Biomechanics of Fracture Fixation - Bone's Big Rules
- Key concepts:
- Stress ($F/A$): Force/area.
- Strain ($\Delta L/L$): Relative deformation.
- Young's Modulus ($E = Stress/Strain$): Stiffness.
- Bone properties:
- Anisotropic: Direction-dependent properties.
- Viscoelastic: Rate-dependent response (stronger if rapid).
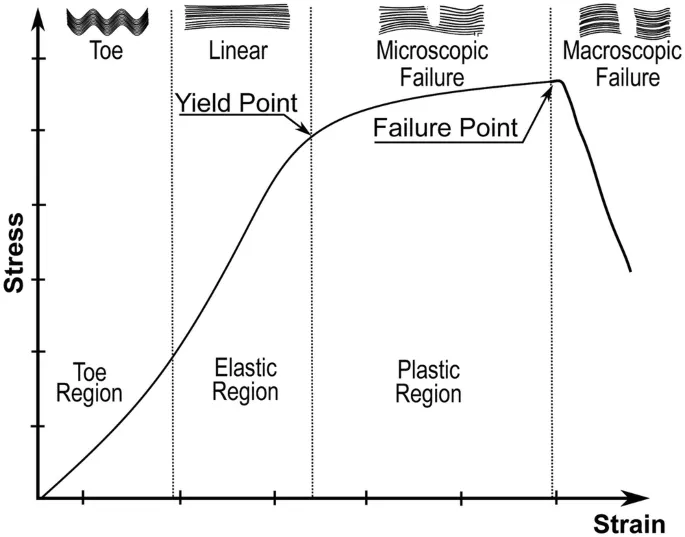
- Stress-Strain Curve:
- Elastic deformation: Reversible.
- Yield Point: Elastic limit, onset of plastic change.
- Plastic deformation: Permanent.
- Ultimate Failure Point: Fracture.
- Bone types:
- Cortical: Dense, high stress resistance, low strain capacity.
- Cancellous: Spongy, lower stress resistance, high strain capacity.
⭐ Wolff's Law states that bone remodels in response to mechanical stress.
Biomechanics of Fracture Fixation - Stability Secrets
⭐ Perren's Strain Theory: Fracture healing is inversely proportional to interfragmentary strain.
- Stability Goal: Create optimal mechanical environment for bone union.
- Absolute Stability:
- No motion at fracture site; aims for primary bone healing.
- Requires anatomical reduction and interfragmentary compression.
- Interfragmentary strain < 2%.
- Examples: Lag screws, compression plates.
- Relative Stability:
- Allows controlled motion; promotes secondary bone healing via callus.
- Maintains alignment, length, and rotation.
- Interfragmentary strain 2-10%.
- Examples: Intramedullary nails, bridge plates, external fixators.

Biomechanics of Fracture Fixation - Hardware Heroes
📌 Screws Squeeze, Plates Protect, Nails Navigate, ExFix Externalize.

Implants achieve fixation by applying biomechanical principles:
- Screws: Convert rotational force (torque) into axial force (compression).
- Lag Screw: Compresses fragments; near cortex overdrilled, far cortex tapped.
- Pitch: Thread distance; ↑pitch for cancellous bone. Core diameter dictates strength.
| Implant | Mechanism Highlights | Stability Type | Load Transfer | Key Advantage |
|---|---|---|---|---|
| Screws | Interfragmentary Compression (Lag) | Absolute | Sharing | Direct compression |
| Plates (Conv.) | Compression (DCP), Bridging, Neutralization | Absolute/Relative | Bearing/Sharing | Versatile, anatomical reduction |
| Plates (Locking) | Fixed-angle construct, Bridging | Absolute (Angular) | Bearing | Good in osteoporotic bone, preserves periosteum |
| IM Nails | Intramedullary Splinting | Relative | Sharing | Central, less soft tissue stripping |
| Ex-Fix | External Bridging, Neutralization, Compression/Distraction | Relative | Bearing (Frame) | Minimally invasive, for open #, adjustable |
Biomechanics of Fracture Fixation - Fixation's Fate
- Bone Healing & Stability:
- Primary (Direct) Healing: Requires absolute stability (e.g., compression plates).
- Contact Healing: No gap, direct osteonal bridging.
- Gap Healing: Gaps <1mm filled by lamellar bone. Minimal callus.
- Secondary (Indirect) Healing: Requires relative stability (e.g., IM nails, casts, ex-fix).
- Forms robust callus via endochondral & intramembranous ossification. More physiological.
- Primary (Direct) Healing: Requires absolute stability (e.g., compression plates).
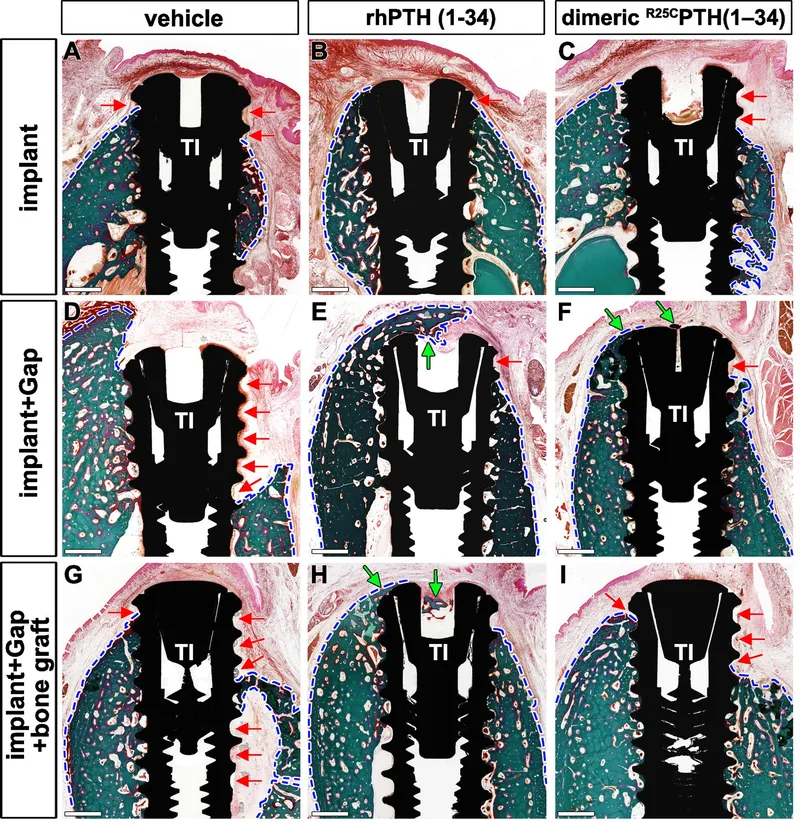 vs. secondary bone healing (callus))
vs. secondary bone healing (callus))
- Complications & Failure Pathways:
- Implant Failure:
- Fatigue: Cyclic loading leads to material failure.
- Overload: Single high-energy event exceeds implant strength.
- Non-Union: Often precedes/causes implant failure. Key factors:
- Excessive motion at fracture site (inhibits vascularization, disrupts callus).
- Poor vascularity/blood supply (ischemia).
- Infection.
- Large fracture gap.
- Implant Failure:
⭐ Stress shielding beneath a rigid plate can lead to cortical osteopenia and refracture upon implant removal.
High-Yield Points - ⚡ Biggest Takeaways
- Stress shielding from overly rigid plates causes osteopenia under the plate.
- DCPs convert torsional/bending forces to axial compression for primary healing.
- Locking plates offer fixed-angle stability, vital for osteoporotic/comminuted fractures.
- IM nails, as internal splints, share load, ideal for diaphyseal fractures.
- Relative stability (nails, ex-fix) promotes secondary healing (callus); absolute stability (plates) for primary healing.
- Shorter implant working length equals increased stiffness and reduced motion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

