VHD Overview - Murmur Mania
- Lesions: Stenosis (narrowing, obstructs flow) or Regurgitation (leaking, backflow).
- Causes: Rheumatic heart disease (RHD), degeneration, endocarditis, congenital.
- Murmurs: Turbulent flow sounds. Key: Timing (systolic/diastolic), character, location, radiation.
- Systolic: Between S1-S2 (e.g., AS, MR).
- Diastolic: Between S2-S1 (e.g., AR, MS).
- Dynamic Auscultation: Maneuvers (Valsalva, squatting) alter murmurs, aiding diagnosis.
⭐ Austin Flint murmur: A functional mid-diastolic rumble at the apex in severe aortic regurgitation, mimicking mitral stenosis.
Mitral Stenosis - Rheumatic Remnants
- Etiology: Predominantly Rheumatic Heart Disease (RHD).
- Patho: Leaflet fibrosis, commissural fusion → "fish-mouth" valve.
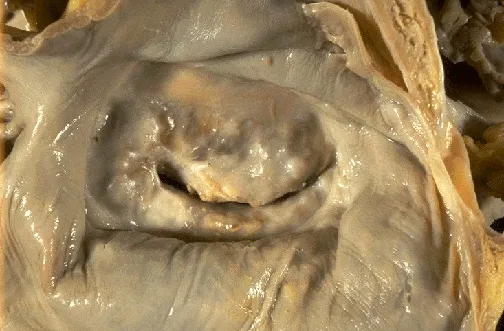
- Hemodynamics:
- ↓MVA (Normal 4-6 cm²; MS < 2.5 cm²; Severe < 1.5 cm²).
- ↑LA pressure → LA enlargement (AFib, thrombi risk) → pulmonary HTN.
- Auscultation:
- Loud S1 (mobile leaflets).
- Opening Snap (OS) after S2 (earlier = severe).
- Mid-diastolic rumbling murmur (apex, L. lateral, bell).
- 📌 Mnemonic: MS LA LA - MS causes LA LArgenent, Loud S1, OS.
⭐ Often unmasked/worsened by pregnancy's increased cardiac output, making it the most common valvular issue in gestation.
Mitral Regurgitation - Floppy Valve Fiasco
- Patho: LV → LA systolic backflow. Causes: MVP (floppy valve), RHD, IE, papillary muscle rupture, LV dilatation.
- Symptoms: Acute: pulmonary edema. Chronic: dyspnea, fatigue, AF.
- Signs: Pansystolic murmur (apex → axilla), S3, hyperdynamic apex.
- Dx: Echo confirms. ECG: LAE, LVH. CXR: cardiomegaly.
- Rx: Medical: ACEi, diuretics. Surgical: Valve repair/replacement if severe/symptomatic or LV dysfunction (EF < 60%, LVESD > 40 mm).
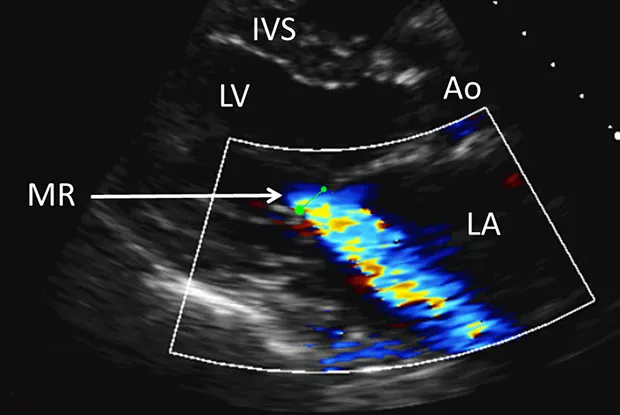
⭐ Giant V waves in LA pressure tracing are characteristic of severe MR.
Aortic Stenosis - Calcific Constriction

- Etiology: Most common valvular abnormality; age-related degenerative calcification (>65 yrs) or calcification of congenitally bicuspid aortic valve (<65 yrs).
- Pathophysiology: Obstruction to left ventricular (LV) outflow → ↑ LV pressure → concentric LV hypertrophy (LVH).
- Clinical Features: 📌 SAD triad: Syncope (exertional), Angina, Dyspnea (exertional).
- Harsh crescendo-decrescendo systolic ejection murmur at right upper sternal border, radiates to carotids.
- Pulsus parvus et tardus (weak and delayed carotid upstroke).
- Severity: Severe AS if aortic valve area (AVA) < 1.0 cm² or mean gradient > 40 mmHg.
⭐ Bicuspid aortic valve is a common congenital heart defect predisposing to earlier onset calcific aortic stenosis, often by age 50-60.
Aortic Regurgitation - Diastolic Drama
- Patho: Diastolic blood backflow (Aorta → LV) → ↑LV preload → LV dilation & hypertrophy.
- Etiology (Chronic): RHD, bicuspid valve, Marfan's. (Acute): IE, dissection.
- Murmur: High-pitched, blowing, early diastolic decrescendo murmur (LSB/RSB).
- 📌 Austin Flint murmur: Mid-diastolic rumble at apex.
- Signs: Wide pulse pressure. Peripheral: Corrigan's (water-hammer), de Musset's (head bob).
⭐ Hill's sign: Popliteal SBP > Brachial SBP by >20 mmHg (severe if >60 mmHg).
- Echo: Confirms, severity, LV function (EF < 50% often guides surgery).
High‑Yield Points - ⚡ Biggest Takeaways
- Rheumatic fever: Most common cause of mitral stenosis; features Aschoff bodies.
- Mitral Valve Prolapse: Mid-systolic click; associated with Marfan/Ehlers-Danlos.
- Aortic Stenosis: Classic SAD triad (Syncope, Angina, Dyspnea); often senile calcific.
- Infective Endocarditis: Tricuspid valve in IV drug users (often S. aureus).
- Aortic Regurgitation: Austin Flint murmur, de Musset's sign, water-hammer pulse.
- Libman-Sacks endocarditis: Sterile vegetations in SLE; affects both valve surfaces.
- Carcinoid heart disease: Affects right-sided valves (tricuspid/pulmonary) with fibrous plaques.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

