Principles of Plate Osteosynthesis - Metal Meets Bone
- Plate Osteosynthesis: Surgical fracture fixation with plates/screws for anatomical restoration.
- AO Principles:
- Anatomic reduction: Precise fragment realignment.
- Stable fixation: Absolute or relative.
- Blood supply preservation: Minimize soft tissue trauma.
- Early mobilization: Safe, active movement.
- 📌 Mnemonic: ASBE (Absolute Stability, Blood supply, Early mobilization).
- Constructs:
- Load-sharing: Plate & bone share load.
- Load-bearing: Plate bears entire load.
- Healing:
- Primary: Absolute stability, no callus.
- Secondary: Relative stability, callus.

⭐ Absolute stability (rigid plate) → primary bone healing (minimal callus). Relative stability (bridging plate) → secondary bone healing (callus).
Types & Functions of Plates - The Right Fit
-
Plate Types:
- DCP (Dynamic Compression Plate): Oval holes → compression.
- LC-DCP (Limited Contact DCP): Undercut, ↓vascular injury.
- LCP (Locking Compression Plate): Locking/non-locking screws; angular stability. Internal fixator.
- Reconstruction: Malleable (pelvis).
- Tubular (1/3, 1/4): Low-stress (fibula).
- Specialty: Anatomical (PHILOS, condylar buttress).
-
Plate Functions: 📌 (CNBBT)
- Compression: Static (prebend)/dynamic (eccentric screw).
- Neutralization: Protects lag screws.
- Buttress: Supports articular fragments (tibial plateau).
- Bridging: Spans comminution; length/alignment.
- Tension Band: Tension → compression.

-
DCP vs. LCP:
Feature DCP LCP Mechanism Friction Angular stability (int. fixator) Screw I/F Plate compresses bone Screws lock to plate Stability Relative (axial) Absolute (angular) Blood ↓ contact ↑ preserved (min. contact) Indication Simple #, good bone Osteoporotic, comminuted periart. #
⭐ LCPs: internal fixators, angular stability independent of plate-bone friction. Ideal for osteoporotic bone & comminuted periarticular #.
Indications & Contraindications - Plating Go/No-Go
Indications (Go):
- Articular Fx (anatomic reduction, abs. stability): e.g., tibial plateau, distal radius.
- Diaphyseal Fx: Forearm (gold standard), humerus, femur, tibia.
- Periarticular Fx, osteotomies, nonunion/malunion.
Contraindications (No-Go):
- Absolute: Active infection, severe soft tissue compromise.
- Relative: Severe osteoporosis, unfit for surgery, high comminution (IMN better), non-compliance.
Open Fractures (Gustilo-Anderson):
- Type I & II → primary plating; Type III → staged.
⭐ Plating of both-bone forearm fractures in adults is the gold standard to restore rotational stability (pronation/supination).

Surgical Technique - Plating Playbook
- Pre-op: Templating, implant selection.
- Approach: Meticulous soft tissue handling (preserve blood supply).
- Reduction: Direct/Indirect. Provisional K-wires.
- Plate: Type/length selection. Contour (DCP vital; LCP less if internal fixator).
- Screws: Lag (interfragmentary compression); DCP (eccentric drilling for compression). Conventional: 3-4 bicortical screws/6-8 cortices per main fragment. LCP: 3 locking screws/fragment. Length: perforate far cortex 1-2mm.
- Intra-op Imaging: Confirm reduction & hardware.
⭐ To achieve compression with a DCP, the screw is inserted into the eccentric portion of the oval hole, away from the fracture line; tightening the screw then draws the bone fragment towards the fracture.

Complications - Plate Pitfalls
- Intraoperative: Neurovascular injury, iatrogenic fracture.
- Early Postop: Infection (superficial/deep), hematoma, wound dehiscence, compartment syndrome.
- Late Postop:
- Implant failure (bending/breakage, screw pull-out/loosening).
- Biological failure (nonunion, malunion, delayed union).
- Refracture (post-plate removal), stress shielding & osteopenia, hardware irritation.
- Prevention: Asepsis, gentle tissue handling, stable fixation.
- Management (Key):
- Infection: Debridement, antibiotics, ?implant removal.
- Nonunion: Bone grafting, revision fixation.
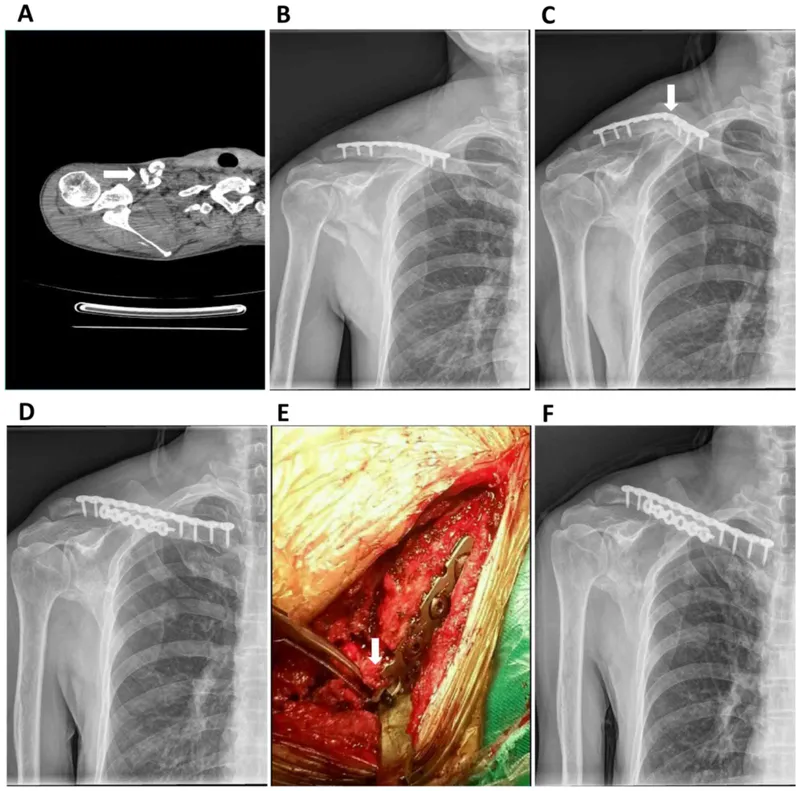
⭐ Stress shielding under a very rigid plate can lead to cortical osteopenia beneath it, ↑ risk of refracture after implant removal if bone hasn't fully remodeled.
High‑Yield Points - ⚡ Biggest Takeaways
- Plate osteosynthesis provides absolute stability, crucial for direct (primary) bone healing.
- Dynamic Compression Plates (DCP) achieve compression via eccentric screw drilling.
- LC-DCP reduces plate-bone contact, better preserving periosteal blood supply.
- Locking plates create a fixed-angle construct, acting as an internal fixator, vital for osteoporotic or comminuted fractures.
- Key indications: articular fractures, forearm fractures, and osteotomies.
- Stress shielding beneath the plate can cause osteopenia and risk of refracture post-removal.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

