Pericardial Basics - Heart's Cozy Coat
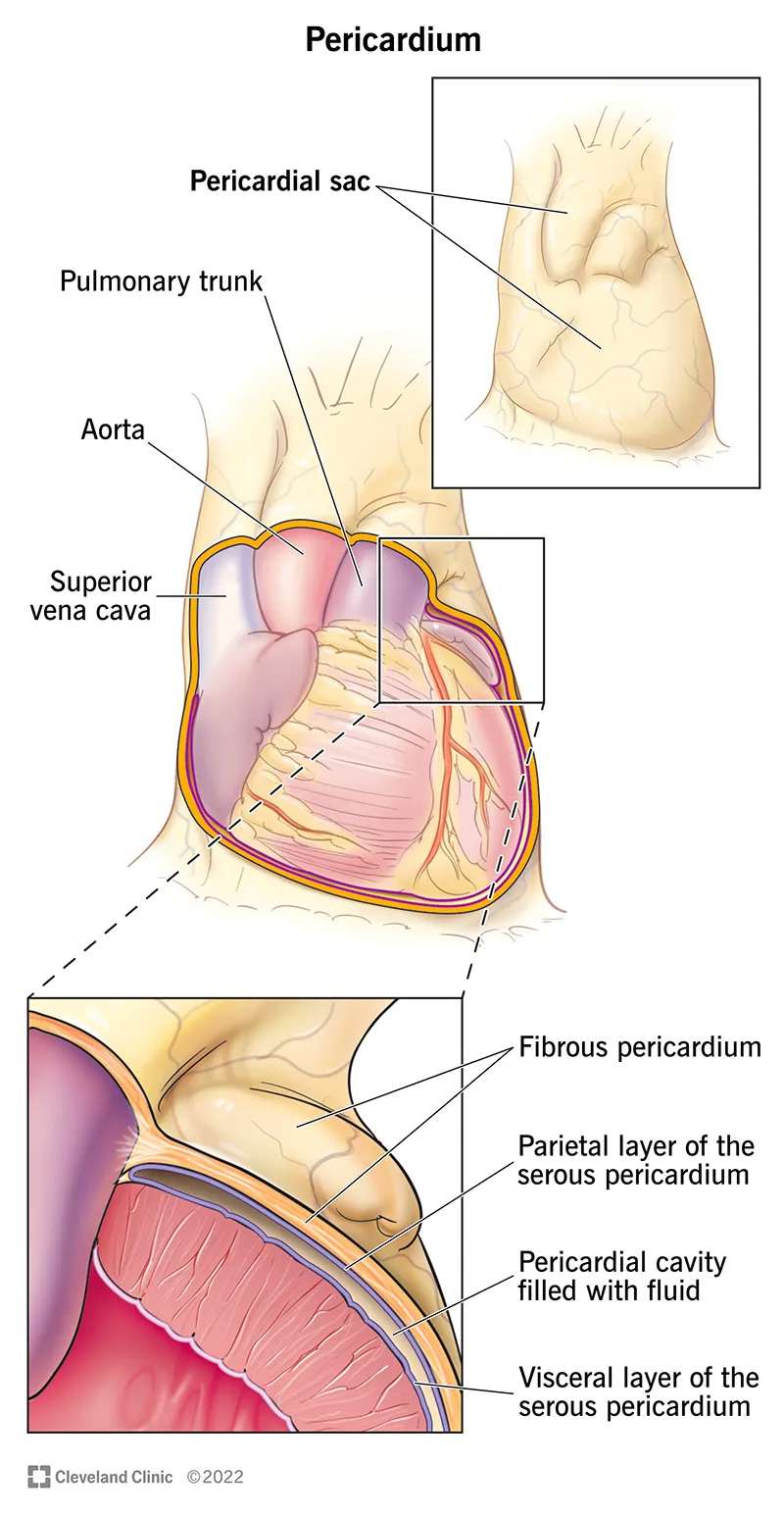
- Layers & Space:
- Outer: Tough Fibrous Pericardium.
- Inner: Serous Pericardium:
- Parietal layer (lines fibrous).
- Visceral layer (epicardium; on heart surface).
- Pericardial Cavity: Space between serous layers; contains 15-50 mL of lubricating fluid.
- Core Functions:
- Limits acute cardiac distension.
- Reduces friction during cardiac motion.
- Barrier against infection/inflammation.
⭐ The pericardium is composed of an outer fibrous layer and an inner serous layer (parietal and visceral, with the pericardial cavity between them).
Acute Pericarditis - Chest Pain Drama
- Etiology: Most common: Idiopathic, Viral (Coxsackie B). Others: Uremia, Post-MI (Dressler's syndrome), TB, Autoimmune (SLE), Neoplastic.
- Clinical: Sharp, pleuritic chest pain (relieved sitting up/leaning forward, worse supine). Fever. Pericardial friction rub (triphasic, transient).
- ECG: Diffuse concave ST elevation & PR depression. Stages:
- I: Widespread ST↑, PR↓
- II: ST/PR normalize
- III: T-wave inversions
- IV: ECG normalizes

- Diagnosis: Requires ≥2 of 4 criteria:
- Typical pericarditic chest pain
- Pericardial friction rub
- Characteristic ECG changes (new ST↑ or PR↓)
- New or worsening pericardial effusion
⭐ The most common causes of acute pericarditis are idiopathic and viral infections.
- Management: NSAIDs (e.g., ibuprofen) + Colchicine (reduces recurrence). Corticosteroids for refractory cases or specific indications (e.g., autoimmune, uremic if NSAIDs fail/contraindicated).
Effusion & Tamponade - Squeezing The Pump
- Pericardial Effusion: Fluid >50mL in pericardial space.
- Cardiac Tamponade: Effusion causing hemodynamic compromise.
- Pathophysiology: ↑ Intrapericardial pressure → ↓ Venous return → ↓ Diastolic filling → ↓ Stroke volume → Hypotension, shock.
- Clinical (Tamponade):
- Beck's Triad: Hypotension, ↑JVP (Distended Neck Veins), Muffled heart sounds. 📌 3 D's: Decreased Arterial Pressure, Distended Jugular Veins, Distant Heart Sounds.
- Pulsus Paradoxus: >10 mmHg SBP fall on inspiration.
- Tachycardia, dyspnea.
- Diagnosis:
- Echocardiography (key): Effusion size, diastolic RV/RA collapse, swinging heart.
- ECG: Low voltage QRS, electrical alternans.
- Management:
- Urgent Pericardiocentesis: Diagnostic & therapeutic for tamponade.
- IV fluids (temporizing).
- Treat underlying cause.
⭐ Electrical alternans on ECG is highly suggestive of large pericardial effusion and cardiac tamponade.

Constrictive Pericarditis - Heart In A Vise
Thickened, fibrotic, often calcified pericardium restricts diastolic filling.
- Etiology: Idiopathic, post-surgery, radiation, TB, recurrent pericarditis.
- Pathophysiology: Impaired ventricular filling → equalization of diastolic pressures.
- Clinical: RHF (edema, ascites), dyspnea.
- Pericardial knock (early diastolic).
- Kussmaul's sign (paradoxical ↑JVP on inspiration).
- Friedreich's sign (rapid y-descent JVP).
- Diagnosis:
- Echo: Septal bounce, respiratory variation in inflow.
- CT/MRI: Pericardial thickening >4mm, calcification.
- Cath: Dip-and-plateau (square root sign).
⭐ Kussmaul's sign, a paradoxical rise in jugular venous pressure during inspiration, is a characteristic finding in constrictive pericarditis.
- Management: Pericardiectomy.

CP vs. Restrictive Cardiomyopathy (RCM)
| Feature | Constrictive Pericarditis (CP) | Restrictive Cardiomyopathy (RCM) |
|---|---|---|
| Pathology | Pericardial (thick, fibrotic) | Myocardial (stiff, infiltrated) |
| Diastolic Filling | External constraint | Stiff myocardium |
| Pressures | Equalized diastolic | LV > RV diastolic |
| Pericardial Knock | Present | Absent |
| Kussmaul's Sign | Common | Rare |
| Pericardial Thickening | >4mm, calcification | Normal |
High‑Yield Points - ⚡ Biggest Takeaways
- Fibrinous pericarditis: most common, post-MI (Dressler's syndrome), uremia; key sign is friction rub.
- Constrictive pericarditis: impaired diastolic filling; look for Kussmaul's sign, pericardial knock.
- Cardiac tamponade: Beck's triad (hypotension, JVD, muffled sounds) and pulsus paradoxus are classic.
- Acute pericarditis: commonly viral (Coxsackie B); causes sharp chest pain, diffuse ST elevation.
- Tuberculous pericarditis: a major cause of chronic constrictive pericarditis in endemic areas.
- Uremia and malignancy are important non-infectious causes of pericarditis and large effusions respectively.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

