Basics of Staging - Staging 101 - Tumor Blueprints
- Purpose: Essential for predicting prognosis, guiding treatment strategies, and standardizing research communication.
- Key Elements:
- G (Grade): Tumor aggressiveness (histology).
- T (Tumor): Primary tumor's local extent/size.
- M (Metastasis): Distant spread (present/absent).
- 📌 Mnemonic: GTM - Go To Meet (the patient's needs with staging).
⭐ Accurate staging is the most crucial factor for determining prognosis and treatment strategy in musculoskeletal tumors.
Enneking System - Enneking's Map - Charting Tumors
The Musculoskeletal Tumor Society (MSTS) or Enneking system stages bone and soft tissue tumors for surgical planning.
-
Benign Tumor Stages (Arabic numerals):
- 1 (Latent): Intracapsular, inactive, well-marginated.
- 2 (Active): Intracompartmental, expansile, defined borders.
- 3 (Aggressive): Extracompartmental, locally destructive, ill-defined.
-
Malignant Tumor Staging (GTM System):
- G (Histologic Grade):
- G1: Low-grade malignant
- G2: High-grade malignant
- T (Anatomic Site - Compartment):
- T1: Intracompartmental (tumor confined within one anatomic compartment)
- T2: Extracompartmental (tumor extends beyond its originating compartment)
- M (Metastasis):
- M0: No metastasis
- M1: Metastasis present
- G (Histologic Grade):
-
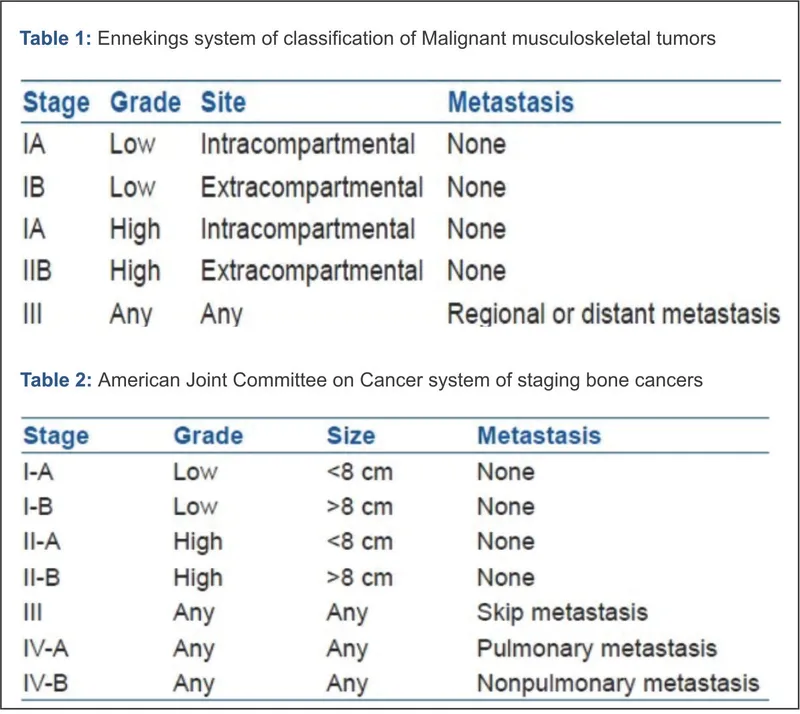
Malignant Stages:
- Stage IA: G1, T1, M0 (Low grade, Intracompartmental, No mets)
- Stage IB: G1, T2, M0 (Low grade, Extracompartmental, No mets)
- Stage IIA: G2, T1, M0 (High grade, Intracompartmental, No mets)
- Stage IIB: G2, T2, M0 (High grade, Extracompartmental, No mets)
- Stage III: Any G, Any T, M1 (Metastasis present)
⭐ The Enneking system (MSTS) is primarily used for surgical staging of primary bone sarcomas and aggressive benign tumors.
AJCC TNM System - The Universal Code
AJCC 8th Ed: Global standard for bone & soft tissue sarcoma (STS) staging.
- T (Tumor):
- STS: Size (T1: ≤5cm; T2: >5-≤10cm; T3: >10-≤15cm; T4: >15cm), depth, compartment.
- Bone: Extent in bone, adjacent structures.
- N (Nodes):
- N0: No regional node metastasis.
- N1: Regional node metastasis.
- (NX: Unassessable - avoid).
- M (Metastasis):
- M0: No distant metastasis.
- M1: Distant metastasis (e.g., lungs).
- G (Grade):
- Crucial for prognosis. Gx (unassessable), G1 (Low), G2/G3 (High).
- Stage Groups (I-IV):
- Combines T,N,M,G; separate for Bone & STS. Higher stage = worse prognosis.
⭐ The AJCC TNM system is the most widely used staging system for both bone and soft tissue sarcomas globally, crucial for multidisciplinary communication.
Staging Workup - Diagnostic Path - Unmasking Stages
- Biopsy: Crucial for diagnosis. Core needle preferred; incisional if needed.
⭐ A well-planned biopsy is critical in musculoskeletal oncology; a poorly performed biopsy can compromise limb salvage options and adversely affect prognosis.
- Imaging Protocol:
- X-ray: Initial assessment.
- MRI: Details local extent, soft tissue, neurovascular involvement.
- CT Chest: Screens for lung metastases.
- Bone Scan/PET-CT: Detects skeletal metastases, assesses systemic spread.
High‑Yield Points - ⚡ Biggest Takeaways
- Enneking staging for bone tumors: Benign (1-Latent, 2-Active, 3-Aggressive); Malignant (I-Low, II-High grade; III-Metastasis).
- Malignant Enneking: A for intracompartmental, B for extracompartmental.
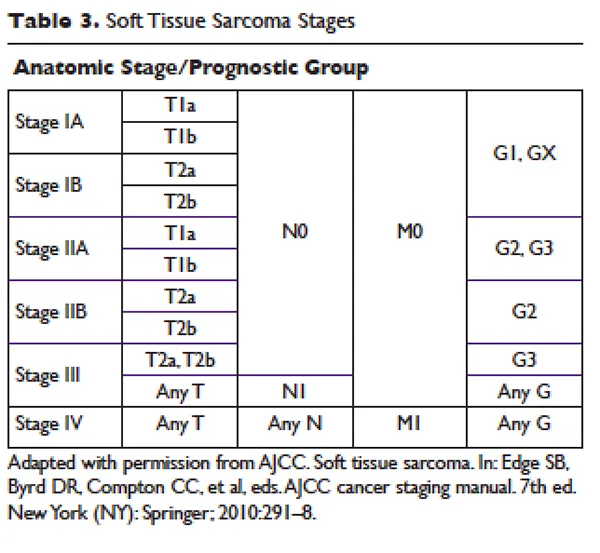
- AJCC staging (TNM + Grade) for soft tissue sarcomas; grade is most prognostic.
- MSTS components: Grade (G), Site (T) (intra/extracompartmental), Metastasis (M).
- Staging guides treatment: observation, curettage, wide excision, amputation, or neoadjuvant therapy.
- Improper biopsy can upstage a tumor by violating compartments.
- Skip metastases in bone tumors imply Stage III (M1) in Enneking anco MSTS staging systems for musculoskeletal tumors are crucial for prognosis and treatment planning. Enneking staging is primarily for bone tumors, categorizing them by grade (G), local extent (T), and metastases (M). Benign lesions are staged 1 (latent), 2 (active), 3 (aggressive). Malignant lesions are Stage I (low-grade), II (high-grade), III (metastases), with A (intracompartmental) or B (extracompartmental). AJCC staging is more common for soft tissue sarcomas, also using TNM and grade. Grade is a critical prognostic factor. Proper biopsy technique is vital to avoid tumor spillage and upstaging. Staging dictates surgical margins and adjuvant therapy needs. Skip metastases are considered distant metastases (M1).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

