Upper Limb Prosthetics - Limb Loss Lowdown
-
Prosthesis: Artificial device replacing a missing body part. Orthosis: Device supporting/correcting a body part or its function.
-
Goals of UL Prosthetics: Restore function (grasp, reach), cosmesis, enable Activities of Daily Living (ADLs).
-
Amputation Levels & Fitting Implications:
- Forequarter: Loss of entire shoulder girdle; complex fitting, often cosmetic or body-powered hook.
- Shoulder Disarticulation (SD): Through shoulder joint; socket covers shoulder, suspension can be challenging.
- Transhumeral (TH/AE): Above elbow; requires elbow unit, good for myoelectric control.
- Elbow Disarticulation (ED): Through elbow joint; humeral condyles aid suspension, external elbow hinges.
- Transradial (TR/BE): Below elbow; common, good prosthetic function, some forearm rotation preserved.
- Wrist Disarticulation (WD): Through wrist; preserves distal radioulnar joint (DRUJ), allows some forearm rotation.
- Transcarpal: Through carpal bones; partial hand, often custom silicone restoration.
- Digital: Finger/thumb amputation; can be cosmetic or functional (e.g., opposition post).
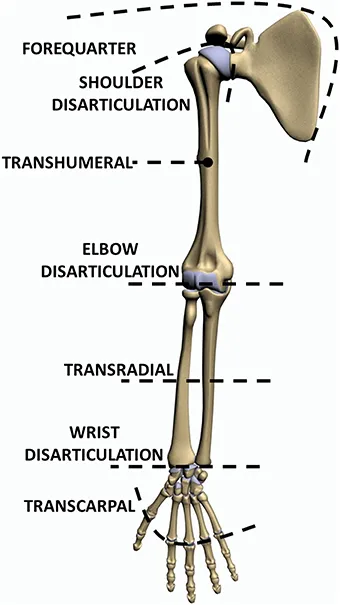
⭐ The transradial amputation is the most common major upper limb amputation level, offering good prosthetic function and versatility with various prosthetic designs.
Upper Limb Prosthetics - Armamentarium Array
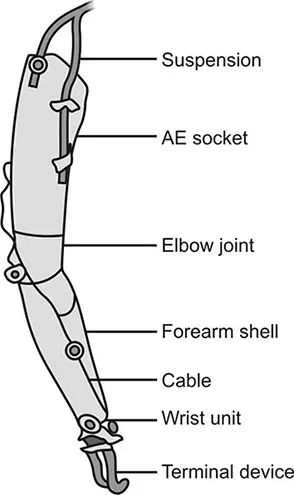
- Socket:
- Design: Total contact for optimal load distribution.
- Materials: Thermoplastic (e.g., polyethylene), laminated resins.
- Suspension Systems:
- Harness (e.g., Figure-of-8), suction (valve/sleeve), anatomical (supracondylar), osseointegration.
- Control Systems:
- Body-powered: Cables transmit body motion.
- Myoelectric: EMG sensors detect muscle signals.
- Terminal Devices (TDs):
- Hooks: Durable, precise, functional. Hands: Cosmetic, varied grip.
- Types: Passive (cosmetic), Body-powered (Voluntary Opening - VO / Voluntary Closing - VC), Externally powered (myoelectric).
⭐ Voluntary opening (VO) hooks are generally more durable and require less effort to operate for sustained grip than voluntary closing (VC) hooks.
- Wrist Units:
- Friction control, quick-disconnect, flexion/extension, rotation units.
- Elbow Units:
- Locking mechanisms (manual/automatic), passive (friction), active (body/external power).
- Shoulder Units:
- For high-level amputations (disarticulation/forequarter); passive or specialized joints.
Upper Limb Prosthetics - Pick Your Power-Arm
| Type | Mechanism of Action | Control Method | Energy Source | Advantages | Disadvantages |
|---|---|---|---|---|---|
| Passive | Static, cosmetic appearance | None | None | Lightweight, good cosmesis | No active function |
| Body-Powered | Cables & harness, body movement driven | Gross body motion | User's body | Durable, proprioception, lower cost | Harness discomfort, high effort |
| Myoelectric | EMG signals from residual muscles | Muscle contraction | Battery | Intuitive control, strong grip force | Heavy, expensive, needs maintenance |
| Hybrid | Combination of body & external power | Mixed | Mixed | Optimizes function/weight/cost | Can be complex to operate/maintain |
⭐ Myoelectric prostheses offer more natural control and grip strength but are heavier, more expensive, and require more maintenance than body-powered options.
Upper Limb Prosthetics - Fit, Function, Fixes
- Prosthetic Prescription Principles:
- Consider: Level of amputation, patient's functional needs, vocation, age, cognitive ability, personal preference, and cost.
- Key Prosthetic Checkout Points (Static & Dynamic Assessment):
- Fit: Snug socket, no pistoning, pressure distribution.
- Comfort: Absence of pain, wearable for daily activities.
- Function: Smooth operation of terminal device and controls.
- Alignment: Anatomically correct joint positioning, good posture.
- Cosmesis: Patient satisfaction with appearance.
- Common Stump & Prosthetic Complications:
- Stump Issues: Skin breakdown, edema, neuromas, phantom limb pain/sensation.
- Prosthetic Issues: Mechanical failure, socket discomfort, harness issues.
- Prosthetic Training & Rehabilitation Goals:
- Master donning/doffing, control strategies, functional task integration.
- Achieve maximal independence in Activities of Daily Living (ADLs).
⭐ The 'golden period' for fitting an upper limb prosthesis is generally considered to be within the first 30-90 days post-amputation for optimal functional outcomes.
High‑Yield Points - ⚡ Biggest Takeaways
- Transradial amputations (below-elbow) are the most common upper limb level.
- The Krukenberg operation creates a functional pincer from forearm bones (radius and ulna).
- Myoelectric prostheses are controlled by EMG signals from residual limb muscles.
- Terminal devices: Hooks offer superior function; hands provide better cosmesis.
- Proper socket fit is crucial for comfort, suspension, and prosthetic control.
- Shoulder disarticulation prostheses often require an external power source.
- Phantom limb pain is a frequent complication managed with multimodal therapy, not solely by prosthesis use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

