Spinal Tumors: Classification & Red Flags - Location & Alarms
- Classification (by Dural Relationship):
- Extradural (ED): Most common (~55%). Outside dura. Often metastatic (lung, breast, prostate).
- Vertebral bodies, epidural space.
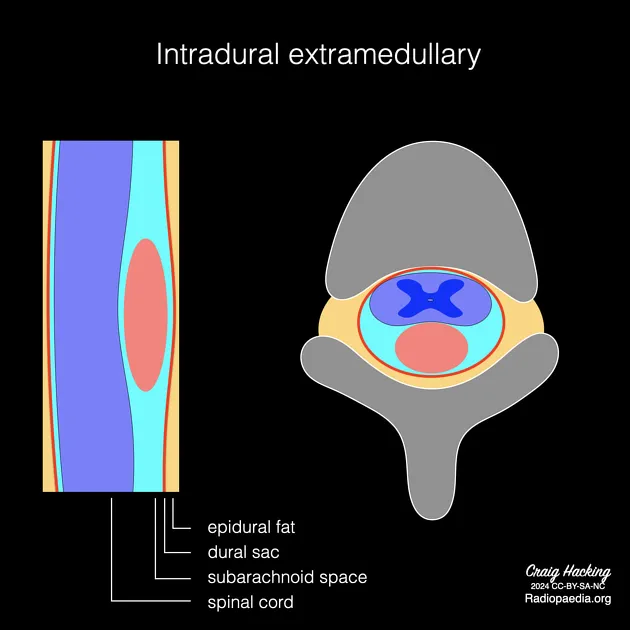
- Intradural-Extramedullary (IDEM): ~40%. Within dura, outside cord.
- Meningiomas, nerve sheath tumors (schwannomas, neurofibromas).
- Intramedullary (IM): Least common (~5%). Within spinal cord.
- Ependymomas, astrocytomas.
- Ependymomas, astrocytomas.
- Extradural (ED): Most common (~55%). Outside dura. Often metastatic (lung, breast, prostate).
- Red Flags (Alarm Symptoms):
- Pain: Persistent, progressive, non-mechanical; worse at night/recumbency.
- Neurological deficits: Weakness, sensory loss, gait issues, bowel/bladder dysfunction (⚠️ Cauda Equina Syndrome).
- Systemic: Unexplained weight loss, fever.
- History of malignancy.
- Age: <20 or >50 years.
- No improvement after 4-6 weeks conservative therapy.
⭐ Most spinal metastases occur in the thoracic spine. Common primary sources: Lung, Breast, Prostate (📌 Mnemonic: LBP - Lung, Breast, Prostate).
Spinal Tumors: Diagnosis & Key Players - Unmasking Culprits
- Diagnosis:
- Clinical: Persistent, progressive back pain (esp. night, non-mechanical), radiculopathy, myelopathy (motor/sensory deficits, sphincter dysfunction).
- Imaging:
- MRI with Gadolinium: Gold standard for diagnosis & surgical planning. Defines tumor extent, cord compression, neural involvement.
- CT Scan: Best for bony architecture, matrix calcification, useful for biopsy guidance.
- X-ray: Initial screen; may show vertebral collapse, pedicle erosion, lytic/blastic lesions.
- Biopsy: Histopathological confirmation (CT-guided or open) is essential for definitive diagnosis and guiding treatment.

| Tumor | Location (Typical) | Key Features / Buzzwords |
|---|---|---|
| Metastases | Extradural (Vertebral) | Most common; Prostate, Breast, Kidney, Thyroid, Lung (📌 PB KTL); Night pain. |
| Meningioma | Intradural-Extramedullary | F > M; Thoracic; Dural tail sign. |
| Schwannoma | Intradural-Extramedullary | Nerve root; Dumbbell shape; Antoni A/B. |
| Ependymoma | Intramedullary | Central canal; Hemorrhage; Hemosiderin cap; Myxopapillary (filum). |
| Astrocytoma | Intramedullary | Infiltrative; Eccentric; Poorly defined. |
| Chordoma | Extradural (Sacrum/Clivus) | Midline; Locally aggressive; Physaliphorous cells. |
| Multiple Myeloma | Extradural (Vertebral) | Most common primary malignant bone tumor; Lytic "punched-out" lesions. |
Spinal Tumors: Management & Stability - Strategic Interventions
- Management Goals: Neural decompression, spinal stability, tumor control, pain relief.
- Treatment Pillars:
- Surgery: Excision, decompression, fusion/instrumentation.
- Radiotherapy (RT): EBRT, SRS; for radiosensitive tumors or as adjuvant.
- Chemotherapy: Systemic (e.g., myeloma, lymphoma).
- Steroids: Manage edema & acute neuro-deficits.
- Spinal Instability Neoplastic Score (SINS):
- Guides surgical decision-making.
- Score: Stable (0-6), Potentially Unstable (7-12), Unstable (13-18).
- Assesses: Location, pain, lesion type, alignment, vertebral body collapse (>50%), posterior element involvement.
⭐ > Patients with a SINS score of ≥7 often benefit from surgical consultation regarding stabilization, regardless of oncologic prognosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Metastatic tumors are the most common spinal tumors (e.g., from breast, lung, prostate).
- Persistent back pain, especially night pain or pain unrelieved by rest, is a key symptom.
- MRI with gadolinium is the imaging modality of choice for diagnosis and staging.
- Multiple myeloma is the most common primary malignant bone tumor affecting the spine.
- Osteoid osteoma: characteristic night pain relieved by NSAIDs; nidus visible on CT.
- Chordomas: locally aggressive malignant tumors, typically in the sacrum/clivus.
- Neurological deficits (e.g., weakness, sensory loss, bowel/bladder dysfunction) warrant urgent evaluation for cord compression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

