CP Basics - Brainy Beginnings
- Cerebral Palsy (CP): Permanent, non-progressive group of disorders affecting movement & posture.
- Etiology: Brain injury or malformation; prenatal, perinatal, or early postnatal (up to age 2-3 years).
- Key: Brain lesion is static; musculoskeletal manifestations can progress or change over time.
- Motor Types:
- Spastic (~75%): Most common; UMN lesion, velocity-dependent ↑tone.
- Dyskinetic (Athetoid, Dystonic): Involuntary movements; basal ganglia damage.
- Ataxic: ↓Balance & coordination; cerebellar lesion.
- Mixed patterns.
- GMFCS (Gross Motor Function Classification System): Levels I (most able) to V (severely limited).
⭐ Spastic diplegia is the most common pattern in premature infants, often linked to periventricular leukomalacia (PVL).

Ortho Manifestations - Twisted Troubles
- Spasticity & Dystonia: Primary motor disorders causing muscle imbalance, abnormal posture.
- Contractures: Fixed joint limitations. Common:
- Hip: Flexion, adduction (scissoring)
- Knee: Flexion
- Ankle: Equinus (toe-walking)
- Torsional Deformities: Rotational bone issues.
- Femur: ↑Anteversion (in-toeing)
- Tibia: External/Internal torsion
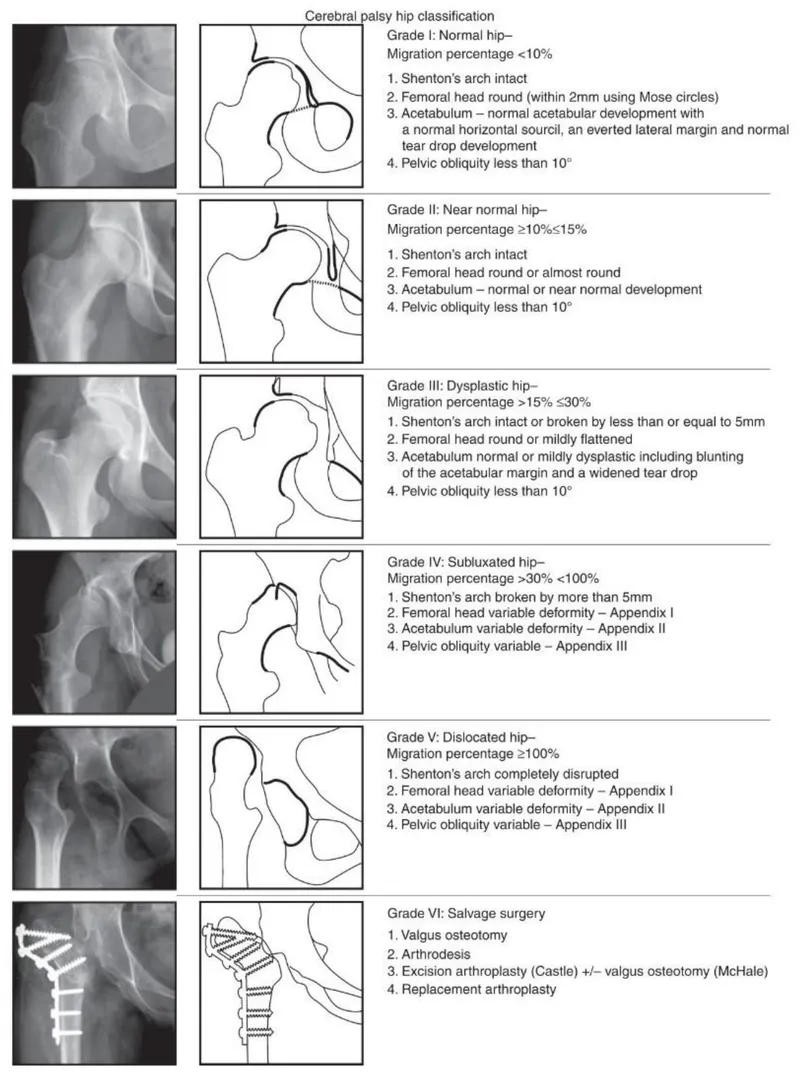
- Hip Dysplasia/Dislocation: Progressive. Risk ↑ with GMFCS level; ~50% in GMFCS V.
- Spinal Deformities: Scoliosis (most common), kyphosis, lordosis.
- Foot Deformities: Equinovarus, planovalgus common.
- Gait Patterns: Characteristic - Scissoring, crouch, equinus.
⭐ Hip subluxation/dislocation is common, especially in non-ambulatory children (GMFCS IV-V).
 in CP OR Post-operative rehabilitation protocols in CP orthopaedic surgery OR Long-term outcomes of orthopaedic interventions in CP OR Quality of life considerations in orthopaedic management of CP OR Ethical considerations in surgical decision-making for CP OR Team approach in managing orthopaedic aspects of CP diagram OR Cerebral palsy classification by motor type and topography diagram OR Common musculoskeletal problems in adults with cerebral palsy OR Transition of care for adolescents with CP to adult services OR Evidence-based guidelines for orthopaedic care in CP OR Latest research advancements in CP orthopaedics OR NEET PG high-yield orthopaedic facts about cerebral palsy OR Mnemonic for remembering GMFCS levels OR Visual guide to common orthopaedic deformities in CP OR Case study of a CP patient with multilevel orthopaedic issues OR Comparison of conservative vs surgical management in CP orthopaedics OR Red flags in orthopaedic assessment of a child with CP OR Importance of early detection of hip problems in CP OR Radiographic parameters for assessing hip dysplasia in CP OR Surgical techniques for correcting hip subluxation in CP OR Management of knee flexion contracture in CP OR Treatment options for equinus gait in CP OR Spinal fusion for scoliosis in CP indications and outcomes OR Foot and ankle surgery in CP objectives and procedures OR Upper limb orthopaedic problems in CP and their management OR Bone health and fracture risk in individuals with CP OR Pain management in orthopaedic conditions of CP OR Use of assistive technology in CP for orthopaedic goals OR Patient and family education in CP orthopaedic care OR Psychosocial impact of orthopaedic deformities in CP OR Role of orthopaedic surgeon in multidisciplinary CP team OR Common pitfalls in orthopaedic management of CP OR Medicolegal aspects in orthopaedic care of CP OR Future directions in orthopaedic research for CP OR Key orthopaedic syndromes associated with CP OR Genetic basis of CP and its orthopaedic implications OR Neuro-orthopaedic interface in CP management OR Biomechanics of gait deviations in CP OR Muscle pathology in spastic CP and its orthopaedic relevance OR Growth and development considerations in CP orthopaedics OR Nutritional status and its impact on orthopaedic outcomes in CP OR Sleep disturbances related to orthopaedic problems in CP OR Respiratory complications secondary to spinal deformities in CP OR Prevention of orthopaedic complications in CP OR Health-related quality of life measures in CP orthopaedic research OR Functional classification systems in CP beyond GMFCS OR Orthopaedic manifestations in different types of CP (spastic, dyskinetic, ataxic) OR Age-specific orthopaedic concerns in CP (infancy, childhood, adolescence, adulthood) OR Global perspectives on orthopaedic care for CP OR Cost-effectiveness of orthopaedic interventions in CP OR Telemedicine applications in CP orthopaedic follow-up OR Regenerative medicine approaches in CP orthopaedics OR Robotics and AI in CP rehabilitation and orthopaedics OR Patient-reported outcome measures (PROMs) in CP orthopaedic care OR Shared decision-making in CP orthopaedic surgery OR Cultural sensitivity in providing orthopaedic care for CP OR Advocacy for individuals with CP requiring orthopaedic services OR Orthopaedic considerations for sports and recreation in CP OR Management of fractures in children with CP OR Bone density assessment and osteoporosis prevention in CP OR Orthopaedic aspects of dystonia in CP OR Management of windswept deformity in CP OR Surgical correction of femoral anteversion in CP OR Tibial derotation osteotomy in CP indications OR Supramalleolar osteotomy for foot deformities in CP OR Triple arthrodesis in CP foot indications and outcomes OR Baclofen pump for spasticity management in CP orthopaedic context OR Selective dorsal rhizotomy (SDR) and its orthopaedic implications in CP OR Orthopaedic screening guidelines for children with CP OR Monitoring for scoliosis in CP patients OR Bracing for spinal deformities in CP effectiveness OR Femoral head resection (Girdlestone procedure) in CP hip OR Pelvic osteotomies for hip dysplasia in CP OR Soft tissue releases for contractures in CP OR Tendon transfers to improve muscle balance in CP OR Ilizarov technique in CP limb reconstruction OR Growth modulation techniques for angular deformities in CP OR Management of pathologic fractures in CP OR Orthopaedic care in the context of palliative care for CP OR Transitioning orthopaedic care from pediatric to adult providers for CP OR Research priorities in pediatric orthopaedics for cerebral palsy OR Common examination findings in orthopaedic assessment of CP OR Clinical scales used in CP orthopaedic evaluation OR Imaging modalities for orthopaedic problems in CP OR Conservative management strategies for CP orthopaedic issues OR Preoperative planning for orthopaedic surgery in CP OR Anesthesia considerations for orthopaedic surgery in CP OR Postoperative pain management in CP orthopaedic surgery OR Complication avoidance in CP orthopaedic surgery OR Rehabilitation protocols after specific orthopaedic procedures in CP OR Long-term follow-up after orthopaedic surgery in CP OR Evidence for specific orthopaedic interventions in CP (Cochrane reviews) OR Gait analysis interpretation in CP for surgical planning OR Orthotic prescription principles in CP OR Physical therapy goals in different stages of CP OR Occupational therapy interventions for upper limb function in CP OR Speech therapy for dysphagia related to postural issues in CP OR Social work support for families of children with CP undergoing orthopaedic treatment OR Psychological support for children with CP facing orthopaedic surgery OR Nutritional optimization before and after orthopaedic surgery in CP OR Bone mineral density in cerebral palsy and fracture risk OR Vitamin D deficiency in children with cerebral palsy OR Pathogenesis of contractures in cerebral palsy OR Molecular mechanisms of spasticity in cerebral palsy OR Genetic syndromes that can mimic cerebral palsy with orthopaedic features OR Differential diagnosis of early motor delay OR Developmental milestones and their relevance to CP diagnosis OR Role of MRI brain in predicting orthopaedic outcomes in CP OR Electrodiagnostic studies in CP (EMG, nerve conduction) OR Pharmacological management of spasticity in CP (oral medications) OR Intrathecal baclofen therapy for severe spasticity in CP OR Botulinum toxin A injections for focal spasticity in CP: mechanism and technique OR Phenol neurolysis for spasticity in CP OR Orthopaedic complications of spasticity medications OR Surgical management of spasticity (e.g., neurectomy, myelotomy) OR Multidisciplinary spasticity clinic model OR Spasticity assessment scales (e.g., Modified Ashworth Scale, Tardieu Scale) OR Range of motion assessment in CP OR Muscle strength testing in CP (challenges and modifications) OR Observational gait analysis in CP OR 3D gait analysis in CP: parameters and interpretation OR Energy expenditure during gait in CP OR Classification of hip displacement in CP (e.g., Reimers' Migration Percentage) OR Radiographic evaluation of the spine in CP (Cobb angle) OR Foot posture assessment in CP (e.g., Foot Posture Index) OR Upper extremity functional assessment in CP (e.g., QUEST, AHA) OR Patient-reported outcome measures for function and quality of life in CP OR Goal setting in CP rehabilitation (e.g., GAS - Goal Attainment Scaling) OR Principles of neurorehabilitation in CP OR Constraint-induced movement therapy (CIMT) for upper limb in CP OR Bimanual therapy for upper limb in CP OR Hippotherapy and therapeutic riding for CP OR Aquatic therapy for CP OR Strength training programs for children with CP OR Stretching and positioning programs for contracture prevention in CP OR Serial casting for contracture management in CP OR Orthotics for lower limb in CP (AFOs, KAFOs, SMOs) OR Orthotics for upper limb in CP (splints, braces) OR Wheelchair prescription and seating considerations in CP OR Adaptive equipment for activities of daily living in CP OR Augmentative and alternative communication (AAC) for children with CP OR Management of drooling in CP and its postural implications OR Feeding difficulties and nutritional support in CP OR Dental care in children with CP OR Sleep problems in children with CP and orthopaedic contributions OR Pain assessment and management in non-verbal children with CP OR Mental health issues in children with CP and their families OR Transition to adulthood for individuals with CP: orthopaedic and functional aspects OR Employment and independent living for adults with CP OR Sports and recreation for individuals with CP: orthopaedic considerations OR Advocacy and support groups for cerebral palsy OR Ethical dilemmas in the care of children with severe CP OR Research in cerebral palsy: current trends and future directions OR Global burden of cerebral palsy and access to orthopaedic care OR Cerebral palsy registries and their role in research and care improvement OR Telehealth in the management of cerebral palsy OR Assistive technologies and robotics in cerebral palsy rehabilitation OR Gene therapy and stem cell therapy for cerebral palsy: current status OR Prevention of cerebral palsy: antenatal and perinatal strategies OR Early diagnosis and intervention in cerebral palsy OR Neuroimaging findings in different types of cerebral palsy OR Classification of cerebral palsy (motor type, topography, GMFCS) OR Etiology and risk factors for cerebral palsy OR Pathophysiology of brain injury in cerebral palsy OR Epidemiology of cerebral palsy OR Definition of cerebral palsy OR History of understanding and treating cerebral palsy OR Windswept deformity X-ray CP OR Scoliosis X-ray CP GMFCS V OR Crouch gait CP photo OR Equinus foot CP photo OR Spastic hip dislocation CP radiograph OR Femoral anteversion clinical picture CP OR Tibial torsion clinical assessment CP OR Planovalgus foot CP X-ray OR GMFCS levels visual guide OR Orthopaedic manifestations CP summary diagram)
in CP OR Post-operative rehabilitation protocols in CP orthopaedic surgery OR Long-term outcomes of orthopaedic interventions in CP OR Quality of life considerations in orthopaedic management of CP OR Ethical considerations in surgical decision-making for CP OR Team approach in managing orthopaedic aspects of CP diagram OR Cerebral palsy classification by motor type and topography diagram OR Common musculoskeletal problems in adults with cerebral palsy OR Transition of care for adolescents with CP to adult services OR Evidence-based guidelines for orthopaedic care in CP OR Latest research advancements in CP orthopaedics OR NEET PG high-yield orthopaedic facts about cerebral palsy OR Mnemonic for remembering GMFCS levels OR Visual guide to common orthopaedic deformities in CP OR Case study of a CP patient with multilevel orthopaedic issues OR Comparison of conservative vs surgical management in CP orthopaedics OR Red flags in orthopaedic assessment of a child with CP OR Importance of early detection of hip problems in CP OR Radiographic parameters for assessing hip dysplasia in CP OR Surgical techniques for correcting hip subluxation in CP OR Management of knee flexion contracture in CP OR Treatment options for equinus gait in CP OR Spinal fusion for scoliosis in CP indications and outcomes OR Foot and ankle surgery in CP objectives and procedures OR Upper limb orthopaedic problems in CP and their management OR Bone health and fracture risk in individuals with CP OR Pain management in orthopaedic conditions of CP OR Use of assistive technology in CP for orthopaedic goals OR Patient and family education in CP orthopaedic care OR Psychosocial impact of orthopaedic deformities in CP OR Role of orthopaedic surgeon in multidisciplinary CP team OR Common pitfalls in orthopaedic management of CP OR Medicolegal aspects in orthopaedic care of CP OR Future directions in orthopaedic research for CP OR Key orthopaedic syndromes associated with CP OR Genetic basis of CP and its orthopaedic implications OR Neuro-orthopaedic interface in CP management OR Biomechanics of gait deviations in CP OR Muscle pathology in spastic CP and its orthopaedic relevance OR Growth and development considerations in CP orthopaedics OR Nutritional status and its impact on orthopaedic outcomes in CP OR Sleep disturbances related to orthopaedic problems in CP OR Respiratory complications secondary to spinal deformities in CP OR Prevention of orthopaedic complications in CP OR Health-related quality of life measures in CP orthopaedic research OR Functional classification systems in CP beyond GMFCS OR Orthopaedic manifestations in different types of CP (spastic, dyskinetic, ataxic) OR Age-specific orthopaedic concerns in CP (infancy, childhood, adolescence, adulthood) OR Global perspectives on orthopaedic care for CP OR Cost-effectiveness of orthopaedic interventions in CP OR Telemedicine applications in CP orthopaedic follow-up OR Regenerative medicine approaches in CP orthopaedics OR Robotics and AI in CP rehabilitation and orthopaedics OR Patient-reported outcome measures (PROMs) in CP orthopaedic care OR Shared decision-making in CP orthopaedic surgery OR Cultural sensitivity in providing orthopaedic care for CP OR Advocacy for individuals with CP requiring orthopaedic services OR Orthopaedic considerations for sports and recreation in CP OR Management of fractures in children with CP OR Bone density assessment and osteoporosis prevention in CP OR Orthopaedic aspects of dystonia in CP OR Management of windswept deformity in CP OR Surgical correction of femoral anteversion in CP OR Tibial derotation osteotomy in CP indications OR Supramalleolar osteotomy for foot deformities in CP OR Triple arthrodesis in CP foot indications and outcomes OR Baclofen pump for spasticity management in CP orthopaedic context OR Selective dorsal rhizotomy (SDR) and its orthopaedic implications in CP OR Orthopaedic screening guidelines for children with CP OR Monitoring for scoliosis in CP patients OR Bracing for spinal deformities in CP effectiveness OR Femoral head resection (Girdlestone procedure) in CP hip OR Pelvic osteotomies for hip dysplasia in CP OR Soft tissue releases for contractures in CP OR Tendon transfers to improve muscle balance in CP OR Ilizarov technique in CP limb reconstruction OR Growth modulation techniques for angular deformities in CP OR Management of pathologic fractures in CP OR Orthopaedic care in the context of palliative care for CP OR Transitioning orthopaedic care from pediatric to adult providers for CP OR Research priorities in pediatric orthopaedics for cerebral palsy OR Common examination findings in orthopaedic assessment of CP OR Clinical scales used in CP orthopaedic evaluation OR Imaging modalities for orthopaedic problems in CP OR Conservative management strategies for CP orthopaedic issues OR Preoperative planning for orthopaedic surgery in CP OR Anesthesia considerations for orthopaedic surgery in CP OR Postoperative pain management in CP orthopaedic surgery OR Complication avoidance in CP orthopaedic surgery OR Rehabilitation protocols after specific orthopaedic procedures in CP OR Long-term follow-up after orthopaedic surgery in CP OR Evidence for specific orthopaedic interventions in CP (Cochrane reviews) OR Gait analysis interpretation in CP for surgical planning OR Orthotic prescription principles in CP OR Physical therapy goals in different stages of CP OR Occupational therapy interventions for upper limb function in CP OR Speech therapy for dysphagia related to postural issues in CP OR Social work support for families of children with CP undergoing orthopaedic treatment OR Psychological support for children with CP facing orthopaedic surgery OR Nutritional optimization before and after orthopaedic surgery in CP OR Bone mineral density in cerebral palsy and fracture risk OR Vitamin D deficiency in children with cerebral palsy OR Pathogenesis of contractures in cerebral palsy OR Molecular mechanisms of spasticity in cerebral palsy OR Genetic syndromes that can mimic cerebral palsy with orthopaedic features OR Differential diagnosis of early motor delay OR Developmental milestones and their relevance to CP diagnosis OR Role of MRI brain in predicting orthopaedic outcomes in CP OR Electrodiagnostic studies in CP (EMG, nerve conduction) OR Pharmacological management of spasticity in CP (oral medications) OR Intrathecal baclofen therapy for severe spasticity in CP OR Botulinum toxin A injections for focal spasticity in CP: mechanism and technique OR Phenol neurolysis for spasticity in CP OR Orthopaedic complications of spasticity medications OR Surgical management of spasticity (e.g., neurectomy, myelotomy) OR Multidisciplinary spasticity clinic model OR Spasticity assessment scales (e.g., Modified Ashworth Scale, Tardieu Scale) OR Range of motion assessment in CP OR Muscle strength testing in CP (challenges and modifications) OR Observational gait analysis in CP OR 3D gait analysis in CP: parameters and interpretation OR Energy expenditure during gait in CP OR Classification of hip displacement in CP (e.g., Reimers' Migration Percentage) OR Radiographic evaluation of the spine in CP (Cobb angle) OR Foot posture assessment in CP (e.g., Foot Posture Index) OR Upper extremity functional assessment in CP (e.g., QUEST, AHA) OR Patient-reported outcome measures for function and quality of life in CP OR Goal setting in CP rehabilitation (e.g., GAS - Goal Attainment Scaling) OR Principles of neurorehabilitation in CP OR Constraint-induced movement therapy (CIMT) for upper limb in CP OR Bimanual therapy for upper limb in CP OR Hippotherapy and therapeutic riding for CP OR Aquatic therapy for CP OR Strength training programs for children with CP OR Stretching and positioning programs for contracture prevention in CP OR Serial casting for contracture management in CP OR Orthotics for lower limb in CP (AFOs, KAFOs, SMOs) OR Orthotics for upper limb in CP (splints, braces) OR Wheelchair prescription and seating considerations in CP OR Adaptive equipment for activities of daily living in CP OR Augmentative and alternative communication (AAC) for children with CP OR Management of drooling in CP and its postural implications OR Feeding difficulties and nutritional support in CP OR Dental care in children with CP OR Sleep problems in children with CP and orthopaedic contributions OR Pain assessment and management in non-verbal children with CP OR Mental health issues in children with CP and their families OR Transition to adulthood for individuals with CP: orthopaedic and functional aspects OR Employment and independent living for adults with CP OR Sports and recreation for individuals with CP: orthopaedic considerations OR Advocacy and support groups for cerebral palsy OR Ethical dilemmas in the care of children with severe CP OR Research in cerebral palsy: current trends and future directions OR Global burden of cerebral palsy and access to orthopaedic care OR Cerebral palsy registries and their role in research and care improvement OR Telehealth in the management of cerebral palsy OR Assistive technologies and robotics in cerebral palsy rehabilitation OR Gene therapy and stem cell therapy for cerebral palsy: current status OR Prevention of cerebral palsy: antenatal and perinatal strategies OR Early diagnosis and intervention in cerebral palsy OR Neuroimaging findings in different types of cerebral palsy OR Classification of cerebral palsy (motor type, topography, GMFCS) OR Etiology and risk factors for cerebral palsy OR Pathophysiology of brain injury in cerebral palsy OR Epidemiology of cerebral palsy OR Definition of cerebral palsy OR History of understanding and treating cerebral palsy OR Windswept deformity X-ray CP OR Scoliosis X-ray CP GMFCS V OR Crouch gait CP photo OR Equinus foot CP photo OR Spastic hip dislocation CP radiograph OR Femoral anteversion clinical picture CP OR Tibial torsion clinical assessment CP OR Planovalgus foot CP X-ray OR GMFCS levels visual guide OR Orthopaedic manifestations CP summary diagram)
Gait Parade - Wobbly Walks
- Gait Analysis: Key for diagnosis, prognosis, guiding interventions (orthotics, surgery, therapy). OGA standard; 3D IGA for complex cases.
- Common Patterns:
- Spastic Diplegia:
- Scissoring: Hip adduction/internal rotation.
- Equinus: Toe-walking due to calf spasticity.
- Crouch Gait: ↑ hip/knee flexion, ankle dorsiflexion. From hamstring/psoas spasticity, weak extensors.
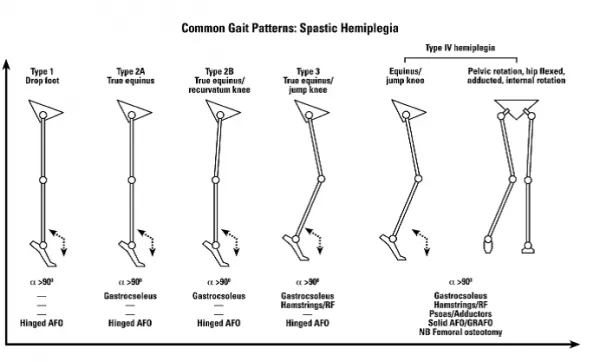
- Spastic Hemiplegia:
- Circumduction: Stiff leg swings outward.
- Equinovarus/Equinovalgus foot.
- Ataxic CP: Wide-based, unsteady, staggering.
- Dyskinetic CP: Variable, involuntary movements.
- Spastic Diplegia:
⭐ Equinus is the most common deformity in spastic CP, often addressed by Achilles tendon lengthening.
 oka
oka
Joint Hit List - Problem Hotspots
- Hip (Most Critical):
- Progressive subluxation/dislocation, common in spastic quadriplegia/diplegia.
- Key contractures: Adduction, flexion, internal rotation.
- Associated: Coxa valga, increased femoral anteversion.
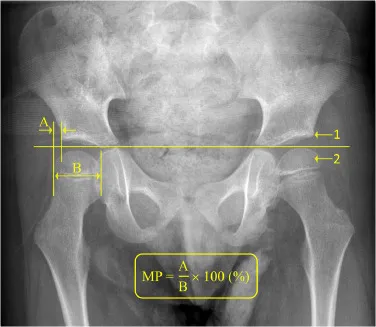
⭐ Reimer's Migration Percentage (MP) > 30% signals hip instability; >40% often warrants surgical intervention.
- Knee:
- Flexion deformity (hamstring spasticity) → crouch gait.
- Patella alta is common. Genu valgum may occur.
- Foot & Ankle:
- Equinus (most frequent; gastrocnemius/soleus spasticity).
- Equinovarus (spastic tibialis posterior).
- Equinovalgus (peroneal spasticity, tight Achilles tendon).
- Spine:
- Neuromuscular scoliosis: Often progressive, long C-shaped curves, with pelvic obliquity.
- Increased kyphosis or lumbar lordosis.
- Upper Limb:
- Shoulder: Adduction, internal rotation. Elbow: Flexion. Forearm: Pronation. Wrist/Fingers: Flexion, thumb-in-palm.
Fix-It Strategies - Untangling Limbs
- Goals: Maximize function, improve gait, correct deformities, manage pain.
- Approach: Multidisciplinary team; individualized treatment plan.
Non-Operative Management:
- Physiotherapy: Essential for stretching, strengthening, gait training.
- Orthotics: Ankle-Foot Orthoses (AFOs) for equinus; splints.
- Medications:
- Botulinum Toxin A: For dynamic spasticity (e.g., calf, adductors); effect lasts 3-6 months.
- Baclofen (Oral/Intrathecal pump): For generalized spasticity.
Operative Management:
- Key Procedures: Tendon lengthening (Achilles, hamstrings), osteotomies (femoral, pelvic), SDR.
⭐ SEMLS addresses multiple deformities in one session, reducing anesthesia exposure & rehab time.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Cerebral Palsy (CP) is the most common childhood motor disability.
- Spasticity is the predominant motor disorder; spastic diplegia is the most frequent type.
- Hip displacement (subluxation/dislocation) is a major concern, especially in non-ambulatory patients.
- Common gait issues include equinus deformity and crouch gait; managed with Botox, orthoses, or tendon lengthening.
- Scoliosis is prevalent, particularly in quadriplegic CP.
- Management involves a multidisciplinary team; GMFCS classifies motor function_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

