Principles of Reconstruction - Blueprint for Bones
- Primary Goals:
- Oncological: Ensure adequate tumor margins (R0 resection).
- Functional: Restore limb function, stability, and pain-free motion.
- Durability: Provide a long-lasting construct, minimizing complications.
- Influencing Factors:
- Patient: Age, comorbidities, functional demands, bone stock.
- Tumor: Type, grade, stage, location, size of defect.
- Soft tissue: Quality and quantity of coverage.
- Timing:
- Immediate: Ideal for most; single-stage procedure.
- Delayed: If infection, inadequate soft tissue, or patient instability.
⭐ The "Reconstructive Ladder" principle guides choice: simplest effective method first, aiming for optimal outcome with least morbidity.
Reconstructive Options - The Bone Builder's Toolkit
Options restore form/function post-resection, from biological grafts to metallic implants, based on defect & patient.
| Option | Type | Key Features | Considerations |
|---|---|---|---|
| Autograft | Biological | Osteoinductive, -genic; No rejection | Limited supply, donor morbidity |
| Allograft | Biological | Structural; Osteoconductive | Disease risk, fracture, non-union |
| APC (Allograft Prosthetic Composite) | Biological | Allograft + Implant | Combined risks |
| Vascularized Graft (e.g., Fibula) | Biological | Living bone, hypertrophy | Complex, donor morbidity |
| Distraction Osteo. (Osteogenesis) | Biological | New bone (Ilizarov) | Lengthy, pin issues |
| Endoprosthesis (Megaprosthesis) | Non-Bio. | Early function. 📌 LIMB: Loosening, Infection, Mechanical fail, Bone loss | High complication risk (LIMB) |
| Arthrodesis | Non-Bio. | Fusion: stable, durable | ↓ Motion |
| Rotationplasty | Non-Bio. | Ankle as knee; durable motor | Cosmesis, young patients |
| Amputation | Non-Bio. | Definitive control | Functional/psychological |

Limb Salvage Surgery - Saving vs. Sacrificing
Limb Salvage Surgery (LSS) involves complete tumor resection with adequate margins, aiming to preserve a functional extremity. Amputation is considered when LSS is not feasible or oncologically unsafe.
- Indications for LSS:
- Resectable tumor with clear margins.
- Intact or reconstructible neurovascular structures.
- Adequate soft tissue and bone for reconstruction.
- Patient preference and good functional prognosis.
- Contraindications for LSS:
- Extensive neurovascular encasement.
- Pathological fracture with gross contamination.
- Uncontrolled infection.
- Poor patient compliance or severe comorbidities.
- MSTS Score: Functional assessment post-LSS; score >75% suggests good outcome.
⭐ Local recurrence is the most common cause of LSS failure, followed by infection and implant failure.
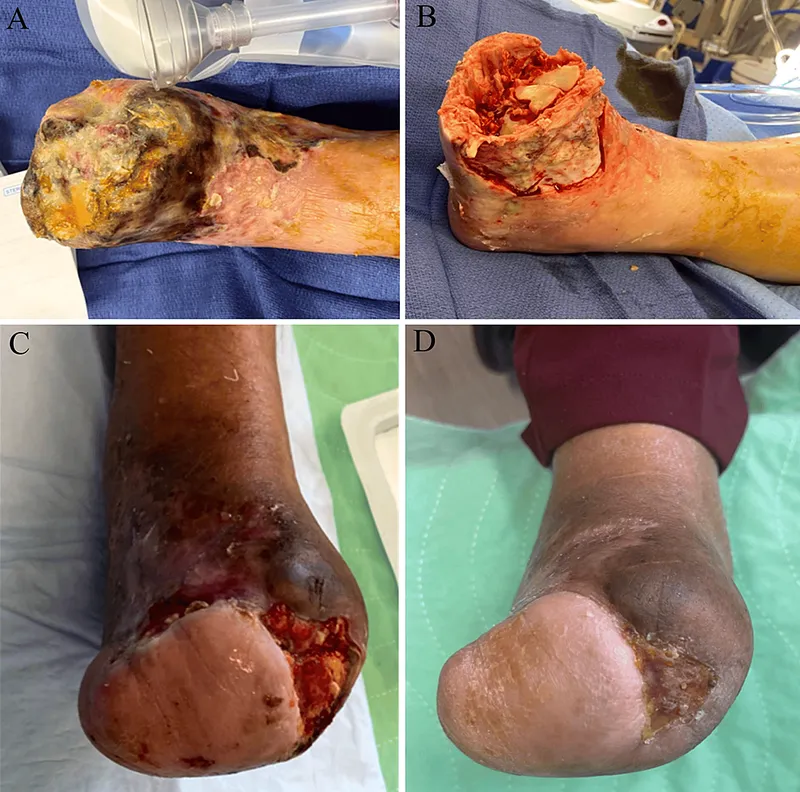
Complications & Outcomes - The Aftermath & Outlook
- Immediate & Early Complications:
- Infection (Surgical Site Infection: ~5-15%)
- Wound issues (dehiscence, hematoma)
- Neurovascular injury, Deep Vein Thrombosis (DVT)/Pulmonary Embolism (PE)
- Late Complications:
- Implant-Related:
- Aseptic loosening
- Structural failure (breakage, wear)
- Periprosthetic fracture
⭐ Aseptic loosening is the most common cause of long-term failure for endoprosthetic reconstructions after tumor resection.
- Tumor-Related:
- Local recurrence (e.g., <10% with wide margins for sarcomas)
- Metastasis
- Implant-Related:
- Functional Outcome:
- Assessed by MSTS (Musculoskeletal Tumor Society), TESS (Toronto Extremity Salvage Score) scores.
- Influenced by: tumor factors, reconstruction type, nerve status, rehabilitation.
- Overall Survival:
- Variable (e.g., Osteosarcoma 5-year survival ~60-70%).
High‑Yield Points - ⚡ Biggest Takeaways
- Reconstruction aims: Limb salvage, restoring function, stability, and achieving local tumor control.
- Enneking classification guides resection and choice of reconstructive technique.
- Key options: Endoprosthetic replacement (EPR), allografts, arthrodesis, rotationplasty.
- EPR is common for joint preservation following wide excision of tumors.
- Major risks: Infection, implant loosening/failure, periprosthetic fracture, allograft non-union.
- Adequate surgical margins are critical to prevent local recurrence.
- Amputation: for unresectable tumors or failed limb salvage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

