Bone Grafting Techniques - Grafting Goals
-
Primary Aims:
- Promote bone healing & fusion (arthrodesis).
- Fill bone defects (trauma, tumor, infection).
- Provide structural support.
- Induce bone formation where absent.
-
Achieved via Key Graft Properties:
- Osteogenesis: Living cells form new bone.
- Osteoinduction: Growth factors recruit & stimulate host cells to form bone.
- Osteoconduction: Scaffold for new bone growth.

⭐ Osteoinduction is the process by which mesenchymal stem cells are recruited and differentiate into osteoblasts, primarily mediated by Bone Morphogenetic Proteins (BMPs).
Bone Grafting Techniques - Sources & Sorts
-
Graft Sources & Properties:
- Autograft: Patient's own bone (e.g., iliac crest, fibula).
- Gold standard; non-immunogenic.
- All 3 properties: Osteogenic, osteoinductive, osteoconductive.
- Cons: Donor site morbidity (pain, infection), limited quantity.
- Allograft: Human donor (cadaveric/living).
- Types: Fresh-frozen, Freeze-Dried (FDBA), Demineralized (DFDBA).
- Properties: Osteoconductive. DFDBA also osteoinductive (BMPs).
- Cons: Potential immunogenicity, disease transmission risk (low), slower incorporation.
- Xenograft: Animal source (e.g., bovine, porcine; processed).
- Properties: Osteoconductive scaffold.
- Cons: Higher immunogenicity risk, potential for zoonoses.
- Synthetics (Alloplastics): E.g., Calcium phosphates (HA, TCP), sulfates, bioactive glass.
- Properties: Osteoconductive. Some osteoinductive if combined with BMPs.
- Cons: Variable resorption, potential mechanical weakness.
- Autograft: Patient's own bone (e.g., iliac crest, fibula).
-
Key Graft Characteristics (📌 GIC):
- OsteoGenesis: New bone formation by viable cells from graft.
- OsteoInduction: Chemical process stimulating host cells to form bone (e.g., BMPs).
- OsteoConduction: Scaffold guiding new bone growth.
⭐ Autograft is the only graft type possessing all three key properties: osteogenesis, osteoinduction, and osteoconduction.
Bone Grafting Techniques - Technique Tidbits
- Autograft Harvest Sites & Techniques:
- Iliac Crest Bone Graft (ICBG):
- Anterior (ASIS): Max 15-20 cc; Risk to Lateral Femoral Cutaneous N. (LFCN).
- Posterior (PSIS): Max 50-70 cc; Risk to Superior Cluneal Nerves.
- Reamer-Irrigator-Aspirator (RIA):
- Intramedullary (femur/tibia).
- Large volume, morselized cancellous graft.
- ↓ Donor site pain vs. ICBG.
- Iliac Crest Bone Graft (ICBG):
- Graft Incorporation - "Creeping Substitution":
- Host vessels invade graft.
- Osteoclasts resorb dead graft bone.
- Osteoblasts lay down new viable bone on graft scaffold.
- Process: Inflammation → Osteogenesis → Angiogenesis → Remodeling.
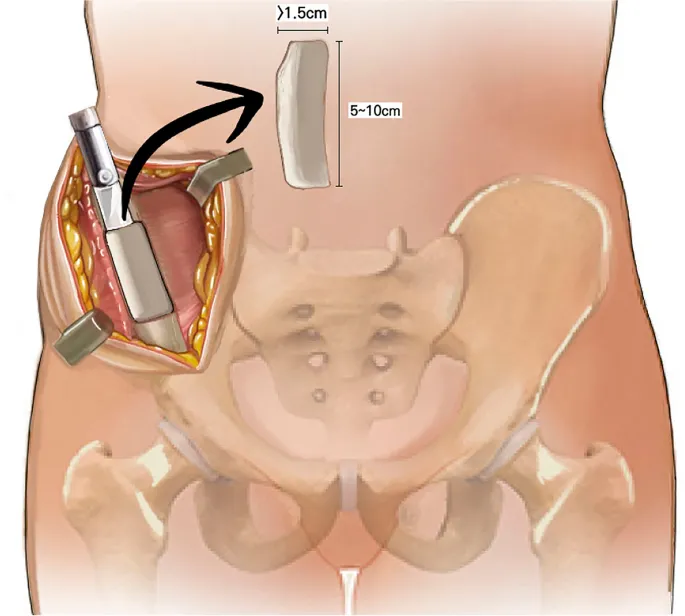
⭐ ICBG is considered the "gold standard" for bone grafting, providing all three properties: osteoconduction, osteoinduction, and osteogenic cells.
Bone Grafting Techniques - Uses & Uh-Ohs
-
Uses (Indications):
- Non-unions / Delayed unions
- Arthrodesis (joint fusion)
- Filling bone defects (trauma, tumor resection)
- Spinal fusion
- Augmenting fracture fixation
-
Uh-Ohs (Complications):
- Donor site morbidity (pain, infection, fracture) - 📌 Most common with iliac crest grafts.
- Graft failure / Non-union
- Infection (recipient or donor site)
- Disease transmission (allograft)
- Rejection / Immunological reaction (allograft)
- Fracture of the graft
⭐ Exam Favourite: Autografts are considered the gold standard due to their osteogenic, osteoinductive, and osteoconductive properties, minimizing rejection risk but having donor site morbidity as a key drawback. Allografts lack osteogenic cells but provide an osteoconductive scaffold and osteoinductive potential (if processed appropriately, e.g., DBM).
High‑Yield Points - ⚡ Biggest Takeaways
- Autograft: Gold standard; provides osteogenesis, osteoinduction, osteoconduction. Iliac crest common donor.
- Allograft: Osteoconductive, weakly osteoinductive; carries disease transmission and immunogenic risks.
- Synthetic grafts: (e.g., CaSO₄, CaP) Osteoconductive, biocompatible, no donor morbidity or disease risk.
- BMPs: Potent osteoinductive agents, stimulating new bone formation.
- Vascularized grafts: (e.g., fibula) Essential for large defects or avascular beds.
- Papineau technique: Staged open cancellous grafting for infected bone defects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

