoses
- Reporting Systems:
- Bethesda (Thyroid)
- Milan (Salivary Gland)
- IAC Yokohama (Breast)
- Paris (Urine)
⭐ Accurate interpretation requires assessing both individual cell morphology and the overall architectural pattern of cell groups, alongside clinical context.
Organ-Specific FNAC - Target Practice
- Thyroid:
- Hashimoto's: Lymphocytes, Hürthle cells.
- Papillary Ca: Nuclear grooves, intranuclear inclusions, psammoma bodies.
- General: Colloid, follicular cells.
- Lymph Node:
- Reactive Hyperplasia: Polymorphic lymphoid population.
- TB Lymphadenitis: Epithelioid granulomas, Langhans giant cells, caseous necrosis.
- Metastasis: Foreign cells.
- Breast:
- Fibroadenoma: Staghorn clusters of ductal cells, bipolar naked nuclei.
- Ductal Carcinoma: Cellular, discohesive malignant cells, pleomorphism.
- Salivary Gland:
- Pleomorphic Adenoma: Chondromyxoid stroma, epithelial/myoepithelial cells.
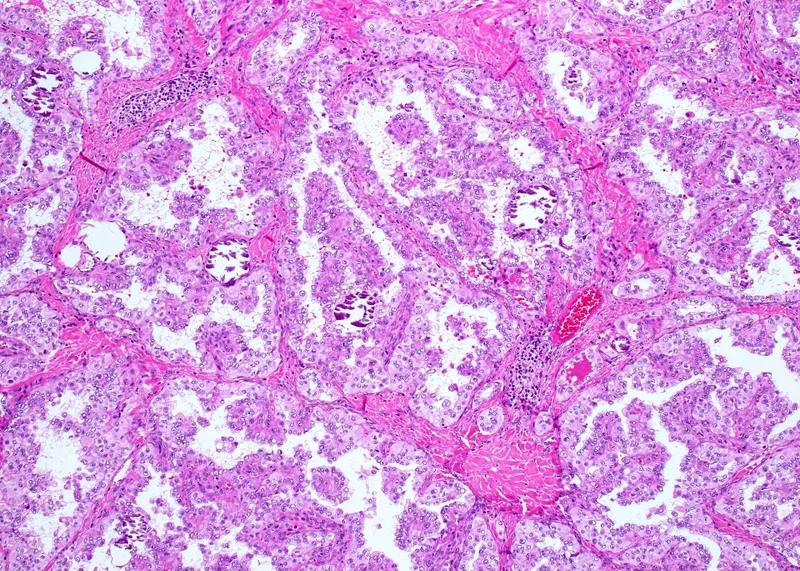
⭐ In thyroid FNAC, nuclear features like grooves, inclusions, and powdery chromatin are key to diagnosing Papillary Thyroid Carcinoma, even with scant cellularity.
High‑Yield Points - ⚡ Biggest Takeaways
- FNAC is a minimally invasive, cost-effective, and rapid diagnostic tool.
- Uses fine needles (typically 22-27 gauge) for cellular material aspiration.
- Key for evaluating palpable lesions: thyroid nodules, breast lumps, lymph nodes.
- Image guidance (USG/CT) is vital for non-palpable or deep-seated lesions.
- ROSE ensures sample adequacy, reducing need for repeat procedures.
- Effectively differentiates benign vs. malignant conditions, guiding management.
- Complications like hematoma are rare and generally minor.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

