Pediatric Bone and Joint Infections - Tiny Bones, Big Trouble
Rapidly progressive infections requiring prompt diagnosis and treatment to prevent long-term sequelae like growth disturbance or chronic infection.
-
Osteomyelitis: Inflammation/infection of bone, typically metaphyseal in children due to rich vascular supply and sluggish flow in sinusoidal veins.
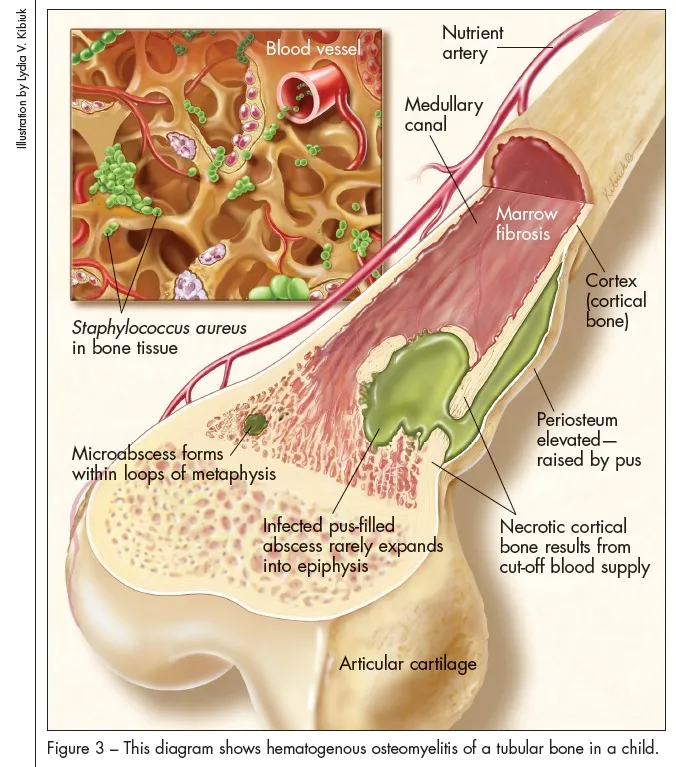
-
Septic Arthritis: Infection within a joint space, most commonly affecting hip or knee.
-
Common Pathogens by Age:
Age Group Predominant Organisms Neonates (<2 months) S. aureus, Group B Streptococcus (GBS), E. coli Infants (2 mo - 5 yrs) S. aureus, Strep. pneumoniae, Kingella kingae Children (>5 yrs) S. aureus (most common), Strep. pyogenes (Group A Strep)
⭐ Staphylococcus aureus is the most common causative organism overall in both pediatric osteomyelitis and septic arthritis across all age groups after the neonatal period for septic arthritis, and overall for osteomyelitis.
Pediatric Bone and Joint Infections - Bone Under Siege
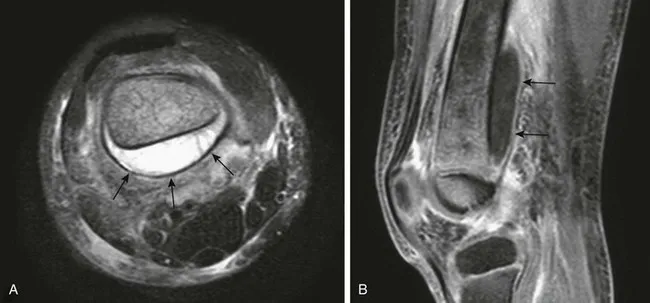
-
Acute Hematogenous Osteomyelitis (AHO):
- Sites: Metaphysis of long bones (femur, tibia).
- Pathogens: S. aureus (most common), Kingella kingae (<4 yrs), Salmonella (sickle cell disease). Neonates: Group B Strep, E. coli.
- Sx: Fever, localized pain/tenderness, limp/pseudoparalysis.
- Labs: ↑CRP (>20 mg/L), ↑ESR (>20 mm/hr). Blood culture.
- Imaging: X-ray (late: periosteal reaction 10-14 days). MRI (best for early diagnosis). Ultrasound (subperiosteal abscess).
- Rx: IV Antibiotics (total 3-6 weeks; initial IV, then PO), e.g., Cloxacillin/Nafcillin or Vancomycin. Surgical drainage if abscess or no response.
- 📌 Mnemonic "LOVES": Long bones, Often metaphyseal, Vascular (hematogenous), ESR/CRP ↑, Staph aureus.
-
Septic Arthritis: Often co-exists or mimics AHO.
- Sx: Acute joint pain, swelling, warmth, ↓Range of Motion, fever.
- Dx: Joint aspiration (WBC >50,000/μL, >75% PMNs, Gram stain, culture).
- Rx: IV antibiotics, prompt surgical drainage.
⭐ MRI is the most sensitive and specific imaging modality for early diagnosis of AHO, detecting changes within 24-48 hours of onset.
Pediatric Bone and Joint Infections - Joint Jeopardy
Septic arthritis (SA) is a joint space infection. Hip & knee are most common. Staphylococcus aureus is the usual culprit; Kingella kingae in toddlers.
Kocher Criteria for Septic Hip (📌 Mnemonic: FENS)
- Fever > 38.5°C
- ESR > 40 mm/hr
- Non-weight bearing (inability to walk/crawl)
- Serum WBC > 12,000/mm³ Each criterion scores 1 point. SA Probability: 0 pts (<0.2%), 1 pt (3%), 2 pts (40%), 3 pts (93%), 4 pts (99%).
Synovial Fluid Analysis in SA
- Appearance: Turbid, purulent
- WBC: > 50,000/mm³ (often > 100,000/mm³)
- PMNs: > 75%
- Gram Stain: Positive in ~30-50%
- Culture: Definitive diagnosis
- Glucose: ↓ (compared to serum)
Diagnosis & Management
- Ultrasound: Detects effusion.
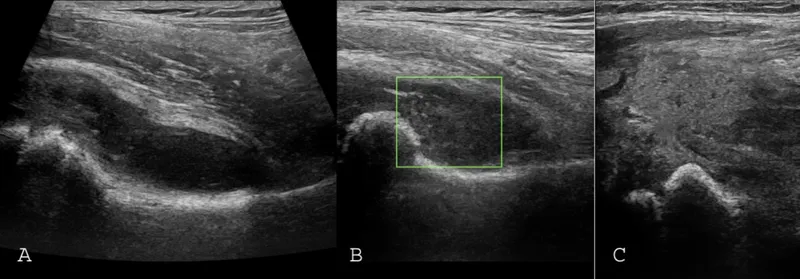
- Arthrocentesis (joint aspiration): Essential for diagnosis.
- Treatment: Prompt surgical drainage (arthrotomy/arthroscopy) & IV antibiotics.
⭐ Septic arthritis of the hip is an orthopaedic emergency requiring prompt surgical drainage and antibiotics to prevent long-term sequelae like avascular necrosis or growth disturbance.
Pediatric Bone and Joint Infections - Special Cases & Aftermath
- Neonatal Osteomyelitis:
- Presents subtly: pseudoparalysis, irritability, ↓feeding.
- Often multifocal; epiphysis commonly affected (transphyseal spread).
- Causative agents: GBS, S. aureus, Gram-negatives (E. coli).
- High risk: growth plate damage, joint destruction.
- Chronic Recurrent Multifocal Osteomyelitis (CRMO):
- Autoinflammatory bone disorder; non-infectious.
- Symmetrical lesions; clavicle, long bone metaphyses.
- Dx of exclusion; biopsy: sterile inflammation.
- Rx: NSAIDs, bisphosphonates, TNF-α inhibitors.
- Sequelae of Infections:
- Growth disturbances: limb length discrepancy, angular deformities (physeal damage).
- Chronic osteomyelitis (Brodie's abscess - localized, walled-off).
- Pathological fractures.
- Joint stiffness, ankylosis, AVN femoral head.
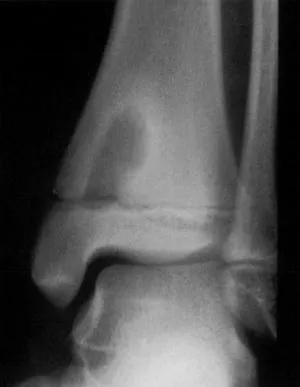
⭐ Neonatal osteomyelitis often presents with subtle signs like pseudoparalysis and can be multifocal, commonly affecting the epiphysis due to unique vascular supply.
High‑Yield Points - ⚡ Biggest Takeaways
- S. aureus is the most common pathogen; consider Kingella kingae in children <3 years.
- Neonatal osteomyelitis: often Group B Strep or E. coli, can be multifocal, may involve epiphysis.
- Kocher criteria (fever, non-weight bearing, ↑ESR, ↑WBC) strongly suggest septic hip arthritis.
- Acute osteomyelitis typically affects long bone metaphysis; MRI is best for early diagnosis.
- Septic arthritis of the hip is an orthopedic emergency requiring urgent surgical drainage and antibiotics.
- Brodie's abscess is a chronic, localized osteomyelitis, appearing as a lytic lesion with sclerotic rim on X-ray.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

