Cervical Anatomy & Biomechanics - Neck's Atlas & Axis
- Atypical Vertebrae:
- C1 (Atlas): No body/spinous process. Ring-like. 📌 Atlas: No body, holds head.
- C2 (Axis): Dens for rotation.
- C7 (Vertebra Prominens): Long, non-bifid spinous process.
- Typical Vertebrae (C3-C6): Small body, bifid spinous process, transverse foramina (vertebral artery).
- Key Ligaments:
- Transverse Lig.: C1-C2 stability (holds dens).
- ALL/PLL: Limit extension/flexion.
- Ligamentum Flavum: Elastic, connects laminae.
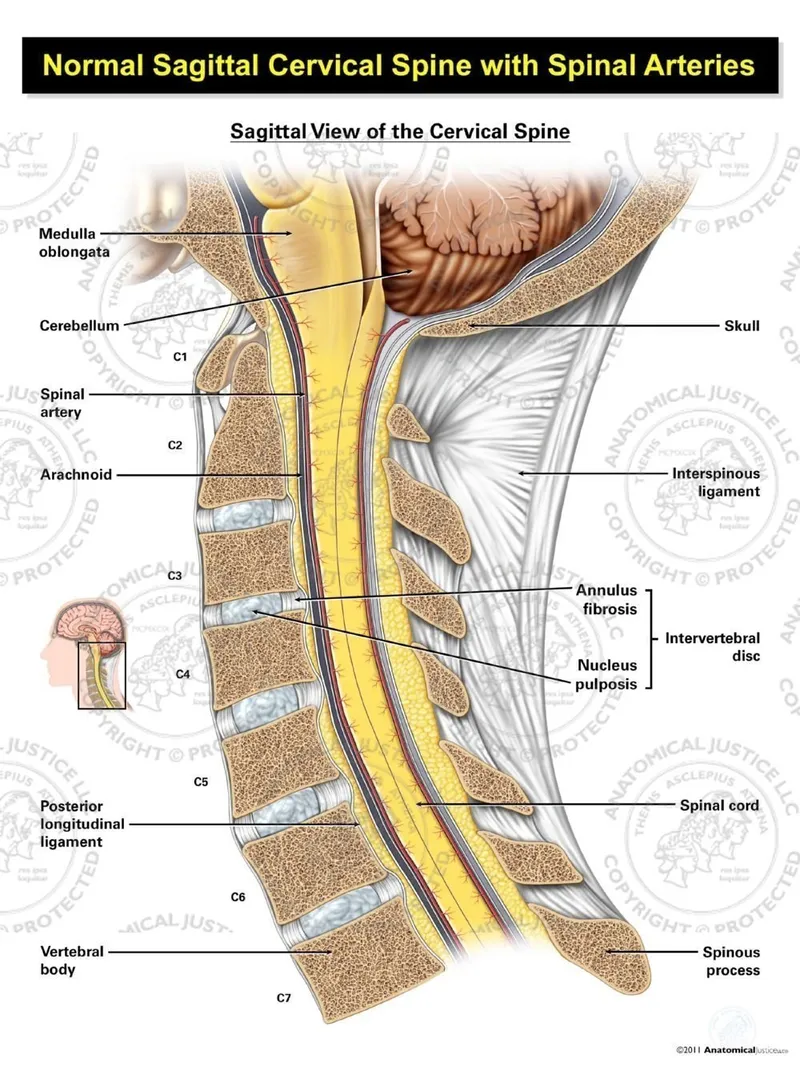
- Joints & Artery Path:
- Uncovertebral (Luschka): C3-C7, guide motion.
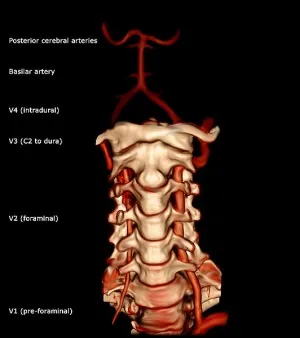
- Vertebral Artery: Enters C6 transverse foramen, ascends C1-C6.
⭐ The vertebral artery typically enters the transverse foramen at C6 and passes through C1-C6, but NOT C7.

- Nerve Root Exit:
- C1-C7: Above corresponding vertebra.
- C8: Below C7 (between C7-T1).
- Normal ROM (approx.): Flexion 45-50°; Extension 50-60°; Lat. Flexion 45°; Rotation 80° (C1-C2 ~50%).
Cervical Spondylosis & PIVD - Aging Neck Pains
Degenerative cascade: disc desiccation, osteophytes, facet arthropathy, ligamentum flavum hypertrophy. Common at C5-C6, C6-C7.
- Features: Axial neck pain, stiffness. Radiculopathy (Spurling's +ve; arm pain, weakness, paresthesia). Myelopathy (gait issues, UMN signs, bowel/bladder changes).
- Imaging:
- X-ray: Osteophytes, ↓ disc height, foraminal stenosis.
- MRI: Gold standard. Disc herniation (protrusion, extrusion, sequestration), cord compression/signal changes.

- Management:
- Conservative: Rest, NSAIDs, physiotherapy, collar.
- Surgical: Progressive neuro deficit, myelopathy, intractable pain after 6-12 wks conservative trial.
⭐ C5-C6 is the most common level affected by cervical spondylosis and disc herniation.
Cervical Myelopathy & Radiculopathy - Pinched Nerves & Cord
- Definitions: Myelopathy (spinal cord compression); Radiculopathy (nerve root compression).
- Causes: Spondylosis, PIVD, trauma, tumor.
| Feature | Cervical Myelopathy | Cervical Radiculopathy |
|---|---|---|
| Pathology | Cord Compression | Root Compression |
| Symptoms | Gait issues, clumsiness, bowel/bladder | Radicular pain/paresthesia |
| Signs (UMN) | Spasticity, ↑reflexes, Babinski, Hoffman's | - |
| Signs (LMN) | LMN signs at lesion level (sometimes) | Myotomal weakness, ↓reflexes |
- Myelopathy Severity Scales: Nurick grade, mJOA score.
- 📌 Mnemonic (Cervical Roots): "C5 keeps deltoids alive, C6 for biceps/wrist extension fix, C7 triceps/wrist flexion heaven, C8 finger flexion great, T1 intrinsics state."

⭐ Cervical myelopathy often presents with a combination of UMN signs below the level of compression and LMN signs at the specific level(s) of compression.
Cervical Spine Trauma - Fractures & Fixes
- Mechanisms: Flexion, Extension, Axial Load, Rotation.
- Stability: Denis 3-column (adapted): ≥2 columns → Unstable. White & Panjabi: >3.5mm displacement, >11° angulation.
- Clearance: NEXUS (No midline Tenderness, Intoxication, altered Alertness, Neuro deficit, Distracting injury). Canadian C-Spine Rule.
- Fractures:
- Jefferson (C1 burst): Axial load.

- Hangman's (C2): Hyperextension; C2 pars fracture.

- Odontoid (Dens) Fx:
- Type I: Tip (Stable).
- Type II: Base (Unstable). 📌 "Type II is Unstable & Nasty"
- Type III: Into C2 body (Stable).
- Teardrop Fx: Flexion (unstable) or Extension.
- Clay-shoveler's Fx: C7 spinous process; stable.
- Jefferson (C1 burst): Axial load.
- SCIWORA: Spinal Cord Injury Without Radiographic Abnormality (children).
- Management: ATLS, immobilization.
⭐ Type II Odontoid fractures are most common and have highest non-union risk due to precarious blood supply.
High‑Yield Points - ⚡ Biggest Takeaways
- Jefferson fracture: C1 burst due to axial load; highly unstable.
- Hangman's fracture: Traumatic spondylolisthesis of C2 over C3 (bilateral C2 pars fractures); unstable.
- Odontoid fractures: Type II is most common, most unstable, often needing surgery.
- Cervical spondylosis: Degenerative; osteophytes cause radiculopathy or myelopathy.
- Klippel-Feil syndrome: Congenital fusion; triad: short neck, low hairline, limited neck motion.
- Positive Spurling's test indicates radiculopathy; Hoffman's sign suggests myelopathy_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

