Intro & Epidemiology - Pressure Cooker Heart
- Hypertensive Heart Disease (HHD): Cardiac changes (mainly Left Ventricular Hypertrophy - LVH) from chronic high Blood Pressure (BP e.g., >130/80 mmHg). Heart adapts to increased workload.
- "Pressure Cooker Heart": Increased afterload (resistance) forces the Left Ventricle (LV) to work harder, leading to myocyte hypertrophy.
- Epidemiology: Very common globally; a major cause of heart failure, Ischemic Heart Disease (IHD), and stroke. Affects millions.
- Risk Factors: Age, male sex, African ancestry, obesity, high salt (↑Na⁺) intake, physical inactivity, family history/genetics, Chronic Kidney Disease (CKD).
⭐ Sustained diastolic BP >90 mmHg or systolic BP >140 mmHg significantly increases HHD risk.
Pathophysiology - Strain & Remodel
- Chronic Hypertension (HTN) imposes sustained ↑ afterload (pressure overload) on the Left Ventricle (LV).
- Initial Strain & Compensatory Adaptation:
- LV undergoes concentric hypertrophy: symmetrical ↑ in wall thickness; sarcomeres added in parallel.
- This aims to normalize wall stress per LaPlace's Law ($ \sigma \propto \frac{P \times r}{2h} $).
- Maladaptive Remodeling & Progressive Dysfunction:
- Persistent strain leads to myocyte hypertrophy, apoptosis, and interstitial fibrosis, causing ↑ LV stiffness.
- Results in impaired diastolic function (↓ relaxation & compliance), leading to Diastolic Heart Failure (HFpEF).
- Coronary flow reserve diminishes; myocardial O₂ demand ↑.
- Eventually, LV may dilate, leading to systolic dysfunction (HFrEF).
- Neurohormonal activation (e.g., RAAS, SNS) exacerbates remodeling.
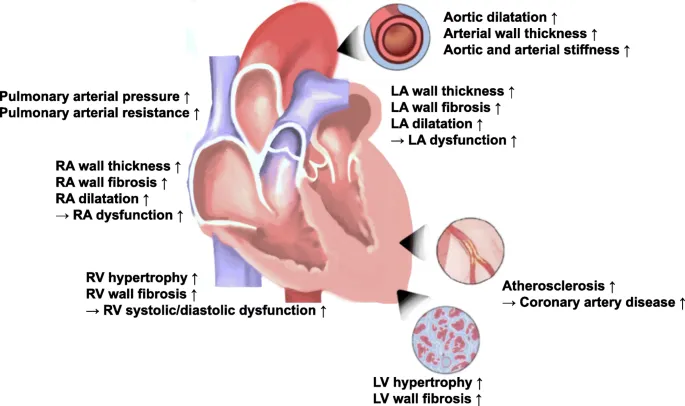
⭐ Hypertensive heart disease typically manifests first as diastolic dysfunction (HFpEF) due to concentric LV hypertrophy and impaired ventricular relaxation and filling.
Morphology - Thick & Stiff Walls
- Gross:
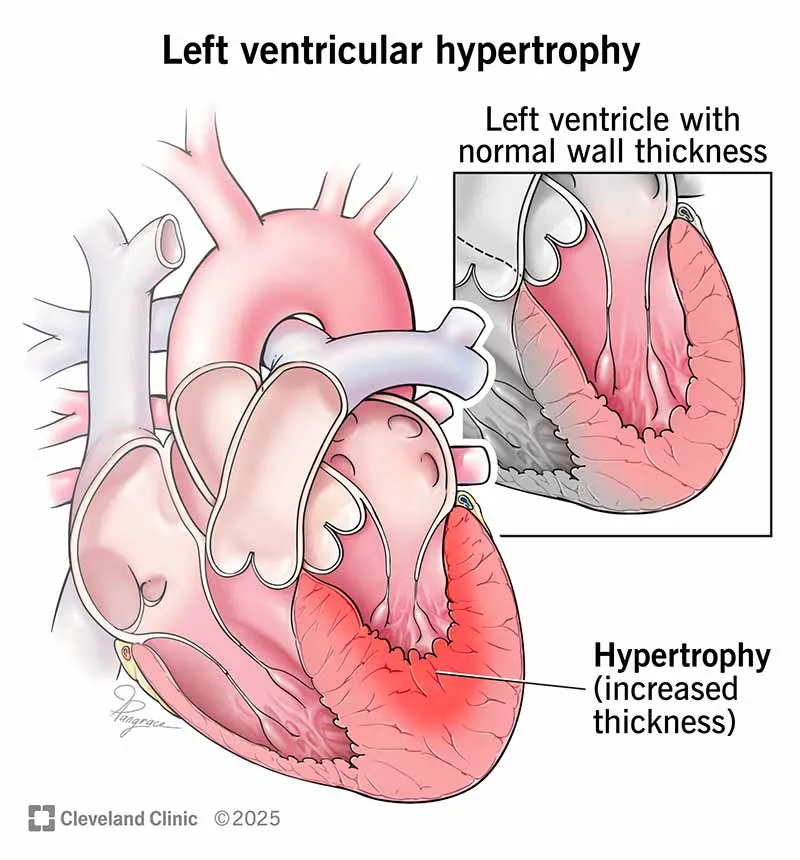
- Symmetrical, concentric Left Ventricular Hypertrophy (LVH).
- ↑ Heart weight (>500g); ↑ LV wall thickness (>2cm).
- Ventricular cavity normal/↓; papillary muscles prominent.
- Left atrial enlargement (due to diastolic dysfunction).
- "Cor bovinum" in severe cases.
- Microscopic:
- Myocyte hypertrophy: ↑ cell size, "boxcar" nuclei (enlarged, hyperchromatic, rectangular).
- Interstitial fibrosis: progressive, patchy → diffuse; ↑ stiffness.
- Small vessel changes: intramyocardial arteriolosclerosis.
⭐ "Boxcar" nuclei (enlarged, rectangular) are key microscopic features in hypertrophied myocytes of hypertensive heart disease.
Clinical Picture - Spotting the Strain
- Often initially asymptomatic; insidious onset.
- Symptoms arise from Left Ventricular Hypertrophy (LVH) & progressive heart failure:
- Dyspnea (exertional, orthopnea, PND)
- Angina, palpitations (atrial fibrillation common)
- Signs:
- Forceful, heaving apex beat
- S4 gallop (stiff LV); later S3 (failure)
- Rales, edema (CHF)
- Diagnosis:
- ECG: LVH criteria (Sokolow-Lyon: S in V1 + R in V5/V6 > 35mm)
- Echocardiography: Gold standard; confirms LVH, assesses diastolic/systolic function.
- CXR: Cardiomegaly, pulmonary congestion.
⭐ Atrial fibrillation is a common arrhythmia in hypertensive heart disease, increasing thromboembolic risk.
Complications & Prognosis - When Pressure Peaks
- Cardiac Complications: CHF (systolic/diastolic), IHD, MI, arrhythmias (esp. AF), Sudden Cardiac Death.
- Extra-cardiac Damage: Stroke, hypertensive nephrosclerosis (→ESRD), advanced retinopathy, aortic dissection.
- Prognosis: Hinges on early diagnosis, consistent BP management, and LVH regression. Aggressive control improves outcomes.
⭐ Development of symptomatic heart failure in HHD carries a grave prognosis, with up to 50% mortality at 5 years if untreated. oka
High‑Yield Points - ⚡ Biggest Takeaways
- Systemic hypertension is the key driver for left-sided hypertensive heart disease (HHD).
- Leads to left ventricular hypertrophy (LVH), initially concentric, as a compensatory mechanism.
- Prolonged LVH causes diastolic dysfunction, progressing to systolic dysfunction and heart failure.
- Microscopic features include myocyte hypertrophy ("boxcar" nuclei) and interstitial fibrosis.
- Major risks: atrial fibrillation, congestive heart failure (CHF), stroke, and sudden cardiac death.
- Diagnosis: LVH with documented hypertension, after excluding other causes like aortic stenosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


