Cardiac Pathology

On this page
🔬 Cardiac Pathology: The Heart's Microscopic Battlefield
The heart's relentless work-100,000 beats daily pumping 2,000 gallons of blood-makes it uniquely vulnerable when cellular machinery fails, oxygen supply falters, or immune attacks turn inward. You'll journey from microscopic injury patterns through ischemic crises, inflammatory assaults, and structural failures to master the diagnostic reasoning and treatment algorithms that distinguish competent clinicians from exceptional ones. This lesson builds your ability to recognize cardiac pathology's signatures, understand why each disease unfolds as it does, and intervene with precision when hearts hang in the balance.

Cardiac pathology transforms abstract disease concepts into tangible cellular realities. Every chest pain, every murmur, every heart failure symptom originates from specific microscopic changes that pathologists decode with mathematical precision. Understanding these cellular signatures unlocks the logic behind every cardiac presentation.
Pathological Process Categories
-
Ischemic Disorders (40% of cardiac deaths)
- Acute coronary syndromes with <6 hour cellular changes
- Chronic ischemia showing fibrosis >25% of myocardium
- Subendocardial pattern: inner 1/3 involvement
- Transmural pattern: full-thickness necrosis
- Watershed zones: border area vulnerability
-
Cardiomyopathies (25% of heart failure cases)
- Dilated: >55mm left ventricular end-diastolic diameter
- Hypertrophic: >15mm septal thickness
- Asymmetric pattern: septal:posterior wall ratio >1.3:1
- Symmetric pattern: concentric thickening >13mm
-
Valvular Pathology (15% of cardiac interventions)
- Stenotic lesions: <1.0 cm² effective orifice area
- Regurgitant lesions: >40% regurgitant fraction
📌 Remember: CARDIAC pathology classification - Coronary (ischemic), Arrhythmogenic, Restrictive, Dilated, Infiltrative, Acute inflammatory, Congenital. Each category has distinct microscopic signatures with specific timeframes for cellular changes.
| Disease Category | Cellular Hallmark | Timeline | Diagnostic Marker | Prognosis | Key Measurement |
|---|---|---|---|---|---|
| Acute MI | Coagulation necrosis | 6-24 hours | Troponin >50x ULN | 10% mortality | >20% LV involvement |
| Dilated CMP | Myocyte hypertrophy | Months-years | BNP >400 pg/mL | 50% 5-year survival | EF <40% |
| Hypertrophic CMP | Disarray + fibrosis | Years-decades | Septal thickness >15mm | 1% sudden death | Gradient >30 mmHg |
| Restrictive CMP | Interstitial fibrosis | Variable | Elevated filling pressures | Poor if advanced | E/A ratio >2 |
| Myocarditis | Lymphocytic infiltrate | Days-weeks | Endomyocardial biopsy | 80% recovery | >14 cells/mm² |
💡 Master This: Every cardiac pathological process creates specific microscopic fingerprints. Ischemia produces coagulation necrosis, inflammation shows lymphocytic infiltrates, and pressure overload generates concentric hypertrophy. Recognition of these patterns enables precise diagnosis within minutes of microscopic examination.
Understanding cardiac pathology's cellular foundation connects directly to recognizing how these microscopic changes manifest as clinical syndromes and guide therapeutic interventions.
🔬 Cardiac Pathology: The Heart's Microscopic Battlefield
⚡ Ischemic Heart Disease: The Oxygen Debt Crisis
Ischemic Cascade Progression
-
Acute Coronary Syndromes (1.5 million cases annually)
- STEMI: complete occlusion with ST elevation >1mm in ≥2 leads
- NSTEMI: partial occlusion with troponin elevation but no ST elevation
- High-risk: TIMI score ≥5 with >40% event rate
- Intermediate-risk: TIMI score 3-4 with 20% event rate
- Low-risk: TIMI score 0-2 with <5% event rate
-
Chronic Ischemic Disease (stable angina patterns)
- Effort angina: symptoms with >75% stenosis during exertion
- Unstable angina: crescendo pattern with plaque rupture risk
- Class I: recent onset severe angina within 2 months
- Class II: accelerating angina with increased frequency
- Class III: rest angina within 48 hours
📌 Remember: TIMELINE for MI evolution - Troponin rises (3-6 hours), Inflammation peaks (24-72 hours), Macrophages arrive (3-7 days), Early granulation (1-2 weeks), Late fibrosis (2-8 weeks), Infarct maturation (2-6 months), New equilibrium (>6 months), Endstage remodeling (years).
⭐ Clinical Pearl: Door-to-balloon time <90 minutes reduces mortality by 25% in STEMI patients. Every 30-minute delay increases 1-year mortality by 7.5%. Troponin elevation >50x upper limit indicates large infarct with >20% left ventricular involvement and doubled mortality risk.
| Infarct Location | Coronary Territory | ECG Changes | Complications | Mortality Risk | Wall Motion |
|---|---|---|---|---|---|
| Anterior | LAD | V1-V6 | Pump failure | 15-20% | Hypokinesis |
| Inferior | RCA | II, III, aVF | Heart block | 5-10% | Akinesis |
| Posterior | LCX/RCA | V7-V9 | Mitral regurg | 8-12% | Dyskinesis |
| Lateral | LCX | I, aVL, V5-V6 | Arrhythmias | 6-8% | Aneurysm |
| RV | RCA | V1, V4R | RV failure | Variable | Tricuspid regurg |
Recognizing ischemic patterns establishes the foundation for understanding how inflammatory processes can mimic or complicate coronary disease presentations.
⚡ Ischemic Heart Disease: The Oxygen Debt Crisis
🔥 Inflammatory Cardiac Diseases: The Immune System's Cardiac Assault
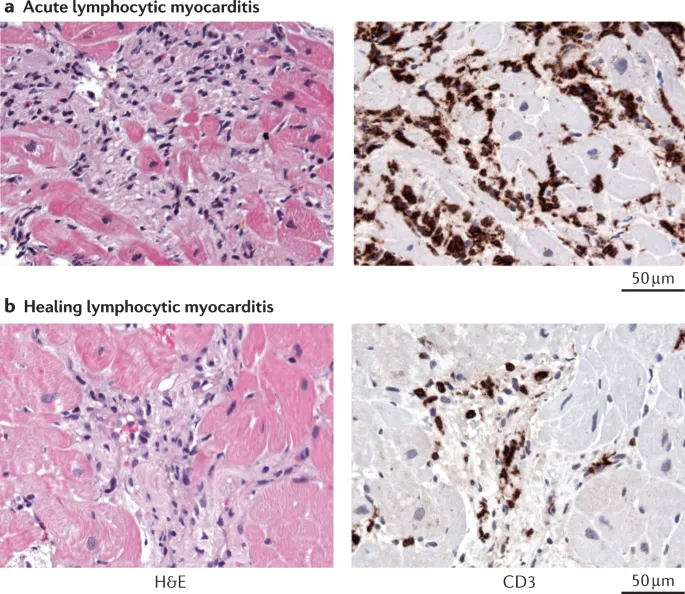
Inflammatory Disease Spectrum
-
Myocarditis (1-5% of viral infections)
- Viral: Coxsackievirus B causes 50% of cases
- Autoimmune: Giant cell myocarditis with <20% 5-year survival
- Acute phase: >14 lymphocytes/mm² on endomyocardial biopsy
- Chronic phase: fibrosis >25% with persistent inflammation
- Fulminant: cardiogenic shock within <2 weeks of symptoms
-
Pericarditis (viral etiology in 80-90% of cases)
- Acute: chest pain with friction rub and ST elevation
- Chronic: >3 months duration with recurrent episodes
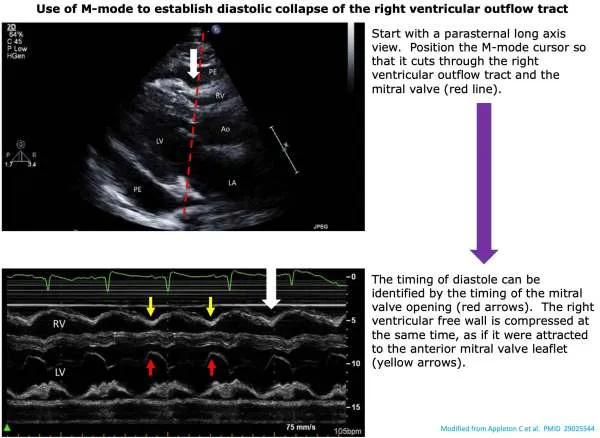
- Constrictive: equalization of diastolic pressures
- Effusive: >20 mm echo-free space around heart
-
Endocarditis (blood culture positive in 85% of cases)
- Acute: S. aureus with rapid valve destruction
- Subacute: Viridans streptococci with indolent course
- Native valve: mortality 15-25% despite treatment
- Prosthetic valve: mortality 25-40% with surgical urgency
📌 Remember: INFLAME criteria for myocarditis - Infiltrate (lymphocytic), Necrosis (myocyte), Fibrosis (interstitial), Left ventricular dysfunction, Arrhythmias, Markers elevated (troponin), Echocardiographic changes. >14 lymphocytes/mm² confirms diagnosis on endomyocardial biopsy.
| Inflammatory Disease | Primary Pathogen | Diagnostic Criteria | Treatment Duration | Mortality Rate | Recurrence Risk |
|---|---|---|---|---|---|
| Viral Myocarditis | Coxsackievirus B | Troponin + MRI | 3-6 months | 5-10% | 10-15% |
| Giant Cell Myocarditis | Autoimmune | Biopsy required | Lifelong | >80% | High |
| Acute Pericarditis | Viral/Idiopathic | Clinical + ECG | 2-4 weeks | <1% | 20-30% |
| Bacterial Endocarditis | S. aureus | Blood cultures + echo | 4-6 weeks | 15-25% | 5-10% |
| Constrictive Pericarditis | Post-surgical | Catheterization | Surgical | 5-15% | Rare |
💡 Master This: Inflammatory cardiac diseases create distinct histological signatures. Lymphocytic infiltrates indicate viral myocarditis, giant cells suggest autoimmune disease, and neutrophilic infiltrates point to bacterial infection. Endomyocardial biopsy remains gold standard for myocarditis diagnosis with >95% specificity when >14 lymphocytes/mm² are present.

Understanding inflammatory patterns provides the foundation for recognizing how structural heart diseases develop through different pathophysiological mechanisms.
🔥 Inflammatory Cardiac Diseases: The Immune System's Cardiac Assault
🏗️ Structural Heart Disease: The Architecture Under Siege
Structural Disease Categories
-
Valvular Diseases (2-7% population prevalence)
- Aortic stenosis: valve area <1.0 cm² with mean gradient >40 mmHg
- Mitral regurgitation: regurgitant volume >60 mL per beat
- Degenerative: myxomatous degeneration in 2% of population
- Functional: annular dilatation with >40 mm diameter
- Rheumatic: commissural fusion with restricted mobility
-
Cardiomyopathies (1:500 population prevalence)
- Hypertrophic: septal thickness >15 mm with dynamic obstruction
- Dilated: ejection fraction <40% with LV diameter >55 mm
- Ischemic: >75% due to coronary artery disease
- Non-ischemic: genetic mutations in 40% of cases
- Toxic: anthracycline-induced with dose-dependent risk
-
Congenital Defects (8 per 1000 live births)
- Simple: ASD, VSD, PDA with left-to-right shunts
- Complex: Tetralogy of Fallot with 4 anatomical components
- Pulmonary stenosis with gradient >50 mmHg
- Ventricular septal defect >1 cm diameter
- Overriding aorta with >50% override
- Right ventricular hypertrophy >15 mm wall thickness
📌 Remember: VALVE assessment parameters - Velocity (peak >4 m/s severe AS), Area (effective orifice <1.0 cm² severe), Left ventricular response (hypertrophy >15 mm), Volume overload (regurgitant >60 mL), Ejection fraction (preserved vs reduced). Each parameter has specific thresholds for severity grading.
| Structural Disease | Key Measurement | Severe Threshold | Surgical Indication | 5-Year Survival | Complication Rate |
|---|---|---|---|---|---|
| Aortic Stenosis | Valve Area | <1.0 cm² | Symptoms + severe AS | >95% | <3% |
| Mitral Regurgitation | Regurgitant Volume | >60 mL | EF <60% or ESD >40mm | >90% | <5% |
| Hypertrophic CMP | Septal Thickness | >15 mm | Gradient >50 mmHg | >95% | <2% |
| Dilated CMP | Ejection Fraction | <35% | Heart failure symptoms | Variable | Variable |
| Tetralogy of Fallot | RV/LV Pressure | >0.7 | Cyanosis or symptoms | >90% | 10-15% |
💡 Master This: Structural heart diseases follow predictable remodeling patterns. Pressure overload creates concentric hypertrophy (thick walls, small cavity), while volume overload produces eccentric hypertrophy (thin walls, large cavity). Understanding these geometric adaptations enables precise hemodynamic assessment and optimal timing of surgical interventions.

Recognizing structural patterns establishes the framework for understanding how these anatomical changes create specific clinical presentations requiring targeted diagnostic approaches.
🏗️ Structural Heart Disease: The Architecture Under Siege
🎯 Diagnostic Pattern Recognition: Decoding the Cardiac Clues
Clinical Presentation Patterns
-
Chest Pain Syndromes (8 million ED visits annually)
- Typical angina: substernal pressure with exertional trigger and nitroglycerin relief
- Atypical angina: 2 of 3 typical characteristics present
- Location: substernal, left arm, jaw radiation
- Quality: pressure, squeezing, heaviness sensation
- Duration: 2-10 minutes with crescendo-decrescendo pattern
- Triggers: exertion, emotion, cold exposure
-
Heart Failure Presentations (6.5 million Americans affected)
- Acute decompensation: rapid onset over hours to days
- Chronic progression: gradual decline over months to years
- NYHA Class I: no symptoms with ordinary activity
- NYHA Class II: slight limitation with ordinary activity
- NYHA Class III: marked limitation with less than ordinary activity
- NYHA Class IV: symptoms at rest or minimal exertion
-
Arrhythmia Patterns (>2.7 million Americans with AFib)
- Paroxysmal: self-terminating within 7 days
- Persistent: sustained >7 days requiring intervention
- Rate control: target <110 bpm for asymptomatic patients
- Rhythm control: cardioversion within 48 hours or anticoagulation

📌 Remember: HEART score for chest pain risk stratification - History (0-2 points), ECG (0-2 points), Age (0-2 points), Risk factors (0-2 points), Troponin (0-2 points). Score 0-3 = <2% risk, Score 4-6 = 12-65% risk, Score 7-10 = >65% risk of 30-day MACE.
| Diagnostic Test | Sensitivity | Specificity | Positive Predictive Value | Negative Predictive Value | Time to Result |
|---|---|---|---|---|---|
| Troponin I | >95% | >90% | Variable | >99% | <1 hour |
| ECG | 70-80% | >95% | >90% | 85% | <5 minutes |
| Stress Echo | 85% | 80% | 85% | 80% | 45 minutes |
| Coronary CTA | >95% | 85% | Variable | >99% | 30 minutes |
| BNP | 90% | 75% | Variable | >95% | <30 minutes |
💡 Master This: Diagnostic pattern recognition combines pretest probability assessment with systematic test interpretation. Bayesian reasoning guides test selection where high pretest probability requires high specificity tests, while low pretest probability needs high sensitivity tests. Understanding test characteristics prevents diagnostic errors and optimizes resource utilization.
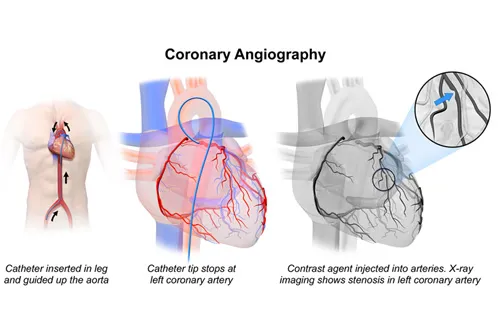
Mastering diagnostic patterns creates the foundation for developing evidence-based treatment algorithms that optimize patient outcomes through targeted interventions.
🎯 Diagnostic Pattern Recognition: Decoding the Cardiac Clues
⚕️ Treatment Algorithms: The Therapeutic Precision Matrix
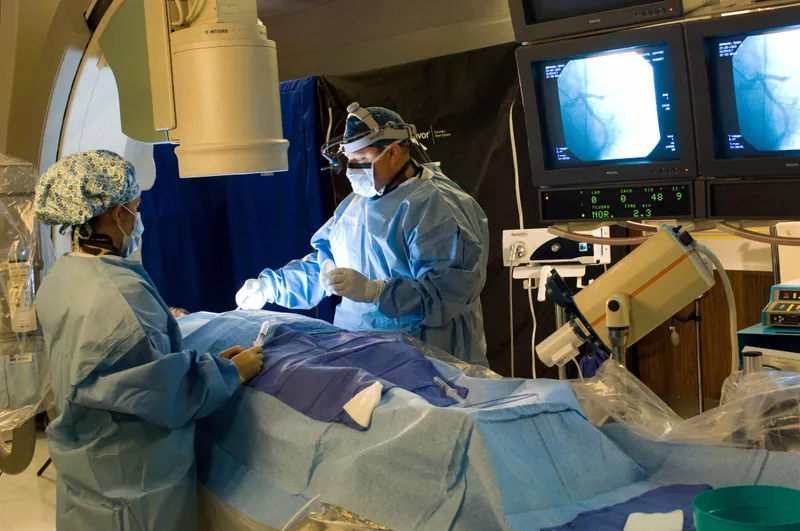
Acute Coronary Syndrome Management
-
STEMI Treatment Protocols (door-to-balloon <90 minutes)
- Primary PCI: >95% reperfusion success with <3% mortality
- Fibrinolytic therapy: 60-80% reperfusion with 6-7% mortality
- Contraindications: active bleeding, stroke <3 months, surgery <2 weeks
- Rescue PCI: indicated if <50% ST resolution at 90 minutes
- Transfer protocols: door-to-balloon <120 minutes including transport
-
NSTEMI/UA Management (risk-stratified approach)
- High-risk: TIMI score ≥5 or GRACE score >140
- Invasive strategy: catheterization within 24 hours
- Eptifibatide: bolus 180 mcg/kg then 2 mcg/kg/min infusion
- Bivalirudin: 0.75 mg/kg bolus then 1.75 mg/kg/hr infusion
- Clopidogrel: 600 mg loading then 75 mg daily
-
Heart Failure Treatment Algorithms (guideline-directed medical therapy)
- ACE inhibitors: target dose or maximum tolerated
- Beta-blockers: start low, go slow with target heart rate 60-70 bpm
- Metoprolol: start 12.5 mg BID, target 200 mg BID
- Carvedilol: start 3.125 mg BID, target 25-50 mg BID
- Bisoprolol: start 1.25 mg daily, target 10 mg daily
📌 Remember: MONA-BASH for acute MI management - Morphine (if needed), Oxygen (if SpO2 <90%), Nitroglycerin (avoid if RV infarct), Aspirin (162-325 mg), Beta-blocker (if no contraindications), ACE inhibitor (start within 24 hours), Statin (high-intensity), Heparin (unfractionated or LMWH).
| Treatment Strategy | Target Population | Primary Endpoint | NNT | Mortality Benefit | Major Bleeding Risk |
|---|---|---|---|---|---|
| Primary PCI | STEMI <12 hours | Reperfusion | 33 | 2-3% absolute | <1% |
| Dual Antiplatelet | ACS patients | Recurrent MI | 67 | 1.5% absolute | 2-4% |
| ACE Inhibitor | Post-MI, HF | CV death | 50 | 2% absolute | Rare |
| Beta-blocker | Post-MI | Sudden death | 84 | 1.2% absolute | Rare |
| High-intensity Statin | ACS | MACE | 74 | 1.4% absolute | <0.1% |
💡 Master This: Treatment algorithms optimize outcomes through systematic risk-benefit analysis. Number needed to treat (NNT) quantifies therapeutic benefit where lower NNT indicates greater efficacy. Dual antiplatelet therapy prevents 1 recurrent MI for every 67 patients treated but causes major bleeding in 2-4%. Understanding these trade-offs enables personalized treatment decisions.
Treatment algorithm mastery provides the foundation for understanding how multiple cardiac conditions interact and require integrated management approaches.
⚕️ Treatment Algorithms: The Therapeutic Precision Matrix
🌐 Advanced Integration: The Cardiac Pathology Synthesis
Multi-System Cardiac Interactions
-
Cardio-Renal Syndrome (>40% of heart failure patients)
- Type 1: acute heart failure causing acute kidney injury
- Type 2: chronic heart failure leading to chronic kidney disease
- Mechanism: reduced renal perfusion + venous congestion
- Biomarkers: creatinine rise >0.3 mg/dL within 48 hours
- Treatment: ultrafiltration removing >500 mL/hour excess fluid
- Prognosis: doubled mortality when both organs involved
-
Cardio-Oncology Interactions (emerging subspecialty)
- Anthracycline cardiotoxicity: dose-dependent with >250 mg/m² threshold
- Trastuzumab-induced cardiomyopathy: reversible in >80% of cases
- Monitoring: LVEF assessment every 3 months during treatment
- Prevention: dexrazoxane reduces cardiotoxicity by 65%
- Management: ACE inhibitors + beta-blockers for LV dysfunction
-
Metabolic-Cardiac Connections (diabetes + CVD)
- Diabetic cardiomyopathy: independent of coronary artery disease
- SGLT2 inhibitors: 35% reduction in heart failure hospitalizations
- Mechanism: natriuresis + improved energetics + reduced inflammation
- Benefits: evident within 3 months of treatment initiation
📌 Remember: CARDIAC multi-system assessment - Cardio-renal (creatinine trends), Arrhythmia burden (Holter monitoring), Respiratory status (BNP levels), Diabetic control (HbA1c targets), Inflammatory markers (CRP, ESR), Anticoagulation needs (bleeding vs thrombosis risk), Cancer therapy effects (cardiotoxicity screening).
| Integration Domain | Key Biomarker | Monitoring Frequency | Intervention Threshold | Outcome Improvement | Cost-Effectiveness |
|---|---|---|---|---|---|
| Cardio-Renal | Creatinine | Every 48 hours | >0.3 mg/dL rise | 25% mortality reduction | High |
| Cardio-Oncology | Troponin | Every 3 months | >ULN elevation | 80% reversibility | Moderate |
| Diabetes-CVD | HbA1c | Every 3 months | >7% target | 35% HF reduction | Very High |
| Heart-Lung | BNP | Monthly | >400 pg/mL | 30% readmission reduction | High |
| Inflammation | CRP | As indicated | >3 mg/L | Variable | Low |
💡 Master This: Advanced cardiac pathology requires systems thinking where single interventions affect multiple organ systems. SGLT2 inhibitors demonstrate pleiotropic effects beyond glucose control, providing cardiovascular benefits through natriuresis, improved cardiac energetics, and reduced inflammation. Understanding these multi-system interactions enables precision medicine approaches that optimize outcomes across multiple domains simultaneously.
This advanced integration framework establishes the foundation for developing rapid mastery tools that synthesize complex cardiac pathology into actionable clinical knowledge.
🌐 Advanced Integration: The Cardiac Pathology Synthesis
🎯 Cardiac Pathology Mastery: The Clinical Command Center
Essential Clinical Arsenal
-
Rapid Assessment Framework (<5 minute evaluation)
- History: chest pain characteristics, timing, triggers, relief factors
- Physical: vital signs, heart sounds, peripheral perfusion, JVD assessment
- S3 gallop: >90% sensitivity for heart failure with EF <40%
- S4 gallop: indicates diastolic dysfunction with preserved EF
- Murmur grading: Grade 4-6 indicates severe valvular disease
- Pulsus paradoxus: >20 mmHg suggests cardiac tamponade
-
Diagnostic Hierarchy (evidence-based prioritization)
- ECG: first-line for acute presentations with <2 minute interpretation
- Troponin: rule-out MI with high-sensitivity assays at 0 and 1 hour
- Echocardiogram: structural assessment with real-time hemodynamics
- Advanced imaging: cardiac MRI for tissue characterization
- Invasive testing: catheterization for definitive coronary assessment
-
Treatment Prioritization Matrix (time-sensitive interventions)
- Immediate (<15 minutes): STEMI, cardiogenic shock, cardiac arrest
- Urgent (<2 hours): NSTEMI, acute heart failure, unstable arrhythmias
- Semi-urgent (<24 hours): stable angina, chronic heart failure
- Elective (days-weeks): routine follow-up, risk factor modification
📌 Remember: CARDIAC mastery checklist - Clinical assessment (history + physical), Acute interventions (time-sensitive), Risk stratification (evidence-based), Diagnostic testing (systematic), Imaging interpretation (structured), Advanced therapies (guideline-directed), Continuous monitoring (outcome-focused). Each element has specific timeframes and measurable endpoints.
| Clinical Scenario | Time to Diagnosis | Key Diagnostic Test | Treatment Window | Success Rate | Mortality Reduction |
|---|---|---|---|---|---|
| STEMI | <10 minutes | ECG | <90 minutes | >95% | 50% relative |
| Cardiogenic Shock | <30 minutes | Echo + Swan-Ganz | <60 minutes | Variable | 30% absolute |
| Acute Heart Failure | <60 minutes | BNP + Echo | <4 hours | >90% | 20% relative |
| Cardiac Tamponade | <15 minutes | Echo | <30 minutes | >95% | Life-saving |
| Aortic Dissection | <30 minutes | CT Angiography | <2 hours | >90% | 40% relative |
💡 Master This: Cardiac pathology mastery requires integration of anatomical knowledge, pathophysiological understanding, clinical correlation, and therapeutic expertise. Expert practitioners develop mental models that enable rapid pattern recognition, accurate risk stratification, and optimal treatment selection. This cognitive framework transforms complex clinical scenarios into manageable decision trees with predictable outcomes and measurable success rates.
🎯 Cardiac Pathology Mastery: The Clinical Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















