AO Principles & Goals - Fixation Foundation
- Core Aim: Achieve prompt, full function of injured limb.
- AO Principles (📌 ARS M): Foundation for internal fixation.
⭐ The four AO principles are:
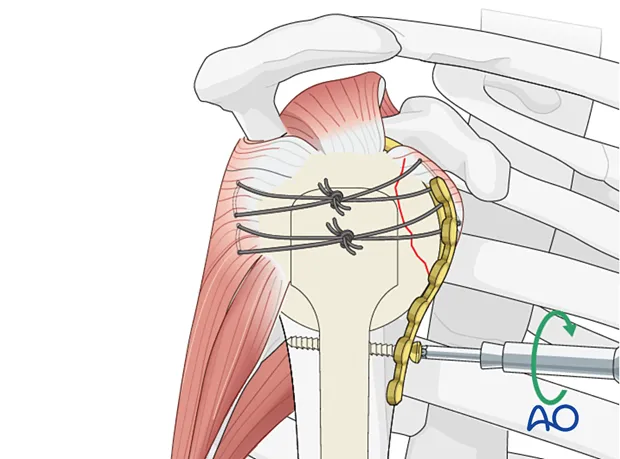
- Anatomic reduction of fracture fragments, particularly in articular fractures.
- Stable internal fixation appropriate to the fracture pattern and biology.
- Preservation of blood supply to soft tissues and bone by careful handling and atraumatic surgical technique.
- Early, active, pain-free Mobilization of muscles and joints adjacent to the fracture, preventing fracture disease.
- Goals (derived from principles):
- Anatomical restoration.
- Stable healing environment.
- Vascularity preservation.
- Rapid functional recovery.
 oka
oka
Implant Types - Hardware Heroes
Materials: Stainless steel, titanium alloys (strength, biocompatibility).
Screws:
| Type | Feature | Sizes (mm) |
|---|---|---|
| Cortical | Fine threads, dense bone | 2.7, 3.5, 4.5 |
| Cancellous | Coarse threads, spongy bone | 4.0, 6.5 |
| Locking | Threaded head locks to plate (fixed-angle) | System-specific |
| Cannulated | Hollow for guidewire, precise placement | Varies |
| Lag (Technique) | Threads far cortex only → compression | Any screw |
| Type/Function | Description | |
| ------------------ | ----------------------------------------------------------------- | |
| Compression | Compresses fracture (DCP: eccentric holes) | |
| Neutralization | Protects lag screws from torsion/bending | |
| Buttress | Supports articular fragments, resists axial load | |
| Bridging | Spans comminution, maintains length/alignment | |
| Locking (LCP) | Angular stability (internal fixator), for poor bone quality | Other Implants: |
- K-wires: 0.6-3.0mm; fixation, guides.
- IM Nails: Load-sharing; long bone diaphyseal #.
- Cerclage Wires: Encircle fragments.

⭐ A lag screw, whether a cortical or cancellous screw, achieves interfragmentary compression when its threads engage only the far fragment, pulling it towards the near fragment where the screw shank glides.
Biomechanics & Stability - Balancing Act
- Strain & Healing: Bone healing depends on strain at fracture site.
- < 2% strain: Primary healing (direct osteonal).
- 2-10% strain: Secondary healing (callus).
-
10% strain: Non-union.
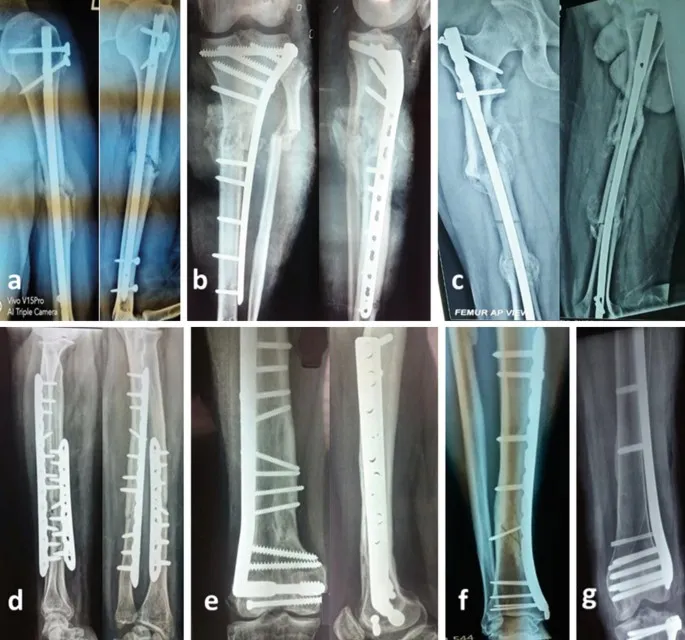
| Feature | Absolute Stability | Relative Stability |
|---|---|---|
| Goal | Rigid fixation, anatomical reduction | Alignment, controlled micromotion |
| Fracture Gap | < 1 mm | > 1 mm / comminuted |
| Methods | Lag screws, Compression plates | IM nails, Bridge plates, Ex-fix, Casts |
| Indications | Simple intra-articular/diaphyseal fx | Comminuted fx, Long diaphyseal/metaphyseal fx |
| Healing | Primary (direct) | Secondary (callus) |
| Callus | Minimal/None | Abundant |
Complications & Considerations - Pitfall Patrol
- Infection: Superficial/deep; prompt antibiotics, possible debridement.
- Implant Failure: Breakage, loosening, migration; revision surgery often needed.
- Union Problems: Non-union, malunion, delayed union impacting function.
- Neurovascular Injury: Iatrogenic risk; meticulous surgical technique crucial.
- Compartment Syndrome: ⚠️ Acute; high risk tibia/forearm; urgent fasciotomy.
- Hardware Irritation: Pain/bursitis over implant; removal post-union if symptomatic.
- Refracture: Post-removal (stress protection) or peri-implant.
- Thromboembolism (DVT/PE): Prophylaxis vital in high-risk patients.
⭐ Stress shielding occurs when a very rigid implant bears most of the physiological load, leading to bone resorption (osteopenia) beneath the plate and increasing the risk of refracture after implant removal.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- AO Principles: Anatomic reduction, stable fixation, preserve blood supply, early mobilization.
- Absolute stability (articular fractures) for primary bone healing (no callus); relative stability (diaphyseal) for secondary healing (callus).
- Lag screw: Provides interfragmentary compression; threads engage far cortex only.
- Plate functions: Compression, neutralization, buttress, tension band, bridging.
- Stress shielding: Rigid fixation may cause osteopenia under the plate.
- Biological fixation: Emphasizes minimal soft tissue stripping to preserve blood supply.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

