Tendon & Fascia Basics - The Body's Tethers
- Tendons: Dense connective tissue; connect muscle to bone; transmit tensile forces.
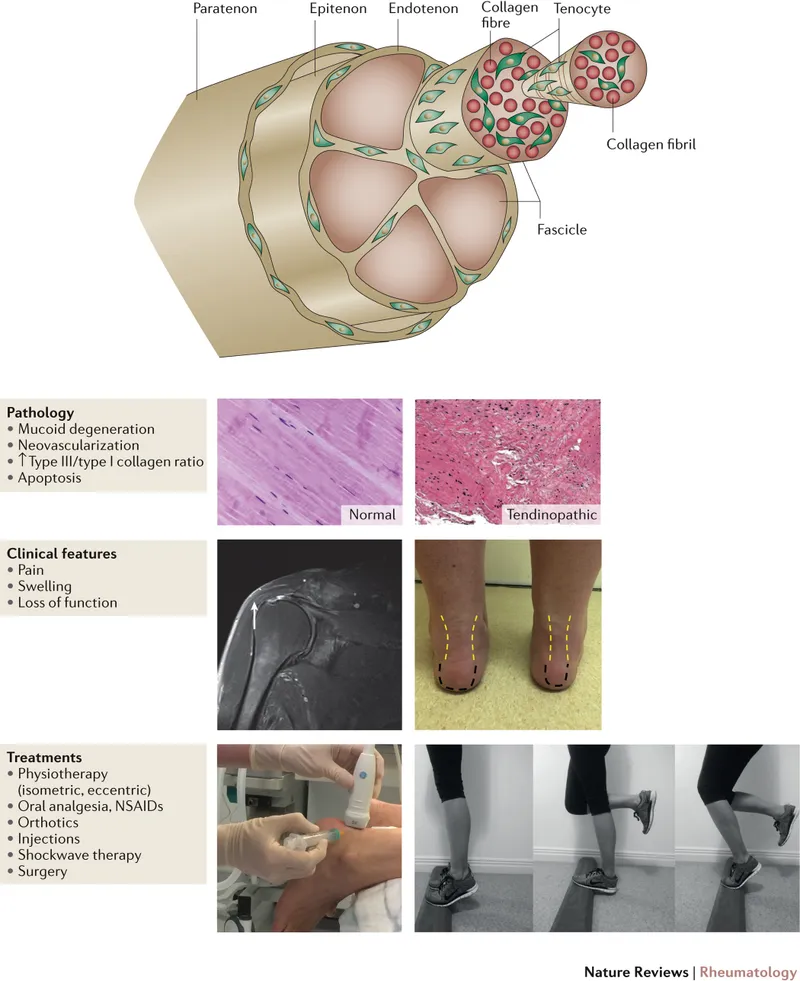
- Structure: Parallel collagen fibers (primarily Type I), fibroblasts (tenocytes), proteoglycans.
- Blood Supply: Limited, mainly at musculotendinous & osteotendinous junctions.
- Fascia: Sheets of connective tissue; envelop muscles, organs, vessels.
- Types: Superficial, deep, visceral.
- Function: Support, compartmentalization, force transmission.

⭐ Tendons are predominantly composed of Type I collagen, providing high tensile strength.
- Innervation: Sensory nerves for proprioception and nociception (pain).
General Tendinopathies - Strained Strands Saga
-
Tendinopathy: Umbrella term for tendon disorders, often from overuse or repetitive microtrauma.
-
Pathogenesis: Imbalance between tendon matrix degeneration & synthesis.
- Failed healing response leads to chronic changes.
-
Spectrum of Tendon Injury:
- Reactive Tendinopathy: Acute overload, non-inflammatory proliferative response, tendon thickening. Reversible.
- Tendon Dysrepair: Attempted healing, ↑ proteoglycans, collagen disorganization, neurovascular ingrowth. Possible reversibility.
- Degenerative Tendinopathy (Tendinosis): Chronic, cell death, matrix breakdown, extensive disorganization, minimal inflammation. Less reversible.
⭐ Tendinosis is a degenerative process characterized by collagen disorganization, increased ground substance, and neovascularization, distinct from primarily inflammatory tendinitis.
- Clinical: Pain with activity, localized tenderness, palpable nodule (in tendinosis).
- Histology:
- Tendinitis: Acute inflammation (neutrophils, macrophages). Rare in chronic cases.
- Tendinosis: Collagen fiber disarray (Type III > Type I), ↑ ground substance (mucoid degeneration), neovascularization, hypercellularity (tenocytes, myofibroblasts), no significant inflammation.
- Common sites: Achilles, patellar, rotator cuff, elbow (epicondylitis).
Fascial Pathologies - Fascia's Fierce Fight
- Plantar Fasciitis:
- Etiology: Repetitive microtrauma (e.g., running), obesity, improper footwear.
- Pathology: Plantar fascia degeneration (calcaneal origin); fibroblastic proliferation, collagen disarray.
- Clinical: Heel pain (worse AM/after rest); medial calcaneal tenderness.
- Dupuytren's Contracture (Palmar Fibromatosis):
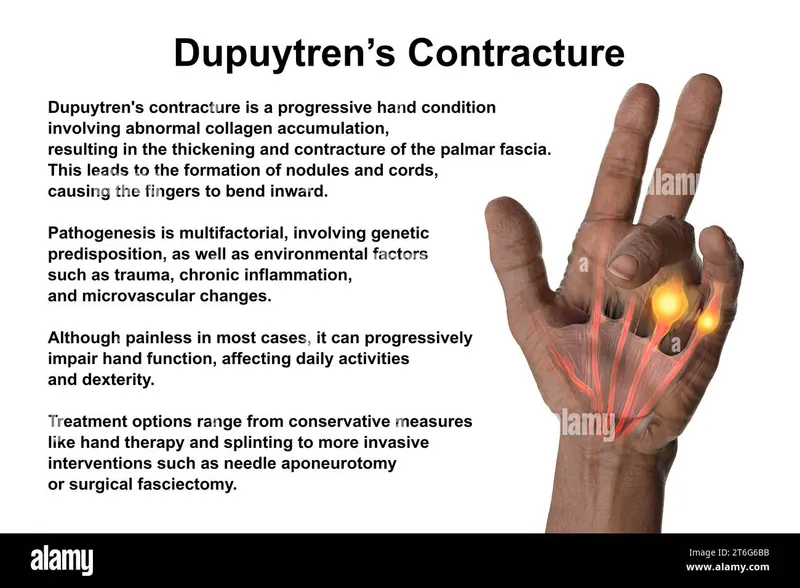
- Pathogenesis: Palmar fascia thickens: nodules → cords → contractures.
⭐ Dupuytren's contracture is characterized by palmar fascial thickening due to proliferation of myofibroblasts and altered collagen (increased Type III).
- Clinical: Painless palmar nodules, progressive flexion contractures (typically 4th & 5th digits, MCP/PIP). Positive "tabletop test".
- Associations: Northern European, alcohol, smoking, DM, epilepsy. 📌 "Dupuytren's: Digits Draw Down"
- Ledderhose Disease (Plantar Fibromatosis):
- Plantar foot nodules; like Dupuytren's but in feet. May be painful.
- Plantar foot nodules; like Dupuytren's but in feet. May be painful.
Specific Tendon Syndromes - Spotlight on Sorrows
- Achilles Tendinopathy: Overuse; pain posterior heel/calf. ↑Risk: fluoroquinolones. Degeneration.
- Rotator Cuff Tears: Supraspinatus (abduction initiation) common. Pain on abduction/overhead. Drop arm test +.
- Lateral Epicondylitis (Tennis Elbow): Extensor Carpi Radialis Brevis origin. Pain lateral elbow, wrist extension.
- Medial Epicondylitis (Golfer's Elbow): Common flexor-pronator origin. Pain medial elbow, wrist flexion.
- De Quervain's Tenosynovitis: Abductor Pollicis Longus (APL) & Extensor Pollicis Brevis (EPB) tendons (1st dorsal compartment).
⭐ Finkelstein's test (passive ulnar deviation of wrist, thumb flexed in palm) is pathognomonic for De Quervain's tenosynovitis.
- Ganglion Cyst: Mucin-filled synovial cyst (often wrist). Transilluminates. Usually asymptomatic.
High‑Yield Points - ⚡ Biggest Takeaways
- Tendinopathy is primarily degenerative due to failed healing, not inflammatory.
- De Quervain's tenosynovitis affects APL & EPB tendons; Finkelstein test is key.
- Trigger finger (stenosing tenosynovitis): A1 pulley thickening causes digit locking.
- Dupuytren's contracture: Palmar fibromatosis (nodules, cords); common in Northern Europeans, associated with diabetes, alcoholism.
- Ganglion cyst: Mucinous degeneration near joints or tendon sheaths; transilluminates.
- Achilles tendinopathy: Common overuse injury; pain at mid-portion or calcaneal insertion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


