Suture Techniques in Orthopaedics - Thread Essentials
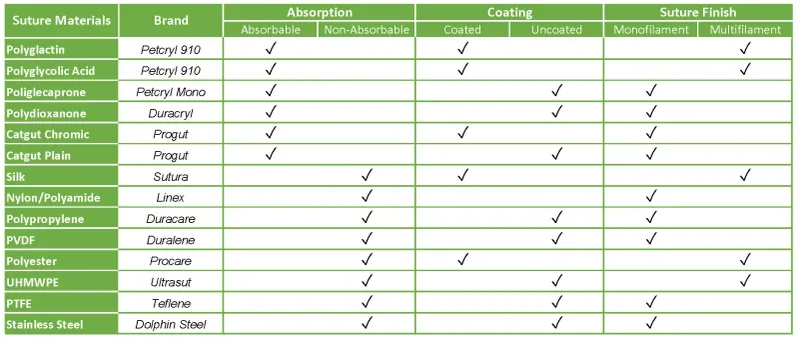
- Types:
- Absorbable: Degrade over time.
- Natural: Catgut (plain, chromic) - high tissue reactivity.
- Synthetic: PGA (Dexon), Polyglactin 910 (Vicryl), PDS II, Monocryl - lower reactivity.
- Non-Absorbable: Permanent.
- Natural: Silk - braided, high tissue reactivity.
- Synthetic: Nylon (Ethilon), Polypropylene (Prolene), Polyester (Ethibond), Steel.
- Absorbable: Degrade over time.
- Properties:
- Tensile Strength: Resists breakage.
- Knot Security: Holds knots.
- Tissue Reactivity: Inflammatory response.
- Memory: Returns to original shape.
- Capillarity: Wick effect (fluid absorption).
- Sizing (USP): More zeros (e.g., 5-0) = smaller diameter.
⭐ Prolene (Polypropylene) is preferred for tendon repairs requiring high tensile strength and minimal tissue reaction.
Suture Techniques in Orthopaedics - Point & Tie Perfection
- Suture Materials:
- Types: Absorbable (Vicryl, PDS); Non-absorbable (Prolene, Ethibond).
- Structure: Monofilament (↓ drag, ↓ infection) vs. Multifilament (↑ handling, ↑ knot security, ↑ infection risk).
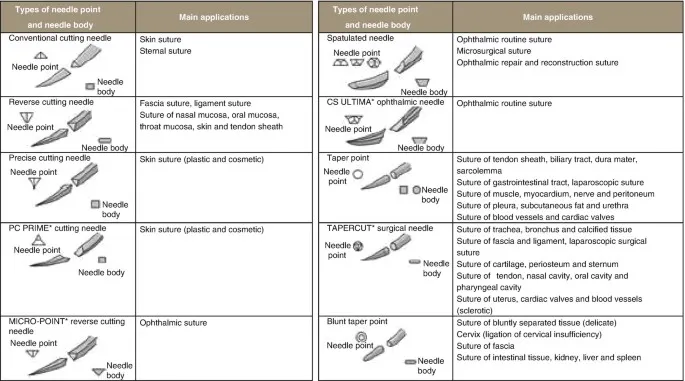
- Orthopaedic Needles:
- Common: Taper-point (muscle, fascia), Reverse Cutting (tendon, ligament; ↓ pull-through), Conventional Cutting (skin).
- Size denoted by number (larger number = smaller needle).
- Knot Tying:
- Square Knot: Foundation; min 3-4 throws for security.
- Surgeon’s Knot: Double first throw for ↑ friction under tension.
⭐ In tendon repair, locking sutures (e.g., Krackow, Kessler) or multi-strand techniques significantly enhance repair strength and reduce gapping.
Suture Techniques in Orthopaedics - Stitching Strong Repairs
- Principles: Asepsis, atraumatic handling, good apposition, secure knots, preserve vascularity.
- Suture Materials:
- Absorbable: Vicryl, PDS (long-term), Monocryl (short-term).
- Non-absorbable: Prolene, Ethibond, FiberWire (high strength).
- Needle Types: Taper (fascia), Reverse Cutting (skin, tough tissue).
- Knot Security: Square/Surgeon's knot. Min. 3-4 throws (monofilament), 2-3 (braided).
- Common Techniques:
- Skin: Simple interrupted, Vertical/Horizontal mattress, Subcuticular.
- Tendon: Kessler, Bunnell, Krackow (locking loop).
- Meniscus: All-inside, Inside-out, Outside-in.
⭐ The Krackow stitch, a locking loop technique, offers superior strength for tendon-to-bone or ligament-to-bone repairs, crucial in ACL reconstruction.
Suture Techniques in Orthopaedics - Complications & Pro Tips
- Common Complications:
- Infection (stitch abscess, SSI)
- Wound dehiscence, edge necrosis
- Suture sinus or granuloma
- Allergic reaction to suture material
- Iatrogenic neurovascular injury
- Hypertrophic scarring or keloid
- Suture extrusion ("spitting")
- Hematoma/Seroma formation
- Pro-Tips for Success:
- Meticulous aseptic technique.
- Suture Selection: Match material (absorbable/non-absorbable, mono/braided) and size to tissue.
- Knot Tying: Secure square knots, avoid excessive tension. "Approximate, don't strangulate."
- Technique: Evert skin edges. Minimize tension (undermine if needed).
- Gentle tissue handling prevents ischemia.
- Cosmesis: Use subcuticular sutures for aesthetic results.
- Removal: Timely, site-specific (face 3-5d, limbs 10-14d, joints 14d).
⭐ Monofilament sutures (e.g., Prolene, PDS) are preferred over multifilament (e.g., Silk, Vicryl) in contaminated wounds due to lower infection risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Knot security is paramount; surgeon's knot ensures reliability, while sliding knots (e.g., Duncan loop) are key in arthroscopy.
- Use absorbable sutures (e.g., Vicryl, PDS) for deep tissues and non-absorbable (e.g., Ethibond, FiberWire) for tendons, ligaments, or skin needing prolonged strength.
- Monofilament sutures (e.g., PDS, Prolene) generally cause less tissue reaction and have ↓ infection risk compared to multifilament (e.g., Vicryl, Ethibond).
- Common tendon repair techniques include Kessler, Bunnell, and modified Kessler; locking sutures like Krackow provide ↑ repair strength.
- Suture anchors are indispensable for secure reattachment of soft tissues (ligaments, tendons) to bone.
- Needle selection is critical: tapered needles for delicate tissues, cutting needles (conventional or reverse) for tougher structures like skin or fibrocartilage.
- Tensile strength, knot holding capacity, and tissue reactivity are primary factors guiding suture material choice for optimal healing outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

