Fibrous Dysplasia & Friends - Bone Weavers
- Fibrous Dysplasia (FD): GNAS1 mutation. Benign fibro-osseous lesion.
- Types: Monostotic (80-85%), Polyostotic.
- McCune-Albright Syndrome: Polyostotic FD, café-au-lait ("Coast of Maine"), endocrinopathy (e.g., precocious puberty).
- X-ray: Ground-glass, expansile; Shepherd's crook deformity (femur).
- Histo: "Chinese letters" woven bone in fibrous stroma; no osteoblastic rimming.
- Osteofibrous Dysplasia (OFD):
- Location: Anterior tibia/fibula cortex. Usually < 10 yrs.
- X-ray: Intracortical, lytic, often bubbly.
- Histo: Zonal pattern; woven bone rimmed by active osteoblasts.
- Key: Differentiate from adamantinoma (epithelial component).
⭐ In Fibrous Dysplasia, the characteristic "ground-glass" appearance on X-ray is due to the disorganized woven bone.

NOFs & Simple Cysts - Empty Nesters
-
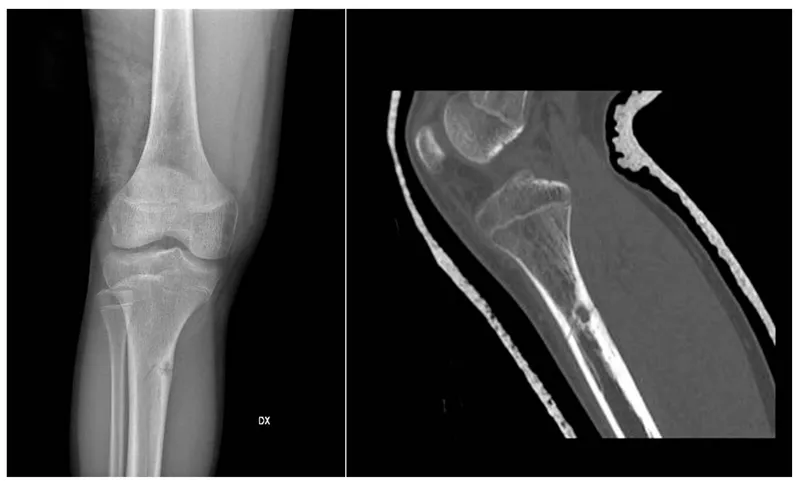
Non-Ossifying Fibroma (NOF / Fibrous Cortical Defect):
- Common benign fibroblastic lesion; ages 4-15 yrs.
- Location: Eccentric, intracortical, metaphysis (distal femur, tibia).
- X-ray: Lytic "soap bubble" appearance, sclerotic rim.
- Usually asymptomatic; most regress spontaneously.
- Tx: Observation. Curettage/grafting if symptomatic, >50% cortical involvement, or fracture.
-
Simple Bone Cyst (Unicameral Bone Cyst - UBC):
- Benign fluid-filled cavity; ages 5-15 yrs.
- Location: Central, intramedullary, metaphysis (proximal humerus > femur); migrates from physis.
- X-ray: Centrally lytic, thinned cortex, may show slight expansion.
- High risk of pathological fracture (~90%).
- Tx: Steroid/BM injection. Curettage/grafting for active/recurrent cysts.
⭐ UBC: "Fallen leaf" sign (fractured cortical bone fragment within cyst) is pathognomonic.
ABC & Reactive Builders - Expansive Efforts
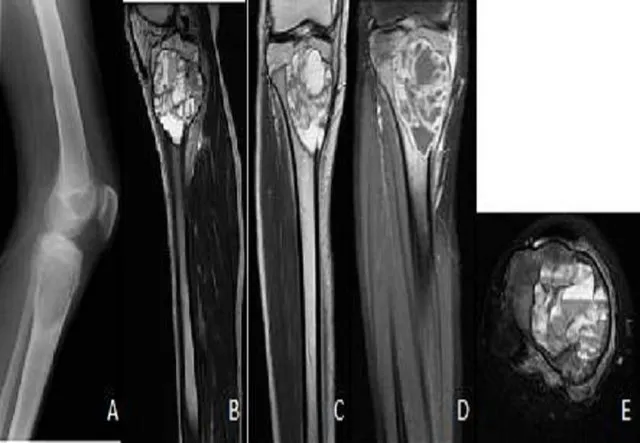
- Aneurysmal Bone Cyst (ABC)
- Benign, expansile, blood-filled cystic lesion; locally destructive.
- Age: 10-20 yrs; metaphysis (long bones), posterior spine.
- X-ray: "Soap bubble" appearance. MRI: Classic "fluid-fluid levels".
- Genetics: USP6 gene rearrangement (~70%).
- Tx: Curettage & bone grafting; sclerotherapy.
- Myositis Ossificans (MO)
- Reactive heterotopic ossification in muscle/soft tissue; often post-trauma.
- 📌 Mnemonic: "MOre Trauma, MOre Bone".
- Progression: Painful soft mass → painless, hard, well-defined lesion.
- Imaging: "Zonal phenomenon" (peripheral mature bone, central lucency). ⚠️ Early biopsy may mimic sarcoma!
- Tx: Conservative; excise if symptomatic post-maturation (6-12 mths).
⭐ ABC is notorious for its "fluid-fluid levels" on MRI, a key diagnostic clue.
Systemic Signals & Cell Stories - Body's Bone Banter
- Brown Tumor (Osteitis Fibrosa Cystica)
- Non-neoplastic bone lesion from ↑Parathyroid Hormone (PTH).
- Patho: ↑Osteoclast activity → bone resorption, cysts with hemosiderin-laden macrophages, giant cells.
- X-ray: Well-defined lytic, often expansile lesions; "salt-and-pepper" skull.
- Rx: Manage underlying hyperparathyroidism.
- Langerhans Cell Histiocytosis (LCH)
- Clonal proliferation of Langerhans cells (CD1a+, S100+).
- Spectrum:
- Eosinophilic Granuloma: Solitary/multiple bone lesions.
- Hand-Schüller-Christian: 📌 Triad: Bone lesions, Exophthalmos, Diabetes Insipidus (BED).
- Letterer-Siwe: Acute, disseminated, infants, poor prognosis.
- X-ray: "Punched-out" lytic lesions (geographic), beveled edge; vertebra plana ("coin-on-edge").

⭐ Histology: Birbeck granules (intracytoplasmic, "tennis-racket" appearance on Electron Microscopy) are pathognomonic for LCH.
High‑Yield Points - ⚡ Biggest Takeaways
- Fibrous Dysplasia: Ground-glass matrix, Shepherd's crook deformity; associated McCune-Albright.
- Unicameral Bone Cyst (UBC): Fallen leaf sign; common in proximal humerus/femur.
- Aneurysmal Bone Cyst (ABC): Expansile, lytic lesion with fluid-fluid levels; locally aggressive.
- Non-Ossifying Fibroma (NOF): Common fibrous defect; eccentric, soap-bubble appearance, often self-limiting.
- Eosinophilic Granuloma (LCH): Vertebra plana, punched-out lytic lesions; floating tooth.
- Osteoid Osteoma: Nocturnal pain relieved by NSAIDs; central nidus <1.5 cm.
- Brown Tumor: Due to hyperparathyroidism; presents as lytic lesions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

