Indications & Biopsy - Heartfelt Handoff
- Indications for Transplant:
- End-stage heart failure (HF) refractory to maximal medical/device therapy.
- NYHA Class III (ambulatory) or IV.
- Common causes:
- Dilated Cardiomyopathy (DCM) - leading cause.
- Ischemic Cardiomyopathy (ICM).
- Severe, inoperable valvular or congenital heart disease.
- Refractory life-threatening arrhythmias.
- Predicted < 1-year survival without transplant.
- End-stage heart failure (HF) refractory to maximal medical/device therapy.
- Endomyocardial Biopsy (EMB):
- Primary tool for monitoring allograft rejection.
- Acute Cellular Rejection (ACR).
- Antibody-Mediated Rejection (AMR).
- Procedure: Right ventricular samples via jugular/femoral vein.
- Grading: ISHLT classification for ACR severity.
- Protocol: Routine surveillance, frequency ↓ over time.
- Primary tool for monitoring allograft rejection.
> ⭐ Endomyocardial biopsy (EMB) is the gold standard for monitoring cardiac allograft rejection.
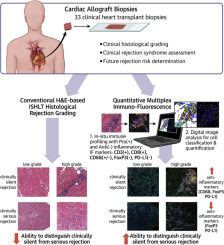
Rejection Types - Immune System Scuffles
- Immune responses against donor heart. Classified by timing & mechanism.
-
Hyperacute Rejection:
- Immediate (minutes-hours).
- Mediator: Pre-formed Donor-Specific Antibodies (DSAs) vs ABO/HLA.
- Patho: Thrombosis, necrosis.
⭐ Hyperacute rejection, occurring minutes to hours post-transplant, is mediated by pre-formed donor-specific antibodies (DSAs) against ABO or HLA antigens.
-
Acute Cellular Rejection (ACR):
- Weeks-months (common).
- Mediator: T-lymphocytes.
- EMB: Lymphocytic infiltrate, myocyte damage (ISHLT Grade 0R-3R).
-
Acute Antibody-Mediated Rejection (AMR):
- Days-months.
- Mediator: DSAs (often anti-HLA), complement.
- EMB: Microvascular inflammation, C4d deposition (ISHLT pAMR Grade 0-3).
-
Chronic Rejection (Cardiac Allograft Vasculopathy - CAV):
- Months-years (leading late cause).
- Patho: Diffuse concentric intimal thickening of coronaries ("onion skinning").
- Result: Ischemia, MI, graft failure.
Grading Rejection - Scorecard Showdown
- Standardized assessment of rejection severity.
- Acute Cellular Rejection (ACR) - ISHLT 2004 Grades:
- Grade 0R: No rejection.
- Grade 1R (Mild): Interstitial/perivascular infiltrate; ≤1 focus myocyte injury.
- Grade 2R (Moderate): ≥2 foci infiltrate, myocyte injury.
- Grade 3R (Severe): Diffuse infiltrate, multifocal injury ± edema, hemorrhage, vasculitis.
- Antibody-Mediated Rejection (AMR) - ISHLT Pathologic (pAMR) Grades:
- pAMR 0: Negative.
- pAMR 1(H+): Histology + Immunopathology (C4d/C3d/CD68).
- pAMR 1(I+): Immunopathology only.
- pAMR 2: Severe/diffuse Histology + Immunopathology.
- pAMR 3: Severe changes (capillary injury, hemorrhage, necrosis) + Immunopathology.
- Correlate with DSA & clinical status.
⭐ The International Society for Heart and Lung Transplantation (ISHLT) provides standardized grading criteria for acute cellular rejection (ACR) and antibody-mediated rejection (AMR).
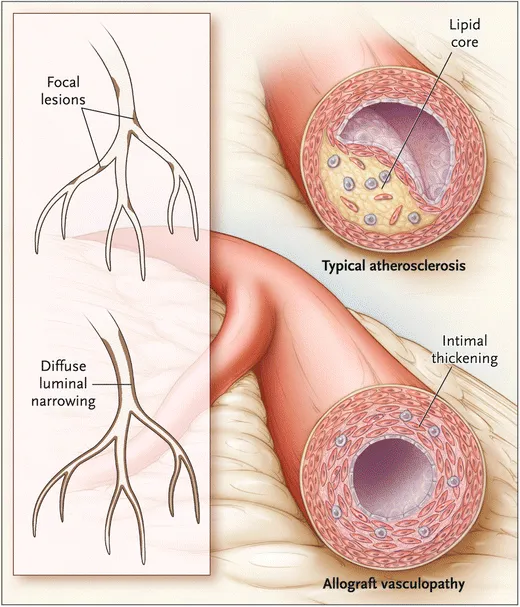
Chronic Rejection & Complications - Long-Haul Headaches
- Cardiac Allograft Vasculopathy (CAV): Primary chronic rejection form; major cause of late graft loss.
- Patho: Diffuse, concentric intimal thickening of coronary arteries (epicardial & intramyocardial), leading to luminal stenosis.
- Mechanism: Endothelial injury, smooth muscle cell proliferation, inflammation, ECM deposition. Immune (alloantibodies, T-cells) & non-immune factors (e.g., CMV, dyslipidemia).
- Clinical: Often silent ischemia/MI (denervated graft), arrhythmias, progressive heart failure.
- Dx: Intravascular ultrasound (IVUS) is gold standard; angiography less sensitive for early disease.
⭐ Cardiac Allograft Vasculopathy (CAV) is a form of chronic rejection characterized by diffuse, concentric intimal thickening of coronary arteries, leading to late graft failure.
- Other Major Long-Term Complications:
- Malignancy: Increased risk. Post-Transplant Lymphoproliferative Disorder (PTLD) - often EBV-driven; skin cancers (SCC > BCC).
- Infections: Opportunistic due to chronic immunosuppression (e.g., CMV, Aspergillus, Pneumocystis jirovecii).
- Drug Toxicity: Calcineurin inhibitor (CNI) nephrotoxicity; steroid-induced diabetes, hypertension, dyslipidemia.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyperacute rejection: Minutes to hours, pre-formed anti-donor Abs (ABO/HLA); widespread thrombosis, ischemic necrosis.
- Acute Cellular Rejection (ACR): T-cell mediated, peaks 1-3 months; Endomyocardial Biopsy (EMB) shows lymphocytic infiltrate, myocyte damage.
- Antibody-Mediated Rejection (AMR): Donor-specific Abs (DSA), C4d deposition in capillaries, microvascular inflammation, poor prognosis.
- Chronic Rejection (Cardiac Allograft Vasculopathy - CAV): Major long-term limit; diffuse concentric intimal thickening of coronaries, leading to ischemia, graft failure.
- Infections: Major mortality risk with immunosuppression; CMV, fungal, bacterial pathogens common.
- Post-Transplant Lymphoproliferative Disorder (PTLD): EBV-driven B-cell proliferation; risk ↑ with intensity of immunosuppression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

