Forces, Stress & Strain - Biomechanics Basics Blitz
- Force (F): Push/pull causing acceleration/deformation. Types: Compressive, Tensile, Shear, Torsional, Bending.
- Stress ($\sigma$): Force per unit area. $\sigma = F/A$. Unit: Pascals (Pa).
- Strain ($\epsilon$): Relative deformation due to stress. $\epsilon = \Delta L/L_0$. Dimensionless.
- Stress-Strain Relationship:
- Elastic Modulus (Young's Modulus, E): Material stiffness. $E = \sigma / \epsilon$ in elastic region.
- Yield Strength: Stress at elastic limit, onset of plastic deformation.
- Ultimate Tensile Strength (UTS): Max stress material withstands before necking/failure.
- Fracture Point: Point where material breaks.
- Material Behaviour:
- Ductile: Undergoes significant plastic deformation before fracture.
- Brittle: Fractures with little or no plastic deformation. 
⭐ Cortical bone is anisotropic. Compressive strength \approx 170-200 MPa; tensile strength \approx 100-130 MPa. Strongest under compression.
Bone & Soft Tissue Properties - Tissue Toughness Trials
- Toughness: Material's ability to absorb energy and plastically deform before fracturing.
- Calculated as the total area under the stress-strain curve.
- Units: Energy per unit volume, e.g., $J/m^3$.
- Factors Influencing Toughness:
- Loading Rate: Viscoelastic tissues show rate-dependent toughness.
- Temperature: Lower temperatures can induce brittleness.
- Microstructure: Collagen quality/orientation, mineral density (bone), porosity.
- Notches/Defects: Act as stress concentrators, reducing toughness.
- Common Toughness Tests:
- Impact Tests (e.g., Charpy, Izod): Measure energy absorbed during sudden impact leading to fracture.
- Fracture Toughness ($K_{IC}$): Quantifies resistance to propagation of a pre-existing crack.
- Clinical Significance:
- Bone: Decreases with age, osteoporosis. Cortical bone generally tougher.
- Soft Tissues (tendons, ligaments): Dependent on collagen network integrity.

⭐ Bone's remarkable toughness arises from its hierarchical composite structure, involving mechanisms like crack deflection and microcracking at different length scales, which dissipate energy.
Joint Kinematics & Kinetics - Motion Mechanics Medley
- Kinematics: Motion description.
- Osteokinematics: Bone movement (flexion, abduction) in planes (sagittal, frontal, transverse).
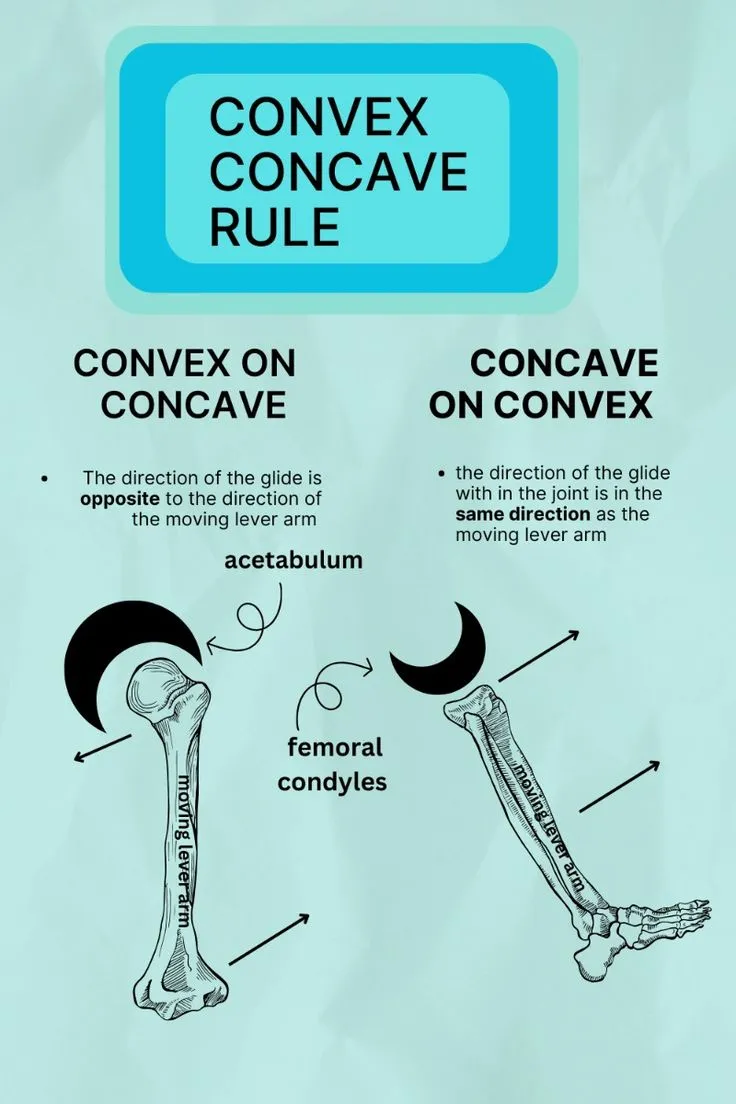
- Arthrokinematics: Joint surface motion: roll, slide, spin.
- 📌 Convex-Concave Rule: Convex on concave: roll opposite slide. Concave on convex: roll same as slide.
- Degrees of Freedom (DOF): Independent rotations.
- Kinetics: Forces causing motion.
- Forces: Internal (muscle), External (gravity).
- Levers:
- Class 1: Fulcrum central (triceps).
- Class 2: Load central (calf raise).
- Class 3: Effort central (biceps) - most common.
- Torque: $T = F \times d$. Rotational force.
- Joint Reaction Force (JRF): Inter-articular force.
- Pressure: $P = F/A$.
⭐ Most body levers are Class 3: ↑speed/ROM, ↓force.
Implant Biomechanics & Fixation - Fixation & Fusion Facts
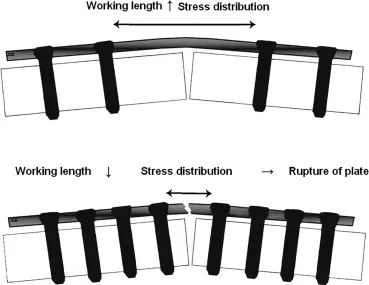
- Implant Stiffness & Load:
- Stress Shielding: ↑ Implant stiffness (e.g., Co-Cr > SS > Ti) → ↓ bone load → bone resorption.
- Load Sharing: Desirable; implant & bone share stress, promotes healing. Titanium alloys (lower Young's Modulus) better.
- Fixation Stability Types:
- Absolute Stability: No motion (e.g., compression plating). Primary bone healing (no callus).
- Relative Stability: Micromotion (e.g., IM nails, ex-fix, bridge plates). Secondary bone healing (callus).
- Screws & Plates:
- Screws: Cortical (dense bone, smaller pitch), Cancellous (spongy bone, larger pitch).
- Locking Plates (LCP): Angular stability.
⭐ LCPs act as "internal-external fixators," crucial for osteoporotic or comminuted fractures due to angular stability.
- Arthrodesis (Fusion):
- Goal: Bony union across a joint.
- Requires: Decortication, bone graft (autograft = gold standard), stable fixation, compression.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Stress (Force/Area) causes Strain (deformation); Young's Modulus measures material stiffness.
- Bone is anisotropic (properties vary with load direction) and viscoelastic (stress-strain behavior is time-dependent).
- Wolff's Law: Bone remodels in response to mechanical stresses; disuse leads to atrophy.
- The load-deformation curve illustrates elastic limit, yield point, plastic deformation, and ultimate failure point.
- Key forces on bone: Tension, compression, shear, torsion, and bending.
- Stress shielding occurs when an implant bears most of the load, leading to bone resorption around it.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

