Modern Prosthetics - Bionic Breakthroughs Beckon
- Aim: Maximize function restoration, significantly improve user's quality of life.
- Core Principles:
- Intuitive Control: Myoelectric sensors, brain-computer interfaces (BCIs).
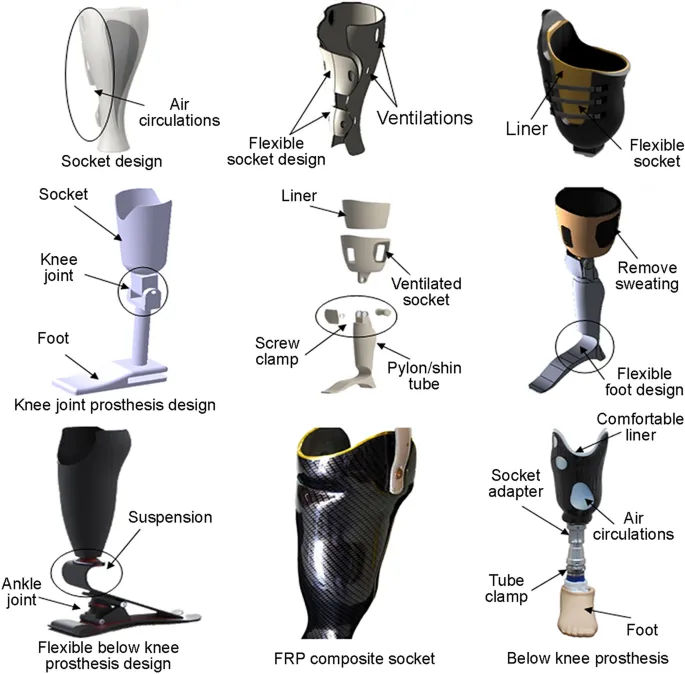
- Enhanced Comfort: Custom sockets, lighter materials (e.g., carbon fiber).
- Superior Cosmesis: Realistic appearance, matching skin tones.
- Emerging Technologies:
- Targeted Muscle Reinnervation (TMR) for more natural control.
- Osseointegration for direct skeletal attachment, improved proprioception.
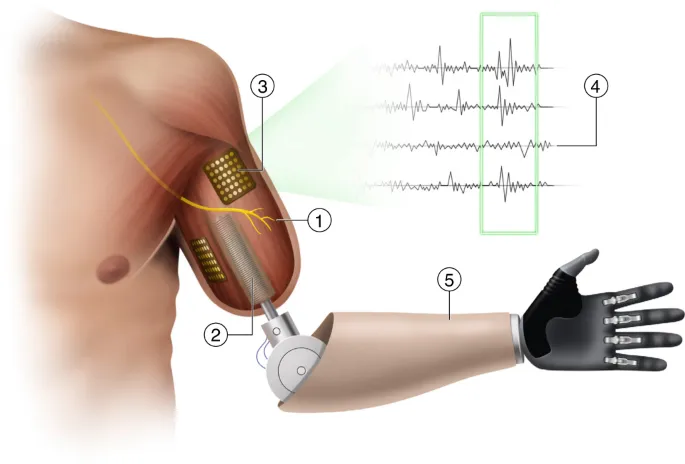
⭐ The primary goal of modern prosthetics is to restore maximum possible function and improve quality of life, focusing on aspects like intuitive control, comfort, and cosmesis.
Materials & Manufacturing - Building Better Bionics
-
Advanced Manufacturing:
- CAD/CAM: Precise digital design for custom-fit components.
- 3D Printing (Additive Manufacturing): Rapid creation of complex, lightweight, patient-specific parts.
-
Key Materials:
| Material | Properties | Primary Uses |
|---|---|---|
| Carbon Fiber | ↑Strength-to-weight, energy return, durable | Pylons, dynamic feet, keels |
| Titanium Alloys | ↑Strength, biocompatible, corrosion-resistant | Endoskeletal parts, joints |
| Silicone | Flexible, comfortable, skin-like, good grip | Liners, sleeves, cosmetic covers |
| Thermoplastics | Moldable, adjustable, lightweight, cost-effective | Sockets (esp. preparatory) |
Neural Interfaces - Mind-Moving Miracles
Harnessing the body's signals for intuitive prosthetic control.
- Myoelectric Control (EMG): Surface electrodes detect muscle electrical signals, translating intent into prosthetic movement.
- Targeted Muscle Reinnervation (TMR):
⭐ Targeted Muscle Reinnervation (TMR) surgically re-routes residual peripheral nerves to reinnervate new muscle targets, providing more intuitive and distinct EMG signals for prosthetic control.
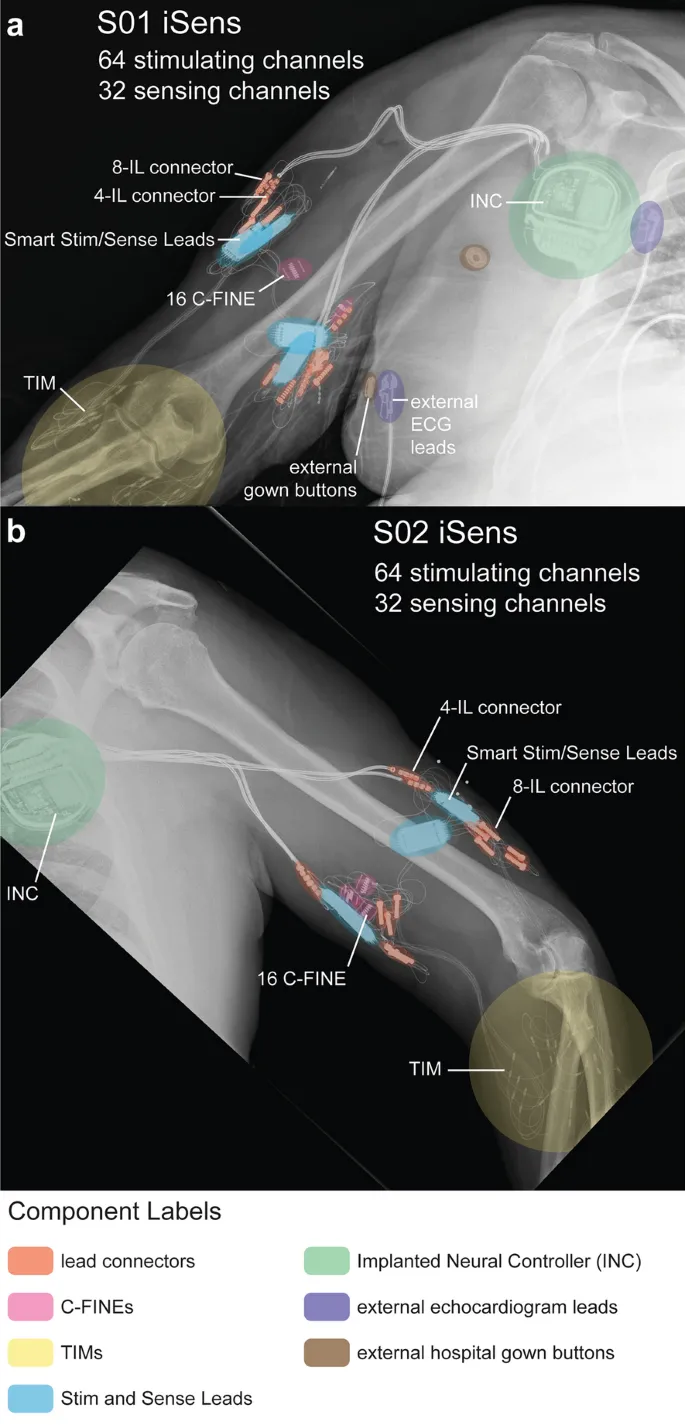
- Implanted Myoelectric Sensors (IMES): Electrodes in muscle offer higher fidelity signals.
- Brain-Computer Interfaces (BCIs): Emerging; directly decodes brain activity (EEG/ECoG) for control.
- Pattern Recognition: Algorithms interpret complex signals for smoother, natural prosthesis function.
Osseointegration & Sensation - Feeling Fused Future
- Osseointegration: Prosthesis directly anchored to bone.
- Pros: Enhanced stability, proprioception; eliminates socket problems (skin breakdown, discomfort).
- Cons: Surgical risks (infection), longer rehabilitation time.
⭐ Osseointegration offers direct skeletal attachment of prostheses, eliminating socket-related issues (like skin breakdown, poor fit) and improving proprioception and energy transfer.
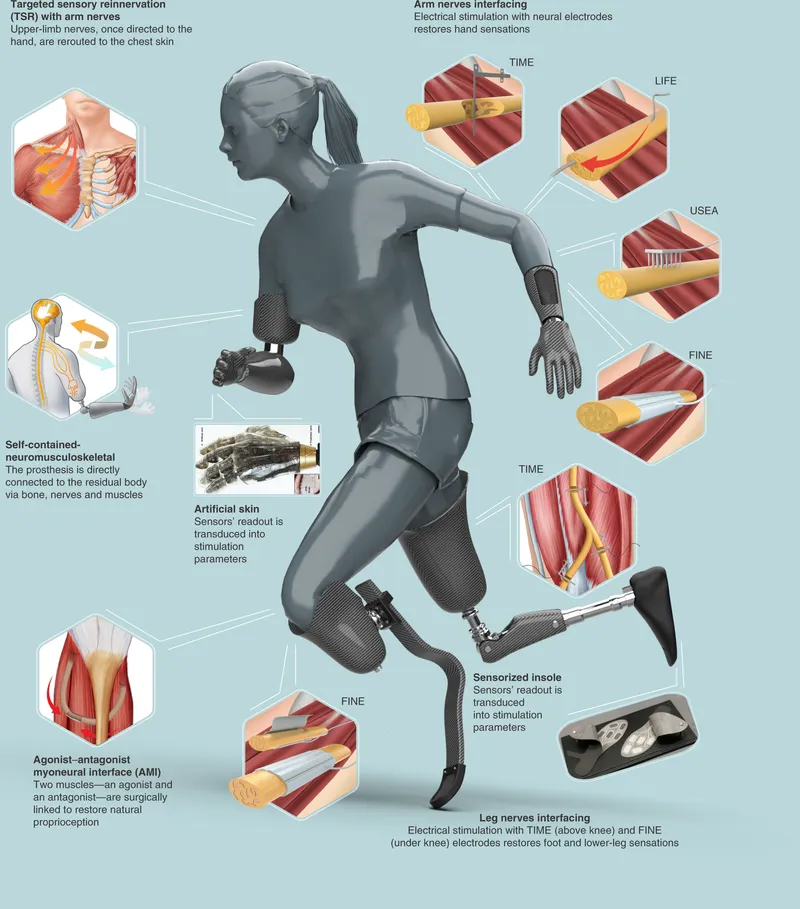
- Sensory Feedback Restoration:
- Targeted Muscle/Sensory Reinnervation (TMR/TSR): Redirected nerves enable intuitive control, sensation.
- Neural Interfaces: Direct nerve stimulation for touch/temperature.
- Impact: Better dexterity, reduced phantom pain, improved embodiment.
 oka
oka
Specialized Prosthetics - Tailored Tech Tomorrow
- Activity-Specific Prostheses:
- Tailored for sports (running blades), specific tasks.
⭐ Activity-specific prostheses, such as energy-storing running blades (e.g., Cheetah Flex-Foot), are designed to optimize performance for particular high-impact activities and sports.
- Advanced Myoelectric Control:
- EMG-driven, intuitive movement.
- Pattern recognition for multiple grips.
- Targeted Muscle Reinnervation (TMR):
- Amplifies control signals for complex prostheses.
- Osseointegration:
- Direct skeletal attachment; improved stability, proprioception.
- Eliminates socket issues.
- Emerging: Brain-Computer Interfaces (BCIs), sensory feedback.

High‑Yield Points - ⚡ Biggest Takeaways
- Myoelectric prostheses are controlled by EMG signals from residual muscles, offering intuitive movement.
- Targeted Muscle Reinnervation (TMR) significantly improves myoelectric control, especially for proximal amputations.
- Osseointegration involves direct skeletal attachment, enhancing load transfer and sensory feedback.
- Microprocessor-Controlled Knees (MPKs) adapt to gait variations, improving safety and reducing falls.
- Advanced materials (e.g., carbon fiber, titanium) create lightweight, durable, and high-strength prostheses.
- 3D printing facilitates cost-effective, patient-specific socket design and component manufacturing.
- Emerging sensory feedback systems aim to restore proprioception and tactile sensation to users.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

