Osteomyelitis: The Basics - Bone Under Siege
- Definition: Inflammation of bone & marrow, primarily infection-driven.
- Etiology:
- Most common: Staphylococcus aureus.
- Neonates: Group B Strep, E. coli.
- Sickle cell: Salmonella spp. (📌 Sickle cell - Salmonella)
- IVDU: Pseudomonas, S. aureus.
- Routes of Infection:
- Hematogenous: Children (long bone metaphysis), adults (vertebrae).
- Contiguous: Trauma, surgery, ulcers.
- Direct: Open fractures.
- Classification (Duration):
- Acute: < 2 weeks.
- Chronic: > 6 weeks or relapse.
- Key Pathological Features:
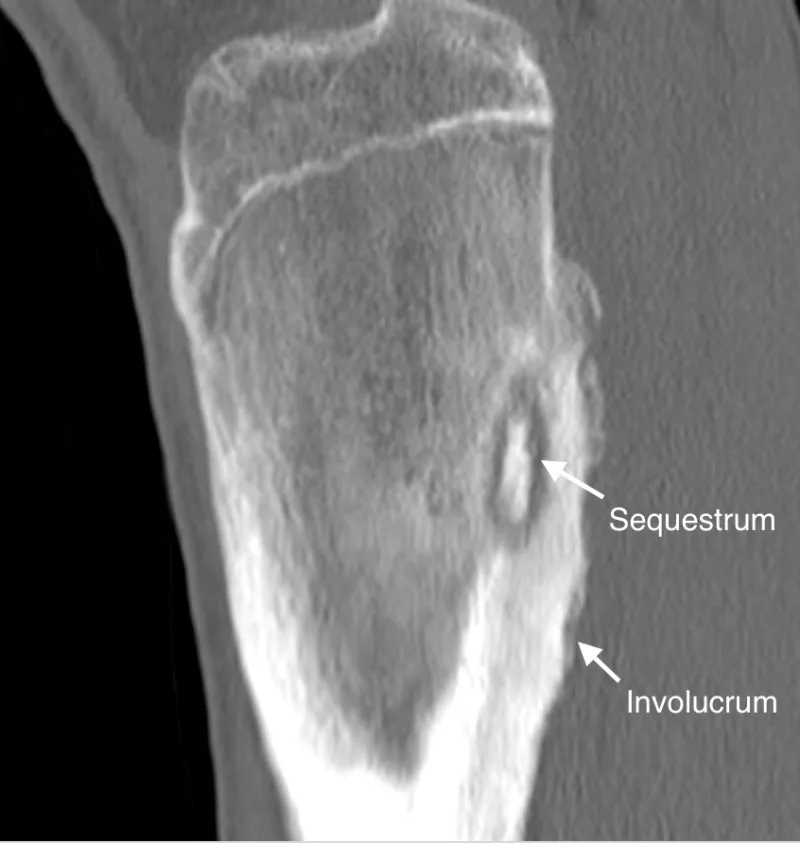
- Sequestrum: Necrotic bone.
- Involucrum: New periosteal bone.
- Cloaca: Sinus tract.
- Brodie's Abscess: Chronic localized abscess.
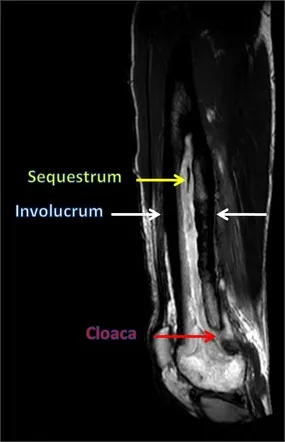 ⭐ > In children, hematogenous osteomyelitis typically targets long bone metaphysis due to its unique vascularity (sluggish sinusoidal flow).
⭐ > In children, hematogenous osteomyelitis typically targets long bone metaphysis due to its unique vascularity (sluggish sinusoidal flow).
Pathogens & Pathways - Invaders & Inroads
- Key Pathogens:
- Staphylococcus aureus: Most frequent.
- Neonates: Grp B Strep, E. coli.
- Sickle Cell Disease: Salmonella spp.
- IV Drug Users (IVDU): Pseudomonas aeruginosa, S. aureus.
- Prosthetic Joints: S. epidermidis.
- Puncture Wounds (foot): Pseudomonas aeruginosa.
- Vertebral (Pott's Disease): Mycobacterium tuberculosis.
- Invasion Routes:
- Hematogenous: Children (metaphysis), adult vertebrae. Via metaphyseal capillary loops.
- Contiguous Spread: From adjacent infections (e.g., diabetic foot ulcers).
- Direct Implantation: Trauma, open fractures, surgery.
- Pathogenesis Unveiled:
- Bacterial invasion → Acute inflammation, suppuration.
- → ↑Intraosseous pressure & vascular occlusion.
- → Ischemic necrosis → Sequestrum (avascular bone fragment).
- → Periosteal reaction → Involucrum (new bone surrounding sequestrum). 📌 Sequestrum (dead) 'sequestered' by Involucrum (new).
- → Chronic: Draining sinus, Brodie's abscess.
⭐ Salmonella osteomyelitis is a classic association with Sickle Cell Disease due to factors like vaso-occlusion causing bone infarcts and impaired phagocytosis.
Signs, Symptoms & Sleuthing - Cracking the Case
- Clinical Picture:
- Acute: Fever, intense localized bone pain, warmth, swelling, ↓ limb use.
- Chronic: Persistent dull pain, sinus tract (pus discharge), recurrent flares.
- Lab Markers:
- ↑ WBC, ↑ ESR (often >70 mm/hr), ↑ CRP (monitors therapy).
- Blood cultures: Positive in ~50% acute cases.
- Imaging Insights:
- X-ray: Early changes subtle (10-14 days); later: periosteal reaction, sequestrum.
- MRI: Gold standard for early detection; shows marrow edema, abscess.
- CT: Details cortical destruction, sequestra.
- Bone Scan: Sensitive, not specific.
- Definitive Diagnosis:
- Bone biopsy (histopathology & culture) is crucial.
⭐ Sequestrum (dead bone) and Involucrum (new bone formation around sequestrum) are hallmark radiological signs of chronic osteomyelitis.
Special Forms & Fixes - Variants & Victory
- Key Variants:
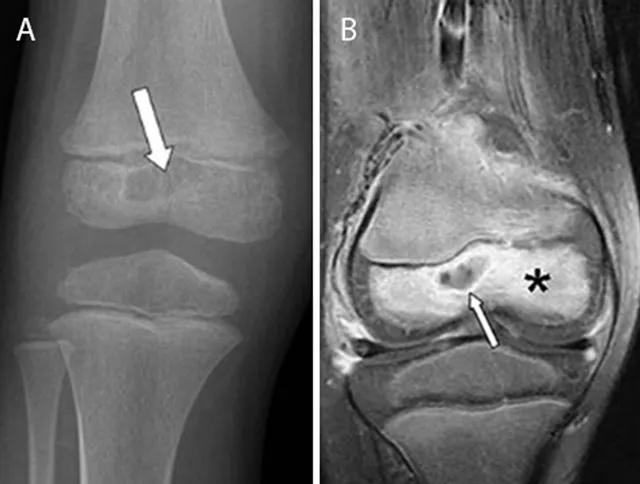
- Brodie's Abscess: Chronic, localized intraosseous abscess. X-ray: lucent nidus, sclerotic rim. Tibia common.

- Garré's Sclerosing Osteomyelitis: Chronic, non-suppurative, prominent periosteal reaction (onion-skin). Mandible.
- Tuberculous Osteomyelitis (Pott's Disease): Spine common. Cold abscess. Phemister's triad (osteoporosis, erosions, ↓joint space).
- Vertebral Osteomyelitis: S. aureus common. Back pain, fever, ↑ESR/CRP.
- Brodie's Abscess: Chronic, localized intraosseous abscess. X-ray: lucent nidus, sclerotic rim. Tibia common.
- Core Management:
- Surgical debridement (sequestrectomy).
- Targeted antibiotics: IV 4-6 weeks, then prolonged oral.
- Stabilization.
- Outcomes & Pitfalls:
- Chronic recurrence, pathological fractures, septic arthritis.
- Growth disturbances (children).
- Secondary Amyloidosis (AA).
⭐ Marjolin's Ulcer: SCC in chronic sinus. Biopsy non-healing ulcers highly suspicious, especially if >10 years history of osteomyelitis drainage.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of osteomyelitis is Staphylococcus aureus.
- Salmonella is characteristic in sickle cell disease patients.
- Pseudomonas aeruginosa is common in IV drug users and puncture wounds through shoes.
- Tuberculous osteomyelitis (Pott's disease) typically affects the spine, causing vertebral collapse and kyphosis.
- Brodie's abscess: chronic, localized osteomyelitis, often in metaphysis.
- Sequestrum (dead bone) & involucrum (new bone) are hallmarks of chronic osteomyelitis.
- MRI is most sensitive imaging for early diagnosis of acute osteomyelitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

