Trauma

On this page
🚨 Trauma Command Center: Your Emergency Response Arsenal
Trauma care compresses life-or-death decisions into minutes, demanding you recognize injury patterns, anticipate physiological collapse, and orchestrate complex interventions while the clock runs mercilessly. You'll master the systematic approach that transforms chaos into controlled response-from initial assessment through diagnostic strategy to definitive treatment-learning how expert clinicians read the body's crisis signals, decode mechanism-based injury signatures, and mobilize coordinated care systems. This lesson builds your command of trauma's unique physiology, sharpens your pattern recognition across blunt and penetrating injuries, and equips you with the algorithms that save lives when every second counts.
📌 Remember: ABCDE - Airway with C-spine, Breathing, Circulation, Disability (neurologic), Exposure/Environment. This sequence prioritizes life-threatening conditions in order of immediacy, with airway obstruction causing death in 3-5 minutes, respiratory failure in 5-10 minutes, and hemorrhagic shock in 10-30 minutes.
The trauma response system operates on the principle of damage control - rapid identification and temporary stabilization of life-threatening injuries before definitive repair. This approach reduces mortality by 25-40% compared to immediate definitive surgery in unstable patients.
| Priority Level | Time Frame | Intervention | Mortality Impact | Success Rate |
|---|---|---|---|---|
| Primary Survey | 0-5 min | ABCDE assessment | 80% reduction | >95% |
| Resuscitation | 5-15 min | IV access, fluids | 60% reduction | 85-90% |
| Secondary Survey | 15-30 min | Head-to-toe exam | 40% reduction | 90-95% |
| Definitive Care | 30-60 min | OR/ICU transfer | 25% reduction | 70-85% |
| Damage Control | 60-120 min | Staged procedures | 35% reduction | 75-80% |
- Mechanism-Based Assessment
- Blunt trauma accounts for 85% of cases in India, primarily motor vehicle accidents
- Penetrating trauma represents 15%, with increasing urban violence
- High-velocity injuries: energy >2000 ft-lbs, extensive tissue damage
- Low-velocity injuries: energy <1000 ft-lbs, localized damage
- Blast injuries involve primary (pressure wave), secondary (projectiles), tertiary (displacement), and quaternary (burns/inhalation) mechanisms
💡 Master This: Energy transfer determines injury severity - kinetic energy equals ½mv², meaning velocity has exponential impact. A 10 mph increase in vehicle speed increases injury energy by 44%, explaining why high-speed crashes produce disproportionately severe injuries despite seemingly modest speed differences.
The systematic trauma approach prevents the 30% error rate seen with unstructured assessments. Missed injuries occur in 8-15% of trauma patients, with 65% discovered during secondary survey and 35% during tertiary survey within 24-48 hours.
Understanding trauma pathophysiology reveals why hemorrhage causes 40% of trauma deaths, traumatic brain injury accounts for 30%, and airway compromise represents 10%. The remaining 20% result from multiple organ failure, sepsis, and late complications. This knowledge guides resource allocation and treatment priorities in the critical first hour when survival is determined.
🚨 Trauma Command Center: Your Emergency Response Arsenal
⚡ Physiological Storm: The Body's Crisis Response
📌 Remember: 3-for-1 Rule - For every 1 mL of blood lost, 3 mL of crystalloid is required for adequate resuscitation due to rapid redistribution from intravascular to interstitial space. This explains why 2-3 liters of normal saline may be needed to replace 1 liter of blood loss.
The inflammatory response begins within minutes, with cytokine release (TNF-α, IL-1, IL-6) peaking at 2-6 hours. This systemic inflammatory response syndrome (SIRS) can progress to multiple organ dysfunction syndrome (MODS) in 15-25% of major trauma patients, with mortality rates of 30-50% when ≥3 organs are involved.
| Shock Class | Blood Loss | Heart Rate | Blood Pressure | Mental Status | Urine Output |
|---|---|---|---|---|---|
| Class I | <15% (<750mL) | <100 bpm | Normal | Alert | >30 mL/hr |
| Class II | 15-30% (750-1500mL) | 100-120 bpm | Normal | Anxious | 20-30 mL/hr |
| Class III | 30-40% (1500-2000mL) | 120-140 bpm | Decreased | Confused | 5-15 mL/hr |
| Class IV | >40% (>2000mL) | >140 bpm | Severely Low | Lethargic | <5 mL/hr |
- Metabolic Consequences
- Oxygen debt accumulates when delivery falls below 8-10 mL/kg/min
- Lactate levels rise above 2.5 mmol/L indicating anaerobic metabolism
- Normal lactate: 0.5-1.5 mmol/L
- Mild elevation: 2.5-4.0 mmol/L suggests tissue hypoperfusion
- Severe elevation: >4.0 mmol/L indicates significant shock
- Base deficit >-6 mEq/L correlates with >25% blood loss
- Coagulopathy develops early, with 25% of trauma patients arriving with abnormal clotting
💡 Master This: The lethal triad components are interconnected - hypothermia reduces enzyme function by 50% for every 10°C drop, acidosis shifts the oxygen-hemoglobin dissociation curve rightward (reducing oxygen delivery), and coagulopathy prevents effective hemostasis. Breaking this cycle requires simultaneous correction of all three components.
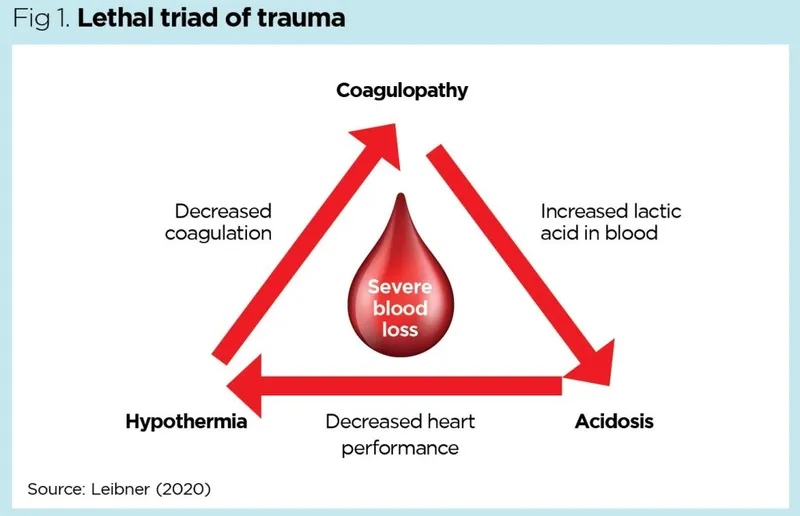
Cellular dysfunction begins when oxygen delivery falls below critical thresholds. Mitochondrial respiration fails, ATP production drops by 70-80%, and cellular membrane integrity deteriorates. This explains why early aggressive resuscitation within the first 6 hours improves survival by 40-50% compared to delayed intervention.
The neuroendocrine response involves massive cortisol release (5-10x normal), growth hormone elevation (10-20x normal), and insulin resistance development within hours. These changes mobilize energy stores but can lead to hyperglycemia (>200 mg/dL) in 60-80% of trauma patients, requiring careful glucose management to prevent secondary complications.
Understanding these physiological responses enables targeted interventions that support the body's compensatory mechanisms while preventing progression to irreversible shock and multi-organ failure.
⚡ Physiological Storm: The Body's Crisis Response
🎯 Pattern Recognition Matrix: Injury Signature Decoding
📌 Remember: KINEMATICS - Kinetic energy, Impact direction, Nature of forces, Energy dissipation, Multiple impacts, Associated injuries, Time factors, Injury severity, Comorbidities, Secondary survey findings. This framework systematically evaluates mechanism to predict injury patterns.
Motor Vehicle Collision Patterns follow predictable biomechanical principles based on impact direction and restraint use:
-
Frontal Impact Injuries
- Unrestrained: Head/facial trauma (70%), cervical spine (15%), chest (60%), abdominal (40%)
- Restrained: Chest wall (45%), abdominal (25%), lower extremity (30%)
- Seatbelt sign indicates 50% chance of intra-abdominal injury
- Airbag deployment reduces head injury by 60% but increases upper extremity fractures
- Speed >35 mph: Multiple system involvement in >80% of cases
-
Side Impact Patterns
- Near-side: Head (80%), cervical spine (25%), chest (70%), pelvis (45%)
- Far-side: Cervical spine (35%), opposite-side chest (40%)
- Lateral compression pelvic fractures in 60% of significant side impacts
- Aortic injury risk increases 3-fold with side impact >40 mph
⭐ Clinical Pearl: Waddell's Triad in pediatric pedestrian injuries - lower extremity fracture from bumper impact, chest/abdominal trauma from hood contact, and head injury from ground impact. This pattern occurs in 40% of child pedestrian accidents and should prompt systematic evaluation of all three body regions.
| Fall Height | Injury Pattern | Mortality Risk | Common Injuries | Energy (ft-lbs) |
|---|---|---|---|---|
| <10 feet | Single system | <5% | Extremity fractures | <500 |
| 10-20 feet | Dual system | 15-25% | Spine, pelvis | 500-1500 |
| 20-40 feet | Multi-system | 40-60% | Head, chest, abdomen | 1500-3000 |
| >40 feet | Massive trauma | >80% | Multiple organ systems | >3000 |
-
Gunshot Wounds
- Low velocity (<1000 fps): 2-3x bullet diameter tissue damage
- High velocity (>2000 fps): 10-30x bullet diameter cavitation
- Temporary cavity creates pressure waves causing distant organ damage
- Rifle wounds have 5-10x higher energy than handgun wounds
- Shotgun injuries: Distance determines pattern - <10 yards acts like single projectile
-
Stab Wounds
- Thoracic: 15% require thoracotomy, 85% managed conservatively
- Abdominal: 50% have peritoneal penetration, 25% require surgery
- Weapon length and trajectory predict organ involvement
- Retroperitoneal injuries easily missed on initial assessment
💡 Master This: Energy dissipation determines injury severity more than weapon type. A knife wound that transects major vessels can be more immediately life-threatening than a high-velocity gunshot that misses vital structures. Focus on anatomical damage and physiological impact rather than mechanism alone.
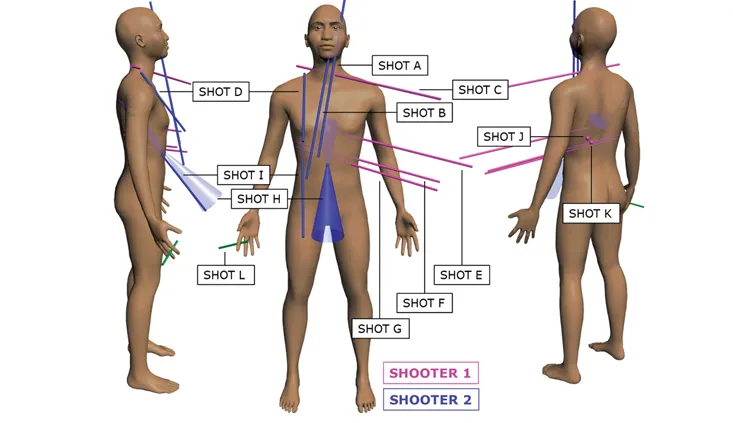
Blast Injury Recognition involves understanding the four phases of blast trauma:
- Primary (pressure wave): Tympanic membrane rupture (50%), pulmonary contusion (30%), bowel perforation (15%)
- Secondary (projectiles): Penetrating injuries, 70% involve extremities
- Tertiary (displacement): Blunt trauma patterns, 40% have head injuries
- Quaternary (burns/inhalation): 60% have combined injury patterns
Age-Related Injury Patterns modify standard assessment approaches:
- Pediatric (<16 years): Head injury in 80%, abdominal injury often without external signs, flexible ribs allow internal damage without fractures
- Elderly (>65 years): Ground-level falls cause significant injury, anticoagulation increases bleeding risk 3-5x, osteoporosis increases fracture risk at lower energy levels
Recognition of these patterns enables targeted evaluation, appropriate resource allocation, and early identification of life-threatening injuries that might otherwise be missed during initial assessment.
🎯 Pattern Recognition Matrix: Injury Signature Decoding
🔬 Diagnostic Precision: The Investigation Arsenal
📌 Remember: FAST-PLUS - Traditional 4 views (RUQ, LUQ, pelvis, cardiac) plus lung sliding assessment and IVC evaluation. This extended protocol increases diagnostic yield by 25% and provides information about pneumothorax and volume status in addition to free fluid detection.
Laboratory Investigations provide rapid physiological assessment with specific trauma-relevant parameters:
- Initial Labs (within 10 minutes)
- Hemoglobin: May be normal initially despite significant blood loss
- Lactate: >2.5 mmol/L indicates tissue hypoperfusion
- Lactate clearance >20% in first 6 hours predicts survival
- Failure to clear lactate associated with 3-fold mortality increase
- Base deficit: >-6 mEq/L suggests >25% blood loss
- INR/PT: Baseline coagulopathy present in 25% of trauma patients
| Laboratory Value | Normal Range | Mild Abnormal | Severe Abnormal | Clinical Significance |
|---|---|---|---|---|
| Lactate | 0.5-1.5 mmol/L | 2.5-4.0 mmol/L | >4.0 mmol/L | Tissue hypoperfusion |
| Base Deficit | ±2 mEq/L | -3 to -6 mEq/L | >-6 mEq/L | Metabolic acidosis |
| Hemoglobin | 12-16 g/dL | 8-10 g/dL | <8 g/dL | Blood loss severity |
| INR | 0.8-1.2 | 1.3-1.5 | >1.5 | Coagulopathy risk |
| Troponin | <0.04 ng/mL | 0.04-0.4 ng/mL | >0.4 ng/mL | Cardiac contusion |
Imaging Protocols are tailored to mechanism and clinical presentation:
-
Pan-CT Scanning (head, chest, abdomen, pelvis)
- Sensitivity: 95-98% for significant injuries
- Scan time: <5 minutes with modern multidetector CT
- Reduces missed injury rate from 15% to <3%
- Radiation exposure: 20-30 mSv (equivalent to 2-3 years background)
- Indications: High-energy mechanism, altered mental status, multiple injuries
-
Selective Imaging for stable patients
- Chest X-ray: Detects 90% of pneumothorax, 70% of hemothorax
- Pelvic X-ray: 95% sensitive for unstable pelvic fractures
- Can be omitted if CT pelvis planned and patient stable
- Clinical examination has 90% sensitivity for pelvic fractures
💡 Master This: Imaging timing is critical - unstable patients should never leave the resuscitation area for CT scanning. FAST exam, chest X-ray, and pelvic X-ray provide 80% of immediately actionable information and can be performed during resuscitation without patient transport.
Advanced Diagnostics for specific injury patterns:
-
CT Angiography (CTA)
- Aortic injury: 98% sensitivity, 95% specificity
- Cervical vascular injury: 95% sensitivity for >25% stenosis
- Screening criteria: High-energy mechanism, neurological deficit, cervical hematoma
- False positive rate: <5% with modern protocols
-
Diagnostic Peritoneal Lavage (DPL)
- Indications: Unstable patient with equivocal FAST, penetrating abdominal trauma
- Positive criteria: >10 mL gross blood, >100,000 RBC/μL, >500 WBC/μL
- Sensitivity: 98% for intraperitoneal bleeding
- Specificity: 85% (may be positive with minor injuries)
Point-of-Care Testing enables rapid decision-making:
- Blood Gas Analysis: Provides pH, lactate, hemoglobin in <2 minutes
- Thromboelastography (TEG): Real-time coagulation assessment in 15 minutes
- Portable X-ray: Results available in <5 minutes for unstable patients
Diagnostic Pitfalls to avoid:
- Normal initial hemoglobin doesn't exclude significant bleeding - hemodilution takes hours
- Negative FAST doesn't exclude injury - sensitivity drops to 60% for <500 mL free fluid
- CT contrast allergy shouldn't delay imaging - non-contrast CT provides 85% of diagnostic information
- Pregnancy modifies radiation risk - ultrasound first, CT if life-threatening injuries suspected
Understanding diagnostic capabilities and limitations enables rapid, accurate assessment while avoiding unnecessary delays in critical trauma patients requiring immediate intervention.
🔬 Diagnostic Precision: The Investigation Arsenal
⚙️ Treatment Algorithms: The Intervention Playbook
📌 Remember: CRASH Protocol - Control hemorrhage, Resuscitate appropriately, Assess for other injuries, Stabilize fractures, Hypothermia prevention. This sequence prioritizes interventions that have the greatest impact on survival in the first 60 minutes.
Hemorrhage Control represents the most time-critical intervention:
-
External Hemorrhage
- Direct pressure: Controls 90% of external bleeding
- Tourniquet application: 98% effective for extremity hemorrhage
- Application time: <2 minutes for effectiveness
- Safe ischemia time: 90-120 minutes without permanent damage
- Hemostatic agents: QuikClot, Celox reduce bleeding time by 60-80%
-
Internal Hemorrhage Management
- Massive transfusion protocol (MTP): 1:1:1 ratio of RBC:FFP:platelets
- Activation criteria: >10 units RBC in 24 hours or >4 units in 1 hour
- Survival benefit: 25% mortality reduction with early MTP activation
- Tranexamic acid: 1g IV within 3 hours reduces mortality by 1.5%
- Maximum benefit: When given within 1 hour of injury
- Contraindication: >3 hours post-injury (increases mortality)
- Massive transfusion protocol (MTP): 1:1:1 ratio of RBC:FFP:platelets
| Intervention | Time Window | Success Rate | Mortality Reduction | Complications |
|---|---|---|---|---|
| Tourniquet | <2 min | 98% | 85% for extremity | <2% amputation |
| Massive Transfusion | <30 min | 75-85% | 25% overall | 15% TRALI |
| Damage Control | <60 min | 70-80% | 35% severe trauma | 20% reoperation |
| Tranexamic Acid | <1 hour | 90% | 1.5% overall | <1% thrombosis |
| REBOA | <45 min | 85% | 40% exsanguination | 10% ischemia |
Airway Management in trauma patients requires modified approaches:
-
C-spine Immobilization during intubation
- Manual in-line stabilization reduces cervical movement by 75%
- Video laryngoscopy preferred when available (95% first-pass success)
- Bougie-assisted intubation increases success rate to 98%
- Surgical airway required in <3% of trauma patients
-
Rapid Sequence Intubation (RSI) protocol
- Etomidate 0.3 mg/kg + Succinylcholine 1.5 mg/kg
- Cricoid pressure controversial - may worsen visualization
- Pre-oxygenation: 3-5 minutes with 100% O₂
- Backup plan: LMA or surgical airway if intubation fails
💡 Master This: Surgical airway indications include massive facial trauma, laryngeal injury, inability to open mouth >3 cm, or failed intubation after 2 attempts. Cricothyrotomy can be performed in <60 seconds and provides definitive airway control when other methods fail.
Resuscitation Strategies have evolved toward goal-directed therapy:
-
Fluid Resuscitation
- Initial bolus: 1-2 liters crystalloid for hypotensive patients
- Blood products: Early transition when >2 liters crystalloid required
- Type O negative blood immediately available
- Type-specific blood available in 10-15 minutes
- Crossmatched blood available in 45-60 minutes
-
Monitoring Parameters
- Lactate clearance: Target >20% reduction in 6 hours
- Base deficit: Improvement toward normal (±2 mEq/L)
- Urine output: 0.5-1.0 mL/kg/hr indicates adequate perfusion
- Mean arterial pressure: >65 mmHg for organ perfusion
Damage Control Orthopedics prioritizes life over limb:
- External fixation for unstable fractures allows rapid stabilization
- Temporary spanning of joints preserves length and alignment
- Definitive fixation delayed until physiological stability achieved
- Safe window: 5-11 days post-injury for major procedures
- Early total care appropriate only in stable patients
Temperature Management prevents the lethal triad:
- Active warming to maintain core temperature >35°C
- Warm fluids: All IV fluids and blood products warmed to 37-40°C
- Environmental control: OR temperature >26°C, warming blankets
- Hypothermia reduces clotting factor function by 50% per 10°C drop
- Rewarming rate: 1-2°C/hour to prevent cardiovascular instability
These algorithmic approaches provide systematic, evidence-based care that maximizes survival while minimizing complications in the chaotic trauma environment.
⚙️ Treatment Algorithms: The Intervention Playbook
🌐 Systems Integration: The Trauma Network Architecture
Pre-hospital Integration establishes the foundation for optimal outcomes:
-
Emergency Medical Services (EMS) protocols
- Scene time <10 minutes for penetrating trauma, <20 minutes for blunt trauma
- Transport decisions: "Load and go" vs "Stay and play" based on injury severity
- Trauma triage criteria identify 85% of patients requiring trauma center care
- Helicopter transport reduces mortality by 25% for distances >45 miles
- Communication protocols: Pre-arrival notification allows team preparation
-
Field Interventions focus on life-threatening conditions only
- Airway management: King LT or LMA preferred over field intubation
- IV access: 2 large-bore IVs or intraosseous if difficult access
- Fluid resuscitation: Limited to 1-2 liters crystalloid maximum
- Blood products: Whole blood programs show 30% mortality reduction
📌 Remember: PHTLS Principles - Patient assessment, Hemorrhage control, Treatment priorities, Load and go decisions, Support and communication. Field providers focus on rapid assessment, hemorrhage control, and expeditious transport rather than extensive field treatment.
Hospital System Coordination requires multidisciplinary integration:
- Trauma Team Activation criteria
- Highest level: Penetrating torso/neck, GCS <9, SBP <90, respiratory compromise
- Second level: High-energy mechanism, multiple injuries, significant comorbidities
- Response time: <5 minutes for highest level activation
- Team composition: Trauma surgeon, emergency physician, anesthesiologist, nurses
| System Component | Response Time | Success Metric | Quality Indicator | Benchmark |
|---|---|---|---|---|
| EMS Response | <8 minutes | Scene time <20 min | Protocol compliance | >90% |
| Trauma Activation | <5 minutes | Team assembly | Door to OR <60 min | >85% |
| Blood Bank | <15 minutes | Type-specific blood | MTP activation <30 min | >95% |
| OR Availability | <30 minutes | Surgical start | 24/7 capability | 100% |
| ICU Admission | <60 minutes | Bed availability | Monitoring capability | >90% |
Resource Allocation requires dynamic coordination:
-
Operating Room Management
- Dedicated trauma OR available 24/7 with <30 minute activation
- Backup OR capability for multiple casualties or complex cases
- Equipment standardization: Trauma packs reduce setup time by 50%
- Staff cross-training: 75% of OR staff trauma-capable
-
Blood Bank Integration
- Massive transfusion protocol activation reduces blood product delivery time to <15 minutes
- Type O negative inventory maintained at >20 units for immediate release
- Thawed plasma available 24/7 reduces preparation time from 45 to <5 minutes
- Platelet inventory managed for <5 day outdating to ensure availability
💡 Master This: Surge capacity planning enables response to multiple casualties - trauma centers must demonstrate ability to handle 2-3x normal volume for 6-8 hours. This requires flexible staffing, equipment reserves, and coordination protocols with regional hospitals.
Quality Improvement Integration drives continuous enhancement:
-
Performance Improvement programs
- Morbidity and mortality conferences review 100% of deaths and major complications
- Benchmarking against national databases (NTDB, TQIP) identifies improvement opportunities
- Risk-adjusted mortality rates account for injury severity and comorbidities
- Preventable death rates <5% in mature trauma systems
-
Registry Data Collection
- Trauma registry captures >150 data elements per patient
- Real-time quality metrics enable immediate process improvement
- Compliance monitoring: >95% adherence to evidence-based protocols
- Outcome tracking: Functional status at discharge and 6 months
Regional Integration extends trauma system benefits:
-
Transfer Protocols ensure appropriate patient distribution
- Interfacility transport for specialized care (neurosurgery, pediatrics, burns)
- Reverse triage when Level I centers reach capacity
- Transfer time <2 hours for time-sensitive conditions
- Communication systems enable real-time bed availability tracking
-
Education and Training programs
- ATLS certification for >90% of trauma team members
- Simulation training improves team performance and communication
- Continuing education: 40 hours/year trauma-specific training
- Competency assessment: Annual skills validation for critical procedures
This integrated approach transforms trauma care from individual heroics to systematic excellence, with coordinated protocols and shared accountability producing optimal outcomes across the entire trauma care continuum.
🌐 Systems Integration: The Trauma Network Architecture
🏆 Mastery Command Center: Your Clinical Excellence Toolkit
Essential Clinical Arsenal - the critical numbers and thresholds that guide every trauma decision:
- Vital Sign Thresholds
- Shock indicators: HR >100, SBP <90, MAP <65, UOP <0.5 mL/kg/hr
- Respiratory distress: RR >30, O₂ sat <90, PaO₂ <60 mmHg
- Intubation criteria: GCS <9, inability to protect airway, respiratory failure
- Ventilator settings: TV 6-8 mL/kg, PEEP 5-10 cmH₂O, FiO₂ to maintain sat >94%
📌 Remember: Rule of 30s - 30% blood loss causes shock, 30 minutes maximum for damage control, 30 mL/hr minimum urine output, 30°C core temperature triggers lethal triad. These thresholds represent critical decision points where intervention becomes life-saving.
Rapid Assessment Framework enables systematic evaluation in <5 minutes:
| Assessment Phase | Time Allocation | Key Elements | Decision Points | Action Triggers |
|---|---|---|---|---|
| Primary Survey | 2 minutes | ABCDE assessment | Life threats | Immediate intervention |
| Resuscitation | 10 minutes | IV access, fluids | Response to treatment | Blood products, OR |
| Secondary Survey | 15 minutes | Head-to-toe exam | Injury identification | Imaging, consultants |
| Definitive Care | 30 minutes | Treatment planning | Operative vs non-op | OR, ICU, floor |
| Disposition | 45 minutes | Resource allocation | Level of care | Transfer, discharge |
Pattern Recognition Mastery - high-yield associations that predict injury patterns:
-
Mechanism-Injury Correlations
- Seatbelt sign → 50% chance of intra-abdominal injury
- Steering wheel deformity → Cardiac contusion in 25%
- Dashboard knee → Posterior hip dislocation in 40%
- Windshield spider → Cervical spine injury in 15%
- **Fall >20 feet → Calcaneus fracture + spine injury in 60%
-
Physical Exam Pearls
- Grey Turner sign → Retroperitoneal bleeding (specificity 95%)
- Cullen sign → Intraperitoneal bleeding (specificity 90%)
- Raccoon eyes → Basilar skull fracture (sensitivity 75%)
- Battle sign → Temporal bone fracture (specificity 85%)
💡 Master This: Energy dissipation principles predict injury severity - kinetic energy = ½mv², meaning velocity has exponential impact. A 20 mph crash has 4x the energy of 10 mph, explaining why high-speed mechanisms produce disproportionately severe injuries.
Treatment Decision Matrix for rapid intervention choices:
-
Hemorrhage Control Hierarchy
- External: Direct pressure → tourniquet → hemostatic agents → surgical control
- Internal: Resuscitation → imaging → intervention (OR vs IR vs observation)
- Massive transfusion: 1:1:1 ratio, TXA within 3 hours, Ca²⁺ replacement
- Damage control: Pack, clamp, shunt → ICU resuscitation → definitive repair
-
Airway Management Algorithm
- Conscious patient: High-flow O₂ → CPAP/BiPAP → intubation
- Unconscious patient: RSI with C-spine protection → surgical airway if failed
- Difficult airway: Video laryngoscopy → bougie → LMA → cricothyrotomy
Quality Metrics that define trauma excellence:
-
Time-Sensitive Indicators
- Door to CT: <30 minutes for stable patients
- Door to OR: <60 minutes for unstable patients
- Blood product delivery: <15 minutes for MTP activation
- Consultant response: <30 minutes for urgent consultations
-
Outcome Measures
- Risk-adjusted mortality: <5% for preventable deaths
- Complication rates: <10% for major complications
- Length of stay: Appropriate for injury severity
- Functional outcomes: >80% return to baseline function
This mastery toolkit transforms trauma complexity into systematic excellence, providing the frameworks, thresholds, and decision trees that enable rapid, accurate, and life-saving trauma care in the most challenging clinical scenarios.
🏆 Mastery Command Center: Your Clinical Excellence Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























