CHD Overview - Embryo's Oopsies
- Incidence: Affects ~8-10 per 1000 live births.
- Critical Embryonic Period: Weeks 3-8 post-conception; crucial for cardiac organogenesis, especially septation and valve formation.
- Etiology: Complex interplay; often unknown.
- Genetic Factors: Chromosomal anomalies (e.g., Trisomies 13, 18, 21), single gene defects (e.g., Noonan syndrome), syndromes (e.g., Turner, DiGeorge 22q11.2 del).
- Environmental Triggers: Maternal infections (e.g., rubella), metabolic conditions (e.g., diabetes, PKU), teratogens (e.g., alcohol, thalidomide, lithium, phenytoin, retinoic acid).
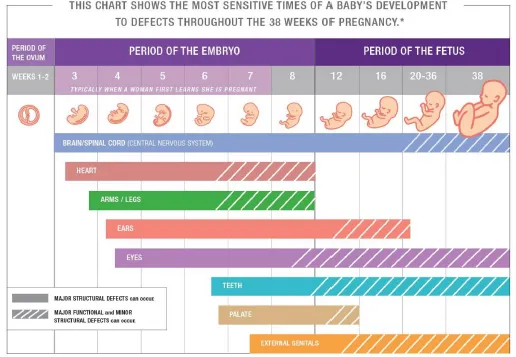
CHD Classification:
⭐ Ventricular Septal Defect (VSD) is the most common congenital heart defect overall (excluding bicuspid aortic valve).
Acyanotic CHD - No Blue Babies
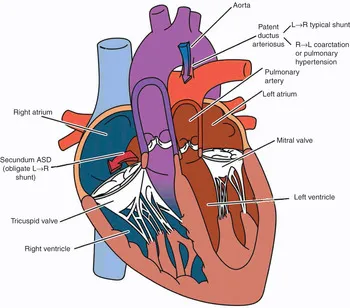
All feature L→R shunts initially. Complications: Pulmonary hypertension, Eisenmenger syndrome (late cyanosis), heart failure.
| Defect | Location/Type | Murmur | CXR Findings | Associations |
|---|---|---|---|---|
| Ventricular Septal Defect (VSD) | Membranous (commonest) | Holosystolic, LLSB | Cardiomegaly, ↑pulmonary vascularity | Down syndrome |
| Atrial Septal Defect (ASD) | Ostium secundum (commonest) | Wide, fixed split S2; ejection systolic murmur ULSB | Cardiomegaly, ↑pulmonary vascularity | Holt-Oram syndrome |
| Patent Ductus Arteriosus (PDA) | Aorta-Pulmonary Artery connection | Continuous machinery murmur 📌 (Gibson's), infraclavicular | Cardiomegaly, ↑pulmonary vascularity | Congenital rubella, prematurity |
- Types: Infantile (preductal), Adult (postductal).
- Clinical: BP ↑ upper limbs, ↓ lower limbs; weak/delayed femoral pulses.
- CXR: Rib notching, "3" sign.
⭐ Continuous machinery murmur is characteristic of Patent Ductus Arteriosus (PDA).
Cyanotic CHD - Code Blue Kids
Characterized by Right-to-Left (R→L) shunts, causing early cyanosis and ↓ $O_2$ saturation.
| Feature | Tetralogy of Fallot (ToF) | Transposition of Great Arteries (TGA) |
|---|---|---|
| Defect | 📌 PROVe: Pulmonary stenosis, RVH, Overriding aorta, VSD (R→L shunt) | Aorta from RV, PA from LV (Parallel circuits; needs shunt for survival) |
| CXR | 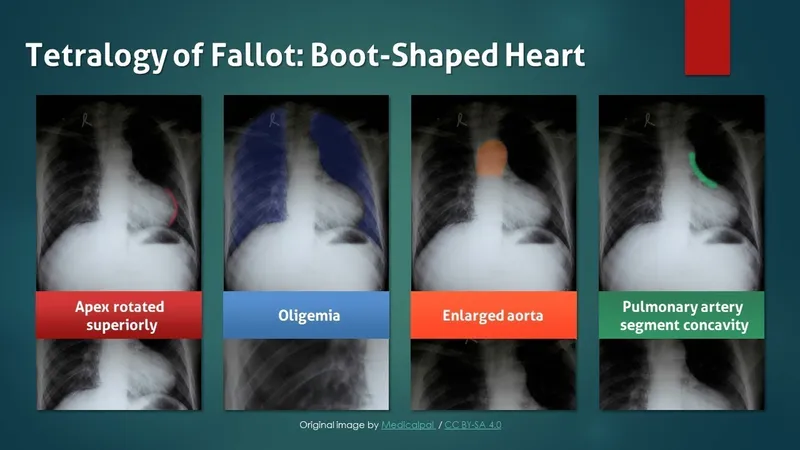 Boot-shaped Boot-shaped | 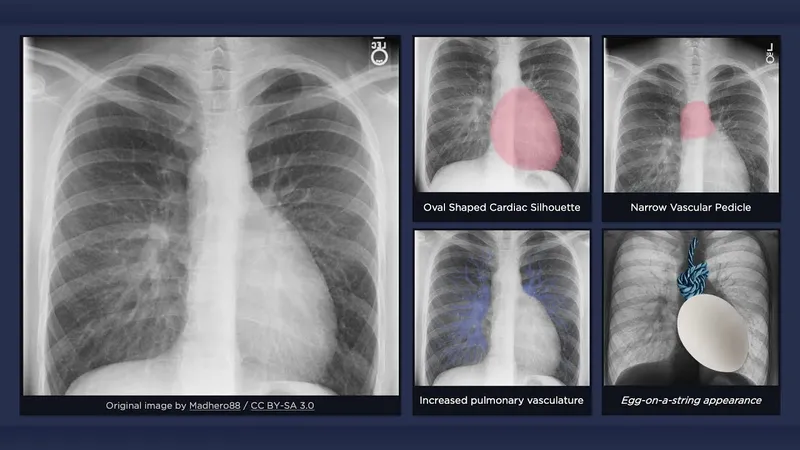 Egg-on-string Egg-on-string |
| Clinical | "Tet spells" (cyanosis, hyperpnea) on crying/exertion | Severe cyanosis from birth; PGE1 for PDA patency |
CHD Complications & Syndromes - Hearts' Hurdles
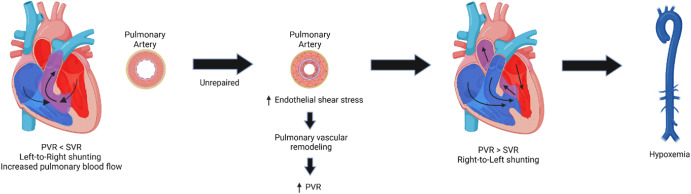
- Eisenmenger Syndrome:
- Definition: Irreversible ↑Pulmonary Vascular Resistance (PVR) → R→L shunt, late cyanosis.
- Pathophysiology:
* Clinical Features: Dyspnea, palpitations, hemoptysis, RV failure.
- Other Key Complications:
- Infective Endocarditis: Prophylaxis for high-risk (unrepaired cyanotic CHD, prosthetic material, prior IE).
- Polycythemia (secondary): Chronic hypoxia → ↑RBCs → hyperviscosity.
- Brain Abscess: R→L shunts bypass lung filtration.
- Paradoxical Embolism: Venous clot → systemic circulation via R→L shunt.
- Associated Genetic Syndromes:
Syndrome Key Associated CHD(s) Down (Trisomy 21) AVSD (Endocardial cushion defect), VSD Turner (XO) Coarctation of Aorta, Bicuspid Aortic Valve DiGeorge (22q11.2) Truncus Arteriosus, Tetralogy of Fallot Marfan Aortic Root Dilatation, MVP ⭐ Endocardial cushion defects (AVSD) are strongly associated with Down syndrome (Trisomy 21).
High‑Yield Points - ⚡ Biggest Takeaways
- Ventricular Septal Defect (VSD) is the most common CHD overall.
- Tetralogy of Fallot (ToF) is the most common cyanotic CHD.
- Eisenmenger syndrome signifies shunt reversal (L→R to R→L) causing late cyanosis.
- Patent Ductus Arteriosus (PDA) presents with a continuous machinery murmur; closed by indomethacin.
- Coarctation of Aorta is linked to Turner syndrome and rib notching.
- Down syndrome is commonly associated with endocardial cushion defects (AVSD).
- Paradoxical emboli can occur with Atrial Septal Defect (ASD) or PFO.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

