Special Stains - Old School Cool
Special stains highlight specific cellular components, aiding diagnosis.
| Stain | Detects | Applications |
|---|---|---|
| PAS | Glycogen, neutral mucins | AdenoCa (mucin), fungi, glycogenoses |
| Mucicarmine | Epithelial mucin | AdenoCa (GIT, breast), signet cells |
| Oil Red O | Lipids (fresh) | Fat embolism, liposarcoma |
| Prussian Blue | Ferric iron ($Fe^{3+}$) | Hemosiderin, asbestos bodies |
| Alcian Blue | Acid mucins (pH specific) | Mesothelioma (pH 2.5), AdenoCa (pH 1.0) |
| Fontana-Masson | Melanin, argentaffin granules | Melanoma, neuroendocrine tumors |
oka
Immunocytochemistry - Antibody Avengers
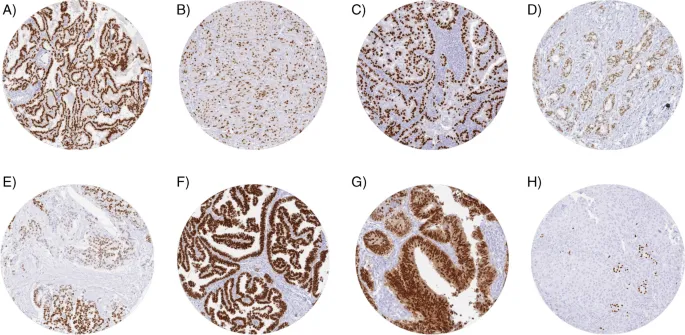
Principle: Specific antigen-antibody binding, visualized by chromogen or fluorescence. Essential for precise cell/tumor typing.
Common ICC Markers & Significance:
| Category | Markers | Key Use / Associations |
|---|---|---|
| Epithelial | Pan-CK, CK7, CK20, EMA, p63, p40 | Carcinomas |
| Mesenchymal | Vimentin, Desmin, SMA, S100 | Sarcomas; Melanoma, Neural (S100) |
| Neuroendocrine | Chromogranin, Synaptophysin, CD56 | Neuroendocrine Tumors (NETs), Small Cell Carcinoma |
| Lymphoid | LCA/CD45, CD20 (B), CD3 (T), MPO | Lymphomas, Leukemias |
| Site-Specific | TTF-1 (Lung/Thyroid), Napsin A (Lung), CDX2 (Colon), GATA3 (Breast/Uro), PAX8 (Renal/Ovary) | Metastasis workup |
| Proliferation | Ki-67 | Proliferative index (e.g., >20% often high grade) |
- Diagnosis: Differentiating poorly differentiated tumors (carcinoma vs sarcoma vs lymphoma).
- Subtyping tumors (e.g., adenocarcinoma vs squamous).
- Identify primary site of metastasis.
- Prognostic/Predictive markers (ER/PR, Her2/neu, PD-L1).
📌 CK7/CK20 Patterns:
- CK7+/CK20-: Lung, Breast, Gynae.
- CK7-/CK20+: Colorectal, Merkel.
- CK7+/CK20+: Urothelial, Pancreatobiliary.
Algorithm for Undifferentiated Tumors:
Pitfalls: Cross-reactivity, improper fixation, interpretation errors.
⭐ > A panel of Calretinin, WT-1, CK5/6 (+ve) and MOC-31, Ber-EP4, CEA (-ve) is characteristic for mesothelioma.
Molecular Diagnostics - Gene Genies
Error generating content for this concept group: Failed to process successful response
Flow Cytometry & Others - Cell Sorting & More
- Flow Cytometry (FC):
- Principle: Light scatter & fluorescence analysis of antibody-tagged cells in suspension.
- Applications: Immunophenotyping (leukemia/lymphoma in fluids, FNA); DNA ploidy (prognosis).
- Advantages: Rapid, quantitative, multi-parameter cell analysis.
- Limitations: Fresh/unfixed sample, viable cells needed; no architectural detail.
- Electron Microscopy (EM):
- Principle: Ultrastructural detail via electron beams.
- Uses: Limited; confirms neurosecretory granules, viruses, ciliary structures.
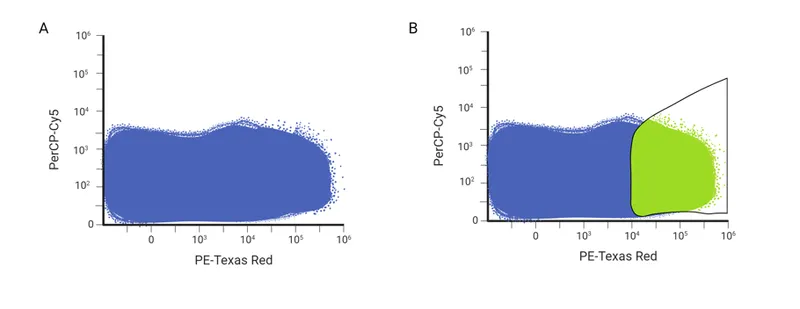
⭐ Flow cytometry: Gold standard for lineage & clonality in suspected lymphomas (FNA/fluids).
High‑Yield Points - ⚡ Biggest Takeaways
- Immunocytochemistry (ICC): Crucial for tumor typing, origin, and prognostic/predictive markers.
- Flow Cytometry: Key for leukemia/lymphoma diagnosis and classification from aspirates.
- Molecular Tests (FISH, PCR): Detect specific genetic alterations (translocations, mutations) for diagnosis/therapy.
- Cell Blocks: Provide tissue architecture; vital for multiple ancillary studies (ICC, molecular).
- Special Stains: Identify specific substances like mucin, glycogen, or microorganisms.
- Liquid-Based Cytology (LBC): Improves sample quality, enables multiple tests from one sample.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

