Pelvic Anatomy - Ring Fundamentals
- Bones: Ilium, ischium, pubis (form acetabulum); sacrum, coccyx. Pelvis = 2 innominate bones + sacrum.
- Key Ligaments:
- Sacrospinous, sacrotuberous (resist external rotation & vertical shear).
- Anterior & Posterior Sacroiliac (SI) ligaments.
- Pubic symphysis.
- Neurovascular:
- Sciatic nerve (L4-S3), lumbosacral plexus.
- Internal iliac artery branches (📌 'I Like Going Places In My Very Own Underwear'). Key: Superior/Inferior gluteal, Obturator artery/nerve.
- Stability: Posterior ring integrity (SI joints, sacrum, iliac wings & ligaments) is crucial.
⭐ The posterior sacroiliac ligament complex is the strongest in the pelvis and crucial for vertical stability.
Pelvic Fractures - Stability Showdown
Stability by Young & Burgess (Y&B), Tile. 📌 Y&B: APC ('Open Book'), LC ('Closed Book'), VS.
| Class. | Mechanism / Key Feature | Stability |
|---|---|---|
| Y&B APC | AP Comp. ('Open Book'); Diastasis >2.5cm unstable | I: Stable; II: RUVS; III: RUVU |
| Y&B LC | Lat. Comp. ('Closed Book'); Rami/Sacral # | I: Stable; II: RUVS; III: RUVU |
| Y&B VS | Vertical Shear; Major disruption | RUVU |
| Tile A | Stable injuries (e.g. Avulsions) | Stable |
| Tile B | Rotational (Open book/Bucket handle) | RUVS |
| Tile C | Rotational + Vertical (VS, severe APC/LC) | RUVU |
⭐ APC Type III ("open book") highest hemorrhage risk.
Acetabular Fractures - Column Conundrums
- Anatomy: Two columns, anterior (iliopubic) & posterior (ilioischial), are key to stability. Also includes walls (anterior, posterior), roof (dome), and quadrilateral plate. Femoral head blood supply primarily via Medial Circumflex Femoral Artery.
- Judet & Letournel Classification: Divides fractures into 5 elementary and 5 associated types, crucial for surgical planning.
Elementary Types Associated Types Posterior Wall T-shaped Posterior Column Posterior Column + Posterior Wall Anterior Wall Transverse + Posterior Wall Anterior Column Ant. Column/Wall + Post. Hemitransverse Transverse Both Columns - Imaging: Radiographs: AP Pelvis. Judet views: 📌 Iliac Oblique = I see Posterior column, Anterior wall; Obturator Oblique = I see Anterior column, Posterior wall. CT scan is gold standard for detailed assessment.
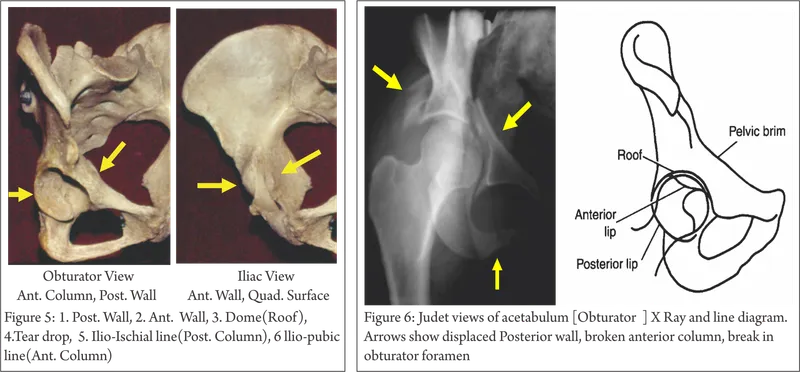
⭐ The posterior wall is the most frequently fractured component of the acetabulum.
Definitive Management - Fixation Focus
Pelvic Fractures:
- Non-operative: Stable (e.g., Tile A, LC-I).
- Operative Indications: Hemodynamic instability, open Fx, symphyseal diastasis >2.5cm, vertical shear, displaced sacral Fx >1cm.
- Fixation Methods: External fixation, anterior ORIF (symphysis/rami), posterior percutaneous SI screws/ORIF.
Acetabular Fractures:
- Non-operative: Undisplaced/minimally displaced (<2mm), congruent joint, roof arc angle >45°.
- Operative Indications: Displacement >2mm, incongruity, posterior wall instability >40-50%, intra-articular fragments, irreducible dislocation.
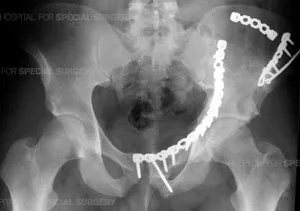
- Surgical Approaches: Kocher-Langenbeck (posterior), Ilioinguinal (anterior), Stoppa.
- Goals (Both): Anatomical reduction, stable fixation, early mobilization.
⭐ Anatomic reduction of the weight-bearing dome of the acetabulum is paramount for preventing post-traumatic arthritis.
Complications - Damage Control
- Early:
- Hemorrhage (pelvic venous plexus; sup. gluteal a., int. pudendal a.)
- Urogenital injury (urethral/bladder)
- Neurologic: Sciatic nerve (peroneal div. common), L5/S1 roots
- DVT/PE, Infection, Morel-Lavallée lesion
- Late:
- Post-traumatic Osteoarthritis (PTOA)
- Malunion/Nonunion
- Heterotopic Ossification (HO); Prophylaxis: Indomethacin 25mg TID or 75mg SR OD
- AVN femoral head, Chronic pain, Sexual dysfunction
⭐ Sciatic nerve injury occurs in up to 20% of acetabular fractures, particularly with posterior dislocations or posterior column/wall fractures, often affecting the peroneal division.
High‑Yield Points - ⚡ Biggest Takeaways
- Young-Burgess classification (APC, LC, VS, CM) guides pelvic ring injury management by mechanism.
- Tile classification (A, B, C) assesses pelvic stability, crucial for surgical decisions.
- Letournel-Judet classification for acetabular fractures uses iliac/obturator oblique (Judet) views.
- Prioritize hemodynamic resuscitation for pelvic hemorrhage; use pelvic binders/ex-fix early.
- High risk of sciatic nerve injury (especially posterior acetabular wall) and urogenital trauma.
- Watch for Morel-Lavallée lesions (closed degloving) with pelvic trauma; can complicate recovery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

