Definition & Classification - Heart's Big Struggle
- Heart Failure (HF): Myocardial dysfunction leading to inadequate tissue perfusion or doing so only with ↑ filling pressures. A clinical syndrome.
- Key Types by Left Ventricular Ejection Fraction (LVEF):
- HFrEF (Systolic HF): LVEF ≤ 40%
- HFmrEF (Mildly Reduced EF): LVEF 41-49%
- HFpEF (Diastolic HF): LVEF ≥ 50%
- NYHA Functional Classes (Symptoms):
- I: No limits.
- II: Slight limit, ordinary activity.
- III: Marked limit, < ordinary activity.
- IV: Symptoms at rest.
- ACC/AHA Stages (Progression):
- A: High risk for HF.
- B: Structural heart dz, no symptoms.
- C: Structural heart dz + symptoms.
- D: Refractory HF.
- Other Classifications:
- Onset: Acute vs. Chronic
- Side: Left (LVF), Right (RVF), Biventricular
- Output: Low-output (common) vs. High-output (e.g., severe anemia, thyrotoxicosis)
⭐ Most common cause of right-sided heart failure (RVF) is left-sided heart failure (LVF).
Etiology & Precipitants - HF's Usual Suspects
-
Underlying Causes (Chronic HF):
- IHD/CAD: Most common cause.
- Hypertension (HTN): Chronic ↑afterload.
- Valvular Disease: e.g., Aortic Stenosis (AS), Mitral Regurgitation (MR).
- Cardiomyopathies: Dilated (DCM), Hypertrophic (HCM), Restrictive (RCM).
- Arrhythmias (Chronic): Atrial Fibrillation (AF), Tachycardiomyopathy.
- High-Output States: Severe anemia, thyrotoxicosis.
- Others: Myocarditis, Pericardial disease (constriction), Toxins (alcohol, doxorubicin).
-
Precipitants (Acute Decompensation):
- 📌 FAILURE Mnemonic:
- Forgot meds / Fluid overload / Food (↑salt).
- Arrhythmia (new AF) / Anemia.
- Ischemia / Infarction / Infection (e.g., pneumonia).
- Lifestyle (excess fluid/alcohol).
- Uncontrolled HTN / Uremia.
- Renal dysfunction.
- Embolism (Pulmonary Embolism - PE) / Endocrine (thyroid disorders).
- Drugs: NSAIDs, steroids, some Calcium Channel Blockers (CCBs), rapid β-blocker changes.
- 📌 FAILURE Mnemonic:

⭐ The most common cause of Right Heart Failure (RHF) is Left Heart Failure (LHF).
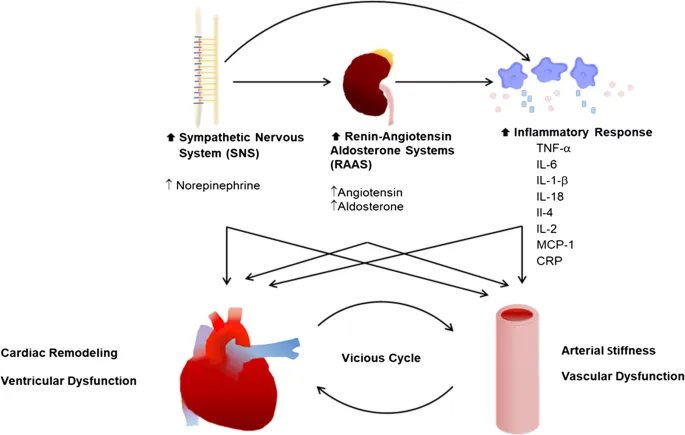
Neurohormonal Mechanisms - Body's Vicious Cycle
Heart failure (HF) triggers detrimental neurohormonal responses, forming a vicious cycle.
- Key Systems (Activated by ↓ Cardiac Output):
- RAAS (Renin-Angiotensin-Aldosterone System): ↓ Renal perfusion → Renin → Angiotensin II (Ang II) → Aldosterone.
- Ang II: Vasoconstriction (↑ afterload), aldosterone (Na⁺/H₂O retention → ↑ preload), cardiac remodeling (fibrosis, hypertrophy).
- SNS (Sympathetic Nervous System): Baroreflex → ↑ Norepinephrine.
- Effects: ↑ Heart rate, ↑ contractility, vasoconstriction. Chronic: β-receptor downregulation, myocyte toxicity, arrhythmogenic.
- AVP (Arginine Vasopressin/ADH): From ↓ CO & Ang II.
- Effects: Vasoconstriction, water reabsorption.
- RAAS (Renin-Angiotensin-Aldosterone System): ↓ Renal perfusion → Renin → Angiotensin II (Ang II) → Aldosterone.
- Counter-Regulatory (Often Overwhelmed):
- Natriuretic Peptides (ANP, BNP): From stretched atria/ventricles.
- Actions: Vasodilation, natriuresis, diuresis; inhibit RAAS & SNS.
⭐ BNP levels are crucial for HF diagnosis, severity assessment, and prognosis.
- Natriuretic Peptides (ANP, BNP): From stretched atria/ventricles.
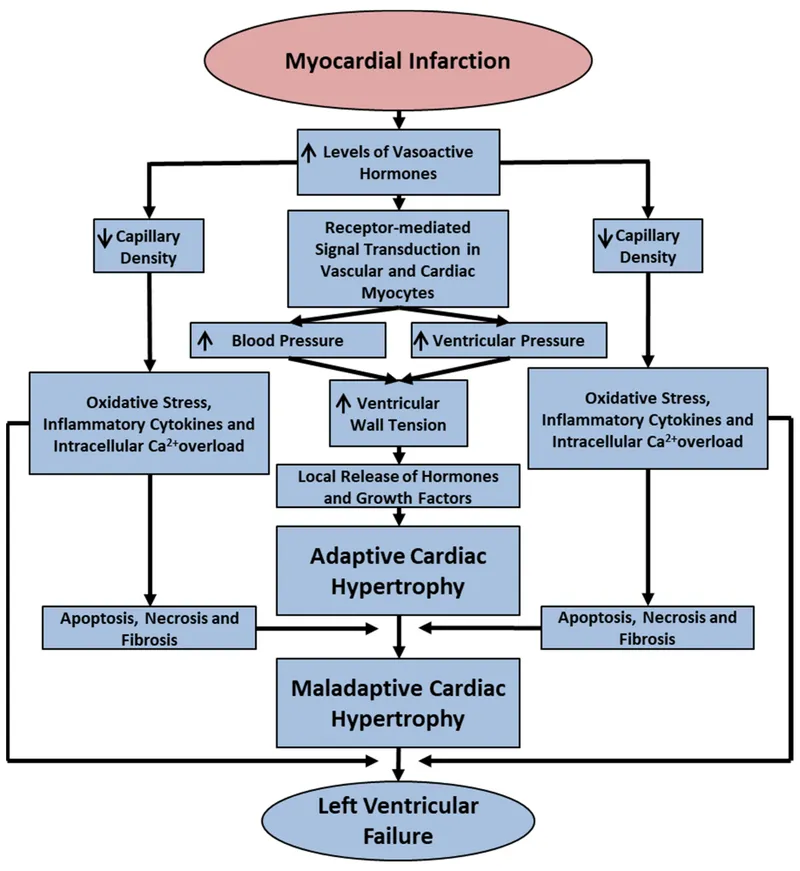
Myocardial Remodeling & Progression - Heart's Slow Change
- Persistent cardiac injury (e.g., MI, chronic overload) triggers sustained neurohormonal (RAAS, SNS) & cytokine (TNF-α, IL-6) activation.
- Drives maladaptive changes in ventricular geometry, mass, & cellular composition:
- Myocyte hypertrophy (later detrimental), dysfunction, apoptosis/necrosis.
- Fibroblast activation → excessive collagen deposition → interstitial/perivascular fibrosis, ↑stiffness.
- Altered ECM turnover: ↑Matrix Metalloproteinase (MMP) activity.
- Results in: Ventricular dilation (eccentric hypertrophy), increased sphericity, impaired pump mechanics.
- Functional impact: ↑Wall stress, ↓systolic/diastolic function, arrhythmogenicity, worsening HF.
⭐ Key drugs (ACEi, ARBs, β-blockers, MRAs) can attenuate/reverse adverse remodeling, improving prognosis in HF.
High‑Yield Points - ⚡ Biggest Takeaways
- Heart failure is the inability to meet metabolic demands or doing so only at ↑ filling pressures.
- Systolic dysfunction (HFrEF) features impaired contractility and ↓ ejection fraction (typically < 40%).
- Diastolic dysfunction (HFpEF) involves impaired ventricular relaxation and filling with a preserved ejection fraction (typically ≥ 50%).
- Key neurohormonal activation includes RAAS and SNS, leading to maladaptive cardiac remodeling.
- BNP (B-type Natriuretic Peptide) is elevated due to ventricular stretch, serving as a crucial diagnostic/prognostic marker.
- Left-sided HF leads to pulmonary congestion (dyspnea, orthopnea); Right-sided HF causes systemic venous congestion (edema, JVD).
- The Frank-Starling mechanism is an initial compensatory response, but becomes detrimental long-term.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

