Lower Limb Prosthetics: Amputation Levels & Basics - Stump Savvy
- Key Amputation Levels:
- Transfemoral (AK): Above knee. Length: 25-30 cm from Gr. Trochanter. Adductor magnus preservation vital.
- Transtibial (BK): Below knee. Most common. Length: 12-17 cm from Med. Tibial Plateau. Long posterior flap preferred. Knee function key.
- Syme's: Ankle disarticulation. Heel pad preserved. Good for end-bearing.
- Ideal Stump Features:
- Shape: Conical/cylindrical.
- Skin: Healthy, mobile scar (posterior in BK).
- Muscles: Stable (myodesis/myoplasty), well-padded.
- No pain, neuroma, bony spurs.

⭐ For Transtibial (BK) amputations, a stump length <5 cm is generally inadequate for prosthetic fitting.
Lower Limb Prosthetics: Prosthetic Components - Limb Lego
- Socket: Interface between residual limb & prosthesis; crucial for comfort & function.
- Types: Patellar Tendon Bearing (PTB), Total Surface Bearing (TSB).
- Materials: Thermoplastics, laminated resins.
- Suspension System: Secures prosthesis to the limb.
- Methods: Suction (total/partial), Silesian belt, pelvic band, shuttle lock/pin system, vacuum-assisted.
- Shank (Pylon): Connects socket to ankle/foot; provides structural support & length.
- Types: Endoskeletal (modular), Exoskeletal (crustacean).
- Knee Unit (for transfemoral/knee disarticulation):
- Axes: Single-axis, polycentric.
- Control: Mechanical friction, hydraulic/pneumatic, microprocessor-controlled (MPC).
- Ankle-Foot Assembly: Restores foot functions; shock absorption, stability.
- Types: SACH (Solid Ankle Cushion Heel), SAFE, Dynamic Response (Energy Storing), Microprocessor Ankles.
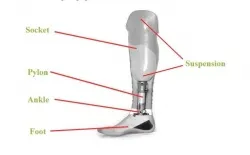
⭐ The SACH (Solid Ankle Cushion Heel) foot is the most basic and widely prescribed prosthetic foot, especially in resource-limited settings, offering durability but limited multi-axial movement and energy return.
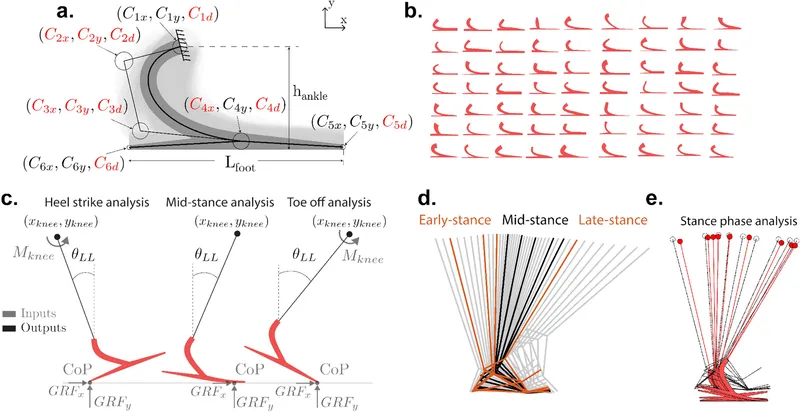
Lower Limb Prosthetics: Gait & Biomechanics - Robo Rhythms
- Goal: Smooth, symmetrical, energy-efficient gait.
- Key Biomechanics: Pelvic motion, knee flexion (stance/swing), prosthetic foot/ankle function.
- Common Gait Deviations (Causes):
- Transfemoral (AK):
- Circumduction (Prosthesis long, ↓ knee flexion).
- Lateral Trunk Bend (Weak abductors, short prosthesis, pain).
- Vaulting (Prosthesis long, poor suspension).
- Transtibial (BK):
- Excessive Knee Flexion - Stance (Stiff heel, socket anterior).
- Insufficient Knee Flexion - Stance (Soft heel, socket posterior).
- Foot Slap (Weak PF bumper, poor fit).
- Transfemoral (AK):
- Energy Cost: ↑ with amputation level.
- Transtibial: ~20% ↑
- Transfemoral (Uni): ~70% ↑
- Bilateral TF: >200% ↑
⭐ > Vaulting (rising on sound limb toe) often indicates the prosthesis is too long or there's insufficient knee flexion during swing.
Lower Limb Prosthetics: Prescription & Complications - Fine-Tune & Fixes
- Prescription Factors: Amputation level (e.g., Transtibial, Transfemoral), K-Levels (K0-K4 for activity/ambulation potential), patient goals, comorbidities.
- Prosthetic Checkout (Fine-Tuning):
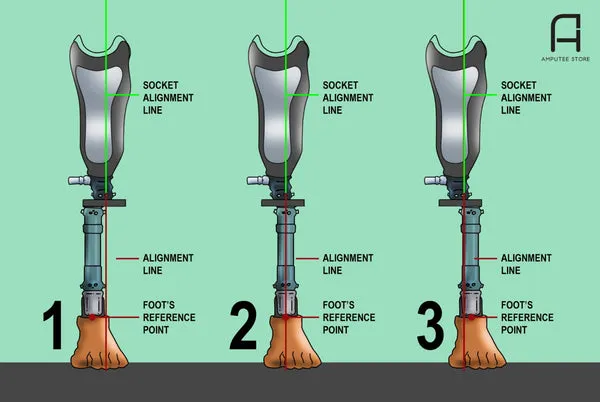
- Static Assessment: Socket fit (e.g., total surface bearing, ischial containment), prosthesis length, suspension efficacy, standing alignment.
- Dynamic Assessment: Gait analysis for smoothness, symmetry, and common deviations (e.g., lateral trunk bending, circumduction, vaulting, foot slap).
- Common Complications & Fixes:
- Skin Issues (e.g., breakdown, dermatitis, infection): Optimize socket fit, improve hygiene, change interface material, manage infection.
- Socket Fit Problems (e.g., pistoning, bell-clanging, localized pain): Socket adjustments (padding, flaring), relining, or new socket fabrication.
- Gait Deviations & Adjustments:
- Lateral Trunk Bending: Correct prosthesis length, address abductor weakness, adjust medial socket wall.
- Circumduction: Shorten prosthesis, reduce knee friction/extension assist.
⭐ Pistoning (vertical movement of residual limb within the socket) is a key indicator of poor suspension or significant residual limb volume change, requiring urgent prosthetic review.
- Phantom Limb Pain vs. Stump Pain: Differentiate for appropriate management (medical, therapy, prosthetic adjustments).
High‑Yield Points - ⚡ Biggest Takeaways
- Transtibial (BK) prostheses are generally more common and allow better function than transfemoral (AK).
- The SACH (Solid Ankle Cushion Heel) foot is a basic, durable, and inexpensive option, often used for initial ambulation.
- Energy-storing feet (e.g., Flex-Foot, carbon fiber) improve gait efficiency and are preferred for active individuals.
- Socket design is critical: Patellar Tendon Bearing (PTB) for BK and Ischial Containment for AK are key concepts for weight distribution and stability.
- Phantom limb pain is a frequent and significant post-amputation issue requiring multimodal management, including medication and therapy.
- Proper prosthetic alignment and socket fit are essential to prevent gait deviations, skin breakdown, and discomfort.
- Osseointegration offers direct skeletal attachment, an advanced option for select patients with problematic socket wear.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

