Endocarditis Basics - Inner Lining Invasion
- Inflammation of the endocardium (inner lining of heart chambers & valves), primarily affecting heart valves.
- Etiology:
- Infective: Bacterial (most common), fungal.
- Non-infective: e.g., Non-bacterial Thrombotic Endocarditis (NBTE).
- Pathogenesis: Endothelial injury → platelet-fibrin nidus (may start as NBTE) → microbial adherence & colonization → vegetation formation.
- Vegetations: Core lesions; consist of microorganisms, fibrin, platelets, inflammatory cells.
- Valve Involvement Order (most to least common): Mitral > Aortic > Tricuspid > Pulmonic (📌 My Awesome Tall Partner).
- IV drug users (IVDU): Tricuspid valve frequently affected (often S. aureus).
- Key Types:
- Acute Bacterial Endocarditis (ABE): Rapid, destructive; high-virulence organisms (e.g., S. aureus); often affects normal valves.
- Subacute Bacterial Endocarditis (SBE): Insidious onset; lower-virulence organisms (e.g., Viridans streptococci); typically on pre-damaged valves.
- Prosthetic Valve Endocarditis (PVE).
⭐ Non-bacterial thrombotic endocarditis (NBTE) is often associated with malignancy or hypercoagulable states, presenting as small, sterile vegetations on cardiac valves.
侵
Etiology & Pathogenesis - Microbial Mayhem
Key Microbial Culprits:
- Bacteria (Dominant):
- Staphylococcus aureus: #1 in acute IE & IVDU (tricuspid focus).
⭐ Staphylococcus aureus is the most common cause of acute Infective Endocarditis (IE) and IE in IV drug users, often affecting the tricuspid valve.
- Viridans streptococci: Subacute IE, damaged native valves (post-dental).
- Streptococcus gallolyticus (bovis): Colorectal cancer link (colonoscopy needed).
- Enterococci: Nosocomial, elderly, post-GU procedures.
- 📌 HACEK: Haemophilus, Aggregatibacter, Cardiobacterium, Eikenella, Kingella (Gram-negative, fastidious, large vegetations, often culture-negative).
- Staphylococcus aureus: #1 in acute IE & IVDU (tricuspid focus).
- Fungi (Candida, Aspergillus): Immunocompromised, PVE, IVDU.
- Non-infective (NBTE): Marantic (cancer), Libman-Sacks (SLE).
Pathogenesis Unveiled:
Clinical Picture - Systemic Storm Signs
- General: Fever (often low-grade), chills, malaise, anorexia, weight loss, night sweats.
- Cardiac:
- New/changed heart murmur (>85% cases).
- Heart failure signs (dyspnea, edema) due to valve damage.
- Peripheral Manifestations (Embolic & Immunologic):
- 📌 Mnemonic: FROM JANE
- Fever
- Roth spots (retinal hemorrhages)
- Osler nodes (painful nodules; fingers/toes)
- Murmur (new/changed)
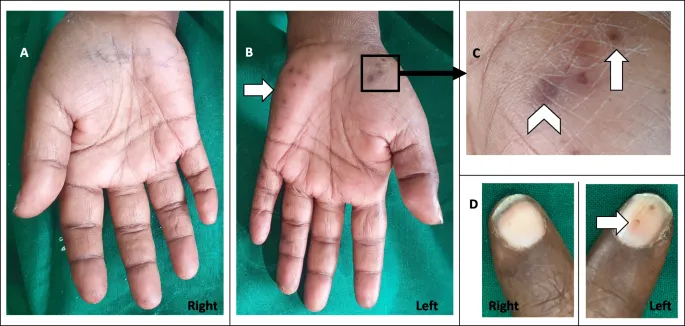
- Janeway lesions (painless macules; palms/soles)
- Anemia
- Nail-bed hemorrhages (splinter hemorrhages)
- Emboli
- Splenomegaly
- Clubbing (late)
- Glomerulonephritis
⭐ Osler's nodes are painful, violaceous nodules typically on fingers/toes (immunological complex deposition), while Janeway lesions are painless, erythematous macules on palms/soles (septic microemboli).
- 📌 Mnemonic: FROM JANE
Diagnosis & Management - Unmasking & Mending
⭐ The Modified Duke Criteria require 2 Major, OR 1 Major + 3 Minor, OR 5 Minor criteria for definite Infective Endocarditis.
- Diagnosis:
- Blood Cultures: 3 sets, 1 hr apart, pre-antibiotics.
- Echocardiography: TTE first; TEE if high suspicion/prosthetic valve/complications.
- Modified Duke Criteria:
- Major: Positive blood culture, Echo evidence (vegetation, abscess, new regurgitation).
- Minor: Predisposition, Fever (>38°C), Vascular (Janeway), Immunologic (Osler, Roth spots), Non-major micro evidence.
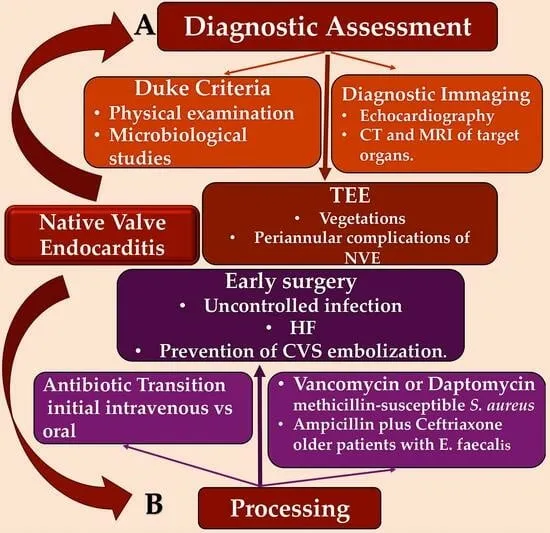
- Management:
- Empirical: Vancomycin + Gentamicin/Ceftriaxone.
- Tailored: Culture-guided, 4-6 weeks IV.
- Surgery: HF, uncontrolled infection, large vegetation (>10mm), emboli, fungal.
High‑Yield Points - ⚡ Biggest Takeaways
- Staph aureus is the most common cause of IE, especially in IVDU (tricuspid). Strep viridans for subacute native valve IE.
- Culture-negative IE: Suspect Coxiella, Bartonella, HACEK, or prior antibiotics.
- Duke criteria (blood cultures, echo: vegetations) are key for diagnosis.
- Peripheral stigmata: Janeway lesions (non-tender), Osler's nodes (tender), Roth spots.
- Libman-Sacks endocarditis (sterile) is linked to SLE.
- Early Prosthetic Valve Endocarditis (PVE): Staph epidermidis is a common cause.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

