IVD Basics: Anatomy & Degeneration - Spine's Shock Absorbers

- Structure: Spine's shock absorbers, between vertebrae.
- Annulus Fibrosus (AF): Outer, tough, fibrocartilaginous rings (Type I collagen). Resists tensile stress.
- Nucleus Pulposus (NP): Inner, gelatinous core (Type II collagen, proteoglycans). Resists compression.
- Cartilaginous Endplates: Hyaline cartilage; interface with vertebral bodies, nutrient supply.
- Function: Shock absorption, load distribution, spinal flexibility.
- Degeneration (Spondylosis): Age-related, starts in NP.
- NP desiccation (↓ proteoglycans, water content).
- AF tears (circumferential/radial).
- Disc height ↓, osteophytes form.
⭐ Most common site for lumbar disc herniation is L4-L5 or L5-S1 due to high biomechanical stress and mobility.
- Blood supply: Avascular in adults; nutrients by diffusion via endplates. 📌 DAN (Disc Avascular Nutrient-diffusion)
Disc Herniation: Pathophysiology & Types - When Cushions Bulge
Pathophysiology: Degeneration of annulus fibrosus (AF) → tears → nucleus pulposus (NP) herniates → neural compression.
Morphological Types:
- Bulge: Symmetrical annular extension; NP contained.
- Protrusion: Focal annular extension; outer AF intact. Base > dome.
- Extrusion: NP through AF; dome > base (mushroom shape).
- Sequestration: Free NP fragment, detached.
Anatomical Locations (📌 Mnemonic: Can Policemen Find Everything?):
- Central: Midline; risk myelopathy/Cauda Equina Syndrome (CES).
- Paracentral (Posterolateral): Most common. Affects traversing nerve root.
- Foraminal: Affects exiting nerve root in foramen.
- Extraforaminal: Affects exiting nerve root lateral to foramen.
⭐ Most common: Posterolateral L4-L5 or L5-S1. An L4-L5 herniation typically compresses the traversing L5 nerve root.
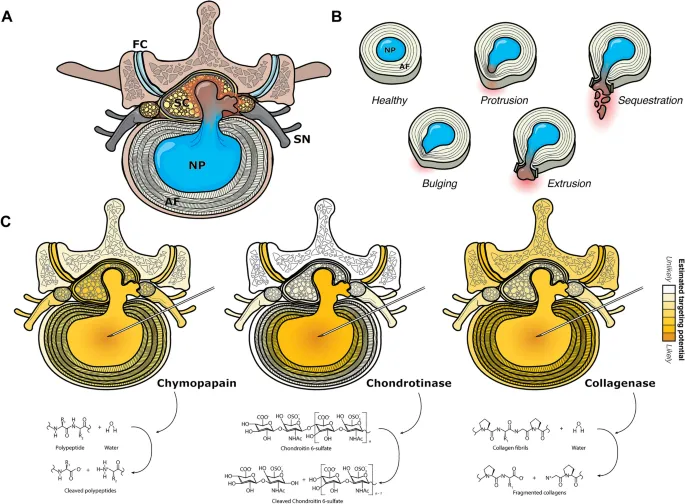 and anatomical locations (central, paracentral, foraminal, extraforaminal))
and anatomical locations (central, paracentral, foraminal, extraforaminal))
Clinical Features: Symptoms & Syndromes - Signals of Distress
- Pain Patterns:
- Axial: Localized (neck/back).
- Radicular: Dermatomal radiation (e.g., sciatica); worse with Valsalva.
- Neurological Signs:
- Sensory: Paresthesia, numbness.
- Motor: Myotomal weakness.
- Reflexes: ↓ (radiculopathy); ↑/Babinski (myelopathy).
- Specific Syndromes:
- Radiculopathy: Nerve root impingement.
- Cervical: Arm pain/deficits.
- Lumbar: Leg pain/deficits (e.g., foot drop L5). Positive SLR.
- Myelopathy: Cord compression.
- Gait issues, UMN signs (spasticity).
- ⚠️ Cauda Equina Syndrome (CES):
- Bilateral sciatica, saddle anesthesia (S2-S5), bowel/bladder dysfunction, ↓ anal tone. Surgical Emergency!
- Radiculopathy: Nerve root impingement.
- Red Flags: ⚠️
- Age <20 or >55 (new onset).
- Night pain, fever, weight loss.
- Progressive neuro deficit, history of cancer.
⭐ Cauda Equina Syndrome (CES) is a critical surgical emergency characterized by bilateral radiculopathy, saddle anesthesia, and sphincter disturbance.

Diagnosis & Management: Finding & Fixing - Charting the Course
-
Diagnosis:
- Clinical Exam:
- History: Radicular pain, numbness, weakness.
- Tests: SLR (Lasegue's) - lumbar; Spurling's - cervical.
- Imaging:
- X-ray: Initial; fracture/instability, disc space.
- MRI: Details herniation, nerve/cord compression.
- CT Myelogram: If MRI C/I.

- EMG/NCS: Confirms radiculopathy, severity.
- Clinical Exam:
-
Management:
- Conservative (Primary):
- Activity modification, NSAIDs, physiotherapy (McKenzie, core strength).
- Epidural steroids for severe radicular pain.
- Surgical Indications:
- ⚠️ Cauda Equina Syndrome (CES) - EMERGENCY! Immediate decompression.
- Progressive motor deficit.
- Intractable pain despite >6-12 weeks conservative care.
- Surgical Options:
- Microdiscectomy/Discectomy.
- Laminectomy/Foraminotomy.
- Spinal Fusion (instability).
- Conservative (Primary):
⭐ MRI is the investigation of choice for diagnosing intervertebral disc prolapse and assessing nerve root compression.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common lumbar disc prolapse: L4-L5, then L5-S1.
- Postero-lateral prolapse affects traversing nerve root (e.g., L4-L5 disc → L5 root).
- SLR test positive indicates sciatic nerve root irritation in lumbar herniation.
- Cauda Equina Syndrome: Surgical emergency; presents with bilateral sciatica, saddle anesthesia, bowel/bladder dysfunction.
- MRI is the gold standard imaging for diagnosing intervertebral disc prolapse.
- Conservative management is first-line for most uncomplicated disc prolapses.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

