Cytopathology

On this page
🔬 Cytopathology: The Cellular Detective's Arsenal
Cytopathology transforms individual cells into diagnostic gold, teaching you to recognize disease at its most fundamental level before it declares itself through symptoms or imaging. You'll master the art of reading cellular architecture, distinguishing benign from malignant changes, and correlating microscopic findings with clinical decisions that directly shape patient outcomes. This lesson builds your pattern recognition skills systematically, from basic morphology through complex multi-system integration, equipping you to make rapid, confident diagnoses from fine needle aspirates, Pap smears, and body fluid specimens that guide everything from cancer staging to infection management.
Cytopathology transforms individual cells into diagnostic gold mines, where a single abnormal nucleus can reveal cancer, infection, or inflammatory processes. This cellular-level medicine demands mastery of morphological patterns, staining characteristics, and clinical correlations that guide patient management decisions.
📌 Remember: CYTOPATHOLOGY - Cells Yield Tremendous Opportunities for Precise Assessment Through Histological Observation, Leading to Optimal Guidance Yielding results. Each letter represents the systematic approach from specimen to diagnosis.
The field encompasses five major specimen categories: exfoliative cytology (cervical, respiratory, urinary), fine needle aspiration (thyroid, lymph nodes, soft tissue), effusion cytology (pleural, peritoneal, pericardial), cerebrospinal fluid analysis, and specialized body cavity sampling. Each category requires distinct collection techniques, processing protocols, and interpretive criteria.
- Exfoliative Cytology
- Cervical screening: 85% reduction in cancer mortality
- Respiratory specimens: 92% sensitivity for malignancy
- Sputum cytology: 3-5 samples required for optimal sensitivity
- Bronchial washings: higher cellular yield than brushings
- Fine Needle Aspiration (FNA)
- Thyroid nodules: 95% diagnostic accuracy when adequate
- Lymph node sampling: 90% concordance with histology
- Minimum 6 clusters of cells required for adequacy
- 22-25 gauge needles optimal for most sites
- Effusion Cytology
- Pleural fluid: 60% malignant when bloody and exudative
- Peritoneal washings: staging accuracy >90% in gynecologic cancers

⭐ Clinical Pearl: Nuclear-to-cytoplasmic ratio >1:2 strongly suggests malignancy, while uniform chromatin distribution indicates benign processes. This ratio assessment requires 400x magnification for accurate evaluation.
| Specimen Type | Collection Method | Processing Time | Diagnostic Yield | Clinical Application |
|---|---|---|---|---|
| Cervical | Liquid-based prep | 30 minutes | 95% adequate | Screening, HPV testing |
| Thyroid FNA | 25-gauge needle | 15 minutes | 90% diagnostic | Nodule evaluation |
| Pleural fluid | Thoracentesis | 45 minutes | 85% sensitivity | Malignancy detection |
| Sputum | Expectoration | 20 minutes | 70% sensitivity | Lung cancer screening |
| CSF | Lumbar puncture | 60 minutes | 95% specificity | CNS malignancy |
Understanding cellular morphology fundamentals unlocks the logic behind every cytological interpretation, setting the foundation for advanced pattern recognition that transforms microscopic observations into life-saving diagnoses.
🔬 Cytopathology: The Cellular Detective's Arsenal
⚙️ Cellular Architecture: The Morphological Command Center
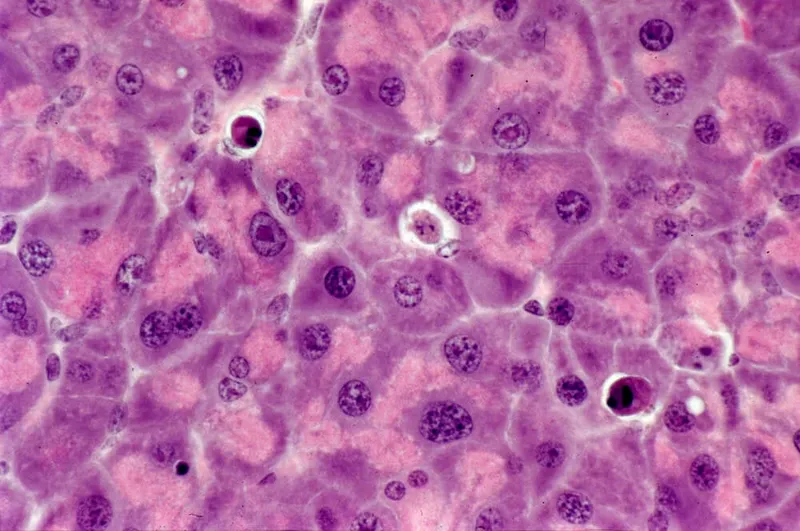
Cellular evaluation follows systematic morphological criteria that predict biological behavior and guide clinical management. Nuclear features provide 70% of diagnostic information, while cytoplasmic characteristics and architectural patterns contribute the remaining 30%. This hierarchical assessment ensures consistent interpretation across different pathologists and institutions.
📌 Remember: NUCLEAR assessment follows Nuclear size, Uniformity, Chromatin pattern, Leolation prominence, Enlargement ratio, Asymmetry detection, Roughness evaluation. Each parameter requires systematic evaluation at 400x magnification.
- Nuclear Morphology Assessment
- Size variation: >3-fold difference suggests malignancy
- Chromatin distribution: irregular clumping indicates neoplasia
- Fine chromatin: uniform distribution in benign cells
- Coarse chromatin: irregular clumping in malignant cells
- Hyperchromasia: increased nuclear staining intensity
- Cytoplasmic Characteristics
- Volume assessment: decreased cytoplasm in high-grade lesions
- Staining properties: basophilia suggests increased RNA
- Eosinophilic cytoplasm: mature differentiation patterns
- Basophilic cytoplasm: active protein synthesis
- Architectural Patterns
- Cellular cohesion: loss of cohesion in malignant processes
- Background changes: tumor diathesis in 60% of malignancies
⭐ Clinical Pearl: Nucleolar prominence correlates with cellular proliferation rate, with nucleoli >2 micrometers suggesting high-grade malignancy. Multiple nucleoli per nucleus indicate aggressive biological behavior.
| Morphological Feature | Benign Pattern | Malignant Pattern | Diagnostic Weight | Sensitivity |
|---|---|---|---|---|
| Nuclear size | Uniform, small | Variable, enlarged | High | 90% |
| Chromatin | Fine, uniform | Coarse, irregular | Very High | 95% |
| Nucleoli | Inconspicuous | Prominent, multiple | Moderate | 75% |
| N:C ratio | <1:4 | >1:2 | High | 85% |
| Cohesion | Maintained | Lost | Moderate | 70% |
Morphological mastery enables rapid pattern recognition, connecting cellular appearance to biological behavior and establishing the framework for systematic diagnostic approaches that ensure consistent, accurate interpretations.
⚙️ Cellular Architecture: The Morphological Command Center
🎯 Pattern Recognition: The Diagnostic Radar System
📌 Remember: PATTERN recognition follows Papillary structures, Architectural loss, Three-dimensional clusters, Tumor diathesis, Epithelial pearls, Rosette formation, Necrotic background. Each pattern correlates with specific diagnostic entities.
-
High-Yield Pattern Recognition Framework
- Papillary clusters: branching architecture suggests papillary carcinoma
- Single cell dispersal: loss of cohesion indicates high-grade malignancy
- Cohesive clusters: >90% benign or low-grade processes
- Discohesive pattern: 75% malignant correlation
- Mixed pattern: intermediate-grade lesions
- Three-dimensional clusters: >6 cell layers suggests malignancy
- Syncytial arrangements: multinucleated giant cells in specific contexts
-
Background Pattern Analysis
- Tumor diathesis: necrotic debris + blood in 60% of malignancies
- Inflammatory background: neutrophils + macrophages suggest infection
- Acute inflammation: neutrophil predominance >80%
- Chronic inflammation: lymphocyte predominance >60%
- Granulomatous: epithelioid cells + giant cells
- Clean background: absence of debris favors benign processes

⭐ Clinical Pearl: Papillary architecture with fibrovascular cores shows 85% correlation with papillary thyroid carcinoma, while follicular patterns require capsular invasion assessment for malignancy determination.
| Pattern Type | Morphological Features | Diagnostic Correlation | Specificity | Clinical Significance |
|---|---|---|---|---|
| Papillary | Branching, fibrovascular cores | Papillary carcinoma | 90% | Excellent prognosis |
| Follicular | Microfollicles, colloid | Follicular neoplasm | 70% | Requires histology |
| Discohesive | Single cells, loss of cohesion | High-grade malignancy | 85% | Poor prognosis |
| Syncytial | Multinucleated, overlapping | Specific tumor types | 95% | Subtype-specific |
| Rosette | Central lumen, radial arrangement | Neuroendocrine tumors | 98% | Hormone production |
- Thyroid: Papillary vs follicular vs medullary patterns
- Breast: Ductal vs lobular vs special type arrangements
- Ductal pattern: cohesive sheets with peripheral palisading
- Lobular pattern: single-file arrangement in linear chains
- Lung: Squamous vs adenocarcinoma vs neuroendocrine patterns
- Lymphoid: Monomorphic vs polymorphic populations
💡 Master This: Pattern recognition speed improves with systematic scanning at 100x magnification followed by detailed evaluation at 400x, achieving diagnostic accuracy >95% through hierarchical pattern assessment.
Pattern mastery creates diagnostic confidence, enabling rapid screening with high sensitivity while maintaining the specificity needed for accurate patient management and treatment planning decisions.
🎯 Pattern Recognition: The Diagnostic Radar System
🔍 Differential Diagnosis: The Systematic Discriminator
📌 Remember: DISCRIMINATE follows Differential features, Immunoprofile needs, Staining patterns, Chromatin differences, Ratio measurements, Infiltration patterns, Mitotic activity, Inflammatory background, Necrosis presence, Architectural loss, Three-dimensional growth, Epithelial markers. Each parameter contributes weighted diagnostic value.
-
Primary Differential Categories
- Benign vs Malignant: fundamental discrimination requiring multiple criteria
- Primary vs Metastatic: architectural patterns and immunoprofile correlation
- Primary tumors: organ-specific patterns with characteristic architecture
- Metastatic disease: discohesive patterns with atypical architecture
- Unknown primary: requires immunocytochemistry in 70% of cases
- Epithelial vs Mesenchymal: cohesion patterns and cellular morphology
- Reactive vs Neoplastic: inflammatory background and cellular uniformity
-
Quantitative Discrimination Criteria
- Nuclear size variation: >3-fold difference suggests malignancy
- Mitotic index: >5 mitoses per 10 HPF indicates high-grade lesions
- Low-grade: <2 mitoses per 10 HPF
- Intermediate-grade: 2-5 mitoses per 10 HPF
- High-grade: >5 mitoses per 10 HPF
- Cellular density: >200 cells per cluster suggests neoplasia
- Background necrosis: >30% field involvement correlates with malignancy
⭐ Clinical Pearl: Chromatin texture analysis provides highest discriminatory value, with coarse, irregularly distributed chromatin showing 95% specificity for malignancy across all organ systems.
| Diagnostic Feature | Benign Range | Borderline Range | Malignant Range | Discrimination Power | Clinical Impact |
|---|---|---|---|---|---|
| Nuclear size | 8-12 μm | 12-15 μm | >15 μm | High | Treatment planning |
| N:C ratio | <1:4 | 1:4 to 1:2 | >1:2 | Very High | Prognosis |
| Chromatin coarseness | Fine, uniform | Slightly coarse | Coarse, irregular | Highest | Grade assignment |
| Nucleolar size | <1 μm | 1-2 μm | >2 μm | Moderate | Proliferation rate |
| Mitotic index | <2/10 HPF | 2-5/10 HPF | >5/10 HPF | High | Aggressiveness |
- Thyroid nodules: Benign vs follicular neoplasm vs papillary carcinoma
- Breast masses: Fibroadenoma vs invasive carcinoma vs lymphoma
- Fibroadenoma: cohesive epithelial sheets with bare nuclei
- Invasive carcinoma: discohesive cells with nuclear pleomorphism
- Lung lesions: Reactive pneumocytes vs adenocarcinoma vs squamous carcinoma
- Lymph nodes: Reactive hyperplasia vs lymphoma vs metastatic carcinoma
💡 Master This: Systematic differential diagnosis requires hierarchical assessment starting with benign vs malignant, followed by primary vs metastatic, then specific subtype classification using quantitative morphometric criteria.
Differential mastery enables confident diagnosis in challenging cases, providing the discrimination skills necessary for accurate patient management and appropriate therapeutic interventions based on precise morphological assessment.
🔍 Differential Diagnosis: The Systematic Discriminator
⚖️ Treatment Correlation: The Clinical Decision Matrix
📌 Remember: TREATMENT correlation follows Tumor grade assessment, Resectability evaluation, Emergency intervention needs, Adjuvant therapy planning, Targeted therapy selection, Monitoring protocols, Efficacy assessment, Neoadjuvant considerations, Timing optimization. Each factor influences patient outcomes.
-
Immediate Clinical Applications
- Emergency diagnosis: same-day results in 80% of cases
- Surgical planning: tumor grade determines resection margins
- Low-grade lesions: conservative margins sufficient
- High-grade lesions: wide margins required
- Metastatic disease: palliative approach consideration
- Therapeutic monitoring: response assessment during treatment
- Prognostic stratification: survival prediction based on morphological features
-
Treatment Algorithm Integration
- Thyroid nodules: Bethesda classification guides surgical decisions
- Breast lesions: ER/PR status determines hormonal therapy
- ER-positive: tamoxifen therapy for 5-10 years
- HER2-positive: trastuzumab therapy improves survival by 30%
- Lung cancer: mutation status guides targeted therapy
- Lymphoma: immunophenotype determines chemotherapy regimen
⭐ Clinical Pearl: Rapid on-site evaluation (ROSE) during FNA procedures achieves adequacy rates >95% and reduces repeat procedures by 60%, enabling immediate treatment planning in surgical settings.
| Diagnostic Category | Treatment Implication | Time to Treatment | Success Rate | Monitoring Protocol |
|---|---|---|---|---|
| Benign | Surveillance only | No urgency | >95% stable | Annual follow-up |
| Atypical | Repeat sampling | 3-6 months | 80% resolution | Close monitoring |
| Suspicious | Surgical consultation | 2-4 weeks | 90% accuracy | Pre-op staging |
| Malignant | Immediate staging | <1 week | >95% accuracy | Treatment response |
| Metastatic | Systemic therapy | <72 hours | 85% palliation | Symptom control |
- Chemotherapy response: cellular morphology changes predict treatment efficacy
- Radiation effects: nuclear changes indicate therapeutic response
- Early response: nuclear swelling and chromatin clumping
- Late response: cellular necrosis and fibroblastic proliferation
- Targeted therapy: molecular markers guide treatment continuation
- Immunotherapy: inflammatory infiltrate indicates immune activation
💡 Master This: Cytopathological diagnosis provides treatment-directing information in >90% of cases, with grade assessment and subtype classification directly influencing surgical approach, adjuvant therapy selection, and long-term monitoring protocols.
Treatment correlation mastery ensures that cytopathological expertise translates into optimal patient care, connecting microscopic observations with evidence-based therapeutic interventions that improve clinical outcomes and patient survival.
⚖️ Treatment Correlation: The Clinical Decision Matrix
🔗 Advanced Integration: The Multi-System Diagnostic Network
📌 Remember: INTEGRATION follows Immunocytochemistry application, Next-generation sequencing, Telepathology consultation, Electronic reporting, Genetic profiling, Risk stratification, Artificial intelligence, Targeted therapy, Imaging correlation, Outcome prediction, Network collaboration. Each component enhances diagnostic precision.
-
Ancillary Testing Integration
- Immunocytochemistry: >200 antibodies available for subtype classification
- Flow cytometry: lymphoid populations characterized with >95% accuracy
- B-cell markers: CD19, CD20, CD79a for lineage determination
- T-cell markers: CD3, CD4, CD8 for subset identification
- Plasma cell markers: CD138, kappa, lambda for clonality assessment
- Molecular diagnostics: mutation detection in minimal specimens
- Fluorescence in situ hybridization: chromosomal abnormalities in single cells
-
Digital Pathology Revolution
- Whole slide imaging: scanning resolution at 0.25 μm per pixel
- AI-assisted diagnosis: pattern recognition algorithms with >90% concordance
- Cervical screening: automated abnormality detection reduces false negatives by 50%
- Thyroid FNA: computer-aided diagnosis improves consistency by 30%
- Telepathology: remote consultation enables expert opinion access
- Quality assurance: automated monitoring of diagnostic accuracy
⭐ Clinical Pearl: Liquid-based cytology combined with HPV testing achieves >99% negative predictive value for cervical cancer, enabling extended screening intervals and improved patient compliance.
| Integration Component | Technology Platform | Diagnostic Enhancement | Implementation Rate | Clinical Impact |
|---|---|---|---|---|
| Digital imaging | Whole slide scanners | Remote consultation | 60% labs | Expert access |
| AI algorithms | Deep learning | Pattern recognition | 25% labs | Consistency |
| Molecular testing | NGS platforms | Mutation detection | 80% labs | Targeted therapy |
| Telepathology | Cloud platforms | Rapid consultation | 40% labs | Rural access |
| LIS integration | Electronic systems | Workflow efficiency | 90% labs | Turnaround time |
- Pharmacogenomics: drug metabolism prediction from cytological specimens
- Biomarker profiling: treatment response prediction with >85% accuracy
- PD-L1 expression: immunotherapy response predictor
- Microsatellite instability: checkpoint inhibitor sensitivity
- Minimal residual disease: treatment monitoring at cellular level
- Circulating tumor cells: metastasis detection and prognosis assessment
💡 Master This: Multi-system integration transforms cytopathology from morphological description to precision medicine platform, enabling personalized treatment selection and real-time therapy monitoring through comprehensive molecular profiling.
Advanced integration mastery positions cytopathologists as central figures in precision medicine, connecting traditional morphological expertise with cutting-edge molecular diagnostics to deliver personalized patient care that optimizes therapeutic outcomes.
🔗 Advanced Integration: The Multi-System Diagnostic Network
🎯 Clinical Mastery: The Rapid-Fire Diagnostic Arsenal
Essential Diagnostic Arsenal for immediate clinical application:
📌 Remember: RAPID diagnosis requires Recognition patterns, Ancillary testing, Pattern correlation, Immediate reporting, Differential ranking. Master these five pillars for clinical excellence.
- Critical Numbers Arsenal
- N:C ratio >1:2: malignancy likelihood 85%
- Nuclear size >15 μm: high-grade lesion 90%
- Mitotic index >5/10 HPF: aggressive behavior 95%
- Chromatin coarseness: malignancy correlation 95%
- Nucleolar prominence >2 μm: proliferation marker 80%
| Rapid Assessment Tool | Time Required | Accuracy Rate | Clinical Decision | Emergency Value |
|---|---|---|---|---|
| ROSE evaluation | <5 minutes | >95% | Adequacy assessment | Prevents repeat |
| Malignancy screen | <10 minutes | >90% | Surgical planning | Same-day surgery |
| Grade assessment | <15 minutes | >85% | Margin planning | Operative strategy |
| Subtype classification | <30 minutes | >80% | Therapy selection | Treatment initiation |
💡 Master This: Cytopathological expertise transforms cellular observations into life-saving diagnoses, requiring continuous pattern recognition training, ancillary testing integration, and clinical correlation skills that directly impact patient survival and treatment outcomes.
🎯 Clinical Mastery: The Rapid-Fire Diagnostic Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















