Spinal Trauma - Pillar Talk
- Vertebral Column: 7 Cervical (C), 12 Thoracic (T), 5 Lumbar (L), 5 Sacral (S-fused), 4 Coccygeal (Co-fused).
- Ligaments: Anterior Longitudinal (ALL), Posterior Longitudinal (PLL), Ligamentum Flavum, Interspinous, Supraspinous.
- Spinal Stability (Denis 3-Column Theory):
- Anterior: ALL, anterior ½ vertebral body & disc.
- Middle: posterior ½ vertebral body & disc, PLL.
- Posterior: Pedicles, facets, lamina, spinous processes, posterior ligaments.
- Injury to ≥2 columns = Unstable.
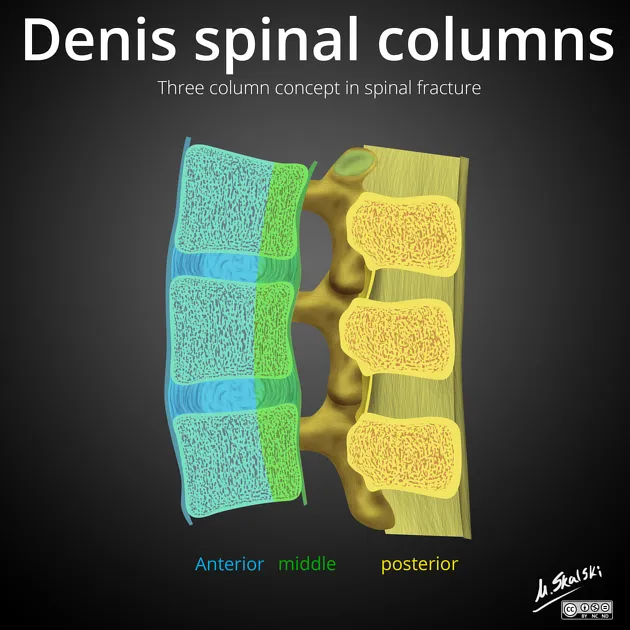
⭐ Middle column involvement is the most critical determinant of instability in Denis' classification; its disruption often implies significant ligamentous and bony damage, leading to a high risk of neurological injury.
Spinal Trauma - Nerve Navigator
- Primary Survey (ATLS): ABCDE. Maintain spinal immobilization (log-roll).
- Neurological Assessment:
- Motor: Key muscles (MRC 0-5).
- Sensory: Key dermatomes (pinprick, light touch).
- Reflexes: DTRs, Bulbocavernosus Reflex (BCR), Anal wink.
- ASIA Impairment Scale: A (Complete) to E (Normal).
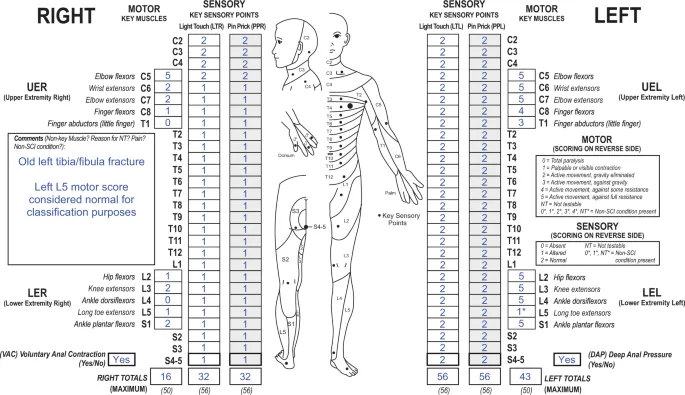
- Differentiating Shock:
- Spinal Shock: Transient loss of spinal reflexes below injury. Flaccid paralysis, areflexia. BCR return signals end.
- Neurogenic Shock: Sympathetic chain disruption (lesions ≥T6). Triad: Hypotension, Bradycardia, Hypothermia (peripheral vasodilation).
⭐ In Neurogenic Shock, hypotension occurs with bradycardia (or normal heart rate), unlike hypovolemic shock which presents with tachycardia due to blood loss and sympathetic response.
Spinal Trauma - Snap & Spot
-
Imaging:
- X-ray: Initial screen. AP/Lateral/Odontoid views. Swimmer's (C7-T1). Flex-Ex for stability (use cautiously).
- CT: Gold standard for complex bone/fractures. Use if X-ray abnormal/inadequate, high-energy trauma, neuro signs.
- MRI: Best for cord, ligaments, discs, hematoma. Use for neuro deficits, suspected ligament injury, clearing C-spine in obtunded patients.
-
Key Fractures:
- Jefferson (C1): Burst fracture of C1 ring (axial load). Unstable if transverse ligament ruptured.
- Odontoid (C2): Anderson & D'Alonzo Types I, II, III (dens fractures).
⭐ Type II (dens base): Most common, highest non-union risk.
- Hangman's (C2): Traumatic spondylolisthesis (hyperextension). Bilateral C2 pars interarticularis fractures.
- Burst (Thoracolumbar): Axial compression, vertebral body comminution, potential canal compromise.
- Chance (Seatbelt): Flexion-distraction injury through all 3 vertebral columns.
Spinal Trauma - Cord Crisis Control
Immediate: ABCDE, spinal immobilization (C-collar, log-roll, spine board). ASIA scale for neuro assessment.
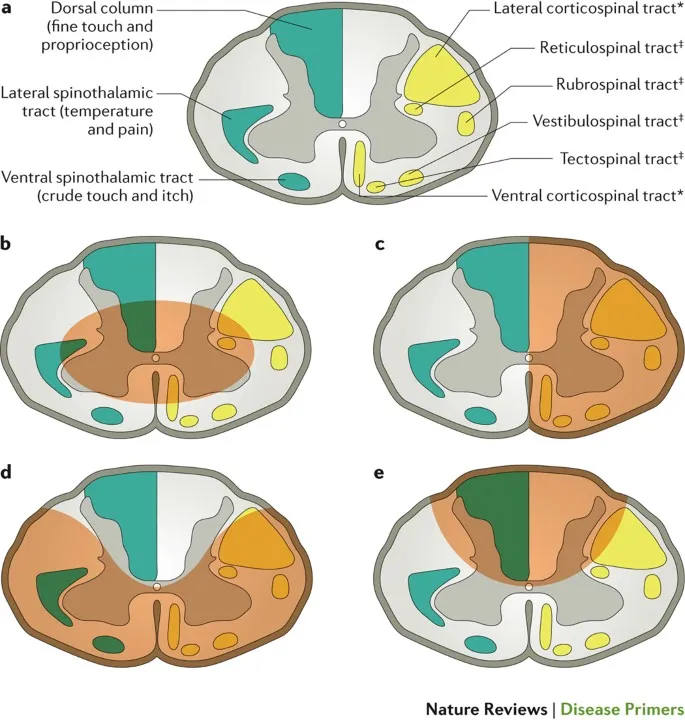
- Incomplete Cord Syndromes:
- Central Cord: Elderly, hyperextension. UL weakness > LL. Sacral sparing. Most common.
- Brown-Séquard: Hemisection. Ipsilateral: motor, proprioception/vibration loss. Contralateral: pain/temp loss.
- Anterior Cord: Flexion/ASA injury. Bilateral motor, pain/temp loss. Proprioception/vibration preserved.
- Complete Cord Injury: Total sensory/motor loss below lesion.
- Cauda Equina Syndrome: LMN (L2↓). Bowel/bladder dysfunction, saddle anesthesia, leg weakness. 📌 S2-S4 keeps it off the floor.
- Conus Medullaris: Sacral cord injury. Mixed UMN/LMN. Symmetric, early bowel/bladder.
⭐ Central Cord Syndrome: Most common incomplete SCI, often in elderly with cervical spondylosis after hyperextension.
Management:
- Methylprednisolone (NASCIS): Controversial. Consider if <8 hrs post-injury. (e.g., 30 mg/kg bolus). ⚠️ High dose, side effects.
- Surgical Decompression/Stabilization: For instability, progressive deficit, cord compression.
- Conservative: Stable injuries, no neuro deficit.
High‑Yield Points - ⚡ Biggest Takeaways
- ASIA Impairment Scale is key for neurological assessment and prognosis.
- Differentiate neurogenic shock (hypotension, bradycardia) from spinal shock (areflexia).
- NEXUS criteria and Canadian C-Spine Rule guide cervical spine clearance.
- Cauda Equina Syndrome requires urgent surgical decompression for bowel/bladder dysfunction.
- Central Cord Syndrome typically shows greater upper limb weakness than lower.
- Odontoid fractures are classified by Anderson & D'Alonzo; Type II most unstable.
- Brown-Séquard syndrome presents with ipsilateral motor/proprioception loss, contralateral pain/temperature loss.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

