Introduction & Epidemiology - Tiny Twisted Toes
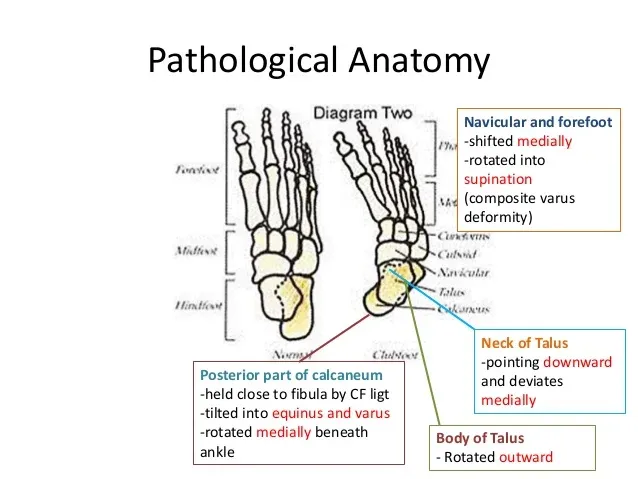
- Definition: Clubfoot (Congenital Talipes Equinovarus - CTEV) is a common, complex congenital foot deformity characterized by abnormal bone positioning and soft tissue contractures.
- Key Components (📌 CAVE): Midfoot Cavus, Forefoot Adductus, Hindfoot Varus, and Hindfoot Equinus.
- Incidence: Affects 1-2 per 1000 live births.
- Risk Factors & Associations:
- Male predominance (M:F = 2:1).
- Bilateral in approximately 50% of cases.
- Positive family history.
- Associated syndromes (e.g., spina bifida).
- Etiology: Largely idiopathic; multifactorial (genetic, intrauterine factors).
⭐ Clubfoot (CTEV) is the most common major congenital musculoskeletal deformity.
Clinical Features & Diagnosis - Spotting the Bend
- Typically painless at birth; rigid deformity.
- 📌 CAVE components define the deformity:
- Cavus: ↑ medial longitudinal arch.
- Adductus (forefoot): Medial deviation.
- Varus (hindfoot): Inversion, heel turns inward.
- Equinus (hindfoot): Plantarflexion, foot points down.
- Affected foot & calf often smaller, shorter.
- Deep posterior & medial skin creases; empty heel pad.
- Diagnosis: Primarily clinical. X-rays (AP/Lat stressed views) for severity assessment & post-treatment monitoring.
- Associated conditions: Check for DDH (~5%), spinal anomalies.
⭐ The CAVE acronym (Cavus, Adductus, Varus, Equinus) describes the four key deformities of clubfoot.
Classification Systems - Sorting the Shapes
- Pirani Score (0-6): Assesses severity for Ponseti. Higher score = more severe.
- Components (6 signs, each scored 0, 0.5, or 1):
Part Sign Hindfoot Posterior Crease (PC) Empty Heel (EH) Rigid Equinus (RE) Midfoot Medial Crease (MC) Curved Lateral Border (CLB) Talar Head Palpation (THP) - Interpretation: Score >4 = severe (more intervention); <2.5 = mild.
- Components (6 signs, each scored 0, 0.5, or 1):
- Dimeglio Score (0-20): Comprehensive.
- Grades: Benign (<5), Moderate (5-9), Severe (10-14), Very Severe (15-20).
⭐ The Pirani score is crucial for assessing severity and monitoring response to Ponseti treatment.
Management Principles - Straightening the Steps
- Ponseti Method (Gold Standard):
- Weekly serial casting (corrects CAVE).
- PAT for residual equinus.
- Final cast (3 wks post-PAT).
- Bracing (Foot Abduction Brace - FAB): Critical to prevent relapse.
- Full-time: 23 hours/day for initial 3 months.
- Part-time: Night & naps until 4-5 years of age.
- 📌 Mnemonic (Correction Order): C.A.V.E. (Cavus, Adductus, Varus, Equinus). Equinus corrected last.
- Surgical options (e.g., PMR): For resistant, recurrent, or late-presenting cases.
⭐ The Ponseti method is the gold standard for clubfoot treatment, achieving >90% success with proper adherence.
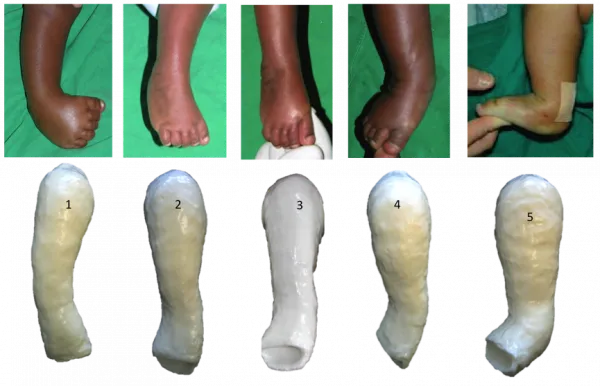
Complications & Prognosis - Future Footprints
- Relapse: Most common; paramount importance of brace compliance.
- Risk factors: poor adherence, severe initial deformity, atypical/complex clubfoot.
- Residual Deformities:
- Dynamic supination (tibialis anterior overactivity).
- Persistent forefoot adductus/cavus.
- Iatrogenic: Rocker-bottom foot; Avascular Necrosis (AVN) of talus (rare, post-extensive surgery).
- Other: Skin irritation/pressure sores (from cast/brace); joint stiffness.
- Prognosis: Generally excellent with Ponseti method; aiming for pain-free, plantigrade, functional foot.
- Foot may be 1-1.5 sizes smaller; calf hypoplasia common.
- Long-term: Good function, active life possible.
⭐ Relapse, often due to non-compliance with bracing, is the most common complication after initial correction of idiopathic clubfoot treated with the Ponseti method.
High-Yield Points - ⚡ Biggest Takeaways
- Clubfoot (CTEV) presents with CAVE deformity: Cavus, Adductus, Varus, Equinus.
- Idiopathic type is most common; rule out syndromic causes (e.g., spina bifida, arthrogryposis).
- Ponseti method is the gold standard treatment, involving serial casting and manipulation.
- Correction sequence: Cavus first, then Adductus/Varus, finally Equinus (often needing percutaneous Achilles tenotomy).
- Foot abduction bracing (e.g., Denis Browne splint) is crucial for 2-4 years post-correction to prevent relapse.
- Radiologically, Kite's angle (AP talocalcaneal angle) is decreased (<20°).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

