MIOS Fundamentals - Tiny Incisions, Big Gains
- Definition: Surgical techniques using small incisions (often < 5 cm), guided by imaging (arthroscopy, fluoroscopy) and specialized instruments.
- Goals: Achieve surgical objectives with ↓ iatrogenic soft tissue trauma, better cosmesis, faster functional recovery.
- Advantages: 📌 SSSLL
- Small scars
- Speedy recovery
- Shorter hospital stay (e.g., < 24-48 hrs)
- Less pain (↓ analgesics)
- Less blood loss (↓ transfusion risk)
- Disadvantages:
- Steep learning curve
- Longer initial operative time
- Higher equipment cost
- ↑ Radiation exposure (fluoroscopy)
- Limited tactile feedback
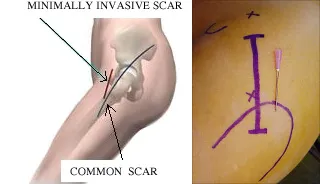
⭐ Reduced iatrogenic soft tissue damage is a primary driver for improved outcomes in MIOS.
MIOS Toolkit - Scopes & Special Gear
- Scopes (Arthroscope/Endoscope): Essential for visualization.
- Common Diameters: 4mm (knee/shoulder), 2.7mm (small joints), 1.9mm (very small joints).
- Components: Lens system, light source (fiberoptic/LED), camera, irrigation/suction channels.
- Viewing Angles: 0°, 30° (most common), 70°.
- Special Instruments:
- Cannulas & Trocars: Portal creation.
- Probes: Tactile feedback, diagnostic.
- Graspers, Punches, Scissors: Specialized, fine-tipped.
- Shavers & Burrs: Motorized, for tissue/bone resection.
- Electrocautery/Ablation: Hemostasis, tissue modification.
- Support Systems:
- Fluid Management: Joint distension, clear view (e.g., saline).
- Video Tower: Monitor, light source, camera unit, recorder.
⭐ Triangulation is the fundamental skill for arthroscopic surgery, allowing instrument manipulation and visualization through separate portals.
oka
MIOS Showcase - Keyhole Ops
Minimally Invasive Orthopaedic Surgery (MIOS) revolutionizes procedures by using small incisions, specialized instruments, and often, camera guidance (arthroscopy/endoscopy). This approach minimizes soft tissue trauma, leading to faster recovery and reduced pain.
- Core Principles: Small portals, specialized long-shafted instruments, advanced imaging (fluoroscopy, arthroscopy).
- General Advantages: ↓ Blood loss, ↓ Post-op pain, ↓ Hospital stay, ↑ Cosmesis, Earlier return to activity.

| Area | Common Procedures | Key MIOS Benefit |
|---|---|---|
| Knee | Arthroscopic Meniscectomy, ACL/PCL Reconstruction, Synovectomy | Rapid functional recovery |
| Shoulder | Rotator Cuff Repair, Bankart Repair, Subacromial Decompression | Improved post-op motion, less pain |
| Hip | Arthroscopic Labral Repair, FAI Correction | Preservation of hip joint |
| Spine | Microdiscectomy, Minimally Invasive TLIF/PLIF | Reduced muscle stripping, less pain |
| Trauma | Intramedullary Nailing, MIPO (Minimally Invasive Plate Osteosynthesis) | Biological fixation, faster union |
- Limitations: Steep learning curve, specialized equipment, potential for neurovascular injury if not meticulous, longer operative times initially.
- Contraindications: Severe deformity, extensive scarring, certain infections, inadequate visualization.
MIOS Hurdles - Dodging Dangers
- Potential Complications:
- Neurovascular injury: Portal creation/instrument passage risk.
- Infection: Port site (superficial) or deep.
- Compartment syndrome: Arthroscopic fluid extravasation.
- Instrument breakage/malfunction.
- Radiation exposure: Increased fluoroscopy use.
- Learning curve: Longer initial operative times, ↑conversion risk.
- Dodging Dangers (Prevention):
- Master anatomy; precise, safe portal placement.
- Meticulous soft tissue handling; minimize trauma.
- Controlled fluid management; monitor inflow/outflow.
- ALARA principle for radiation.
- Systematic training, proctorship.
⭐ Portal-related complications, though infrequent, include nerve damage, infection, and persistent drainage.
High‑Yield Points - ⚡ Biggest Takeaways
- MIOS prioritizes reduced surgical trauma via smaller incisions, leading to faster recovery.
- Benefits include less pain, ↓ blood loss, shorter hospital stays, and improved cosmesis.
- Core techniques: arthroscopy (joints), percutaneous fixation (fractures), endoscopy (spine).
- Robotic assistance enhances precision in procedures like joint replacements.
- Despite benefits, MIOS involves a steep learning curve and requires specialized tools.
- Reduced infection rates are a significant advantage over traditional open surgeries.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

