Implant Basics & Biocompatibility - Host Hugs
- Implant Materials:
- Metals: Titanium (Ti) & alloys, Cobalt-Chromium (Co-Cr), Stainless Steel.
- Polymers: Ultra-High-Molecular-Weight Polyethylene (UHMWPE), Polymethylmethacrylate (PMMA).
- Ceramics: Alumina, Zirconia, Hydroxyapatite (HA).
- Composites: e.g., Carbon-fiber reinforced PEEK.
- Fundamental Properties:
- Biocompatibility: Material performs with appropriate host response; no toxicity, injury, or immune reaction.
- Osseointegration: Direct bone-to-implant structural & functional connection, no intervening soft tissue layer.
- Surface Characteristics: Topography, chemistry, wettability critically affect cellular responses & integration.
- Host Tissue Reactions:
- Initial: Acute inflammation, protein adsorption onto implant surface.
- Foreign Body Reaction (FBR): Chronic phase with macrophages, foreign body giant cells (FBGCs), leading to fibrous tissue encapsulation.
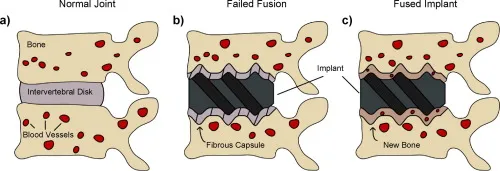
⭐ Titanium and its alloys are widely favored for orthopedic implants due to their excellent biocompatibility, osseointegration, and corrosion resistance.
Aseptic Loosening - Silent Sabotage
- Most common cause of late Total Joint Arthroplasty (TJA) failure; non-infectious.
- Pathogenesis: Wear particles → macrophage activation → cytokine release (TNF-α, IL-1, RANKL) → osteoclastogenesis → periprosthetic osteolysis → implant loosening.
- 📌 PMCOL: Particles → Macrophage activation → Cytokine release → Osteoclast activation/osteolysis → Loosening.
- Wear Debris Types:
- Polyethylene (UHMWPE): Most common, highly osteolytic.
- Metal (Co-Cr, Ti): Metallosis, ALVAL (Aseptic Lymphocyte-dominated Vasculitis-Associated Lesions).
- Ceramic: Inert, low osteolysis; risk of fracture.
- PMMA (cement): Particulate debris contributes.
- Clinical: Insidious onset pain, instability, ↓Range of Motion (ROM).
- Radiology: Radiolucent lines >2mm at interface, component migration/subsidence.
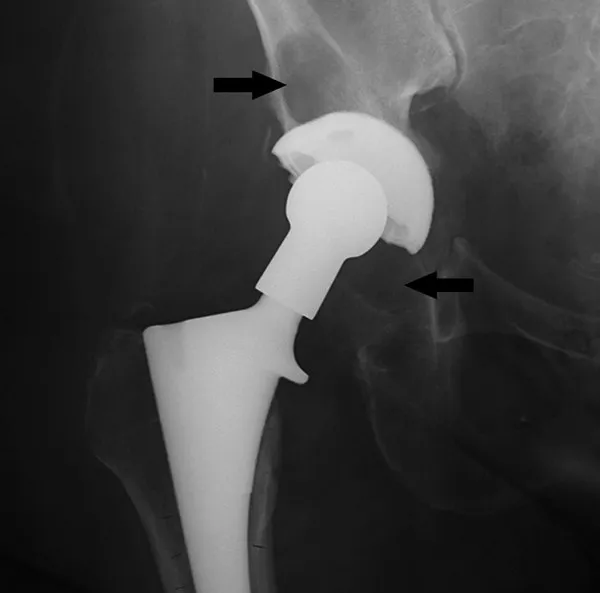
- Histology: Synovial-like interface membrane (SLIM) with macrophages, giant cells, lymphocytes, wear particles.
⭐ Particle-induced osteolysis, driven by macrophage activation (TNF-α, IL-1, RANKL), is the primary mechanism behind aseptic loosening of joint replacements.
Implant Infections - Bug Battles
⭐ Biofilm formation on implant surfaces, commonly by Staphylococcus aureus or Staphylococcus epidermidis, is a critical factor in the pathogenesis and persistence of periprosthetic joint infections (PJI).
- Routes & Timing of Infection:
- Early onset (<3 months post-op): Often high-virulence organisms (e.g., S. aureus, Gram-negatives); direct contamination.
- Delayed onset (3-24 months): Low-virulence organisms (e.g., CoNS, C. acnes); often perioperative seeding.
- Late onset (>24 months): Haematogenous spread from distant infection site.
- Common Pathogens:
- Staphylococcus aureus (most common overall)
- Coagulase-negative Staphylococci (S. epidermidis)
- Streptococci, Enterococci
- Gram-negative rods (e.g., Pseudomonas aeruginosa)
- Host Response & Diagnosis:
- Inflammation, osteolysis, implant loosening.
- Diagnosis: Musculoskeletal Infection Society (MSIS) criteria (synovial fluid WBC count >3000/µL, PMN% >80%, positive cultures).
Material-Specific Pathology - Metal & Poly Woes
- Metal Implants (e.g., Co-Cr, Ti alloys):
- Hypersensitivity: Type IV (Nickel, Cobalt, Chromium). Symptoms: pain, loosening.
- Metallosis: Grey-black tissue; macrophage response to debris.
- Corrosion (fretting, crevice) → ion/particle release.
- ALVAL: With Metal-on-Metal (MoM) implants.
- Polyethylene (UHMWPE) Wear:
- Particle-induced osteolysis ("Polyethylene Disease"): Macrophages phagocytose particles (0.1-1 µm most reactive); release cytokines (TNF-α, IL-1) → osteoclast activation → bone loss.
- Polymethylmethacrylate (PMMA) Bone Cement:
- Aseptic loosening: Interface failure, debris.
- Monomer toxicity: Local necrosis if uncured.
- Third-body wear: Fragments abrade surfaces.
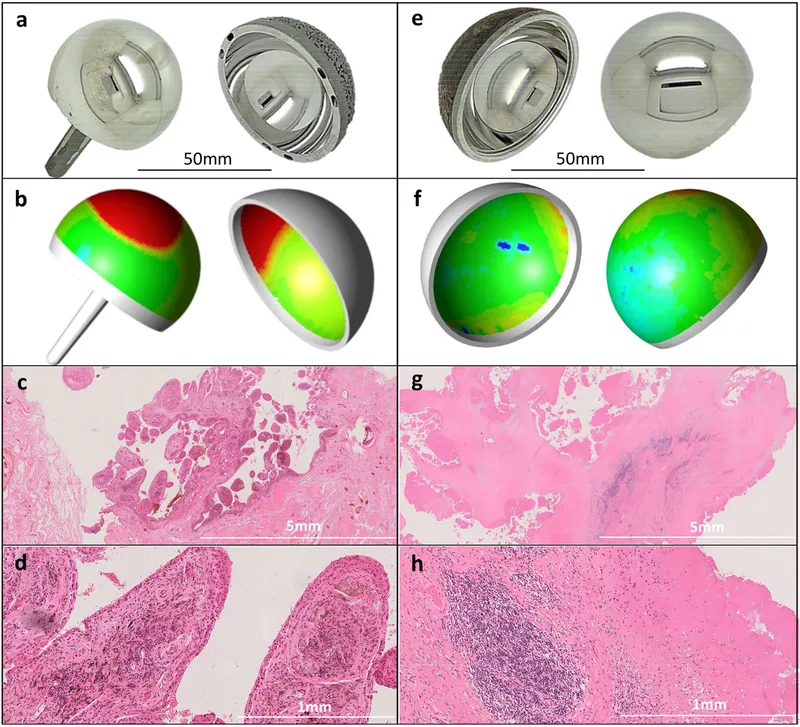
⭐ Aseptic Lymphocyte-Dominated Vasculitis-Associated Lesion (ALVAL) is a specific Type IV hypersensitivity reaction associated with metal-on-metal (especially Co-Cr alloy) hip implants, characterized by perivascular lymphocytic infiltrates.
High‑Yield Points - ⚡ Biggest Takeaways
- Aseptic loosening: Most common failure, due to wear particle-induced osteolysis.
- Periprosthetic infection: Second most common; biofilms (S. aureus) are key.
- Particle disease: Macrophage response to debris (e.g., polyethylene) causing bone loss.
- Metallosis: Reaction to metal debris (MoM implants), may cause pseudotumors (ALVAL).
- Implant fracture and failed osteointegration are other important failure mechanisms.
- PMMA cement debris can induce inflammation and third-body wear.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

