Myocarditis - Heart's Inflamed Fury
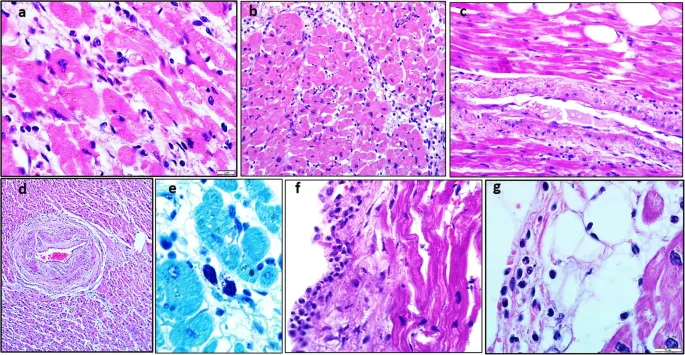
- Definition: Inflammation of myocardium.
- Etiology:
- Viral (Coxsackie B, Adenovirus, Parvovirus B19, HIV, Influenza) - Most common.
- Bacterial (Diphtheria, Lyme disease).
- Protozoal (Trypanosoma cruzi - Chagas disease).
- Autoimmune (SLE, Rheumatic fever).
- Drugs (Clozapine, Doxorubicin).
- Clinical Features: Chest pain, dyspnea, fever, arrhythmias, heart failure.
- Diagnosis:
- ECG: ST-T changes, arrhythmias.
- ↑Cardiac enzymes (Troponin, CK-MB).
- Endomyocardial biopsy (Gold standard): Lymphocytic infiltrate, myocyte necrosis.
⭐ Giant cell myocarditis: Poor prognosis, often requires transplant; characterized by multinucleated giant cells.
- Complications: Dilated cardiomyopathy, sudden cardiac death. 📌 Mnemonic (Causes): Viruses Are Bad Drugs To Really Inflame Hearts (Viral, Autoimmune, Bacterial, Drugs, Toxins, Radiation, Idiopathic, Hypersensitivity).
Cardiomyopathies - Muscle Trouble Tales
- Diseases of heart muscle causing cardiac dysfunction.
- Main types:
- Dilated (DCM): Most common; systolic dysfunction, ventricular dilation.
- Hypertrophic (HCM): Diastolic dysfunction; LVH, often asymmetric septal hypertrophy.
- Restrictive (RCM): Stiff ventricles, impaired diastolic filling; e.g., amyloidosis.
- Arrhythmogenic RV Dysplasia (ARVD): Fibrofatty replacement of RV.
- Takotsubo: Stress-induced; "broken heart" syndrome.
⭐ In HCM, mutations in sarcomeric protein genes (e.g., MYH7, MYBPC3) are common, making it the most common inherited cardiovascular disorder_._
DCM - Big Floppy Heart
- Most common cardiomyopathy. Characterized by LV or biventricular dilation, eccentric hypertrophy & impaired systolic function (EF < 40%), leading to systolic heart failure.
- Etiology: Idiopathic (~50%); others: Alcohol, Genetic (TTN gene), Peripartum, Post-myocarditis (Coxsackie B), Doxorubicin, Chagas. 📌 ABCCCD.
- Gross: Enlarged, heavy, flabby heart ("big floppy heart"); all 4 chambers dilated. Mural thrombi common.
- Histo: Myocyte hypertrophy & degeneration, interstitial fibrosis (often non-specific).
- Clinically: Progressive CHF (dyspnea, fatigue, edema), S3 gallop, arrhythmias, thromboembolic events.
⭐ Mutations in the Titin (TTN) gene are the most common identifiable genetic cause of DCM.
HCM - Thick Stubborn Muscle
- Autosomal dominant; mutations in sarcomeric genes (β-MHC, MYBPC3).
- Patho: Asymmetric septal hypertrophy (ASH) → LVOT obstruction, diastolic dysfunction.
- Sx: Exertional dyspnea, angina, syncope/presyncope. Murmur: Harsh crescendo-decrescendo systolic murmur at LLSB, ↑ Valsalva/standing, ↓ squatting/handgrip.
- Dx: Echo (LVH >15mm not explained by other causes), ECG (LVH, dagger Q waves).
- Rx: β-blockers, verapamil. Avoid +inotropy, ↓preload/afterload (e.g., nitrates, diuretics if obstruction). Septal myectomy/ablation. ICD for SCD risk.
⭐ Most common cause of SCD in young athletes.
RCM & Friends - Stiff & Strange Hearts
- Restrictive Cardiomyopathy (RCM): Stiff, non-compliant ventricles → impaired diastolic filling. Systolic function often preserved.
- Causes: Amyloidosis (MC), sarcoidosis, hemochromatosis, endomyocardial fibrosis (EMF), Loeffler's endocarditis, radiation.
- Clinical: Right HF > Left HF; Kussmaul's sign (↑JVP on inspiration).
- Dx: Echo (bi-atrial enlargement, diastolic dysfunction), biopsy (e.g., Congo red for amyloid).
- Arrhythmogenic RV Dysplasia (ARVD): Fibrofatty RV replacement; AD inheritance. ECG: Epsilon wave. Risk of sudden cardiac death.
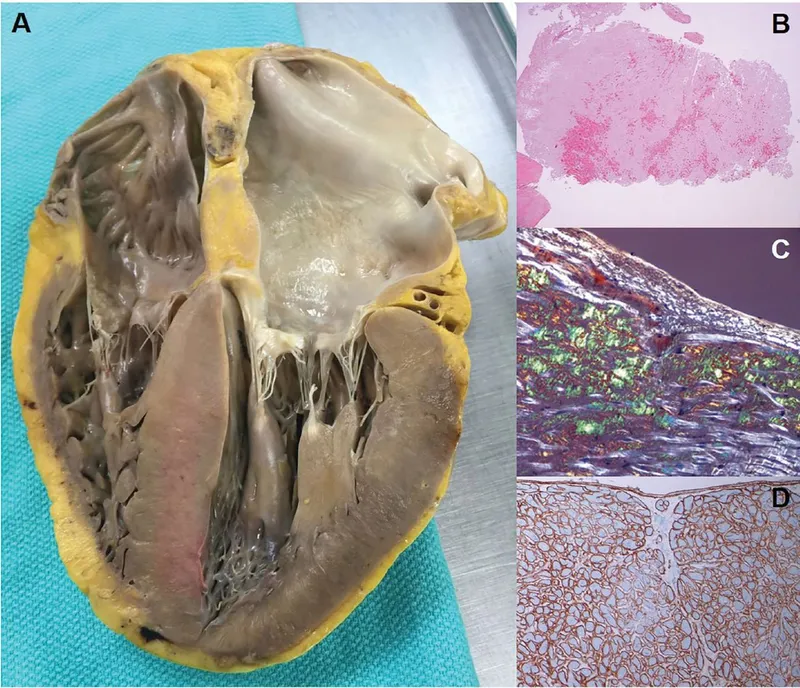
⭐ Low voltage ECG despite LVH on echo is a classic clue for cardiac amyloidosis (a cause of RCM).
High‑Yield Points - ⚡ Biggest Takeaways
- Myocarditis: Most often viral (Coxsackie B); lymphocytic infiltrate with myocyte necrosis.
- Dilated Cardiomyopathy (DCM): Most common; causes include alcohol, genetic, peripartum; leads to systolic dysfunction.
- Hypertrophic Cardiomyopathy (HCM): Autosomal dominant; asymmetric septal hypertrophy, myofiber disarray; risk of SCD.
- Restrictive Cardiomyopathy (RCM): Diastolic dysfunction from stiff ventricles; causes: amyloidosis, sarcoidosis.
- Arrhythmogenic RV Dysplasia (ARVD): Fibrofatty replacement of RV wall; associated with ventricular arrhythmias.
- Chagas disease: Important protozoal cause of myocarditis and DCM.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

