Local Flaps and Soft Tissue Coverage: Principles - Skin Deep Savvy
- Local Flaps: Relocate skin & subcutaneous tissue with its native blood supply to an adjacent defect. Primary goal: "Replace like with like" for optimal function & aesthetics.
- Key Principles:
- Assess Defect: Size, depth, location, surrounding tissue quality.
- Blood Supply: Crucial. Random pattern (dermal/subdermal plexus) vs. Axial pattern (known artery). 📌 Remember: Axial flaps are more robust.
- Planning: Plan in reverse. Ensure tension-free closure. Minimize dog-ears.
- Donor Site: Consider morbidity and closure options.
- Reconstructive Ladder/Elevator: A hierarchical approach to soft tissue reconstruction.
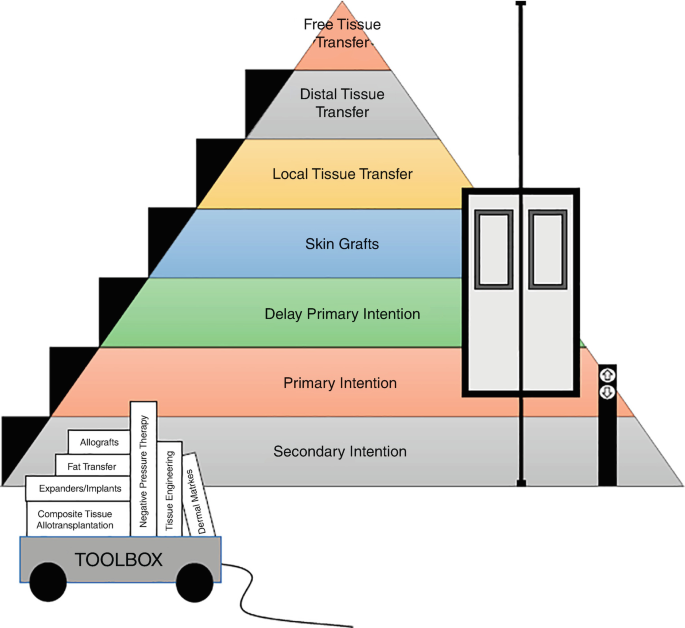
⭐ The Reconstructive Ladder advocates for using the simplest, most reliable method first, progressing to more complex options only as needed.
Local Flaps and Soft Tissue Coverage: Classification - Sorting Skins
Flaps are classified by blood supply, composition, and transfer method, guiding selection for defect coverage.

Classification of Flaps:
| Basis | Types & Key Features |
|---|---|
| Blood Supply | |
| Random Pattern: No specific vessel; dermal-subdermal plexus. Length:width ratio critical (≤ 2:1). | |
| Axial Pattern: Named artery & vein. Greater survival. E.g., Groin flap. | |
| Fasciocutaneous: Includes deep fascia; robust fascial plexus supply. | |
| Musculocutaneous: Muscle carries blood to skin. | |
| Composition | |
| Cutaneous: Skin, subcutaneous tissue. | |
| Fasciocutaneous: Skin, subcutaneous tissue, fascia. | |
| Myocutaneous/Musculocutaneous: Skin, subcutaneous tissue, muscle. | |
| Osteocutaneous: Includes bone with soft tissue. | |
| Specialized: E.g., tendocutaneous, neurocutaneous. |
Local Flaps and Soft Tissue Coverage: Common Types - Surgical Showpieces
- Advancement Flaps:
- Slide directly forward; rely on tissue elasticity.
- Types: Single pedicle, bipedicle, V-Y plasty.
- Use: Small defects, good skin laxity.

- Rotation Flaps:
- Semicircular flap pivots around a point into an adjacent defect.
- Use: Triangular/wedge-shaped defects (e.g., scalp, cheek).

- Transposition Flaps:
- Rectangular/square flap lifted over intervening skin into a nearby defect.
- Pedicle at one end.
- Examples:
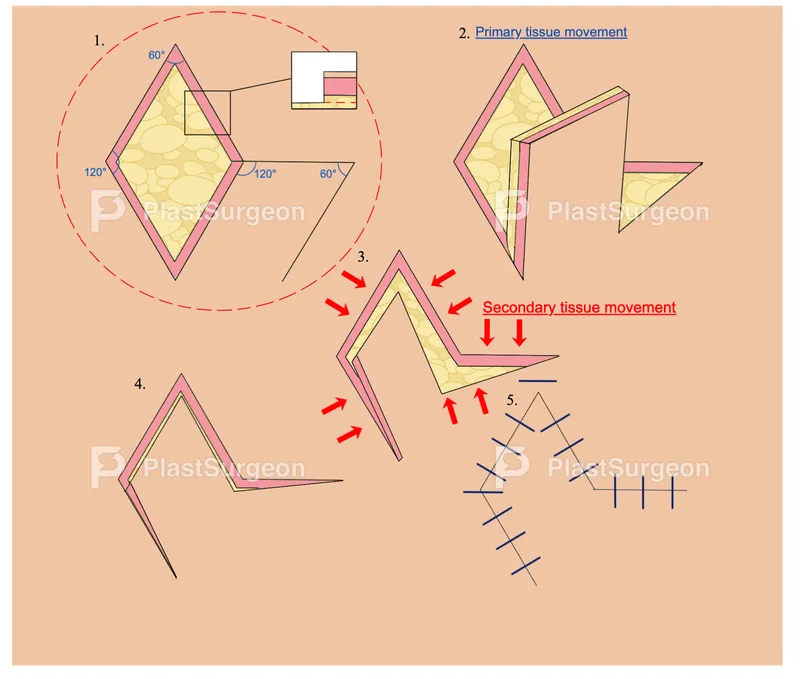
- Z-Plasty: Interposes two triangular flaps. Used for scar contracture release, realigning scars.
- Rhomboid (Limberg) Flap: For 60°/120° rhombic defects.
- Bilobed Flap: Two lobes from a common pedicle.
- Z-Plasty: Interposes two triangular flaps. Used for scar contracture release, realigning scars.
⭐ A Z-plasty with 60° angles theoretically increases length along the central limb by 75%. Angles of 30°, 45°, 60°, and 90° give 25%, 50%, 75%, and 100% theoretical gain, respectively.
Local Flaps and Soft Tissue Coverage: Complications - Trouble Tidings
- Early Complications:
- Hematoma/Seroma: Collection of blood/serum under flap.
- Flap Necrosis: Due to ischemia (venous > arterial).
- Signs: Dusky discoloration, ↓ capillary refill, coolness.
- Infection: Local or systemic signs.
- Late Complications:
- Flap Contracture: Scarring leading to reduced mobility.
- Wound Dehiscence: Separation of wound edges.
- Hypertrophic Scarring/Keloid Formation.
- Altered Sensation: Numbness or hypersensitivity.
⭐ Most common cause of flap failure is venous congestion/thrombosis, not arterial insufficiency.
High‑Yield Points - ⚡ Biggest Takeaways
- Reconstructive ladder: Guides soft tissue coverage choices, from simple closure to free flaps.
- Random pattern flaps: Blood supply from subdermal plexus, limited length-to-width ratio (e.g., 1.5:1).
- Axial pattern flaps: Incorporate a direct cutaneous artery; more reliable with greater length (e.g., groin flap).
- Fasciocutaneous flaps: Include skin, subcutaneous tissue, and deep fascia; robust blood supply.
- Muscle/musculocutaneous flaps: Provide bulk, good vascularity, and help control infection (e.g., latissimus dorsi).
- Propeller flaps: Perforator-based island flaps that rotate around the perforator for versatile coverage.
- Keystone flap: Perforator-based island flap, excellent for defects with moderate skin laxity nearby.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more