ULO: Principles & Classification - Ortho Blueprint
- Definition: External devices for upper limb; restore/improve function, limit motion, or support a segment.
- Goals:
- Immobilization (e.g., fracture, inflammation)
- Mobilization (e.g., contracture, post-surgery)
- Restriction of unwanted motion
- Torque transmission
- Classification by Function:
- Static: No moving parts. Provide support, protection, positioning.
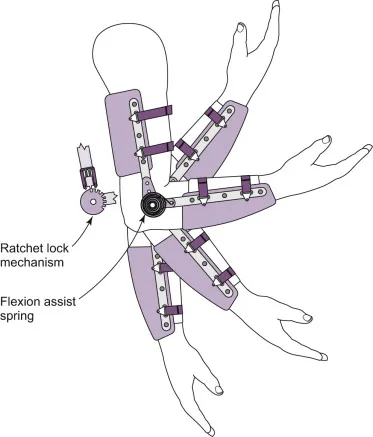
- Dynamic: Incorporate resilient components (springs, elastics). Assist movement, apply controlled force.
- Hybrid: Combine static and dynamic features.
- Nomenclature: Based on joints they encompass (e.g., HO: Hand Orthosis; WHO: Wrist-Hand Orthosis; EWHO: Elbow-Wrist-Hand Orthosis).
⭐ Static orthoses provide rigid support for immobilization, protection, or positioning, while dynamic orthoses incorporate resilient components (springs, elastic bands) to generate force, assist movement, or provide controlled resistance.
 oka
oka
Shoulder & Elbow Orthoses - Proximal Protectors
- Shoulder Orthoses:
- Sling: Support & immobilization.
- Uses: Clavicle/humerus fractures, dislocations, soft tissue injuries.
- Airplane Splint: Abduction (~90°).
- Uses: Brachial plexus injury, post-rotator cuff repair, axillary burns.
⭐ An airplane splint, maintaining the shoulder in approximately 90° abduction, is commonly used for brachial plexus injuries (e.g., Erb's palsy recovery) or post-rotator cuff repair to offload tension.
- Shoulder Immobilizer/Abduction Pillow: Post-op; controls abduction/rotation.
- Sling: Support & immobilization.
- Elbow Orthoses:
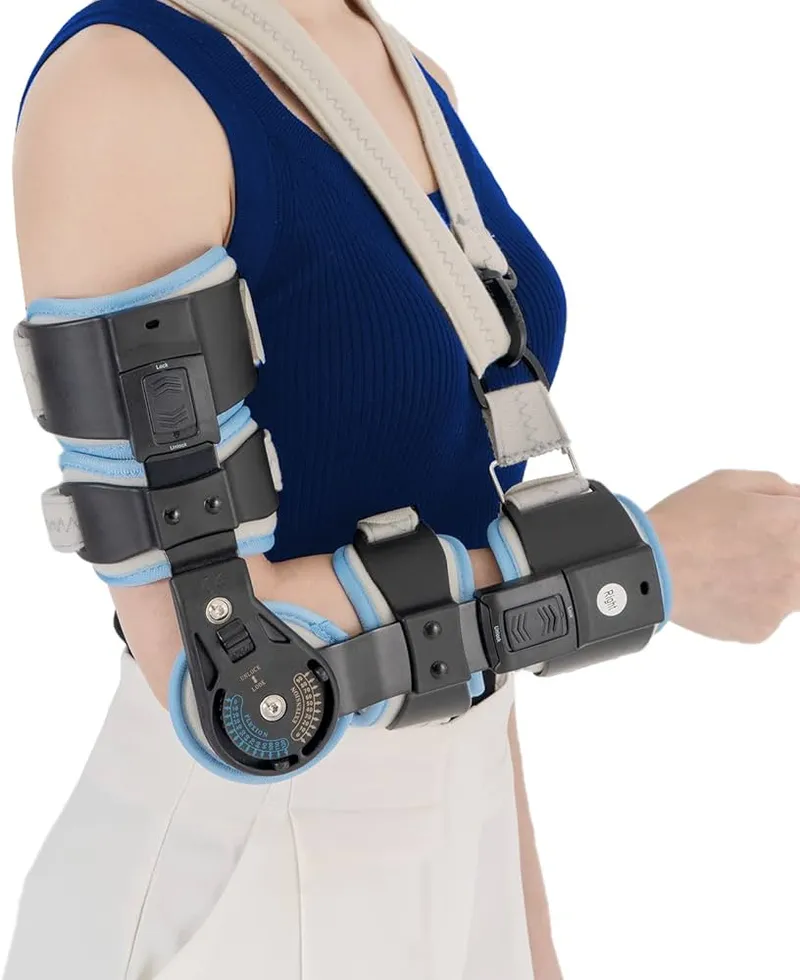
- Hinged Elbow Brace: Controlled ROM.
- Uses: Post-surgery, stable fractures.
- Posterior Elbow Splint/Immobilizer: Immobilization.
- Uses: Acute injuries, unstable fractures.
- Hinged Elbow Brace: Controlled ROM.
Wrist & Hand Orthoses - Dexterity Dynamos
- Goals: ↑ Function, ↓ Pain, Prevent/correct deformity.
- Types:
- Static: Immobilize, position (e.g., Resting Hand Splint).
- Dynamic: Assist/control motion (e.g., outrigger for tendon repair).
- Wrist Orthoses:
- Cock-up Splint:
- Wrist 15-30° ext. 📌 Cock-up for Carpal Tunnel.
- Uses: CTS, sprains, tendinitis.
⭐ A cock-up splint, maintaining the wrist in 15-30° of extension, is a first-line conservative treatment for Carpal Tunnel Syndrome by maximizing carpal tunnel volume.
- Thumb Spica Splint:
- Immobilizes thumb CMC & MCP. 📌 Spica: Scaphoid, Skier's.
- Uses: De Quervain's, scaphoid #, UCL injury.
- Cock-up Splint:
- Hand Orthoses:
- Ulnar Deviation Splint: For RA ulnar drift.
- Finger Splints: Mallet (DIP ext), Boutonniere (PIP ext).
- Resting Hand Splint: Functional position (Wrist 10-20° ext, MCP 45-60° flex).
 oka
oka
Nerve Palsy Orthoses - Neural Navigators
-
Goal: Maintain functional hand position, prevent contractures, assist weak muscles, & promote recovery.
-
Types: Static (immobilize, support) vs. Dynamic (assist movement, apply controlled force).
-
Radial Nerve Palsy (Wrist Drop):
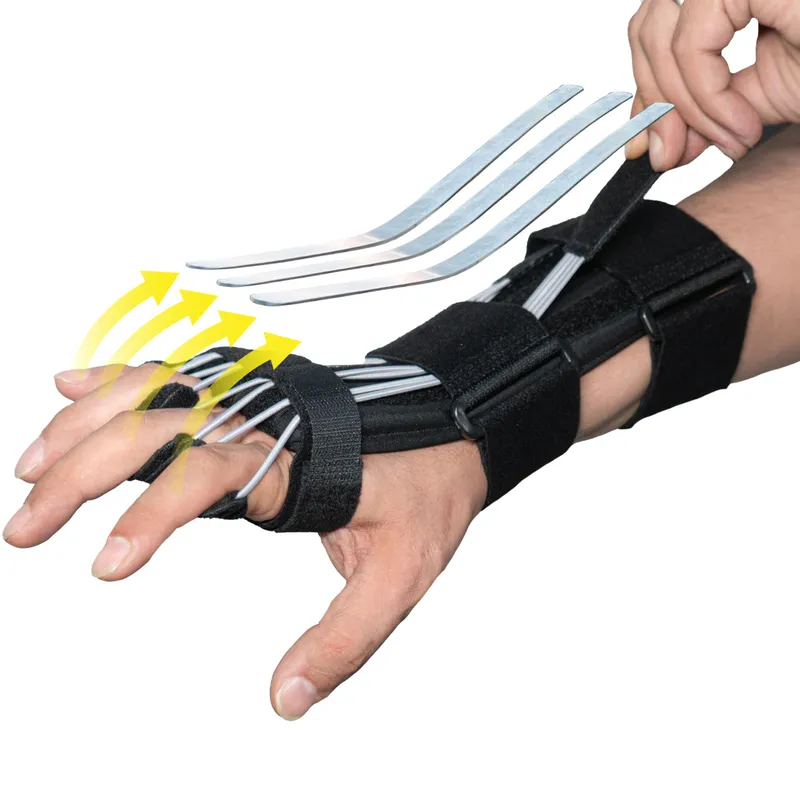
- Orthosis: Wrist cock-up splint (static) or dynamic wrist extension outrigger.
- Function: Supports wrist in extension, allows finger flexion/extension.
- Components: Forearm piece, wrist support, outriggers for MCP extension assist, thumb abduction/extension piece.
⭐ For radial nerve palsy presenting with wrist drop, a dynamic orthosis with MCP extension outriggers and thumb support is crucial to prevent contractures and assist function during nerve recovery.
-
Ulnar Nerve Palsy (Claw Hand - 4th & 5th digits):
- Orthosis: Anti-claw splint / MCP flexion block / lumbrical bar.
- Function: Prevents MCP hyperextension & promotes IP extension of ulnar digits.
-
Median Nerve Palsy (Ape Hand / Benediction Hand):
- Orthosis: Thumb opposition splint (C-bar, thumb spica with opposition post), anti-ape thumb deformity splint.
- Function: Maintains thumb in opposition, preserves web space.
-
Combined Palsies (e.g., Median & Ulnar):
- Orthosis: Custom-designed to address specific deficits, e.g., figure-of-eight splint for combined clawing and thumb adduction.
-
General Principles:
- Lightweight, comfortable, cosmetically acceptable.
- Easy to don/doff.
- Regular follow-up for adjustments. (📌 CARE: Check skin, Adjust fit, Review exercises, Ensure compliance).
High‑Yield Points - ⚡ Biggest Takeaways
- Static orthoses immobilize and support; dynamic orthoses assist or permit motion.
- Cock-up splint for wrist extension (e.g., radial nerve palsy, carpal tunnel syndrome).
- Airplane splint for shoulder abduction (e.g., brachial plexus injury, burns).
- Thumb spica splint immobilizes thumb (e.g., De Quervain's, scaphoid fracture).
- Figure-of-eight splint commonly treats clavicle fractures.
- Knuckle bender splint aids MCP flexion in ulnar nerve palsy.
- Material choice (thermoplastic, metal) dictates rigidity and wear duration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

